- Anatomical terminology
- Skeletal system
- Joints
- Muscles
- Heart
- Blood vessels
- Lymphatic system
- Nervous system
- Respiratory system
- Digestive system
- Urinary system
- Female reproductive system
- Male reproductive system
- Endocrine glands
- Eye
- Ear
Salivary glands
The salivary glands (Latin: glandulae salivariae) are exocrine glands of the digestive system located in the oral cavity or close to it with their ducts opening and excreting their produced secretion in the oral cavity. The salivary glands are classified regarding their size and duct types, and the human body contains two groups of salivary glands - minor and major salivary glands.
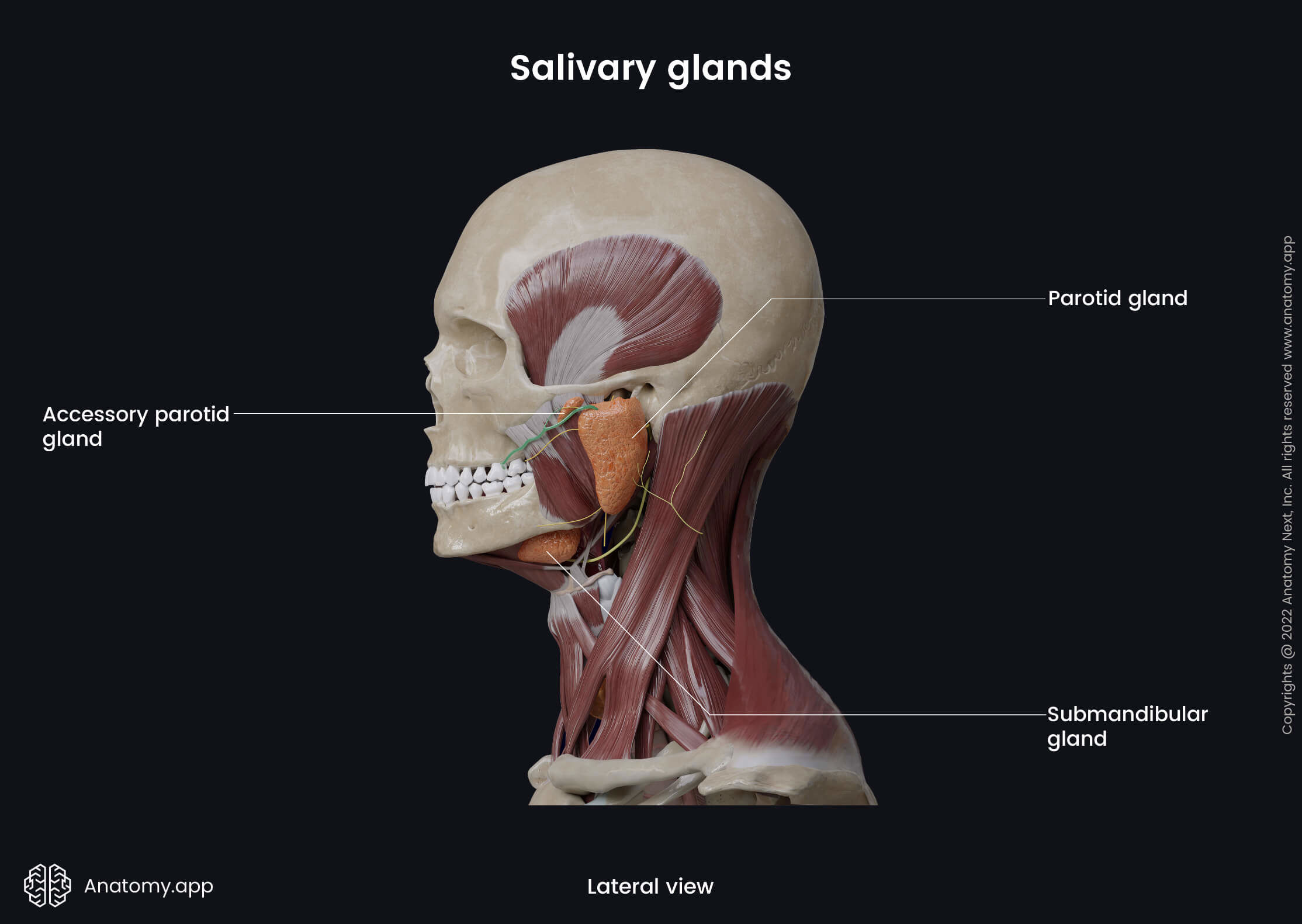
The salivary glands produce and excrete a watery substance called saliva that participates in digestion. The major glands are the primary glands that provide moistening, lubrication and protection of the mucosa of the oral cavity and structures within it. Gland-produced saliva starts the chemical food procession, and it helps in digestion, food lubrication during swallowing and bolus creation.
Minor salivary glands
The minor salivary glands are located within the mucosa of the oral cavity, and each gland excretes saliva on its surface. The minor salivary glands mainly function for the lubrication of the oral cavity. They produce only around 1% of the total daily amount of saliva. Overall, the oral cavity contains about 800 - 1000 dispersed minor salivary glands. They are classified depending on their location, and the oral cavity has four groups of the minor salivary glands:
- Labial salivary glands in the lips
- Buccal salivary glands in the cheeks
- Palatine salivary glands in the palate (subdivided into glands of the hard and soft palate)
- Lingual salivary glands in the tongue
The buccal and labial salivary glands with their ducts open in the oral vestibule, but the ducts of the palatine and lingual glands open in the oral cavity proper.
Major salivary glands
As the name suggests, the major salivary glands are much larger than the minor salivary glands. They are a group or a collection of exocrine tissue providing the secretion of saliva through one central duct that opens in the mucosa of the oral cavity. The major gland-produced saliva mainly provides the initiation of digestion and protection of mucosa. There are three pairs of salivary glands associated with the oral cavity:
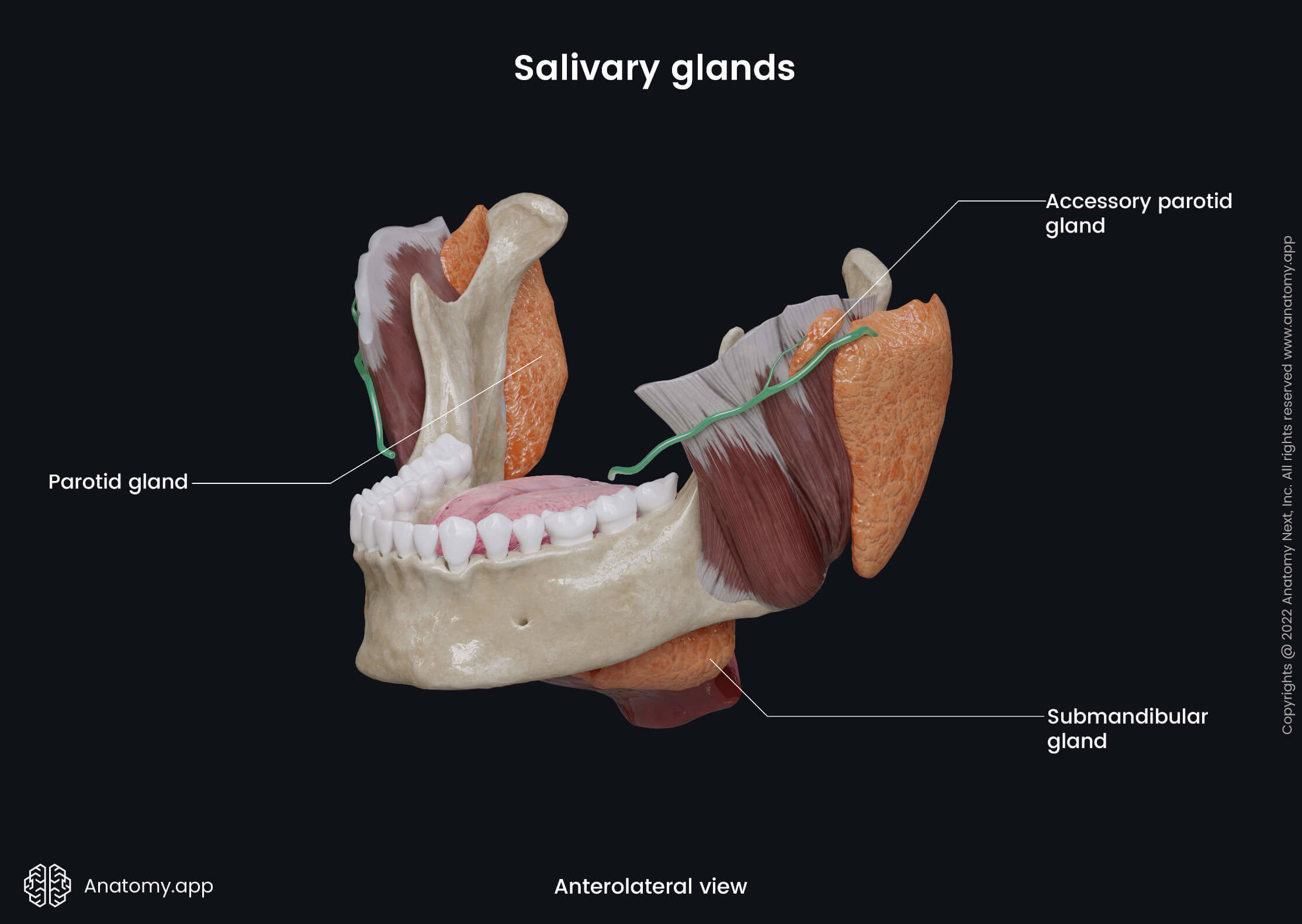
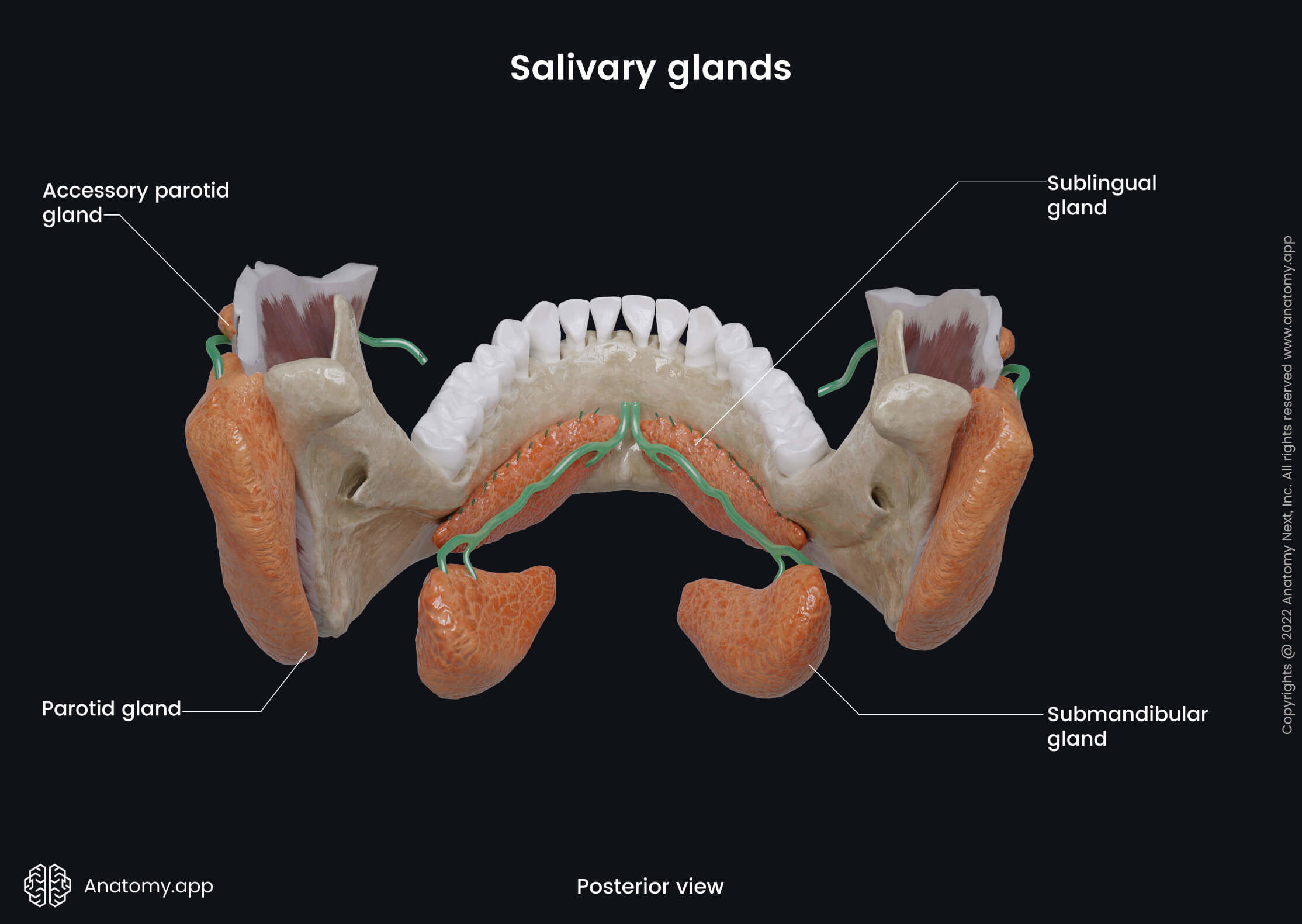
Parotid gland
The parotid gland is the largest salivary gland, and it has an inverted pyramidal shape. The parotid gland participates in the formation of the cheeks by giving them fullness. It weighs around 20 - 30 grams and produces about 60 - 65% of daily saliva. The parotid gland has a fibrous capsule called the parotid sheath formed by the parotid fascia that covers the gland from all sides.
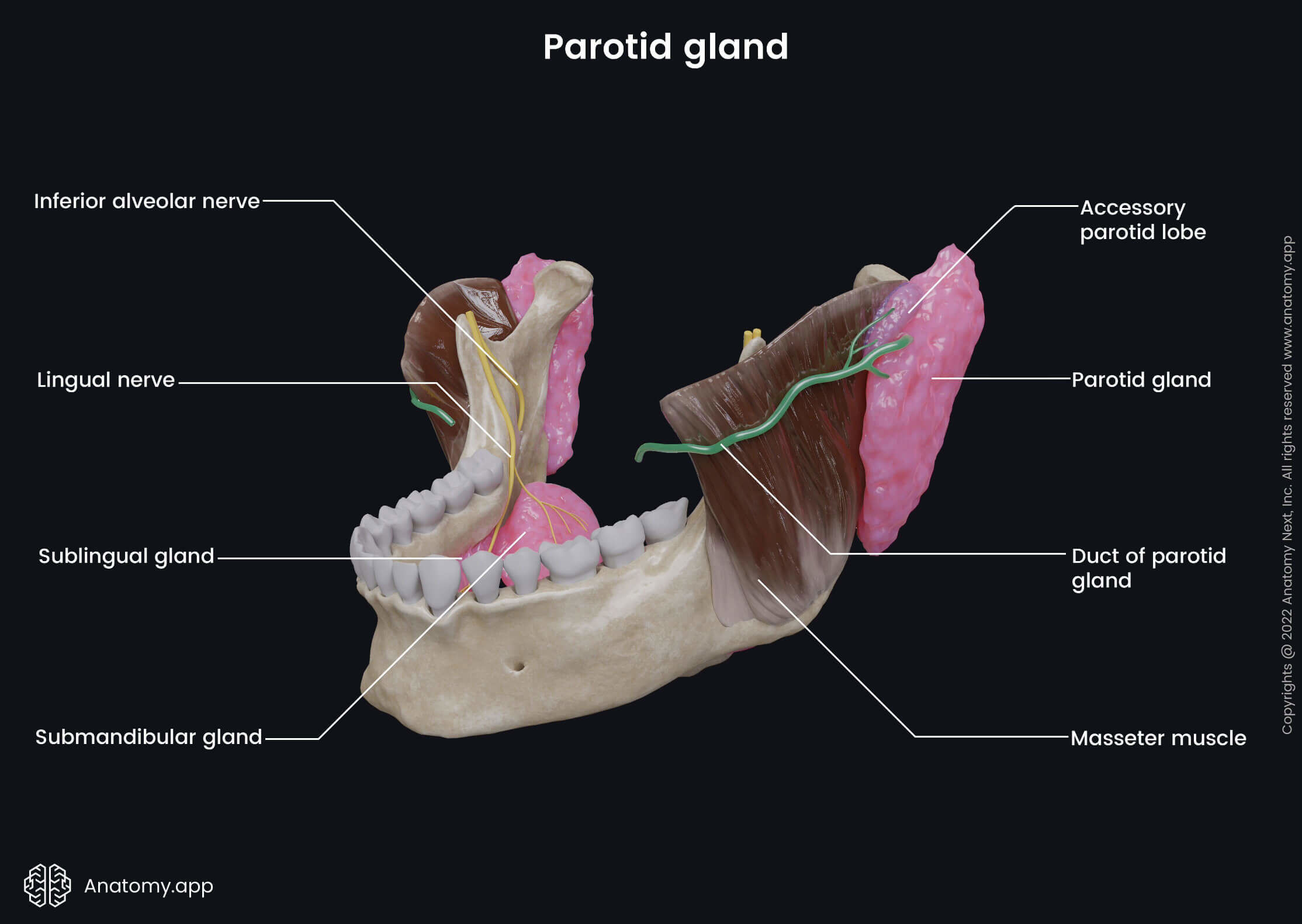
The parotid gland is positioned on the lateral side of the face, anterior to the auricle of the external ear. This region is also known as the parotid or preauricular area. Anterior to the parotid gland is the masseter muscle, while posterior is the external ear and sternocleidomastoid muscle. Superior to the gland is the zygomatic arch, and inferior is the mandible and its angle. The parotid gland has two lobes and one central duct.
Parotid gland lobes
The parotid gland is composed of two parts known as the superficial and deep lobes. Both lobes are separated by the facial nerve (CN VII), and between them are fatty tissues.
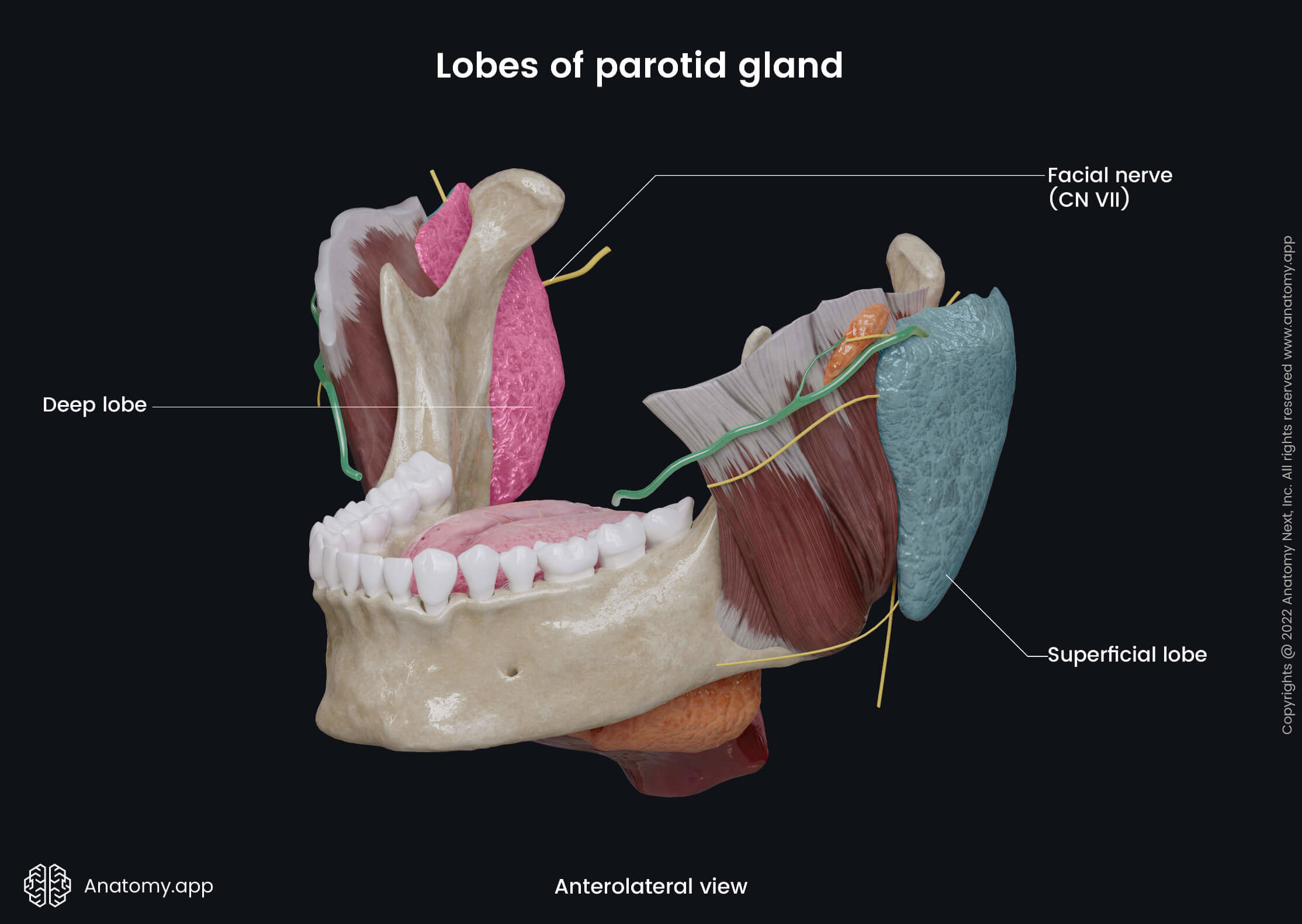
Superficial lobe
The superficial lobe is located lateral to the facial nerve (CN VII). It lies subcutaneously in the preauricular area, anterior to the external acoustic meatus. The superficial lobe lies on the outer surface of the masseter. Superior, it extends to the zygomatic arch, anterior goes to the middle one-third of the masseter, and inferior, the superficial lobe extends until the mandibular angle. In the posterior direction, the superficial lobe turns into the deep lobe.
Deep lobe
The deep lobe is located in the retromandibular fossa and lies medial to the facial nerve (CN VII). Its anterior aspect borders the posterior edge of the mandibular ramus, but the posterior aspect connects with the mastoid process of the temporal bone and sternocleidomastoid muscle. The deep lobe has a medial border with the styloid process of the temporal bone and three muscles originating from it (stylohyoid, stylopharyngeus and styloglossus).
Parotid duct and its opening
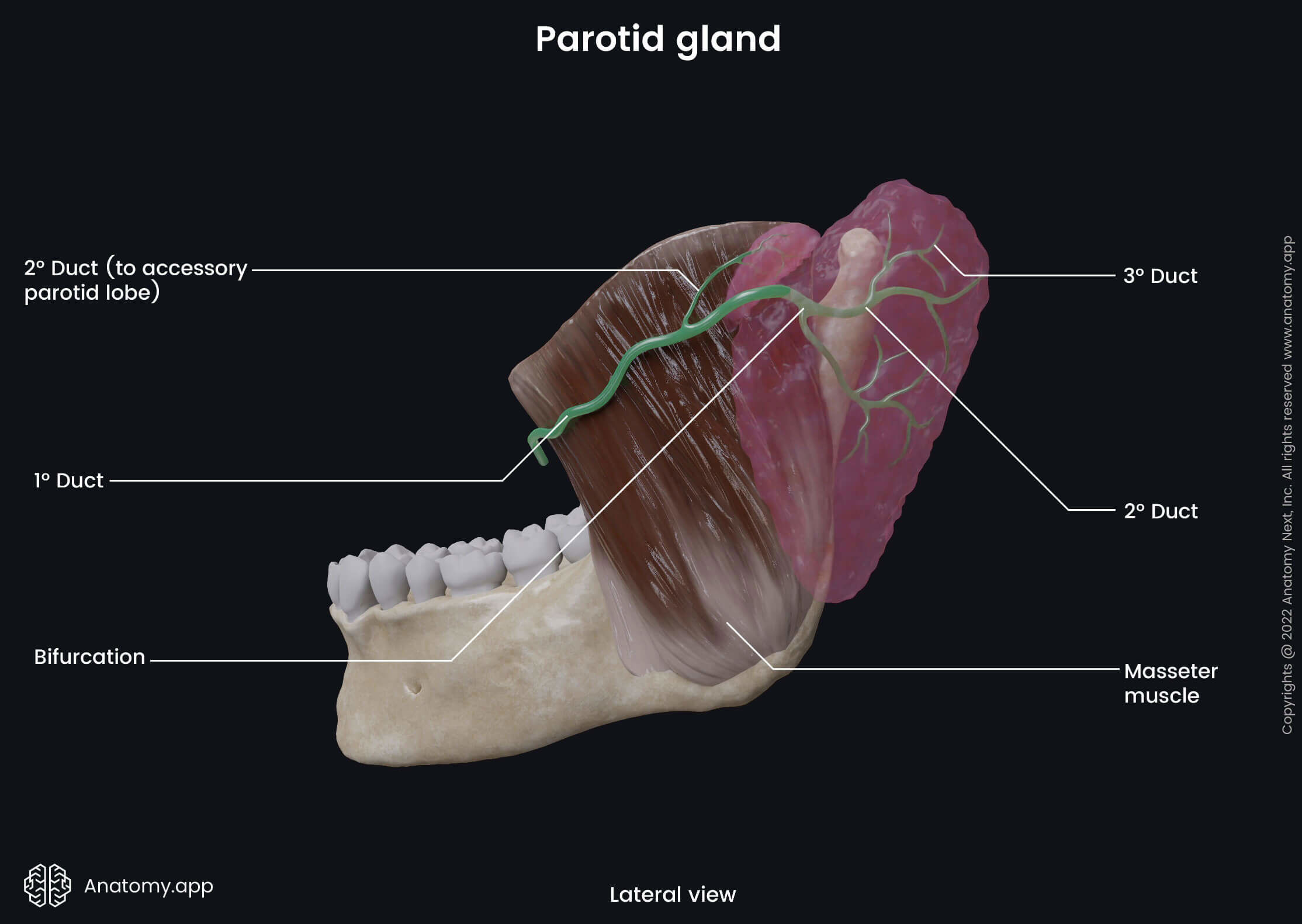
The parotid duct, also known as the Stensen's duct, is the central excretory duct of the parotid gland. It goes through the cheeks, and it is around 5 - 7 cm long and 1.5 - 2.5 millimeters wide. The parotid duct goes from the anterior border of the gland to the zygomatic arch. It extends below the zygomatic arch, wraps around the anterior margin of the masseter muscle, and passes horizontally over its surface.
Next, the parotid duct pierces the buccinator muscle and reaches the oral cavity, where it opens with the papilla of the parotid duct. The papilla is situated within the buccal mucosa opposite the second maxillary molar tooth. Through the parotid duct, saliva from the parotid salivary gland reaches the oral cavity, where it helps in the digestion process and moistens the oral cavity.
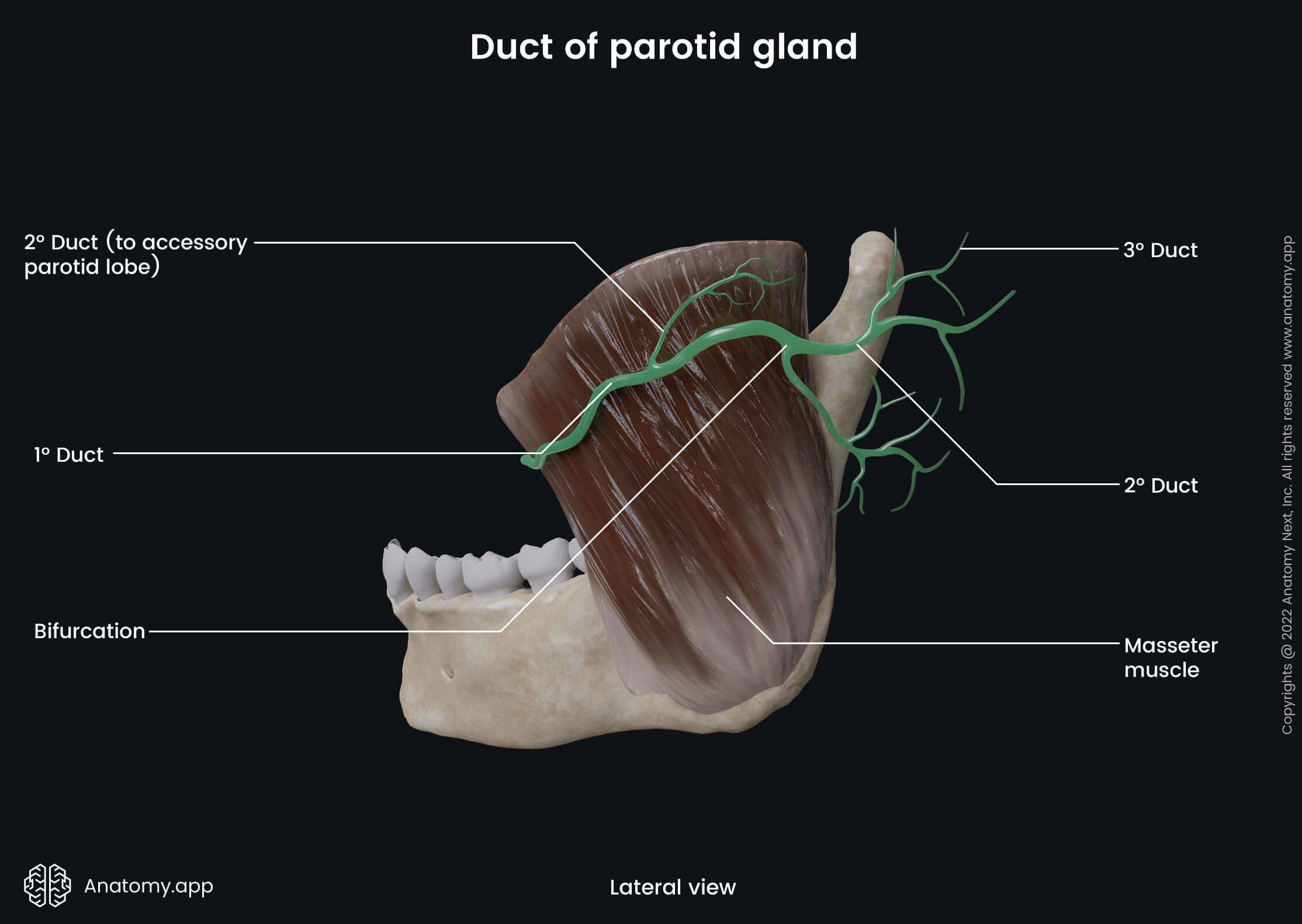
Anatomical relations
Besides the facial nerve (CN VII) passing through the parotid gland and subdividing it, two more anatomical structures cross the parotid gland - the external carotid artery and the retromandibular vein. The facial nerve (CN VII) divides the gland into two lobes and gives its five terminal branches within the gland. More from the superior aspect of the gland arises the temporal and zygomatic branches, while more from the central area - buccal, margin mandibular and cervical branches.
The external carotid artery ascends through the gland and gives two terminal branches - the superficial temporal and maxillary arteries. Also, the posterior auricular artery arises from the external carotid artery within the gland. Within the gland, the maxillary and superficial temporal veins form the retromandibular vein that continues to go through it. The auriculotemporal branches from the mandibular division of the trigeminal nerve (CN V3) also cross the gland.
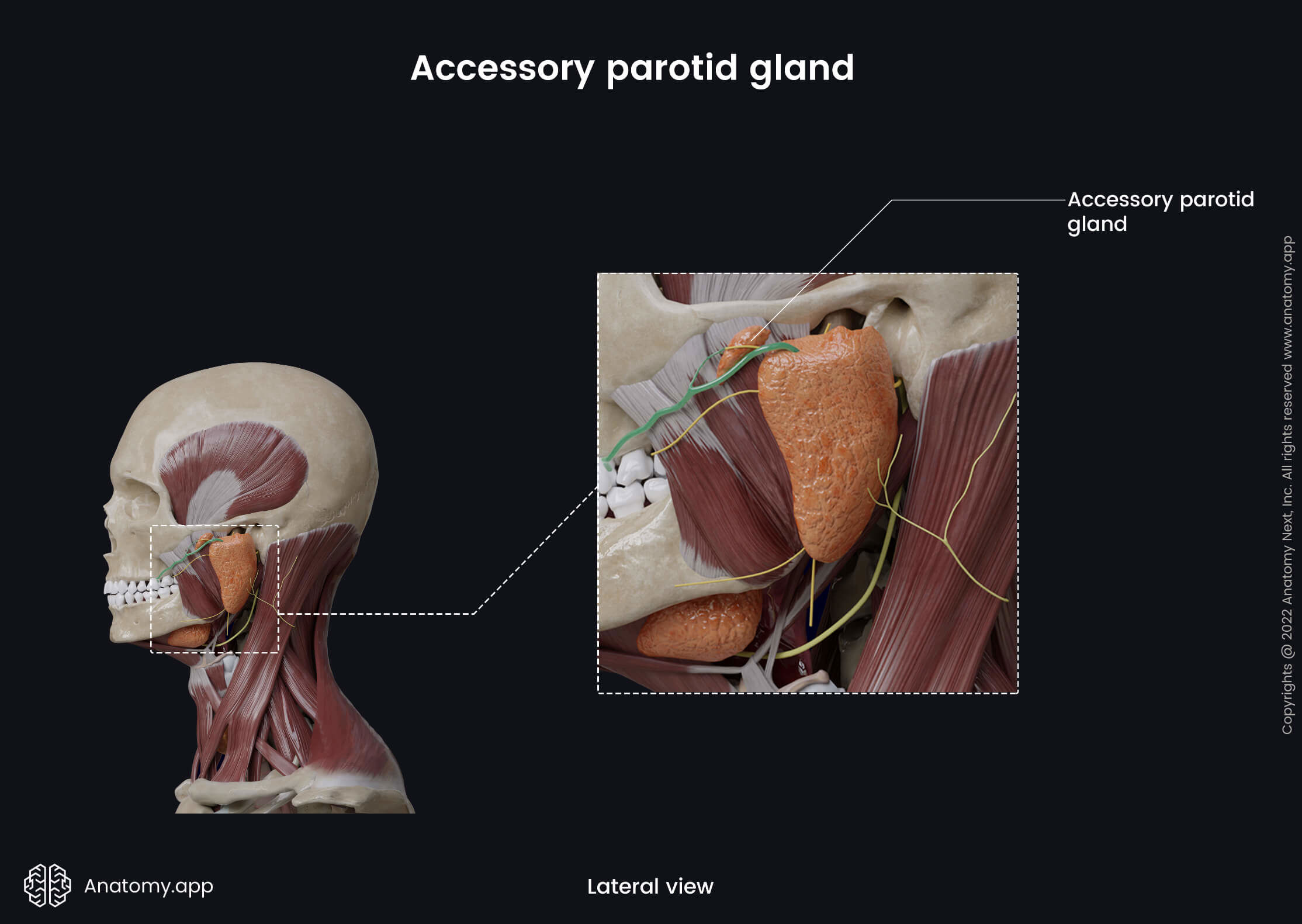
Accessory parotid gland
In about 50% of people, the parotid gland has an accessory parotid gland referred to as the accessory lobe of the parotid gland. It is located anterior and more in the superior aspect of the gland, and its inferior part connects with the superior aspect of the parotid duct. The accessory parotid gland can have one or several smaller ducts connected with the parotid duct.
Submandibular gland
The submandibular gland is the second largest salivary gland, and it is situated below the muscles that form the floor of the oral cavity. Each submandibular gland weighs around 10 grams and appears elongated, a bit flattened and has the shape of the letter "U" (horseshoe-shaped).
Without the stimulation of the parotid gland, the submandibular gland can produce around 70% of the daily saliva. But when the parotid gland receives stimuli, the submandibular gland produces about 10 - 30% of daily saliva. The superficial layer of the cervical fascia encloses the gland and forms a closed space. Like the parotid gland, the submandibular gland has two lobes and one central excretory duct.
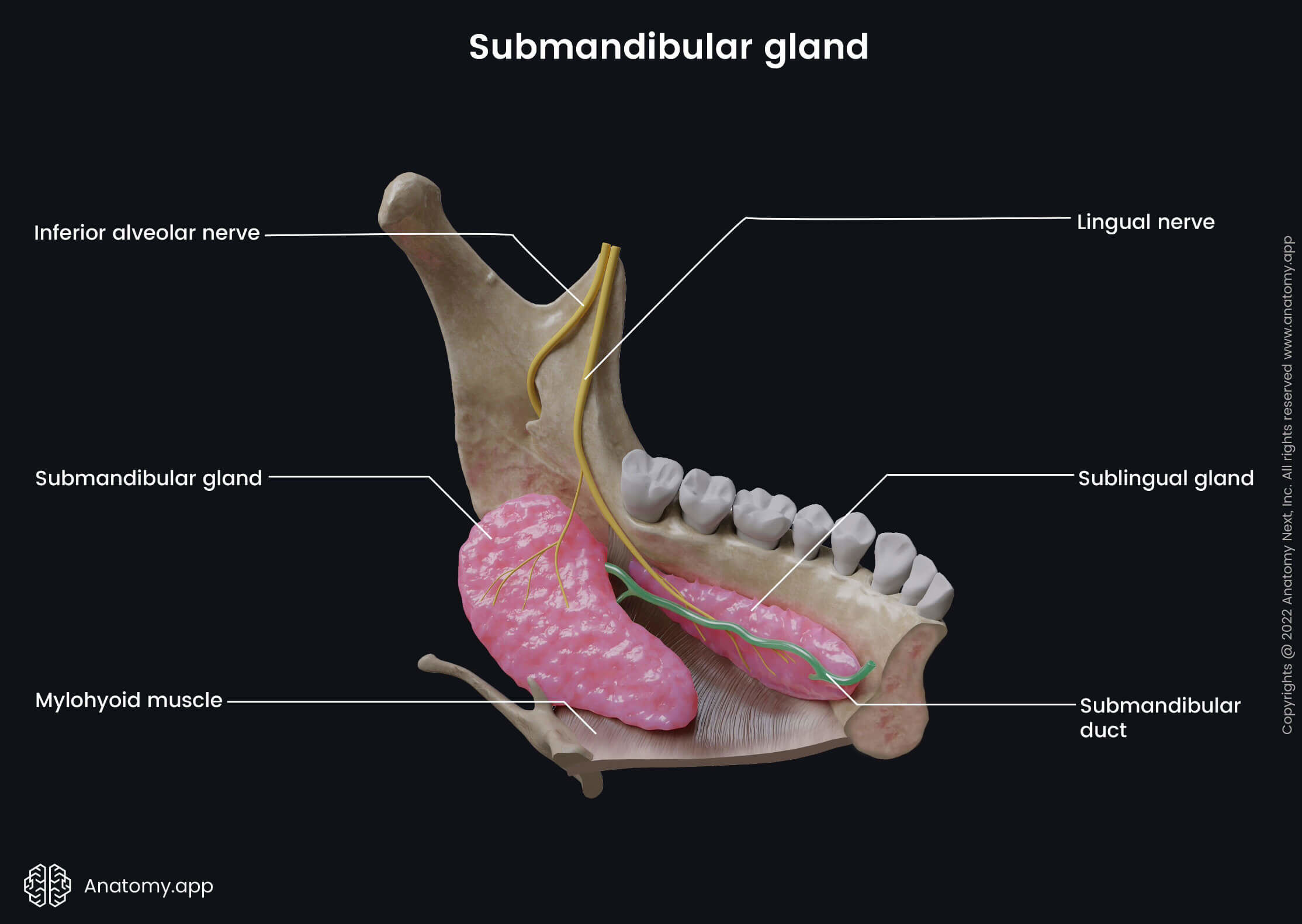
Submandibular gland lobes
The submandibular gland is composed of two lobes - the superficial and deep. Both lobes are continuous with each other, and they are separated by the mylohyoid muscle. Fibers from the posterior border of the mylohyoid extend into the gland, and the gland wraps around them.
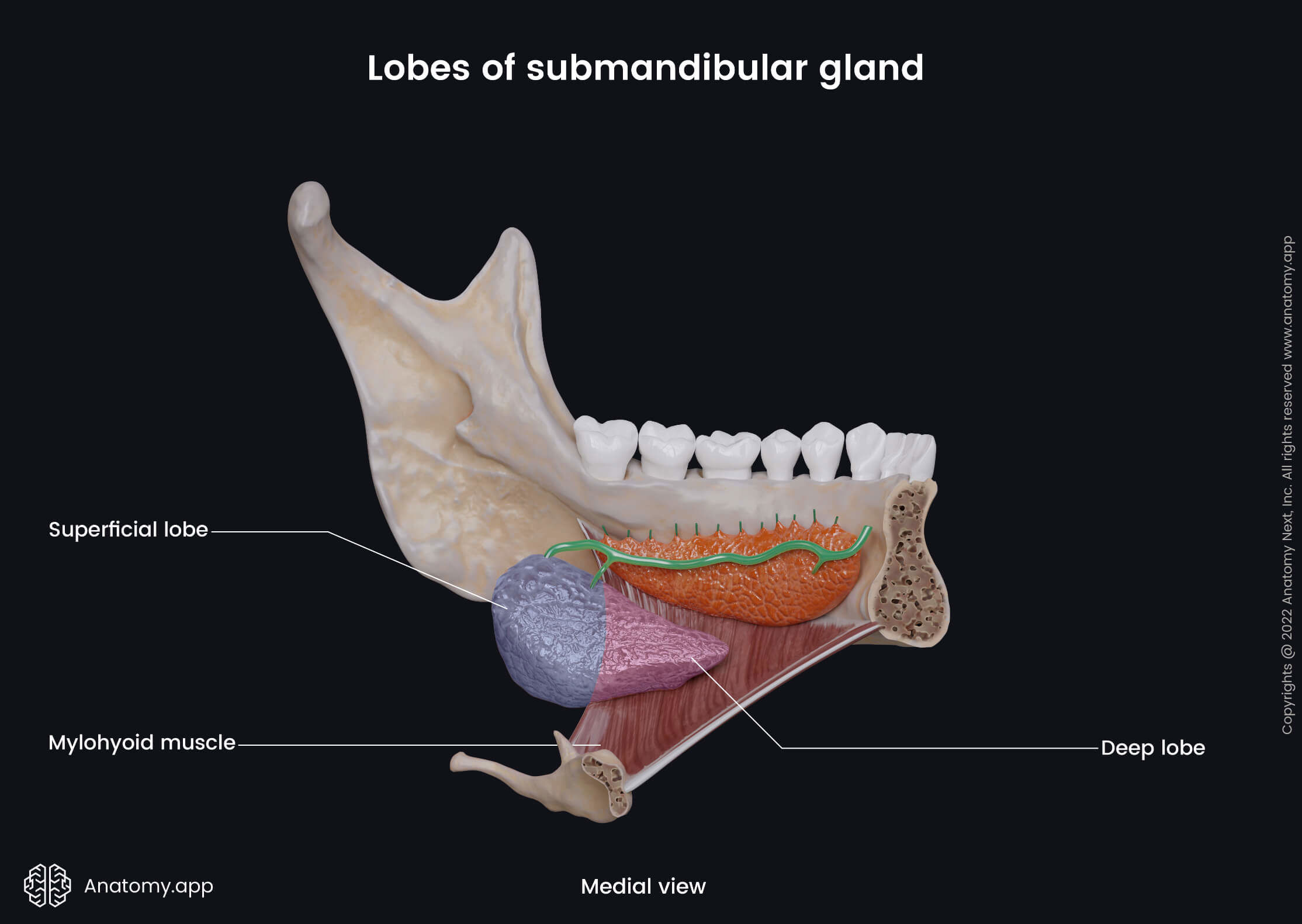
Superficial lobe
The superficial lobe of the submandibular gland is located in the submandibular triangle. The submandibular triangle is a part of the anterior neck triangle, and its borders are defined by the body of the mandible and anterior and posterior bellies of the digastric muscle. The superficial lobe is the largest lobe of two, located more inferior. The deep lobe is located more medial.
Deep lobe
The deep lobe of the submandibular gland lies in the submandibular fossa located on the inner surface of the body of the mandible. The submandibular fossa is situated on the lateral side of the mental spine, inferior to the middle portion of the mylohyoid line. The deep lobe is positioned between the mandibular body on one side and the lateral surface of the hyoglossus muscle on the other.
The deep lobe participates in the formation of the floor of the oral cavity, and it ends close to the posterior aspect of the sublingual gland. The lingual nerve goes along the mandible facing the surface of the deep lobe. It begins lateral to the submandibular duct and goes beneath it in the space between the sublingual and submandibular glands. And finally, the lingual nerve terminates by giving branches.
Submandibular duct and its opening
The saliva from the submandibular gland reaches the oral cavity proper via the submandibular duct - a central excretory duct of the submandibular gland. It is also known as the Wharton's duct, and it is around 4 - 5 centimeters long and 1.5 - 2 millimeters wide.
The submandibular duct wraps around the posterior edge of the mylohyoid muscle and gets above the muscles of the oral cavity floor. Next, it goes in the medial direction, and along the upper surface of the mylohyoid, it reaches the sublingual caruncle (papilla) and opens through it in the oral cavity. On the way to the caruncle, it crosses with the lingual nerve.
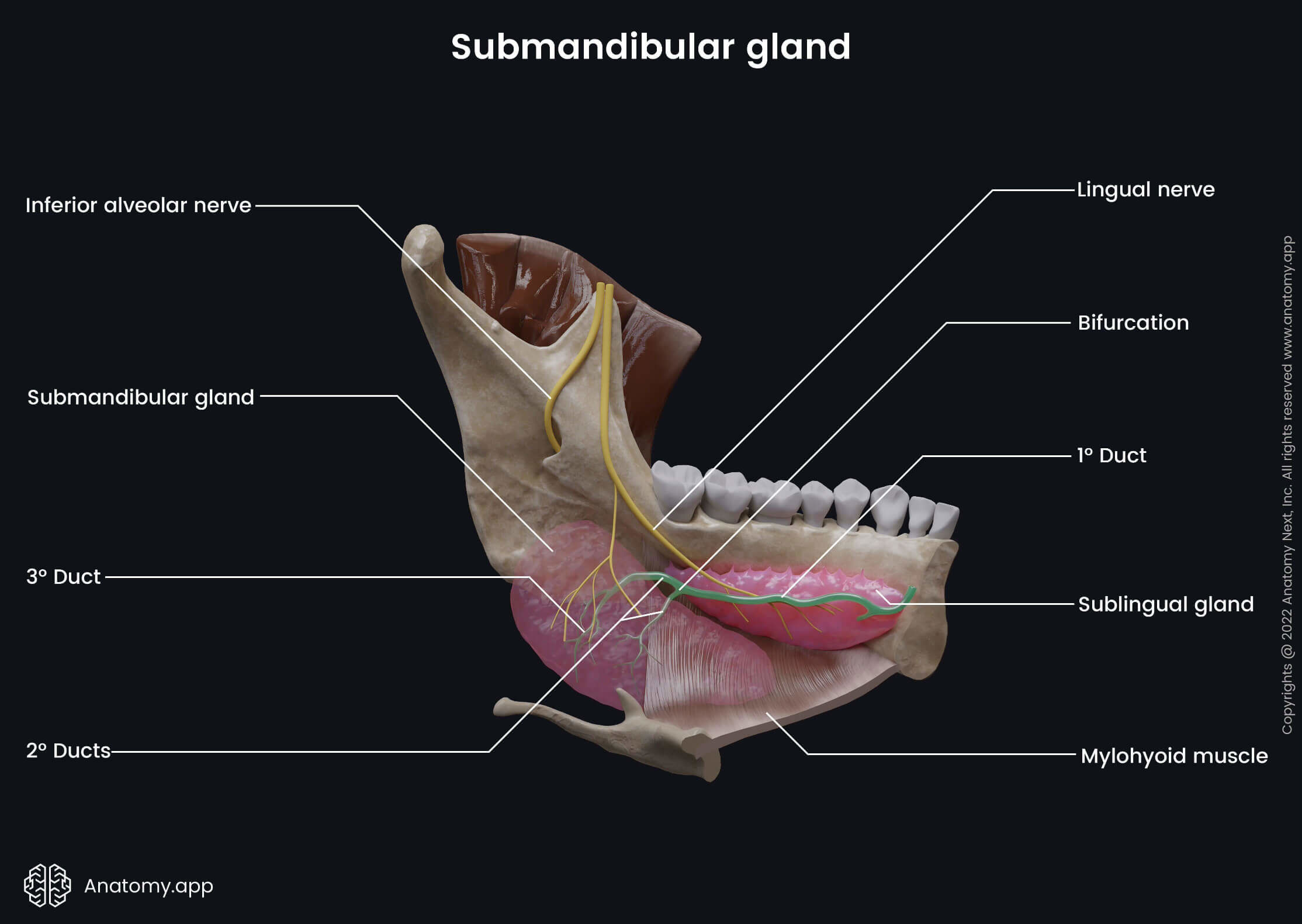
The mucosa covering the ventral surface of the tongue forms a sagittal-oriented fold called the lingual frenulum, and it anchors the tongue to the floor of the oral cavity. On either side of the lingual frenulum, at the site where it terminates, is a small eminence called the sublingual caruncle. It is a papilla at which the main ducts of the sublingual and submandibular salivary glands open.
Sublingual gland
The sublingual salivary gland is the smallest major salivary gland, weighing only around 5 grams. The sublingual glands contribute about 5% of daily saliva. They are directed longitudinally and have a lentiform shape when viewing them along the body of the mandible. The sublingual salivary glands resemble almonds.
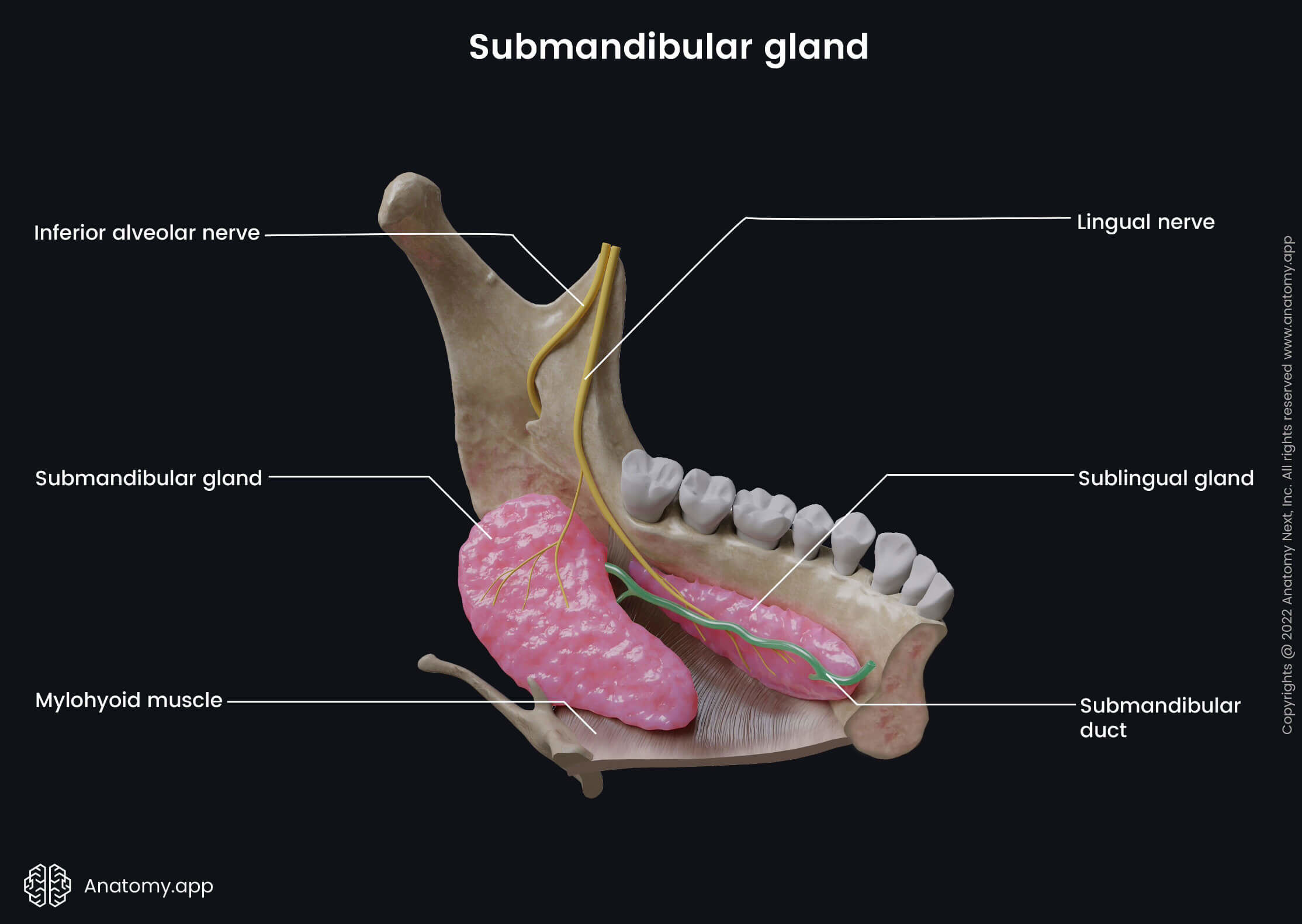
Sublingual gland location and relations
The sublingual salivary glands are located above the muscles of the oral cavity floor, and the mucosa of the oral cavity covers both glands. Above the glands are the lateral sides of the tongue. The inferior aspect of the sublingual gland lies on the superior surface of the mylohyoid muscle. In the medial direction, it connects with the genioglossus and hyoglossus muscles.
Along the gland on its medial side goes the lingual nerve and submandibular duct. The lateral and anterior aspects of the gland face the mandible and lie in the sublingual fossa located on the inner surface of the mandibular body. Both sublingual glands are located very close to each other within the mental spine area of the mandible. The sublingual fossa is positioned on the lateral side of the mental spine, superior to the medial end of the mylohyoid line.
Sublingual duct and its opening
The gland is covered by the mucosa of the oral cavity that forms a mucosal fold called the sublingual plica that overlies the gland. The sublingual plica extends in the lateral direction from the sublingual caruncle. The sublingual gland is classified as the major salivary gland, and therefore, it should have only one central duct. However, it has one major and several minor ducts transporting saliva from the gland directly into the oral cavity.
The central sublingual duct is also called the duct of Bartholin, but the minor ducts are known as the Rvinus ducts. Near the sublingual caruncle, the central duct joins the submandibular duct and, together with it, opens in the sublingual caruncle. Along the sides on the sublingual plicas and towards the sublingual caruncle, the minor ducts of the sublingual salivary gland open.
Salivary gland histology
All major salivary glands are classified as the exocrine type glands, as their produced saliva is transported to a body surface via the ducts. The minor salivary glands are compound glands with a simple duct system, while the major salivary glands are compound glands that contain complex duct systems, and the ducts give branches. All major glands are composed of two parts:
- Stroma - connective tissue portion;
- Parenchyma - consists of secretory cells.
Stroma
All major glands are covered by the connective tissue capsule. From the capsule, the connective tissue goes into the glands and divides them into smaller lobules. The parotid and submandibular glands have not only lobules but also lobes as they are larger than other salivary glands. The connective tissue of the capsule divides the glands into lobes, and within the lobe, the connective tissue subdivides the lobes into lobules. Between the lobules are the parenchyma consisting of secretory cells.
Parenchyma
The terminal secretory unit of the salivary glands is called the acinus. An acinus is also a functional unit of the salivary glands, and it contains mucous, serous or mixed cells depending on the type of saliva they produce. All glands have many myoepithelial cells - contracting cells that help in the excretion process by emptying the ducts from saliva.
Saliva can be either serous, mucous or mixed. Mucous saliva is rich in carbohydrates and mucins, while serous saliva is rich in proteins. The alveolar (acinar) configuration of acini is associated with the serous cells, and alveolar glands contain sac-like secretory portions. The tubular configuration is associated with the mucous cells, and tubular glands have tube-like acini. Minor salivary glands mostly contain mucous cells, and they have tubular acini.
Parotid gland
The parotid gland is a compound acinar (alveolar) gland, and it is the only serous salivary gland. The intralobular connective tissue of the gland contains many blood vessels and fat cells that increase with aging.
Submandibular gland
The submandibular gland is a mixed salivary gland, meaning it contains serous and mucous secretory units. It is a compound tubulo-acinar (tubulo-alveolar) gland. Most acini are mixed or serous, so it mainly produces serous saliva. Serous cells make up about 90 - 95%, while mucous only around 5 - 10%. The submandibular gland is the only salivary gland functioning as an exocrine and an endocrine gland. Its striated ducts produce insulin-like substances and nerve growth factors.
Sublingual gland
The sublingual gland is also a compound tubulo-acinar (tubulo-alveolar) gland. Most acini are mixed or mucous, so the sublingual gland mainly produces mucous saliva, although it can also produce serous saliva.
Duct system
The lobules contain two different intralobular ducts - the intercalated and striated ducts. The striated ducts arise from the intercalated ducts - the smallest ducts that drain individual acini. Outside the lobules within the connective tissue are the interlobular ducts that form the central excretory duct. The epithelium of the central duct is usually the simple columnar, pseudostratified columnar or stratified cuboidal epithelium.
Salivary gland functions
The primary function of all salivary glands, regardless of their size, is to produce saliva - a seromucous transparent and stretchy liquid with a pH of 6.2 - 7.6. Saliva further provides several essential functions described below. It mainly contains water - around 99.5%. All salivary glands produce about 1 - 1.5 liters of saliva per day.
- Saliva regulates the balance of acids and alkalines in the oral cavity. When a person ingests very acidic food, saliva neutralizes the acid and protects the enamel of the teeth. As saliva maintains a constant pH, it is also responsible for the presence of normal oral microflora.
- It moistens and lubricates ingested food and the mucosa of the oral cavity. Saliva protects the mucosa from the mechanical forces and helps in bolus (chewed food mixed with the saliva) formation. Food lubrication allows for more efficiently swallowing. Lubrication also has a protective role as lubricated mucosa makes it harder for bacteria to attach to the epithelium.
- Saliva contains an enzyme called amylase that splits carbohydrates. Therefore, it starts the chemical food procession in the oral cavity.
- It contains proteins, mucus, electrolytes and inorganic substances such as minerals. Therefore, saliva supplies the teeth with minerals (it contains calcium salts).
- Saliva prepares food for taste buds. In order to taste the food, substances within it must be dissolved in saliva, so saliva acts as a solvent.
- It regulates food temperature and makes hot food easy to digest. When hot food is mixed with saliva, food temperature decreases.
- Saliva provides dental hygiene and protection by washing away food remains from the teeth after digestion.
- It contains substances such as lysozyme, IgA and secretory protein complexes providing antibacterial protection.
- Saliva releases mercury and iodine in case of poisoning. Therefore, healthcare professionals inspect saliva to diagnose disorders.
- During embryological development, saliva stimulates the growth of taste buds and odontoblast differentiation.
Neurovascular supply of salivary glands
Arterial blood supply
The arterial blood supply to the parotid gland is provided by the branches of the maxillary, posterior auricular, superficial temporal and transverse facial artery. The submandibular salivary gland is perfused by the submental artery and glandular branches of the facial artery.
The sublingual gland receives arterial blood supply from the sublingual and submental arteries. The first is a branch of the lingual artery, while the second branches of the facial artery. The facial, lingual and posterior auricular arteries arise from the external carotid artery, and the superficial temporal and maxillary arteries are its terminal branches.
Venous drainage
Small veins draining the parotid gland carry venous blood to the superficial temporal vein, which further drains into the retromandibular vein. The retromandibular vein flows into the external jugular vein. The deep lobe of the parotid gland is drained by the pterygoid venous plexus that carry blood next to the maxillary vein. From the maxillary vein, blood reaches the retromandibular vein. The superficial lobe is drained by the facial vein that carries blood next to the internal jugular vein.
Venous drainage of the submandibular gland is provided by the facial and sublingual veins that carry blood next to the internal jugular and lingual veins, respectively. The sublingual gland is drained by the sublingual and submental veins that flow next to the lingual and facial veins, respectively.
Lymphatic drainage
Lymph from the parotid gland is drained to the superficial and deep cervical lymph nodes via the local lymph nodes such as the infraparotid and paraparotid nodes. The parotid gland is surrounded by many regional lymph nodes that create a lymphatic network providing the lymphatic drainage from the surrounding tissue and structures such as the auricle or structures of the middle ear. Most of all nodes are located close to the superficial lobe of the parotid gland. Lymph from the submandibular and sublingual glands is carried to the submandibular and deep cervical lymph nodes.
Innervation
All salivary glands receive nerve supply from both divisions of the autonomic nervous system - the sympathetic and parasympathetic nervous systems. The autonomic nervous system mainly regulates the secretion of saliva, and increased parasympathetic stimulation leads to increased saliva production. But the sympathetic nervous system decreases and inhibits the secretion and reduces the gland blood flow through vasoconstriction (narrowing of the blood vessels).
The parotid gland is supplied by the autonomic and sensory innervation. It receives the parasympathetic innervation through the auriculotemporal and glossopharyngeal (CN IX) nerves. The preganglionic fibers are formed by the lesser petrosal nerve - a branch of the glossopharyngeal nerve (CN IX). They go to the otic ganglion, where they synapse. From the otic ganglion, the postganglonic secretomotor fibers reach the parotid gland via the auriculotemporal nerve. The auriculotemporal nerve is a branch of the mandibular division of the trigeminal nerve (CN V3). The sympathetic innervation of the parotid gland is provided by the superior cervical ganglion. The parotid gland is also innervated by the sensory fibers of the auriculotemporal nerve.
The submandibular and sublingual glands receive parasympathetic innervation from the chorda tympani fibers. The chorda tympani is a branch of the facial nerve (CN VII). Preganglionic fibers go to the submandibular ganglion. Both glands receive the innervation via the postganglionic chorda tympani secretomotor fibers. The sympathetic innervation comes from the superior cervical ganglion. The sensory innervation is provided by the lingual nerve of the mandibular nerve (CN V3).
Salivary gland disorders
The salivary glands have an essential role in digestion, and if the gland is damaged, it can lead to decreased saliva production, causing a wide variety of issues associated with digestion, food swallowing and chewing, infection development, teeth disorders and many more to follow. Salivary gland disorders include such diseases as sialolithiasis, sialadenitis and mumps.
Salivary gland disorders can present as isolated diseases, affecting only the glands, or they can be manifestations of systemic diseases. Sjogren's syndrome is an autoimmune disorder affecting organs that produce secretions and decrease production. One of the symptoms is mouth dryness and salivary gland swelling because of reduced saliva production. The most common causes of salivary gland disorders are as follows:
- Duct obstruction by stones
- Duct twists
- Infections and inflammation
- Systemic and autoimmune diseases
- Tumors
- Excessive alcohol consumption
Sialolithiasis
Sialolithiasis is a disorder characterized by stone formation within the salivary gland ducts, and it is the most common cause of salivary gland swelling. Various factors decrease the secretion of saliva, and it can lead to calcium salt precipitation that can further result in calcium stone formation. Most often, sialolithiasis presents in males between 30 and 65 years.
Usually, sialolithiasis affects the submandibular salivary gland and its ducts. The reason is that the submandibular duct ascends, and saliva drains towards the sublingual caruncle. The submandibular gland is a mixed gland, and it produces serous and mucous saliva. Mucous saliva is more viscous, and it flows slower. The sublingual and minor salivary glands rarely have stones within their ducts.
While the exact mechanism of stone formation is unknown, several factors are related to it. These risk factors include the following:
- Reduced water intake and dehydration (it leads to thickened saliva)
- Reduced food intake (it decreases saliva production)
- Certain medications that reduce saliva production (some antidepressants, antihistamines, antihypertensives, diuretics)
- Systemic diseases (Sjogren's syndrome, systemic lupus erythematosus)
- Radiation therapy for cancers in the oral cavity
- Smoking
- Gout
Stones can be present without any symptoms, but symptoms appear if the stone gets stuck in one of the ducts. The severity of symptoms depends on the blockage of the duct and whether it is entirely or just partially blocked. Sialolithiasis presents with a salivary gland swelling and pain that worsens during eating. Usually, a few hours after eating, the pain disappears as the flow of the saliva normalizes. It can be challenging to swallow the food and open the mouth. Also, mouth dryness can be present.
Small stones usually get out of the ducts on their own, while larger stones typically need surgical removal. Treatment options include extracorporeal silalolithotripsy, endoscopic stone removal, endoluminal balloon dilatation and stone extraction. Untreated sialolithiasis can lead to infection, inflammation or even abscess formation.
Sialadenitis
Sialadenitis is salivary gland inflammation. More often, elderly adults and people who already have sialolithiasis have it. Sialadenitis can be acute or chronic. Usually, it affects the parotid gland, so it is called parotitis. It is caused by various infections, salivary gland stones and autoimmune diseases (Sjogren's syndrome, Wegner's granulomatosis), or the cause can be unknown.
Acute sialadenitis usually is caused by infectious diseases but chronic sialadenitis by autoimmune disorders. The most common cause of acute sialadenitis is a viral infection called mumps. Other viral infections include HIV, parainfluenza, Epstein-Barr virus, cytomegalovirus and coxsackievirus. The most common bacteria causing sialadenitis is Staphylococcus aureus. Usually, sialadenitis presents as a painful and tender lump in the salivary gland area. Also, increased temperature, chills and weakness can be present. In more severe cases, ducts secrete purulent discharge.
Sialadenitis is treated with hydration, painkillers and drugs for the cause. For example, a bacterial infection is treated with antibacterial therapy. Usually, after the treatment is started, sialadenitis soon starts to improve. Besides various drugs, lemon juice or hard candies can be used to increase saliva production. Severe cases can result in abscess formation. However, most patients have a good prognosis, and the condition is self-limiting or is easy to treat.
Mumps
Mumps is an infectious disease with a viral etiology, and it is caused by the mumps virus from the Paramyxoviridae family. Usually, mumps affects the parotid gland, and the disorder is known as mumps parotitis. Mumps parotitis presents with swelling of both or only one parotid gland. The swelling can also present with pain at the site where the gland is located or pain during chewing. Headaches, fever, weakness, appetite loss and muscle aches are also symptoms of mumps parotitis.
Mumps virus is very contagious, and it is spread through direct contact or by air. Before mumps presents with the swelling of the parotid salivary gland, it can manifest with headache, fatigue and low-grade fever. Mumps parotitis can lead to potentially dangerous complications such as:
- Orchitis
- Hearing loss
- Meningitis and encephalitis
- Pancreatitis
In pregnant women, mumps can cause miscarriage. There is no specific treatment. However, the best possible prevention is the MMR vaccination.