- Anatomical terminology
- Skeletal system
- Joints
- Muscles
- Heart
- Blood vessels
- Lymphatic system
- Nervous system
- Respiratory system
- Digestive system
- Urinary system
- Female reproductive system
- Male reproductive system
- Endocrine glands
-
Eye
- Accessory structures of eye
- Ear
Eye
The eye (Latin: oculus) is a bilateral sensory organ, which is responsible for the sense of sight. Anatomically, the eye is formed by the eyeball and accessory structures of the eye. The eyeballs are located in the orbits of the skull. The frontal part of the eye is visible, while the posterior part is in the orbital cavity.
Eyeball
The eyeball is a spheroidal structure containing sense receptors for vision. Even though, most people think that the eyeball is shaped like a ball, it has an almost spherical shape, but is more like a two-piece unit consisting of the anterior and posterior segments.
The eyeball is less high than it is wide. Its height or vertical (sagittal) size is around 23.7 mm, the width or horizontal (transverse) size – approximately 24.2 mm, and the depth or anteroposterior (axial) – 22 to 24.8 mm.
The anterior segment of the eyeball is the frontal part, which small, transparent, and creates around 1/6 of the eyeball. The posterior segment is larger and forms 5/6 of the eyeball. The eyeball has an anterior and a posterior pole. Both poles are connected via the optic axis. The midway between both poles is known as the equator.
The eyeball consists of three layers (fibrous, vascular, nervous) that surround the vitreous body, and other structures that along with the vitreous body belong to the refractive media of the eyeball. The eyeball lies within the orbit and is surrounded by adipose tissue. The eyeball is covered by a thin fascial sheath known as the Tenon’s capsule.
Layers of eyeball
The eyeball has three main layers surrounding the vitreous body:
- Fibrous layer - the outer layer, consisting of sclera and cornea;
- Vascular pigmented layer - the middle layer, formed by choroid, ciliary body, and iris;
- Nervous layer - the inner layer of the eyeball, also known as the retina.
Fibrous layer of eyeball
The fibrous layer of the eyeball consists of two portions: sclera - the largest posterior part, which is white in colour, and cornea - the anterior part of the fibrous layer, resembling a transparent plate. The sclera and cornea are continuous with each other.
Sclera
The sclera is a white outer layer surrounding the posterior five-sixths of the eyeball. The sclera is the thickest posteriorly and its outer surface is smooth, with except for the site where the tendons of the orbital muscles attach to it.
Anteriorly, the sclera is continuous with the cornea. The connection site is called the corneoscleral junction. A circular canal known as the scleral venous sinus (or canal of Schlemm) lies behind the junction. It collects aqueous humor from the anterior chamber of the eye.
The sclera has a posterior pole that is perforated by the optic nerve (CN II) via the posterior scleral foramen. It also has other openings: four anterior openings, four to five middle openings, numerous posterior openings. The sclera has three sublayers:
- Episclera - the outermost layer of the sclera, formed by loose connective tissue, attaches to the Tenon's capsule;
- Scleral stroma - dense irregular connective tissue beneath the episclera;
- Lamina fusca - a thin pigmented innermost layer, which connects the sclera to the choroid.
The sclera receives arterial blood supply by the episcleral plexus, as well as the long and short posterior ciliary arteries. Venous drainage happens through the vorticose veins (also known as vortex veins) that drain into the superior and inferior ophthalmic veins. The sclera is innervated by the long and short ciliary nerves.
The sclera acts as a barrier for other components of the eyeball and protects them from mechanical trauma. The rigid structure of the sclera is the reason why the eyeball can maintain its shape and keep all the structures in place.
Cornea
The cornea covers the frontal one-sixth of the eyeball. It is a circular and transparent layer covering the pupil, iris, and anterior chamber of the eye. The cornea does not contain any blood vessels but has receptors. The cornea consists of five sublayers:
- Stratified corneal epithelium - the superficial layer of the cornea;
- Bowman’s membrane - beneath the epithelium, consists only of irregularly arranged collagen fibers with no cells in it;
- Substantia propria - the thickest layer, making up almost 90% of the cornea;
- Descemet’s membrane - the basement membrane of the corneal endothelium, connected to the network of the scleral venous sinus;
- Corneal endothelium - the deepest sublayer of the cornea, consisting of a single layer of epithelial cells, continuous with the endothelium of the iridocorneal angle.
The cornea is avascular, therefore, the nutrients are supplied by the aqueous humor. The central part of the cornea receives oxygen indirectly from the air, while the peripheral part - by diffusion from the anterior ciliary arteries. The cornea is innervated by fibers from the ophthalmic division of the trigeminal nerve (CN V1), mainly via the long ciliary nerves.
The cornea participates in the refraction of light - the bending of a light wave when it travels through a transparent medium. The cornea has the most considerable refractive power, and its refractive index is different from the refractive index of the air.
Vascular pigmented layer of eyeball
The middle vascular layer of the eyeball is rich with blood vessels and pigment. It is composed of three portions: choroid, ciliary body and iris. The choroid is the largest portion of the vascular layer. One of the main functions of the ciliary body is the production of aqueous humor. The iris contains pigment that determines the eye color of an individual.
There is a hole in the middle of the iris called the pupil. The narrowing of the pupil is provided by the sphincter pupillae, while the widening is provided by the dilator pupillae. These are smooth muscles surrounding the pupil and innervated by the autonomic nervous system.
Choroid
The choroid is a thin coat lining the inner surface of the sclera. It is rich with blood vessels and accounts for almost 90% of the total blood flow within the eyeball. The choroid lies between the optic nerve (CN II) and the ciliary body. It is the thickest at the posterior pole of the eyeball. Between the sclera and the choroid is a space called the perichoroidal space. The choroid has three sublayers:
- Vessel layer - the outermost choroidal layer, contains arteries that are branches of the short posterior ciliary arteries;
- Capillary layer - consists of a network of capillaries that have sac-like dilatations;
- Bruch’s membrane - the innermost layer with five components, including the basement membrane of the capillary endothelium, outer layer of collagen fibers, network of elastic fibers, inner layer of collagen fibers, and the basement membrane of the retina’s pigmented epithelium.
The choroid is supplied by the posterior ciliary arteries arising from the ophthalmic artery. Venous drainage happens through the vorticose veins. Innervation is provided by the long and short ciliary nerves. The main function of the choroid is to provide blood supply to the outer layers of the retina.
Ciliary body
The ciliary body is found in front of the choroid. The ciliary body consists of connective tissue, smooth muscle cells, and blood vessels. The frontal part of the ciliary body is called ciliary crown (corona ciliaris), while the dorsal part – ciliary ring (orbiculus ciliaris).
The ciliary crown gives around 70 radial extensions called ciliary processes, which contain cells that produce aqueous humor. The anterior and long posterior ciliary arteries meet in the anterior part of the ciliary body. The ciliary body is also a passage for nerves. The ciliary body has four sublayers:
- Ciliary epithelium - two layers of cubital cells, has pigmented and unpigmented parts;
- Ciliary stroma - loose connective tissue beneath the epithelium;
- Ciliary muscle - plays an important role in the accomodation process;
- Supraciliary layer - made of collagen fibers.
The ciliary body receives arterial blood supply via the anterior ciliary and long posterior ciliary arteries. The venous blood is drained by the vorticose veins. Innervation of the ciliary body is provided by the short ciliary nerves.
As mentioned, the ciliary body is responsible for the production of the aqueous humor and involved in accommodation. Accommodation is the process during which the eye transforms its optic power to ensure a clear vision or focus on an object as its distance changes.
Iris
The iris is found in front of the ciliary body and is continuous with it. The iris consists of blood vessels, connective tissue, and smooth muscle cells. The iris is a thin, contractile structure with pigment and a central opening – the pupil.
The anterior surface of the iris has two margins or zones - a large ciliary zone and a smaller pupillary zone. Both zones join together in a place called the collarette. The iris divides the space between the cornea and the lens into the anterior and posterior chambers of the eye. From anterior to posterior, the iris is divided into three parts:
- Anterior border layer - the anterior surface of the iris has no epithelium and contains large depressions called the crypts of Fuchs;
- Stroma of the iris - consists of extensively vascular connective tissue containing collagen fibers, fibroblasts, melanocytes, and extracellular matrix, as well as nerve fibers and smooth muscle cells
- Epithelial layers - contains pigmented epithelial cells, located beneath the stroma.
The sphincter pupillae muscle is found in the pupillary zone of the iris, and it narrows the pupil. The dilator pupillae muscle is found as a myoepithelium layer extending from the root of the iris to the sphincter pupillae. The dilator pupillae widens the pupil. By controlling the dilatation and constriction of the pupil, the iris controls how much light enters the eye.
The iris is supplied by radial vessels from the stroma of the iris. The arteries originate from the major arterial circle found in the stroma of the ciliary body. The venous drainage of the iris happens through the veins that follow the mentioned arteries, also creating a minor venous circle. The iris is innervated by the long and short ciliary nerves.
Nervous layer of eyeball (retina)
The nervous layer of the eyeball is called the retina, and it is the deepest layer. It is the light-sensitive structure of the eye, where the neural visual pathway begins. The retina can be further divided into two parts: pigmented or outer layer and neurosensory or inner layer (neural retina). The space between both layers is called the subretinal space. The retina lies between the choroid externally and the aqueous humor internally.
The retina has many sublayers and various types of cells. The neural retina contains three neural cell types: light-sensitive photoreceptor cells (rods and cones), bipolar cells, and ganglion cells of the retina. Additionally, there are supporting cells and other components in the retinal layers. Overall, the retina is made up of ten layers, which are as follows (from outermost to innermost):
- Retinal pigment epithelium - a single layer of cells, separated from the choroid by the Bruch's membrane);
- Photoreceptor layer - contains the light-sensitive parts of the photoreceptor cells (rods and cones);
- External limiting membrane - situated at the bases of the photoreceptor cells, formed by synapses between Müller cells and photoreceptor cells, and between Müller cells themselves;
- Outer nuclear layer - houses the bodies of the rodes and cones;
- Outer plexiform layer - formed by interactions between different cells, including photoreceptor, bipolar and horizontal cells;
- Inner nuclear layer - houses the bodies of different cells, such as the bipolar, horizontal, amacrine and Müller cells;
- Inner plexiform layer - interactions between bipolar, ganglion and amacrine cells;
- Ganglion cell layer - houses the bodies of the ganglion cells;
- Retinal nerve fiber layer - formed by axons of the ganglion cells and retinal vessels;
- Inner limiting membrane - formed by astrocytes and the end feet of the Müller cells, separates the retina from the vitreous body.
The retina receives two types of arterial blood supply. The outer five layers of the retina are avascular and receive an indirect supply from the choroidal capillaries. The inner retinal layers are supplied directly from capillaries connected arising from branches of the central retinal artery. Venous drainage follows a similar path to the arterial blood supply, with veins collecting blood from the retina draining into the central retinal vein. The retina gives rise to the optic nerve (CN II), which is formed by the axons of the ganglion cells.
Within the retina, it has characteristics that work as topographic landmarks for orientating around the retina. The two notable landmarks are the macula lutea and optic disc. The macula lutea is an oval-shaped, highly pigmented area in the center of the inner retinal layer. A few millimeters medially to the macula lutea is the optic disc - the site where the optic nerve fibers leave the retina.
Refractive media of eyeball
The refractive media of the eyeball is made up of structures that take part in focusing the ray of light onto the retina so the photoreceptors can detect them. The eye has four refractive media structures:
- Cornea (described above)
- Lens
- Vitreous body
- Aqueous humor (associated with chambers of the eye)
Lens
The lens is a double-convex, circular and transparent structure located anterior to the vitreous body and posterior to the iris. Together with the cornea, the lens transmits light rays to the retina. The lens is an encapsulated structure surrounded by the aqueous humor. It is divided into anterior and posterior surfaces by the outer margin of the lens, also known as the equator.
The lens is avascular and has no nerve fibers. No other structures are present as the lens needs to keep its transparency. The lens has three parts: lens capsule, lens epithelium, and lens fibers. The elastic capsule surrounds the outer surface of the lens. The lens epithelium lies below the capsule. The fibers of the lens are responsible for the substance of the lens. The lens is connected to the ciliary body via collection of fibers known as the suspensory ligament. It holds the lens in its place.
The majority of the lens consists of the lens fibers, which anteriorly are covered by a single layer of epithelium and are adjective by the outer lens capsule. By the ability to change its shape, the lens selectively transmits light and adjusts the focus of the eye so that a sharp image may be projected on the retina. This process is known as accommodation. The suspensory ligament of the lens takes part in changing the shape of the lens through the accommodation of the eye.
Vitreous body
The vitreous body is the largest structure of the eyeball located posterior to the lens. The vitreous body does not contain blood vessels or nerve ends. It consists of a gel-like liquid - vitreous humor - surrounded by a capsule. The vitreous body has a dense cortex but a liquid-like and looser central part.
At the margin of the optic disc, the vitreous body attaches to the neural retina. In front of the vitreous body is the hyaloid fossa (the anterior concavity), where the lens sits. The hyaloid canal, a remnant of the hyaloid arteria from the embryonic period, passes through the vitreous body.
The vitreous body or the vitreous humor has no colour, and it consists almost only of water. The water forms around 98-99% of the vitreous humor, while the rest is represented by small amounts of hyaluronic acid, glicose, ions, and collagen. The vitreous body contributes to the refraction of light, even though its dioptric index is much smaller than the cornea index and lens index.
Aqueous humor and chambers of eye
The aqueous humor is a transparent watery fluid that is produced by the ciliary body. The fluid fills and helps to form the anterior and posterior chambers of the eye. The anterior chamber is a small space found behind the cornea and anterior to the iris, a part of the ciliary body, and a small area of the anterior surface of the lens. The posterior chamber is a small space between the iris in the front, the ciliary processes surrounding it, and the lens behind it.
The aqueous humor is constantly secreted by the unpigmented epithelial cells of the ciliary processes into the posterior chamber. Further, the fluid flows between the zonular fibers, around the equator of the lens, then through the pupil and the iris into the anterior chamber. Within the anterior chamber, the aqueous humor circulates and then leaves the chamber through the iridocorneal angle in two possible ways. The first and main route is via the canal of Schlemm, while the other path - through the ciliary muscle, an alternative uveoscleral pathway.
Water makes up for approximately 99.9% of the aqueous humor, while the rest 0.01% consists of glucose, amino acids, ascorbic acid and other vitamins. The fluid is rich with nutrients and, therefore, it supplies the cornea and lens, which are avascular structures. The aqueous humor also supports the eyeball, and contributes to maintaining the intraocular pressure.
Accessory structures of eye
The accessory structures of the eye are responsible for such functions as movement of the eyeball and its protection. The accessory structures include the following:
- Eyebrows
- Eyelids and eyelashes
- Conjunctiva
- Lacrimal apparatus
- Extraocular muscles
Eyebrows
The eyebrows are areas above the eyes with short hair. They are situated at the junction of the forehead and the upper eyelid. Each eyebrow has a medial and a lateral end, with the medial end being just below the orbital margin, while the lateral end lies above the orbital margin.
The eyebrows are supplied by branches of the ophthalmic artery. Venous drainage happens through the corresponding veins. The muscles affecting the eyebrows are innervated by the facial nerve (CN VII).
Eyelids and eyelashes
The eyelids are structures working as a barrier to protect the eyes from injury and too much light. The protection is acquired by closing the eyelids. Blinking allows the eyelids to distribute the tears over the anterior surfaces of the eyeballs. Humans have upper and lower eyelids. Between the eyelids is a palpebral fissure - the space between the lateral and medial canthi.
On the edge of each eyelid are hairs known as eyelashes. They are arranged in one layer on each eyelid. The upper eyelid has approximately 90 to 150 longer eyelashes, while the lower eyelid houses around 70 to 80 shorter eyelashes. The eyelashes protect the eyes by keeping dust, dirt or other debris that is in the air from reaching the sensitive and delicate tissues of the eye.
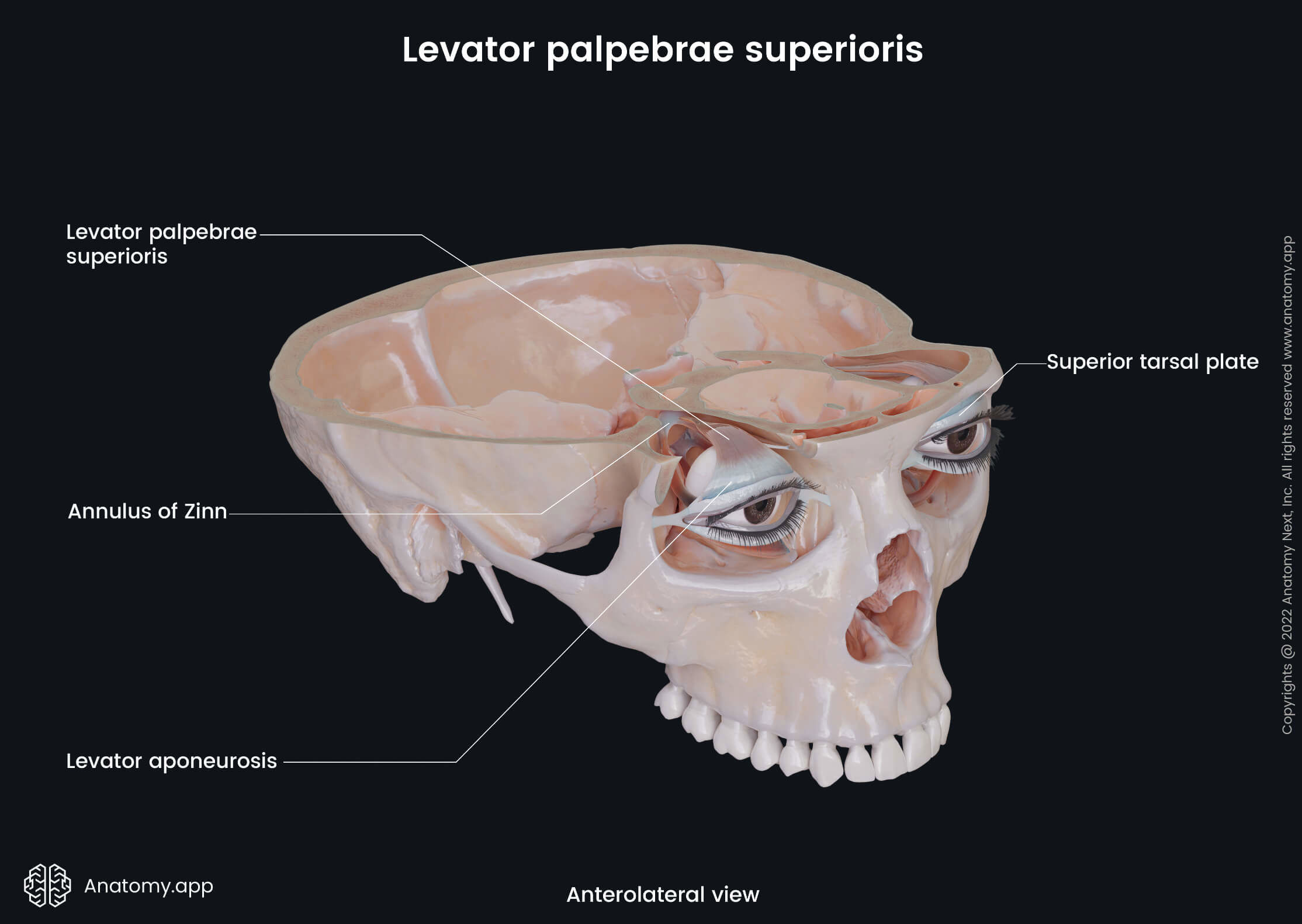
Each eyelid has two parts: orbital part and tarsal part. The division is made by a horizontal furrow called the superior palpebral sulcus. The upper eyelid is an insertion site for a powerful extraocular muscle - the levator palpebrae superioris. The eyelids have six layers (from outermost to innermost):
- Skin of the eyelids - thin and folds easily, has tiny hair with sebaceous glands and sweat glands;
- Subcutaneous tissue - loose and contains many elastic fibers;
- Muscle fibers of the orbicularis oculi - an elliptical muscle surrounding the orbital margin;
- Orbital septum - a membranous sheet forming the base of the eyelid; it attaches to the orbital margin;
- Tarsal plates - made of dense fibrous tissue and are responsible for the shape of the eyelids; contains smooth muscles -superior and inferior tarsal muscles; the superior tarsal muscle aids the levator palpebrae superioris muscle in raising the upper eyelid; the inferior tarsal muscle lowers the lower eyelid;
- Conjunctiva of the eyelid - a mucous membrane covering the inside of the eyelid (the conjunctiva also covers part of the sclera).
The eyelids receive arterial blood supply from the lateral and medial palpebral arteries. Venous drainage happens via veins that drain into the ophthalmic, angular, and superficial temporal veins. The eyelids are innervated by branches of the trigeminal nerve (CN V).
Conjunctiva
The conjunctiva is a thin mucous membrane covering the inner surface of the eyelids and the part of the sclera. It helps to lubricate the eye. The conjunctival epithelium changes into the epidermis of the skin at the eyelid's margin and into the corneal epithelium at the limbus. The conjunctiva can be divided into three parts or regions:
- Palpebral conjunctiva - the part that attaches to the posterior surfaces of the tarsal plates and lines the inner surface of the eyelids;
- Conjunctival fornices - the regions between the palpebral part and the bulbar conjunctiva;
- Bulbar conjunctiva - the part of the conjunctiva in direct contact with the eyeball; it is translucent.
The conjunctiva receives its arterial blood supply from two palpebral arches and anterior ciliary arteries. Venous drainage happens via veins running along the arteries and drain into the palpebral veins or directly into the superior and inferior ophthalmic veins. The different parts of the conjunctiva receive innervation from different branches of the trigeminal nerve (CN V).
Lacrimal apparatus
The lacrimal apparatus is a set of connected anatomical structures located within the orbit that are responsible for the production and drainage of tears.
The lacrimal apparatus includes the following structures:
Lacrimal gland
The lacrimal gland is a paired lobular gland located at the upper lateral corner of the orbit that is responsible for the production of tears. The tears protect and help to maintain the eyeball and refractive structures viable and functional. The lacrimal gland consists of orbital (larger) and palpebral (smaller) parts that are continuous posterolaterally around the concave lateral edge of the aponeurosis of the levator palpebrae superioris muscle.
The lacrimal gland has lobulated tubulo-acinar structure. The lobules are separated by loose connective tissue. The lacrimal gland receives its blood from the lacrimal artery originating from the ophthalmic artery. Venous drainage happens through the superior ophthalmic vein. The lacrimal glands are innervated by branches of the ophthalmic (CN V1), maxillary (CN V2), and facial (CN VII) nerves.
Lacrimal canaliculi
The lacrimal canaliculi are small channels between the puncta lacrimalia and the lacrimal sac that participate in the tear drainage system of the lacrimal apparatus. Each lacrimal canaliculus opens with punctum lacrimalis, an opening on the margin of each lower eyelid in the medial corner of the eye, where the drainage of tears begins. There are two lacrimal canaliculi - superior and inferior.
Lacrimal sac
The lacrimal sac is the upper dilated segment of the nasolacrimal duct that is a part of the tear drainage system of the lacrimal apparatus. The main function of the lacrimal sac is to serve as a reservoir for the overflow of tears. The lacrimal sac is supplied by branches of the ophthalmic, facial, and maxillary arteries. It is innervated by branches of the trigeminal nerve (CN V).
Nasolacrimal duct
The nasolacrimal duct is a channel that is directly continuous with the lacrimal sac and opens into the nasal cavity, forming the final part of the tear drainage system of the lacrimal apparatus. The nasolacrimal duct drains excess tears from the nasolacrimal sac into the nasal cavity, which explains the phenomenon of a running nose when a person is crying. The nasolacrimal duct is supplied by branches of the ophthalmic, facial, and maxillary arteries. It is innervated by branches of the trigeminal nerve (CN V).
Extraocular muscles
The extraocular muscles, also known as the extrinsic muscles of the eyeball, are a set of seven muscles located within each orbit and connected with the eye. There are six extraocular muscles responsible for the eye movements and one providing the elevation of the upper eyelid.
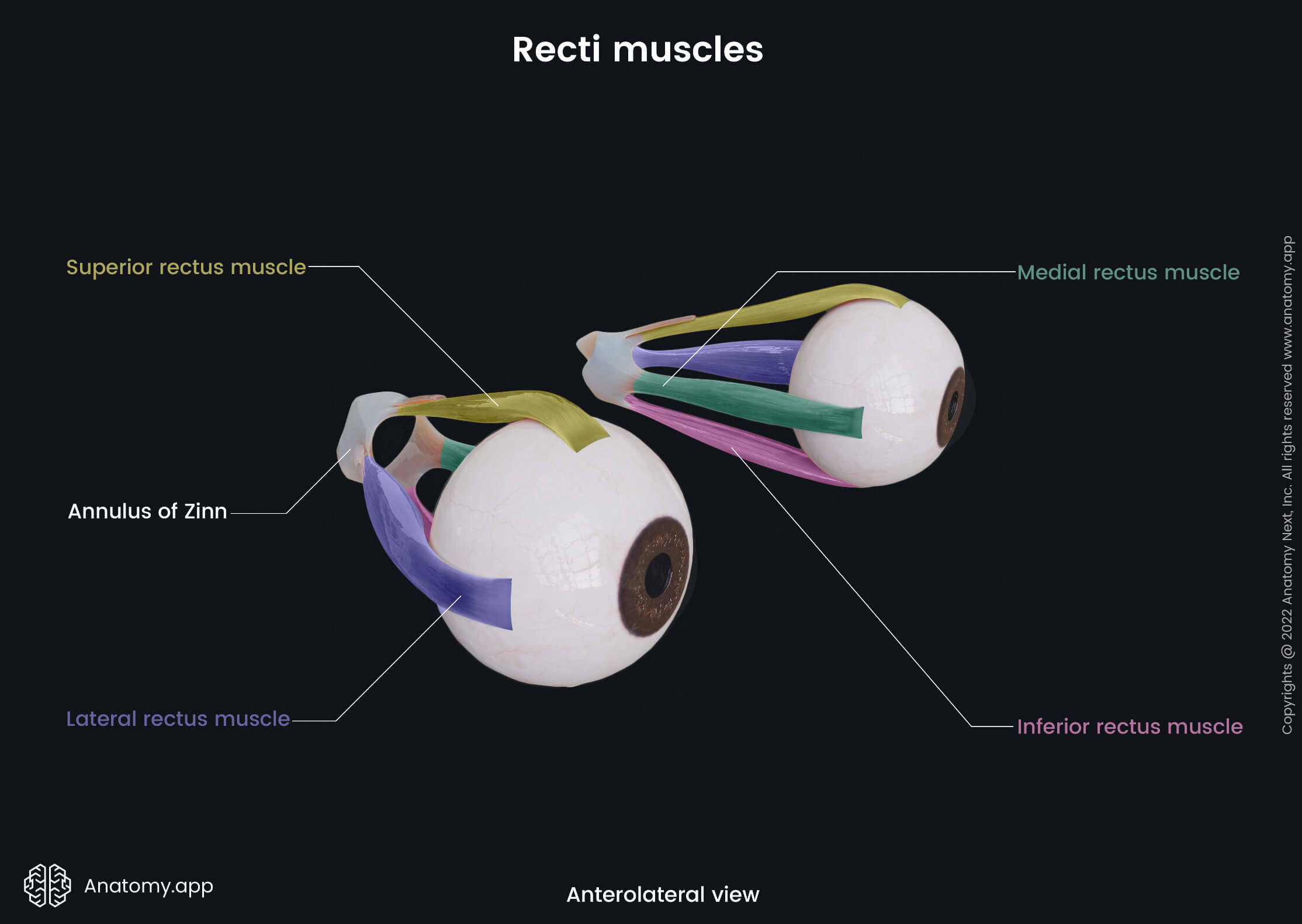
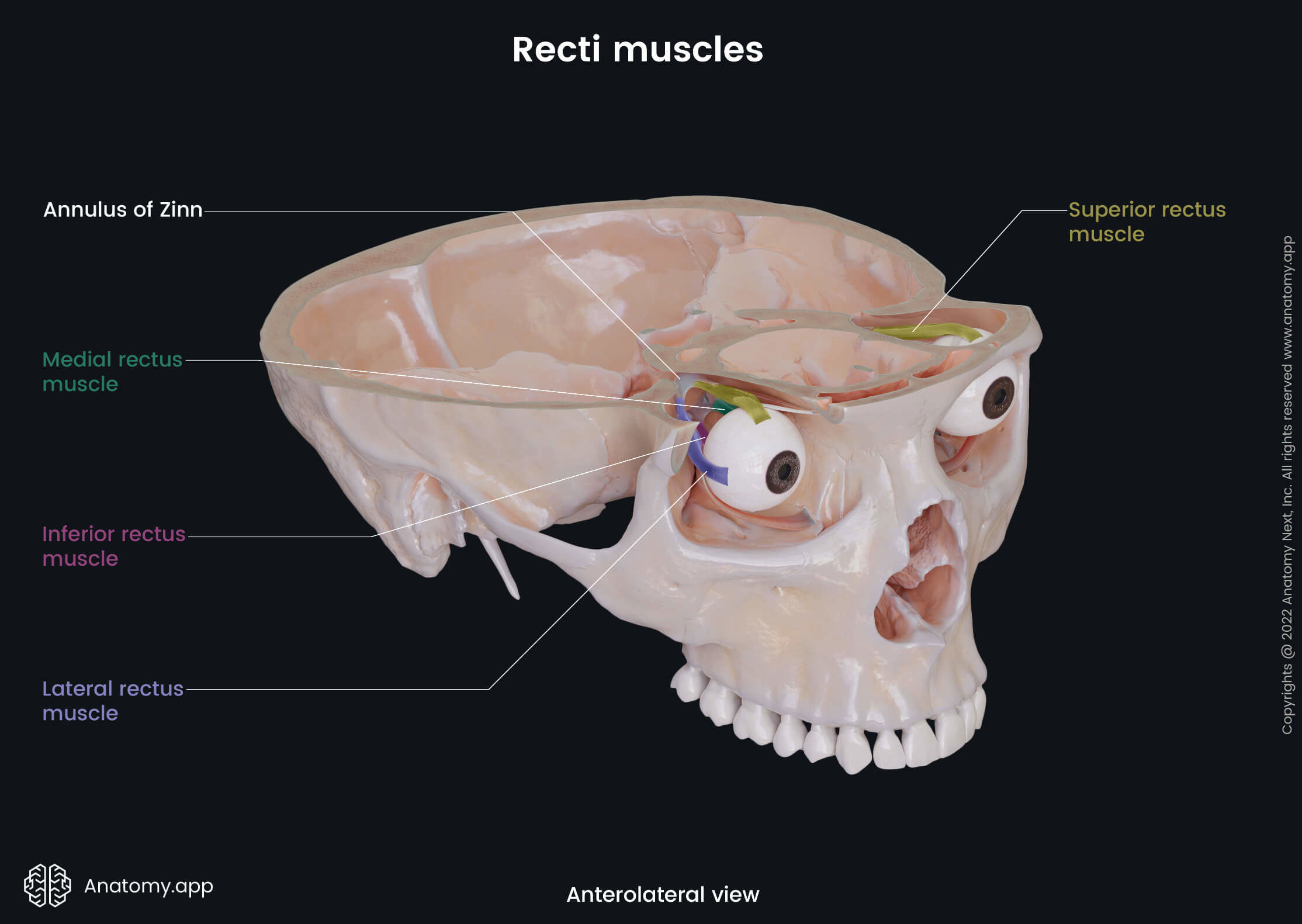
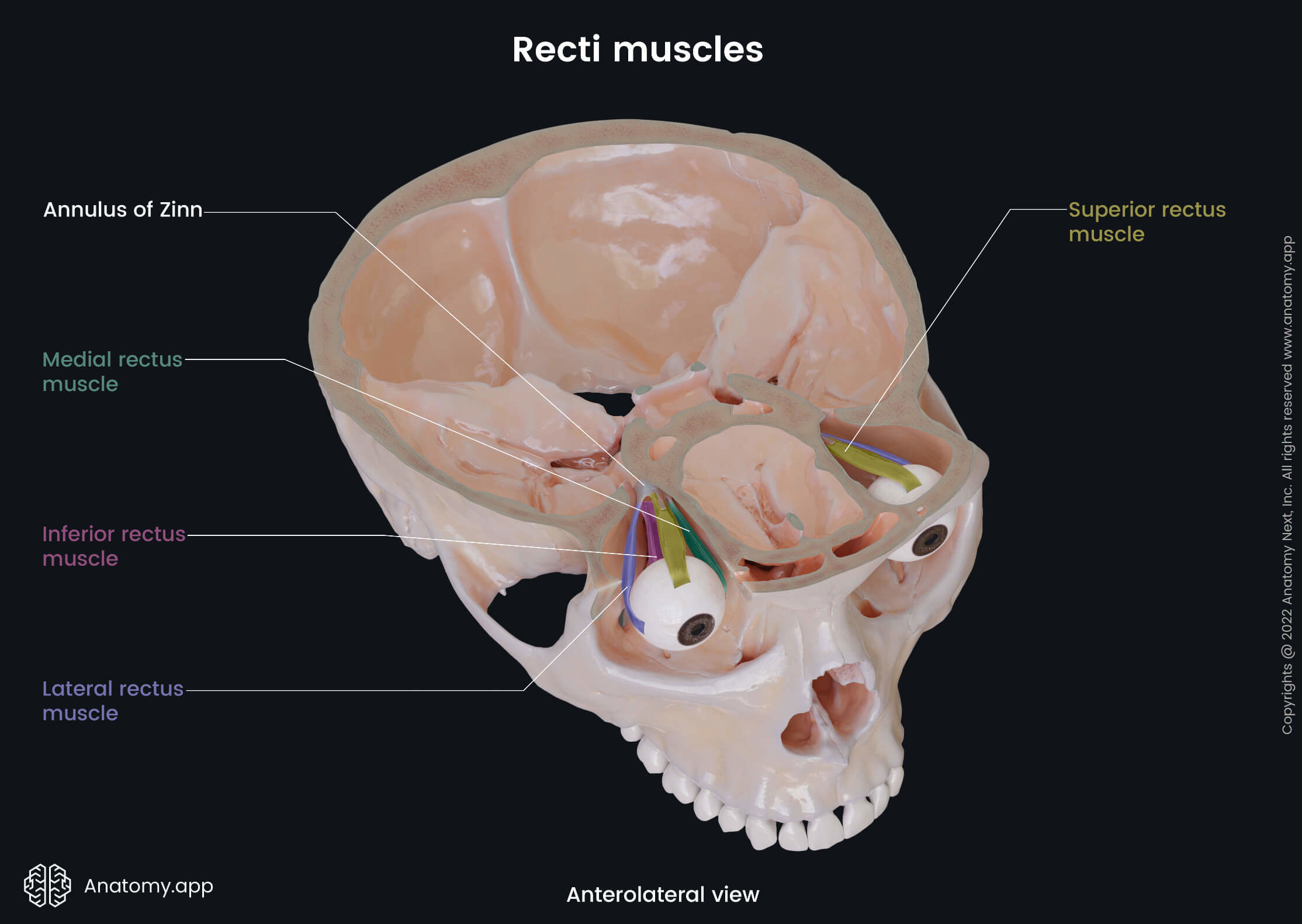
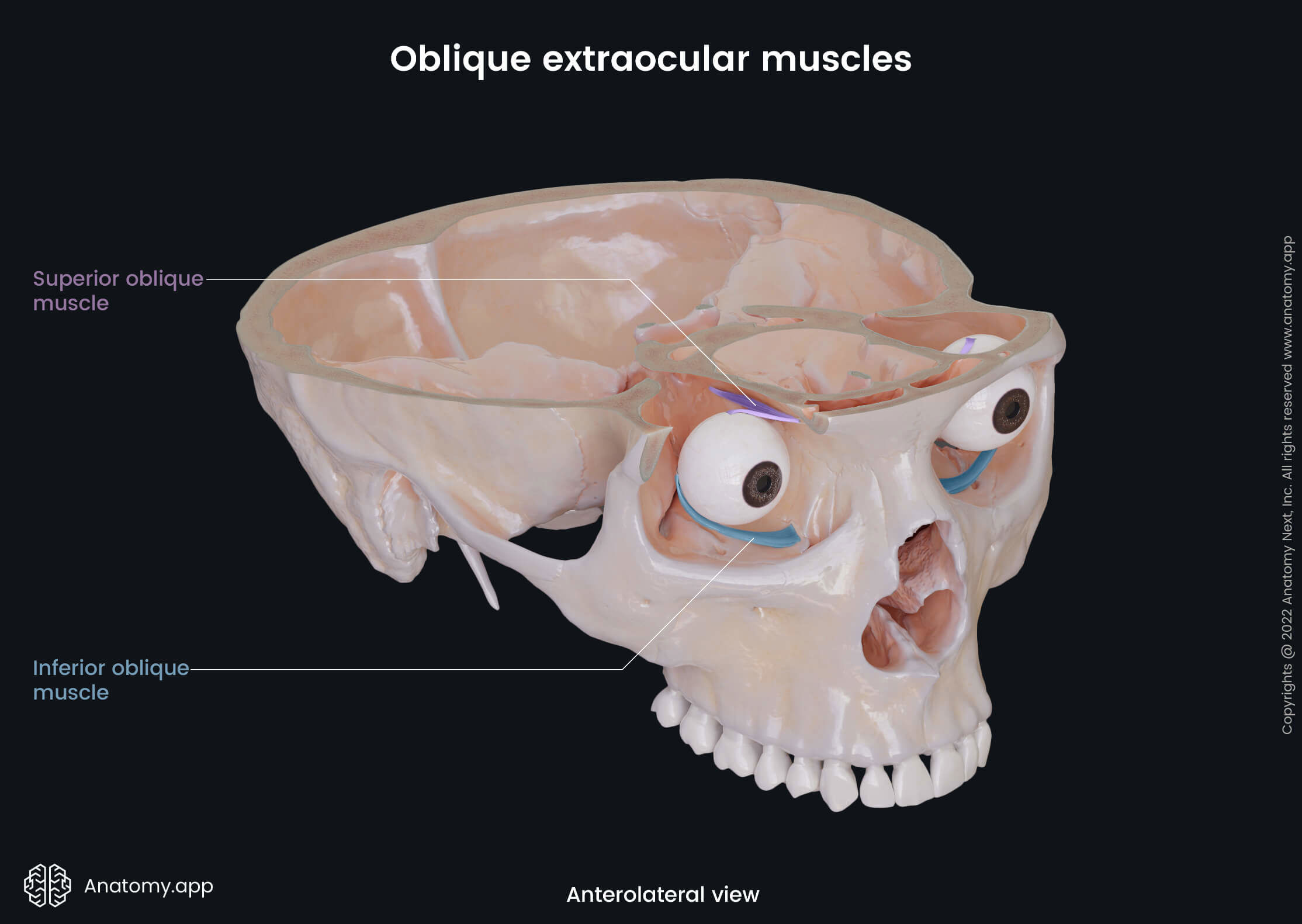
The six extraocular muscles controlling eye movements include four rectus muscles - superior rectus, inferior rectus, medial rectus, lateral rectus, and two oblique muscles - superior oblique and inferior oblique. There is the seventh extraocular muscle that provides the elevation of the upper eyelid, and that is the levator palpebrae superioris.
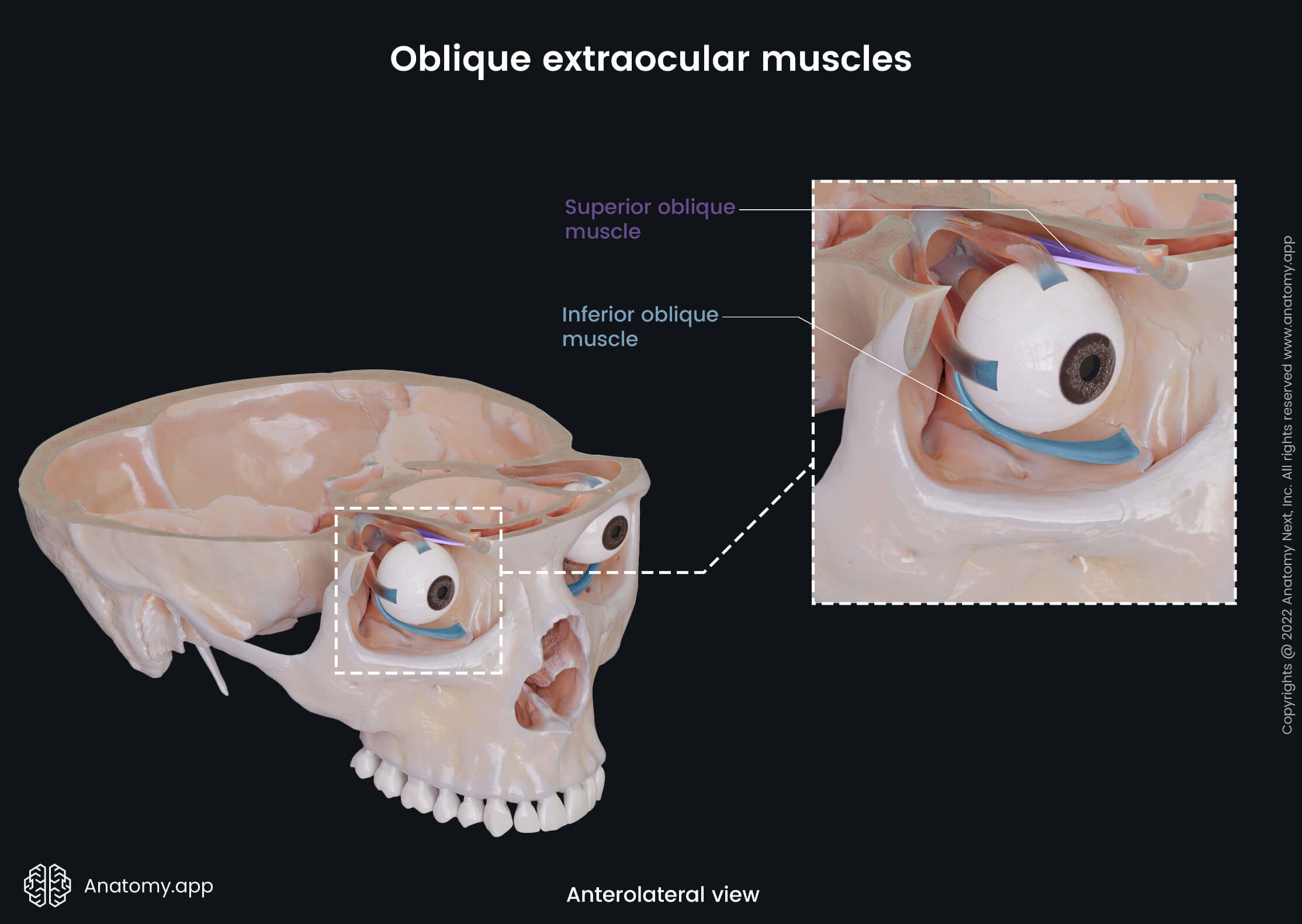
The main actions provided by each extraocular muscle are as follows:
- Superior rectus - elevation and adduction of the eyeball, and medial rotation of the eyeball;
- Inferior rectus - depression and lateral rotation of the eyeball;
- Medial rectus - turning the eyeball medially;
- Lateral rectus - turning the eyeball laterally;
- Superior oblique - intorsion (internal rotation), depression, and abduction of the eyeball;
- Inferior oblique - extortion (external rotation), elevation, and abduction of the eye;
- Levator palpebrae superioris - elevation of the upper eyelid.
The motor innervation of the extraocular muscles is provided by three cranial nerves: oculomotor (CN III), trochlear (CN IV), and abducens (CN VI) nerves. The oculomotor nerve supplies five extraocular muscles: three out of the four rectus muscles (superior, inferior, medial), inferior oblique muscle, and levator palpebrae superioris muscle. The trochlear nerve innervates only the superior oblique, while the abducens nerve supplies the lateral rectus muscle.
References:
- Bekerman, I., Gottlieb, P., & Vaiman, M. (2014). Variations in eyeball diameters of the healthy adults. Journal of ophthalmology, 2014, 503645. https://doi.org/10.1155/2014/503645
- Drake, R., Vogl, W., & Mitchell, A. (2019). Gray’s Anatomy for Students: With Student Consult Online Access (4th ed.). Elsevier.
- Gray, H., & Carter, H. (2021). Gray’s Anatomy (Leatherbound Classics) (Leatherbound Classic Collection) by F.R.S. Henry Gray (2011) Leather Bound (2010th Edition). Barnes & Noble.
- Netter, F. (2019). Atlas of Human Anatomy (7th ed.). Philadelphia, PA: Saunders.
- Snell, R. S., & Lemp, M. A. (1998). Clinical anatomy of the eye (2nd ed.). Carlton: Blackwell Science.