- Anatomical terminology
- Skeletal system
- Joints
- Muscles
- Heart
- Blood vessels
- Lymphatic system
- Nervous system
- Respiratory system
- Digestive system
- Urinary system
- Female reproductive system
- Male reproductive system
- Endocrine glands
- Eye
- Ear
Small intestine
The small intestine (Latin: intestinum tenue) or small bowel is an organ of the digestive system and a part of the gastrointestinal tract extending between the stomach and large intestine. It is a long, hollow tube-like structure located within two cavities - abdominal and pelvic.
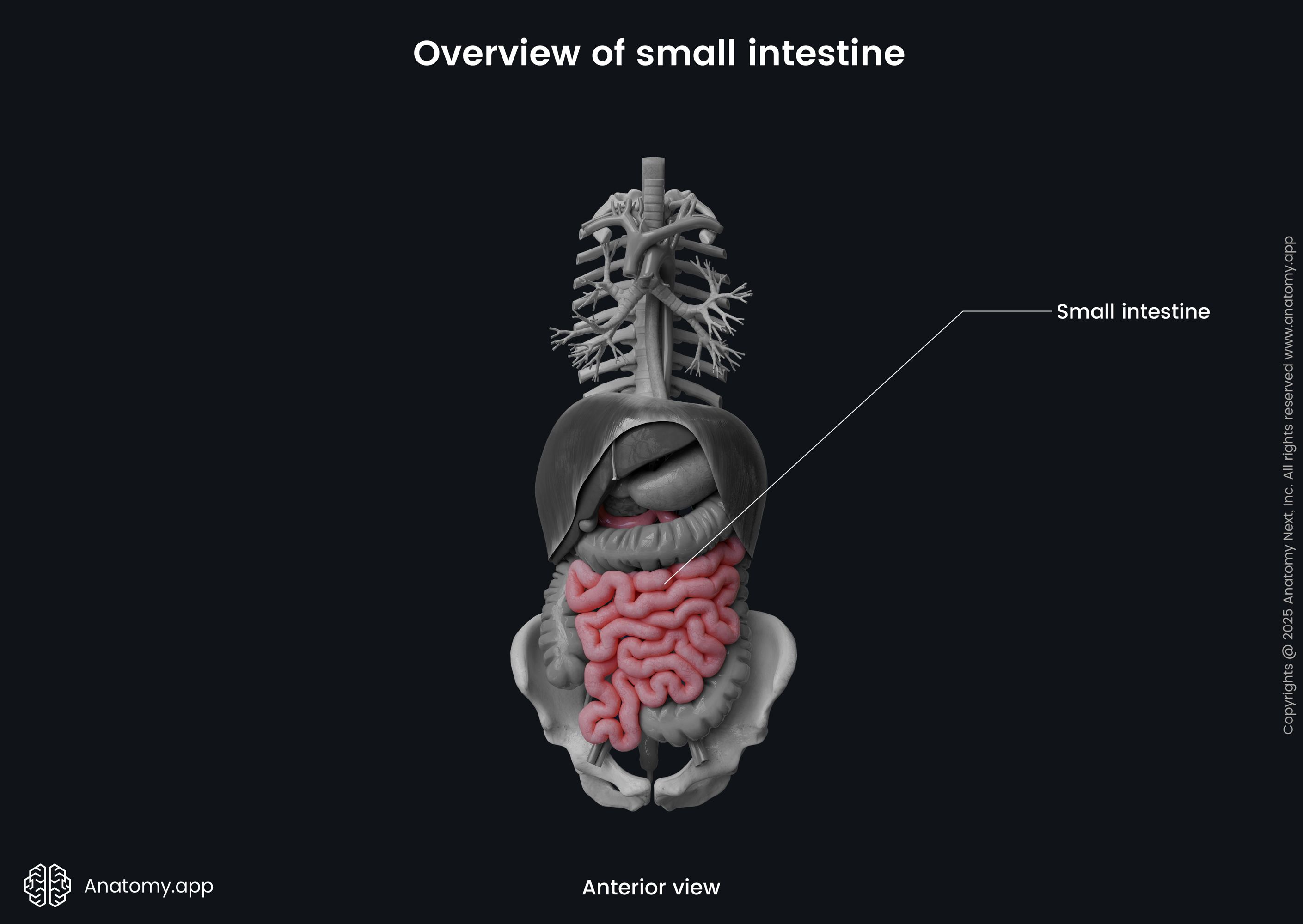
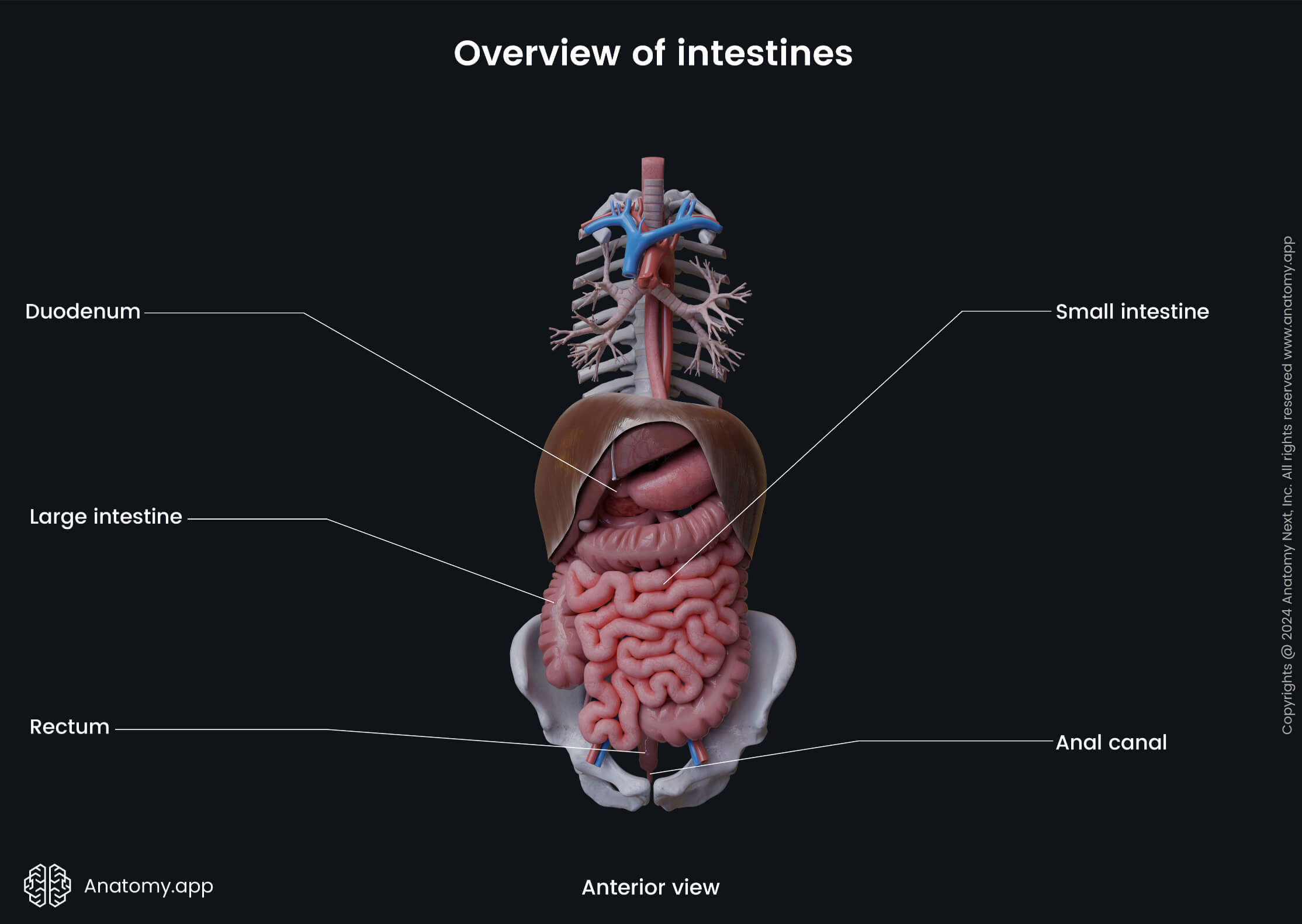
The small intestine begins at the pyloric orifice (opening) and sphincter of the stomach and terminates at the ileocecal junction with the ileocecal orifice and valve. It continues as the cecum - the first portion of the large intestine.
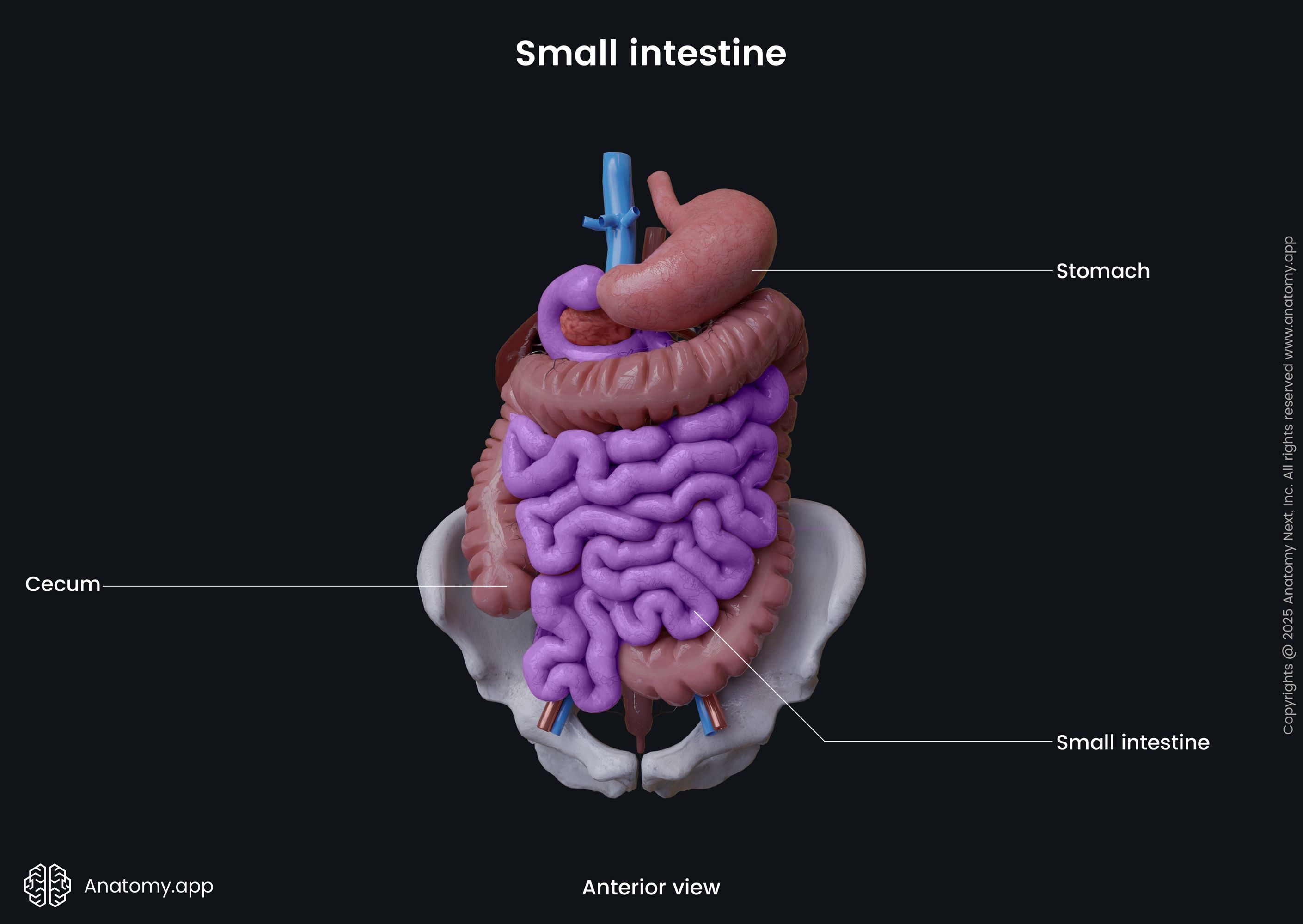
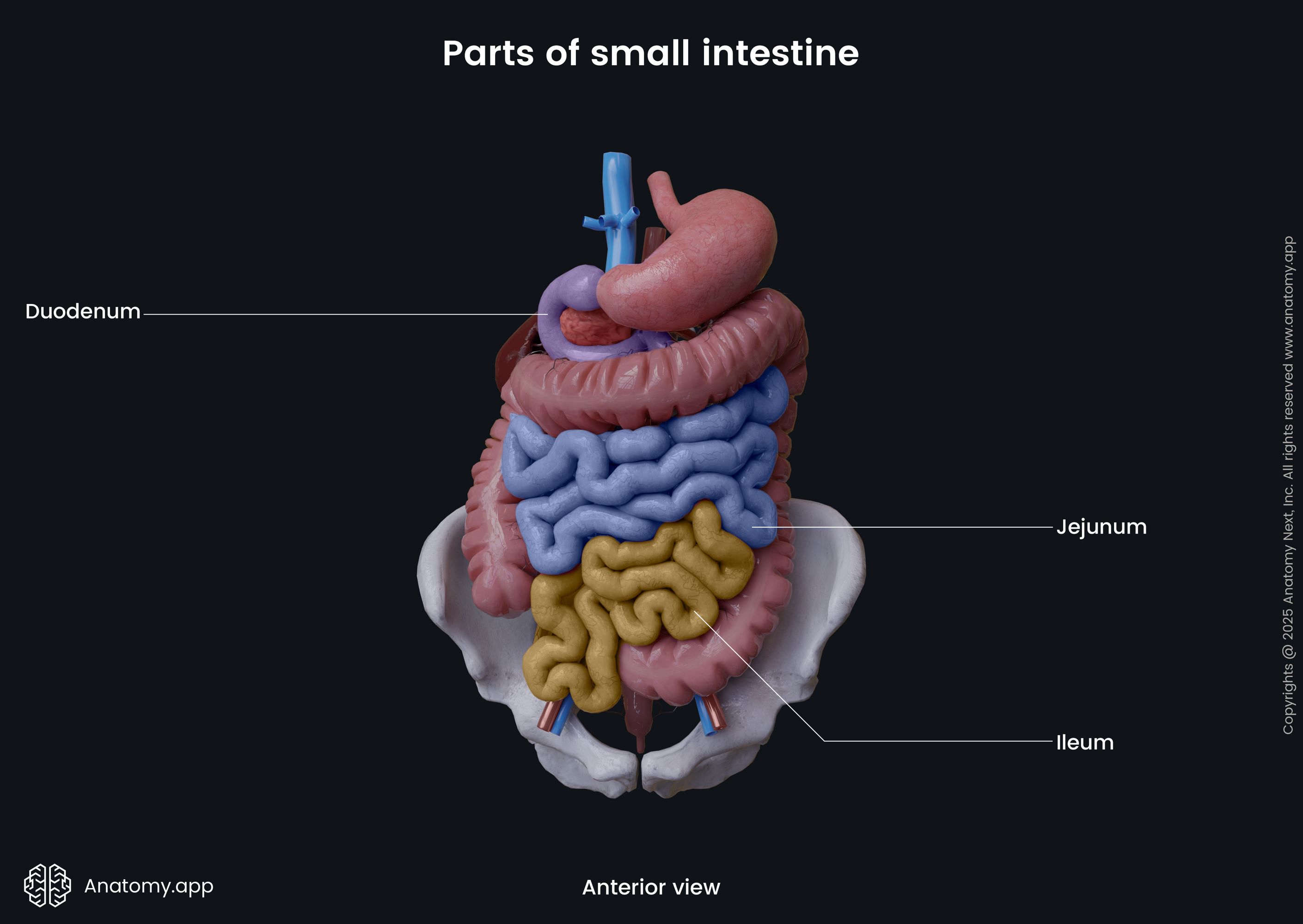
The small intestine occupies the lower abdomen and pelvis. It is composed of three parts: duodenum, jejunum and ileum. The diameter and morphology of the small intestine gradually change toward the large intestine. The duodenum is mostly located in the retroperitoneal space (anatomical space behind the peritoneum) of the abdominal cavity, but the jejunum and ileum lie intraperitoneally (within the peritoneal cavity, meaning the peritoneum covers these organs from all sides) next to the large intestine.
The small intestine is attached to the posterior abdominal wall by a membranous double fold of the peritoneum called the mesentery. This structure allows the small intestine to be relatively mobile and change its location depending on the body position. Also, the jejunum and ileum are covered by the greater omentum - an apron-like structure. The omentum is also a double fold of the peritoneum, which extends between the stomach and transverse colon, attaching them to one another.
The small intestine is the longest part of the gastrointestinal tract and can measure up to 20 - 23 feet (around 6 - 7 meters). The main functions of the small intestine include the following:
- Completion of chemical food processing and nutrient breakdown
- Nutrient and water absorption
- Secretion of hormones and intestinal juice
- Immune response providence and protection against antigens
Small intestine parts
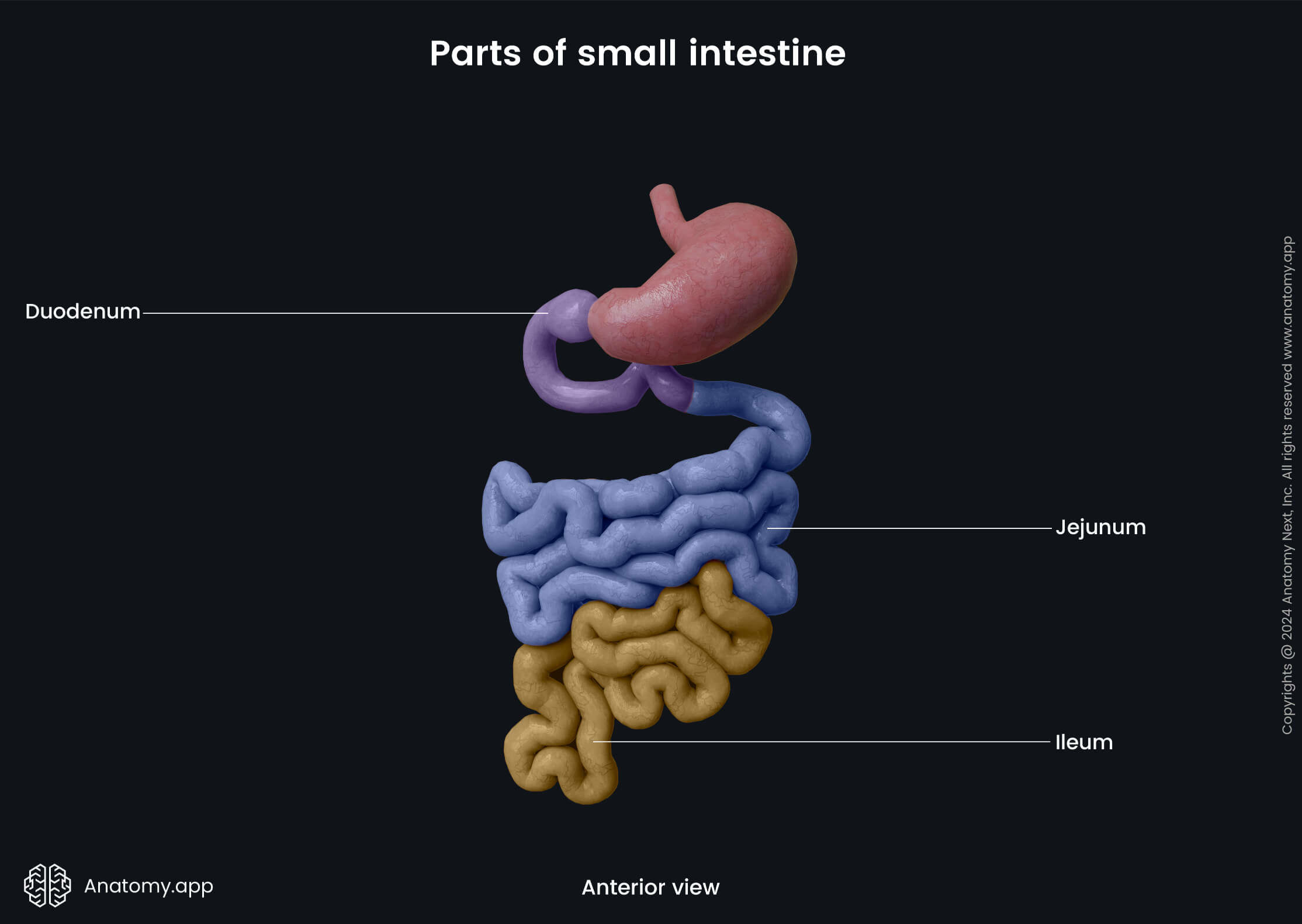
The small intestine is subdivided into three parts - duodenum, jejunum and ileum. Although there are no separation marks between all portions, they can be distinguished by their characteristics. The duodenum is the first part that links the stomach with the small intestine. It is short and has a characteristic shape.

The middle section or the jejunum forms a little bit less than half of the remaining length. It can be recognized by its wider diameter and deeper red color as it contains more blood vessels than the ileum, which is the final and longest portion of the small intestine.
Duodenum
The duodenum is the first, C-shaped part of the small intestine wrapped around the head of the pancreas. It starts at the pyloric orifice of the stomach and ends at the duodenojejunal flexure, where it transitions into the jejunum. The duodenum projects approximately at the level between the first and third lumbar vertebrae (L1 - L3) or simply above the level of the umbilicus.
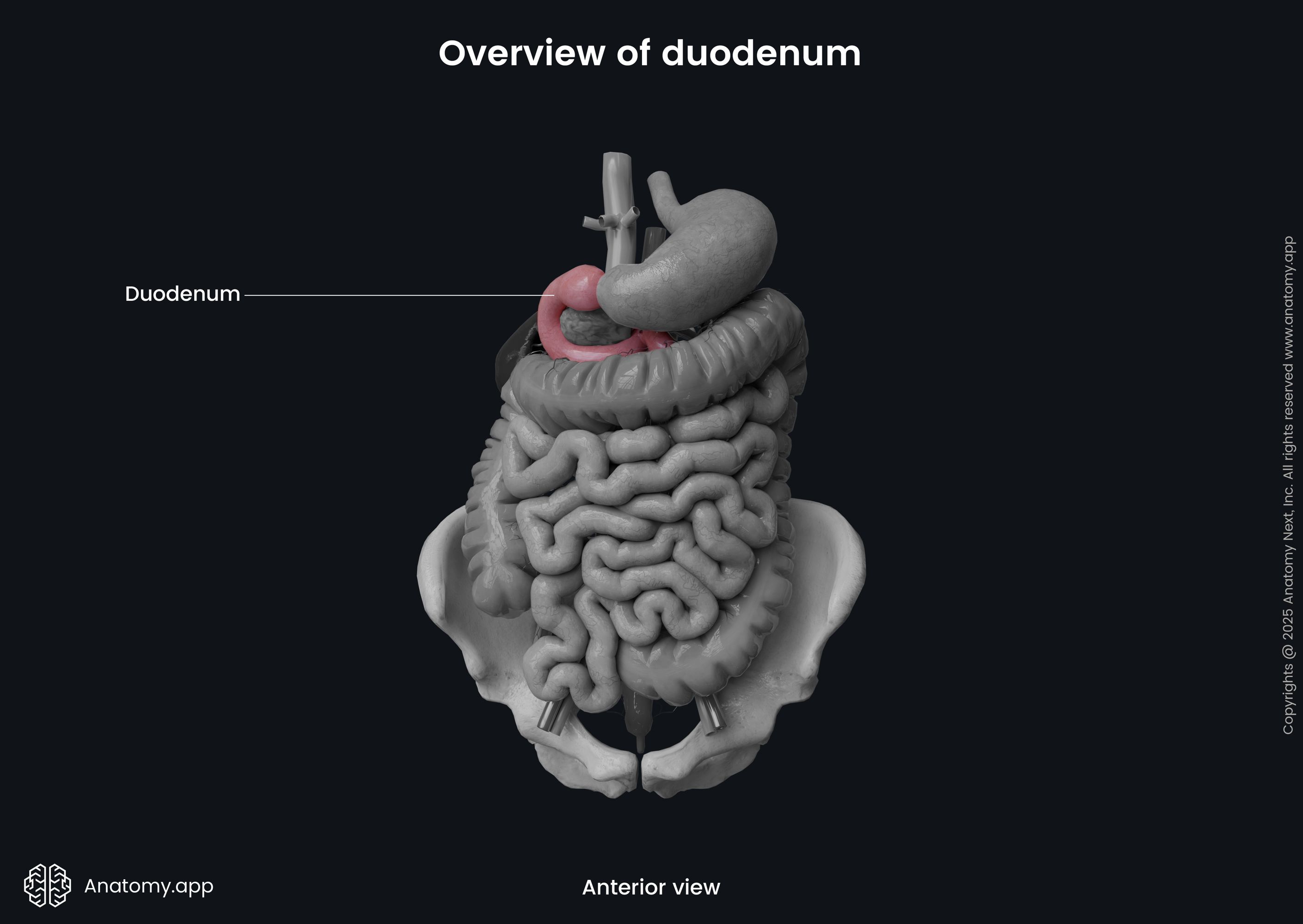
The duodenum has the widest lumen across all small intestine parts. Also, it is the shortest portion, and it is only around 10 inches (25 cm) long. The Latin word duodenum means twelve, and the name of the duodenum derives from the Latin duodenum digitorum, which stands for “twelve fingers breadth in length.”
The duodenum is mostly a retroperitoneal organ except for its initial 1 inch (2.5 cm), which is attached to the hepatoduodenal ligament (a part of the lesser omentum that connects the duodenum with the liver) above and the greater omentum below. The duodenum can be further subdivided into four parts: superior, descending, horizontal and ascending.
Jejunum
The jejunum is the middle portion of the small intestine. It continues from the duodenum at the duodenojejunal flexure that projects at the level of the second lumbar vertebra (L2).
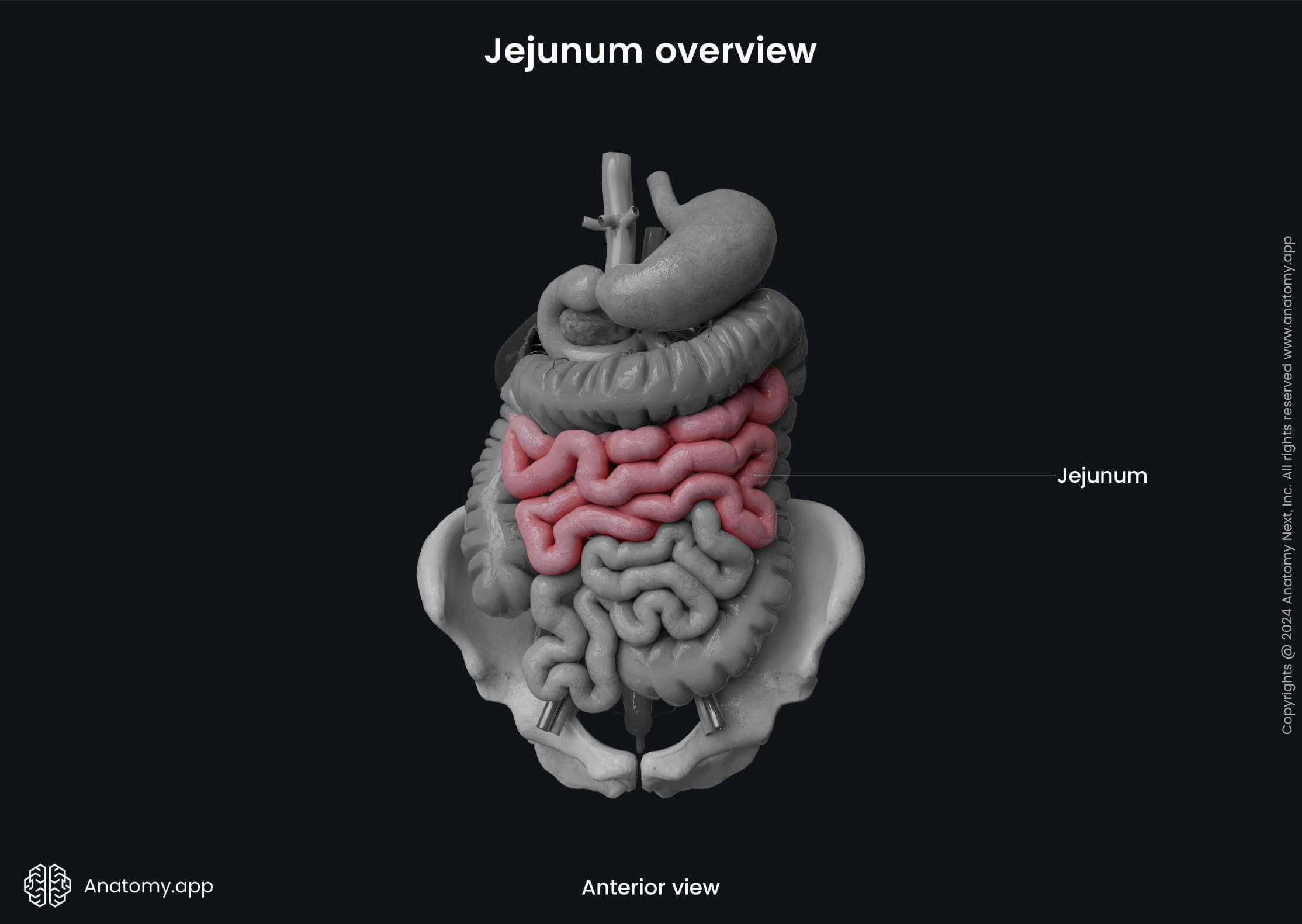
The jejunum is positioned mostly in the left upper quadrant of the abdomen. It has a larger lumen and thicker walls than the ileum. Another characteristic difference of the jejunum is its prominent circular mucosal folds called the valves of Kerckring (plicae circulares or circular folds) that encircle the lumen.
The plicae circulares are more pronounced and numerous in the proximal jejunum and become fewer and lower towards the ileum and almost disappear at its terminal portion. Another significant characteristic of the jejunum is a more vascular wall and longer vasa recta (straight arteries).
There is no distinct border between the jejunum and ileum. To recognize both parts of the small intestine, one needs to know the differences described above. The jejunum makes up around two-fifths, and the ileum forms three-fifths of the remaining length of the small intestine.
Ileum
The ileum takes up the distal three-fifths of the small intestine and is located mainly in the right lower quadrant of the abdomen. The ileum has a relatively narrow lumen, and it is the smallest of all small intestine parts. It also has thinner walls, less prominent and fewer circular folds and shorter vasa recta than the jejunum. The most distal portion of the ileum, known as the terminal ileum, contains only a few circular folds and may appear flat.
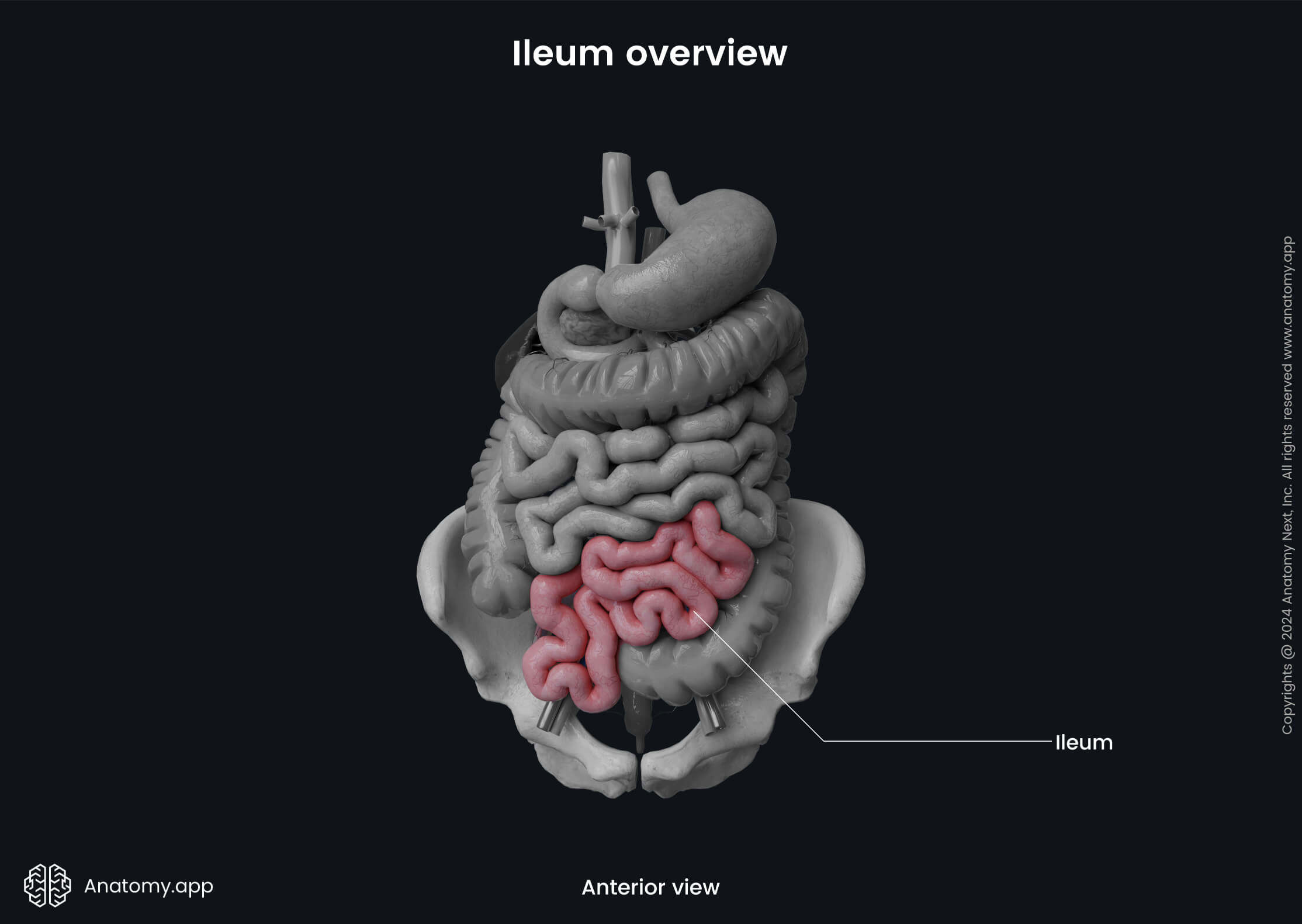
The ileum ends at the ileocecal junction with an ileocecal orifice and valve that separate it from the cecum - the first portion of the large intestine. The ileocecal valve has two flaps or lips that surround the ileocecal opening. The muscle cells of the ileal wall extend into each flap and form a sphincter. Therefore, the ileocecal valve is a functional valve that ensures the intestinal content passage from the ileum to the cecum, preventing content reflux the other way.
Small intestine histology
The wall of the small intestine is formed by four layers:
- Mucosa
- Submucosa
- Muscularis externa
- Serosa
Mucosa
The mucosa or mucosal layer faces the lumen of the small intestine and is in direct contact with its contents. It is composed of three sublayers:
- Epithelium
- Lamina propria
- Muscularis mucosae
The intestinal mucosa is lined by a simple columnar epithelium. The epithelium mainly consists of two types of cells - enterocytes and goblet cells. The enterocytes are columnar intestinal epithelial cells that primarily provide absorptive function. In contrast, the goblet cells produce and secrete mucus that helps to protect the intestine against pathogens and toxins. Also, mucus ensures lubrication and mechanical protection against intestinal contents. Besides epithelial and goblet cells, the epithelium also contains endocrine cells that produce hormones.
Beneath the epithelium is a layer called lamina propria. It is composed of loose connective tissue that supports the epithelial cells. The lamina propria of the small intestine is highly vascular, and it contains many cells, such as the fibroblasts, macrophages, plasmocytes, lymphocytes and many others to follow.
Also, the lamina propria includes a network of lymphoid cell aggregates and tissue called MALT (mucosa-associated lymphoid tissue). MALT presents with lymphoid follicles containing B and T lymphocytes, as well as macrophages. The lymphoid tissue becomes more prominent and more in number towards the ileum. The mucosa of the ileum presents with large aggregated lymphoid follicles that are large enough to be visible to the naked eye, and they are called Peyer’s patches (NOTE: Peyer’s patches are found only in the ileum).
The muscularis mucosae is the muscular layer of the mucosa formed by the smooth muscle cells, and it is situated at the base of the mucosal layer. The mucosa of the small intestine forms finger-like projections called villi. The villi are essential structures as they significantly increase the absorption area of the intestinal wall. The intestinal villi are more numerous and larger in the proximal part of the small intestine (duodenum and jejunum), while the ileum has fewer and smaller villi. The apical ends of the enterocytes are covered by other projections - microvilli. The microvilli appear as small hair-like filaments that also increase the absorption area.
Together with the submucosal layer, the mucosa forms circular mucosal folds called the circular folds (or plicae circulares, or valves of Kerckring) that encircle the lumen of the small intestine and project into it. Like the villi and microvilli, the circular folds also increase the surface area of the small intestine, thus providing the digestion and absorption of nutrients more efficiently. The circular folds are more prominent in the proximal part of the small intestine but become progressively less pronounced distally and may even be absent in the terminal ileum.
Another unique characteristic of the intestinal architecture is the presence of the intestinal glands (also called intestinal crypts or crypts of Lieberkühn). They are located at the bases of two adjacent villi, and they appear as mucosal pits. These glands are simple tubular glands that contain enterocytes, Goblet cells, highly specialized Paneth cells (provide an immune response and produce antibacterial substances), epithelial stem cells and neuroendocrine cells (secreting, for example, cholecystokinin). Intestinal gland cells form an alkaline fluid that dilutes chyme, thus promoting absorption.
Note: Chyme is a thick semi-fluid mass of partly digested food that is mainly mixed with gastric juice and expelled by the stomach into the duodenum.
Submucosa
The submucosa (submucosal layer) is made of loose connective tissue, and it contains blood and lymph vessels and nerve fibers. A specific characteristic of the duodenal submucosa is the presence of the submucosal glands (also called Brunner’s glands). They are branched tubular glands that secrete mucus with an alkaline pH, and the mucus neutralizes the acidic chyme coming from the stomach. Therefore, these glands are more prominent and numerous near the pylorus of the stomach and in the proximal half of the descending duodenum. Within the submucosa is located the submucosal nerve plexus which is called the Meissner’s plexus.
Muscularis externa
The muscularis externa (also called muscularis propria) lies beneath the submucosa, and it consists of two distinct smooth muscle layers. The inner layer is the circular layer, and the outer is the longitudinal layer. The muscularis externa is thicker in the proximal part of the small intestine, gradually becoming thinner towards its distal end. Between both layers is situated the myenteric nerve plexus - the Auerbach’s plexus.
Serosa
The serosa or serous membrane is the outermost layer of the intestinal wall and it is formed by the visceral peritoneum. The serosa is composed of two sublayers: mesothelium, which refers to the simple squamous epithelium, and loose connective tissue beneath it.
Neurovascular supply of small intestine
Arterial blood supply
The arterial blood supply to the small intestine is provided by branches of the celiac trunk and the superior mesenteric artery. The superior and descending parts of the duodenum until the major duodenal papilla are supplied by branches of the celiac trunk. In contrast, the duodenum distal to the major duodenal papilla, jejunum and ileum receive arterial blood from branches of the superior mesenteric artery.
The main arterial supply to the duodenum is ensured by two superior (anterior and posterior) and two inferior (anterior and posterior) pancreaticoduodenal arteries. The superior anterior and posterior pancreaticoduodenal arteries arise from the gastroduodenal artery (a branch of the common hepatic artery that originates from the celiac trunk), and they supply the superior and descending parts (till the major duodenal papilla) of the duodenum. The inferior anterior and posterior pancreaticoduodenal arteries are branches of the superior mesenteric artery, and they supply the remaining descending part, horizontal and ascending portions of the duodenum.
The jejunum and ileum are supplied by the branches of the superior mesenteric artery. The superior mesenteric artery enters the mesentery of the small intestine and gives off numerous jejunal and ileal arteries.
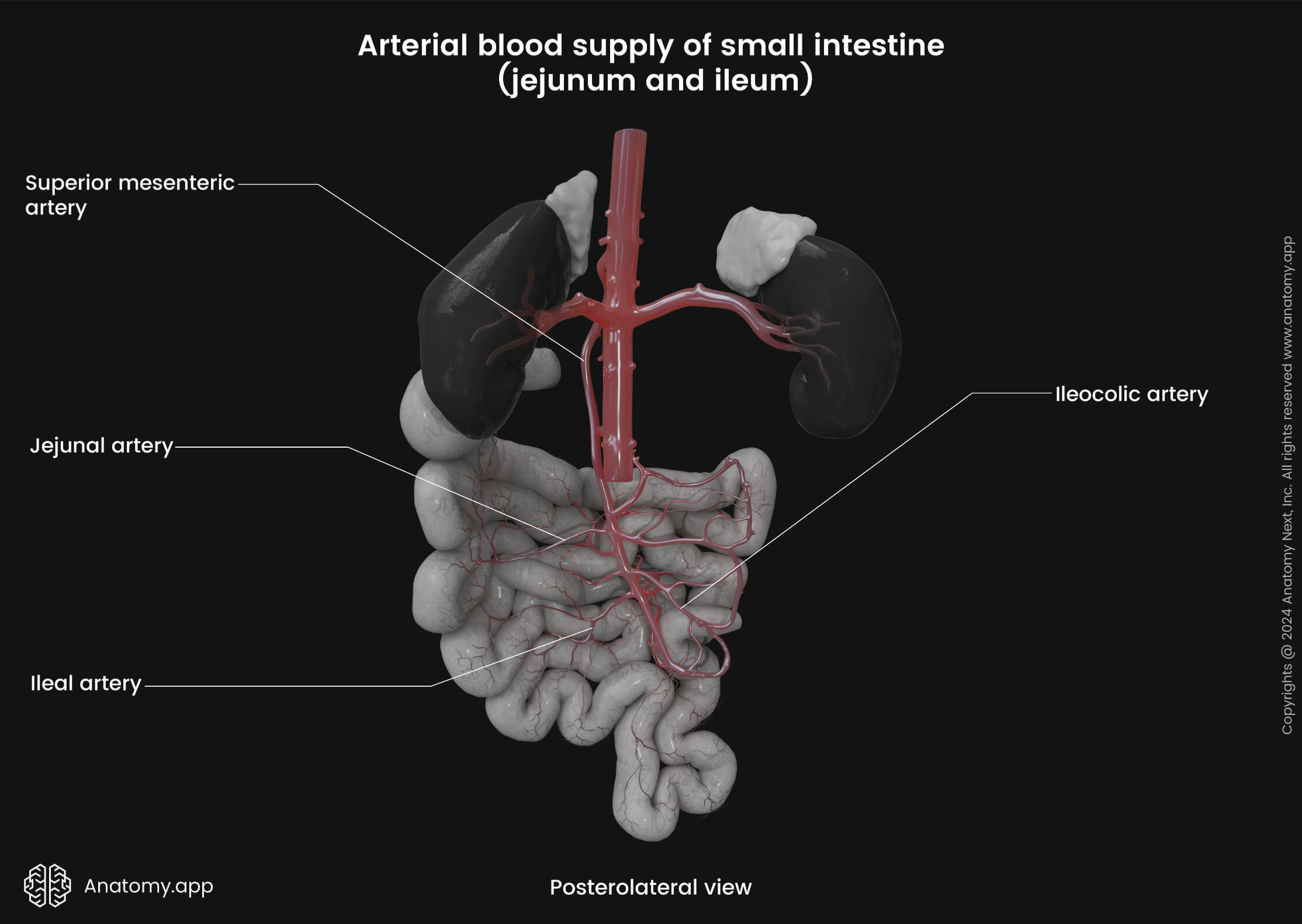
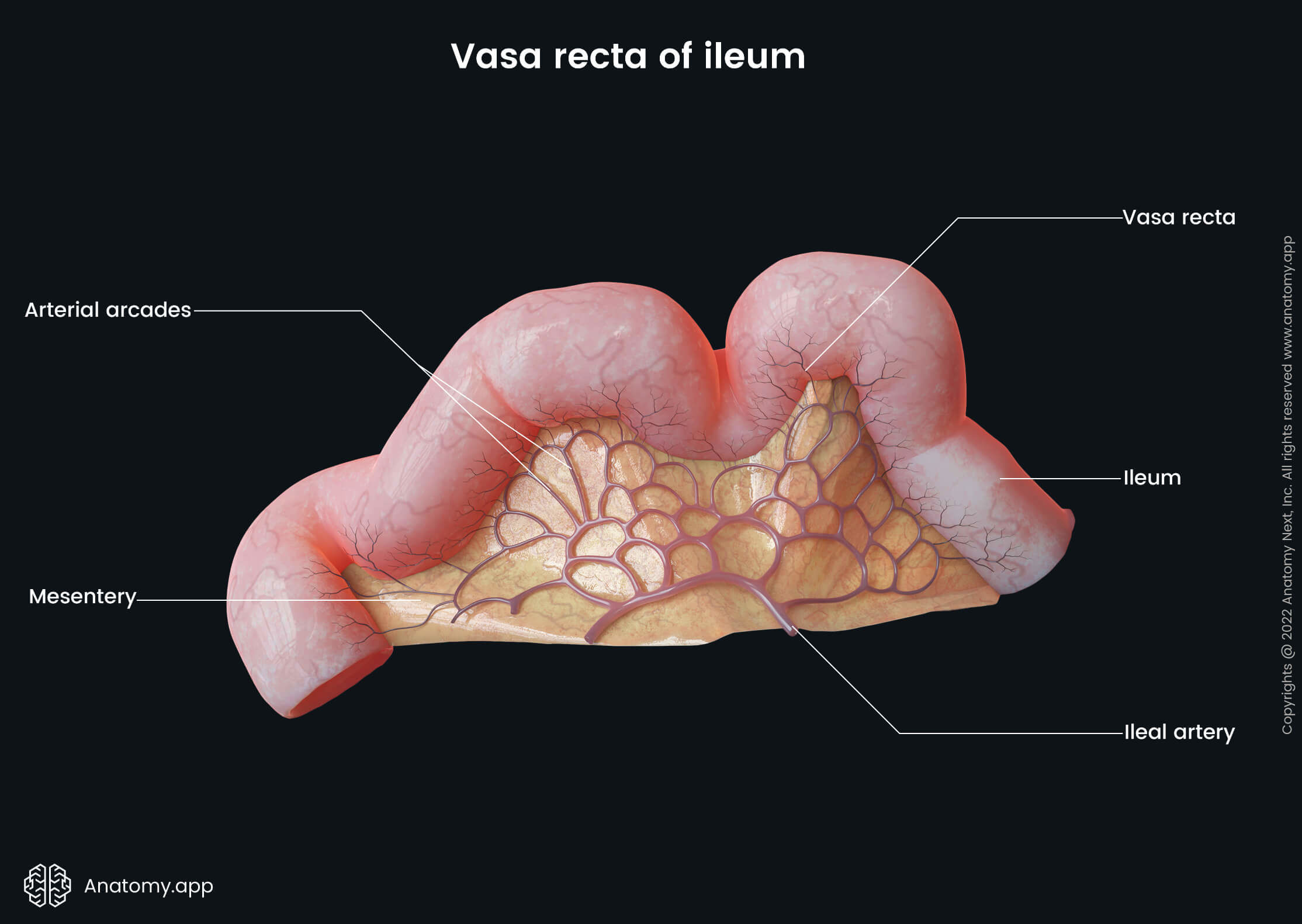
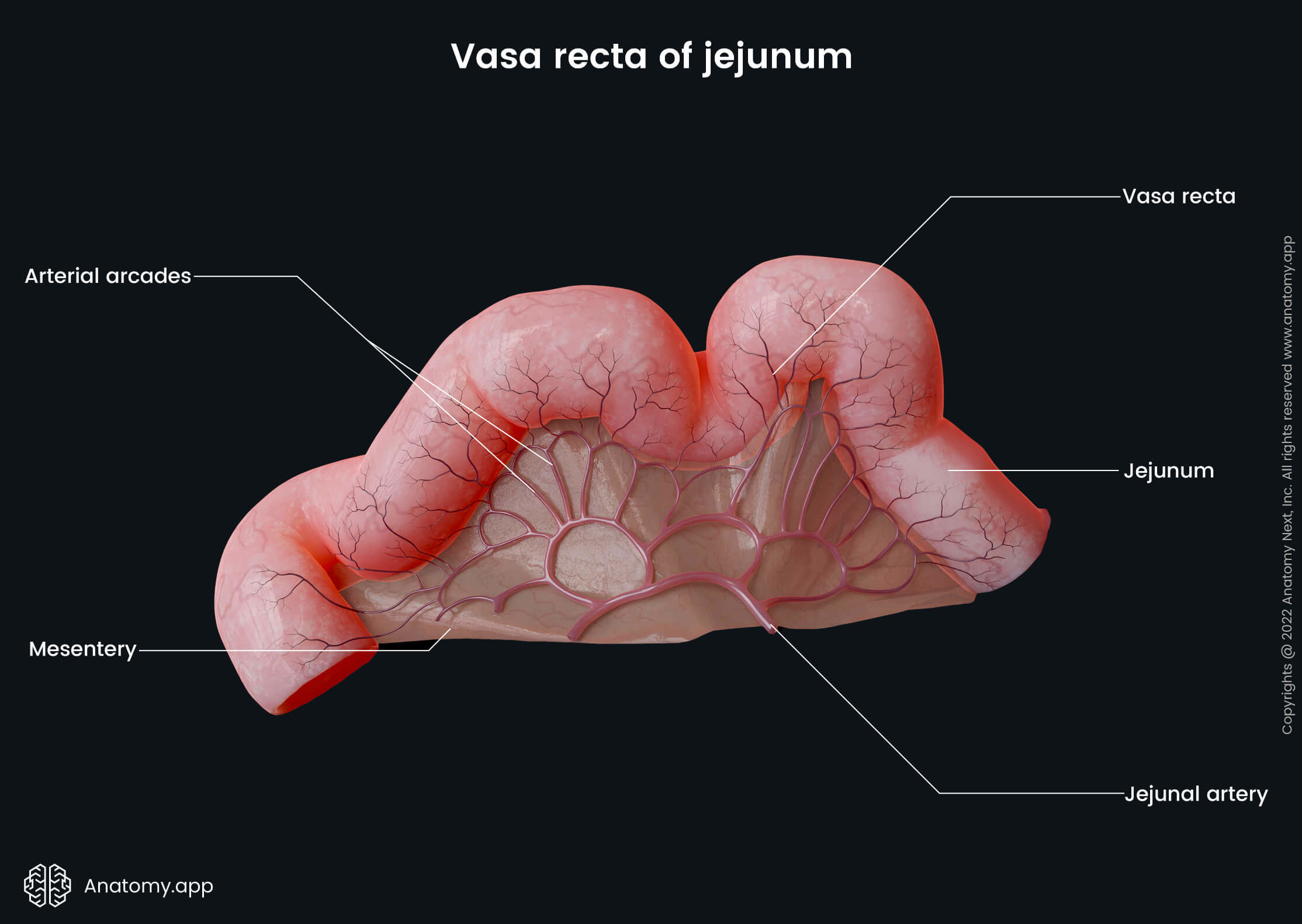
The jejunal and ileal arteries anastomose and form many arterial loops called the arcades. The arcades give off straight arteries that go within the mesentery towards the coils of the small intestine. These straight arteries are known as the vasa recta. Also, the terminal ileum receives arterial supply from another branch of the superior mesenteric artery - the ileocolic artery.
Venous drainage
The venous drainage of the small intestine is provided by the portal venous system. The venous drainage of the duodenum occurs via small duodenal veins that carry venous blood further to the superior and inferior pancreaticoduodenal veins that follow the corresponding arteries and either directly or indirectly drain into the hepatic portal vein.
Each person has four pancreaticoduodenal veins - anterior superior pancreaticoduodenal vein, posterior superior pancreaticoduodenal vein, anterior inferior pancreaticoduodenal vein and posterior inferior pancreaticoduodenal vein. The posterior superior pancreaticoduodenal vein drains into the hepatic portal vein, while the anterior superior pancreaticoduodenal vein flows into the gastrocolic trunk or the right gastro-omental vein. The posterior and anterior inferior pancreaticoduodenal veins drain into the superior mesenteric vein or its first jejunal tributary.
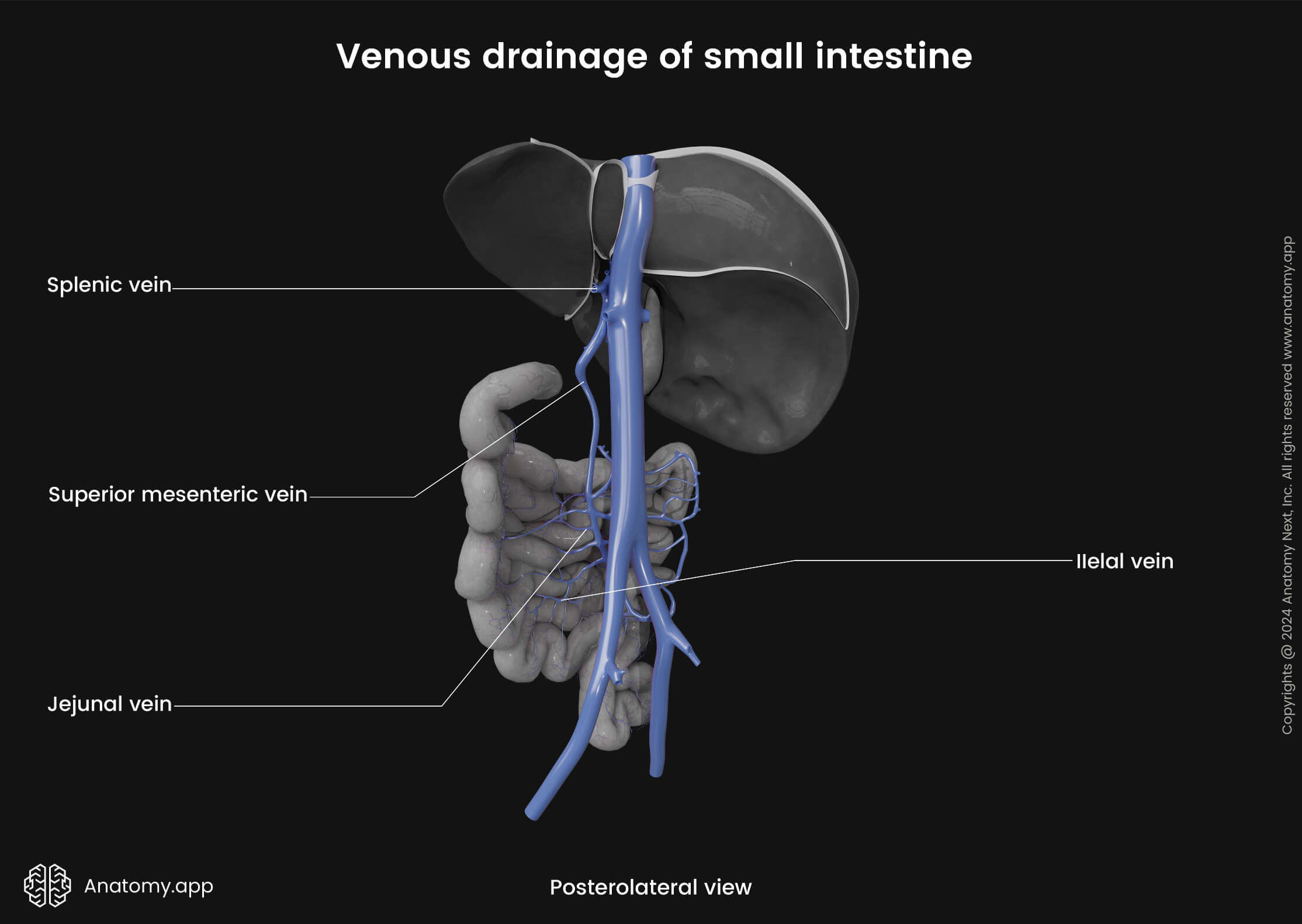
Venous drainage of the jejunum and ileum occurs through small jejunal and ileal veins that carry blood to the superior mesenteric vein that further drains into the hepatic portal vein. The superior mesenteric vein drains some parts of the stomach and greater omentum, small intestine, cecum, ascending colon and transverse colon. It is formed mainly by the tributaries running from the terminal ileum, cecum and vermiform appendix. After merging with the splenic vein behind the head of the pancreas, the superior mesenteric vein drains into the hepatic portal vein.
Innervation
The small intestine receives sympathetic and parasympathetic innervation. The sympathetic innervation occurs via the greater (duodenum) and lesser (jejunum and ileum) thoracic splanchnic nerves that participate in the formation of the superior mesenteric plexus around the superior mesenteric artery and celiac plexus around the celiac trunk. The sympathetic fibers ensure vasoconstriction (narrowing of the lumen of blood vessels) of the intestinal blood vessels, relaxation of smooth muscle cells and inhibition of intestinal gland secretion.
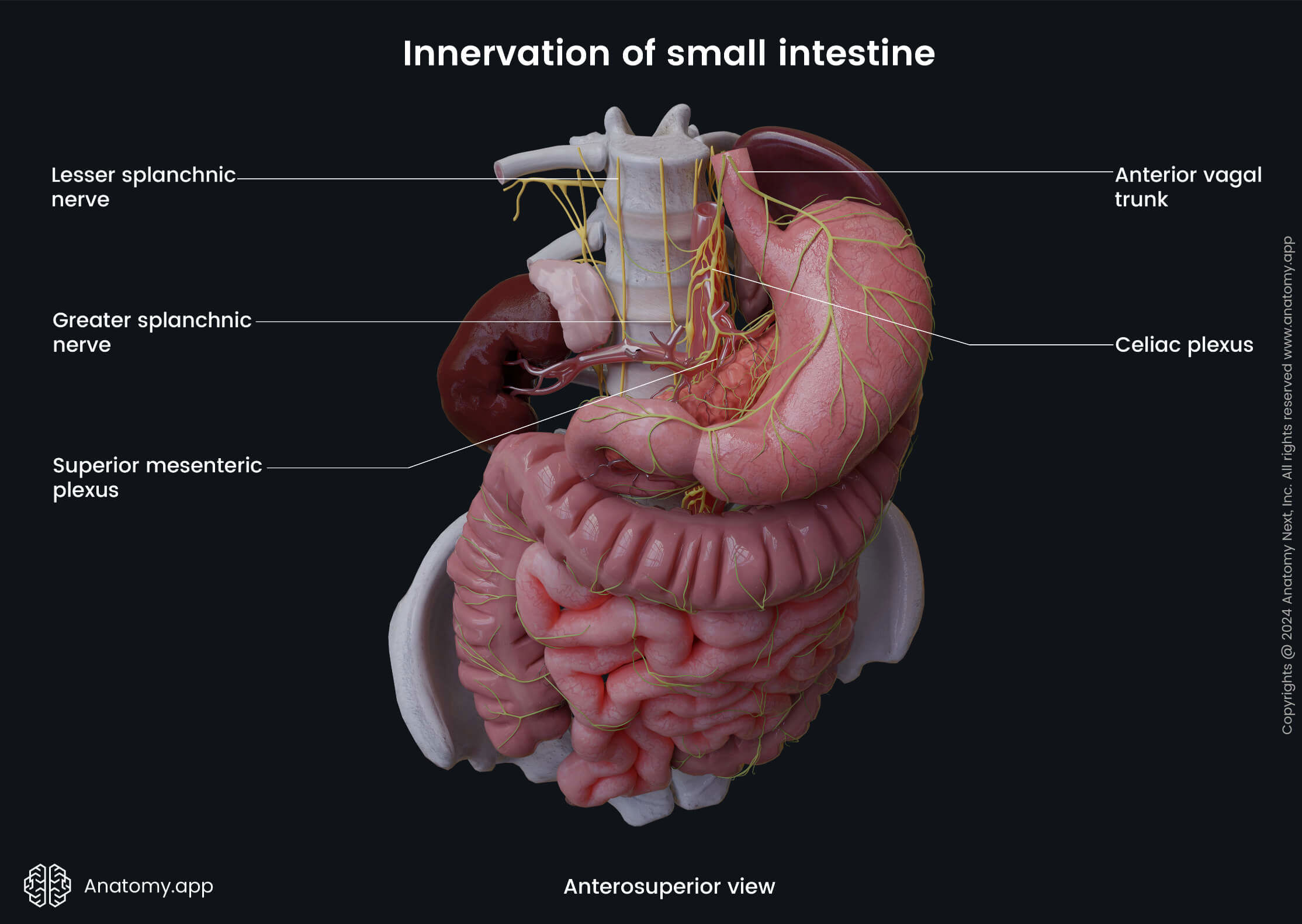
The bodies of the preganglionic sympathetic neurons are located in the gray matter of the fifth to tenth thoracic segments (duodenum: T5 - T9, jejunum and ileum: T9 - T10) of the spinal cord. Axons of these neurons form the greater and lesser thoracic splanchnic nerves that travel to the celiac and superior mesenteric plexuses and synapse there with the neurons of the celiac and superior mesenteric ganglia. Postganglionic axons then travel to the small intestine via the periarterial branches and supply it.
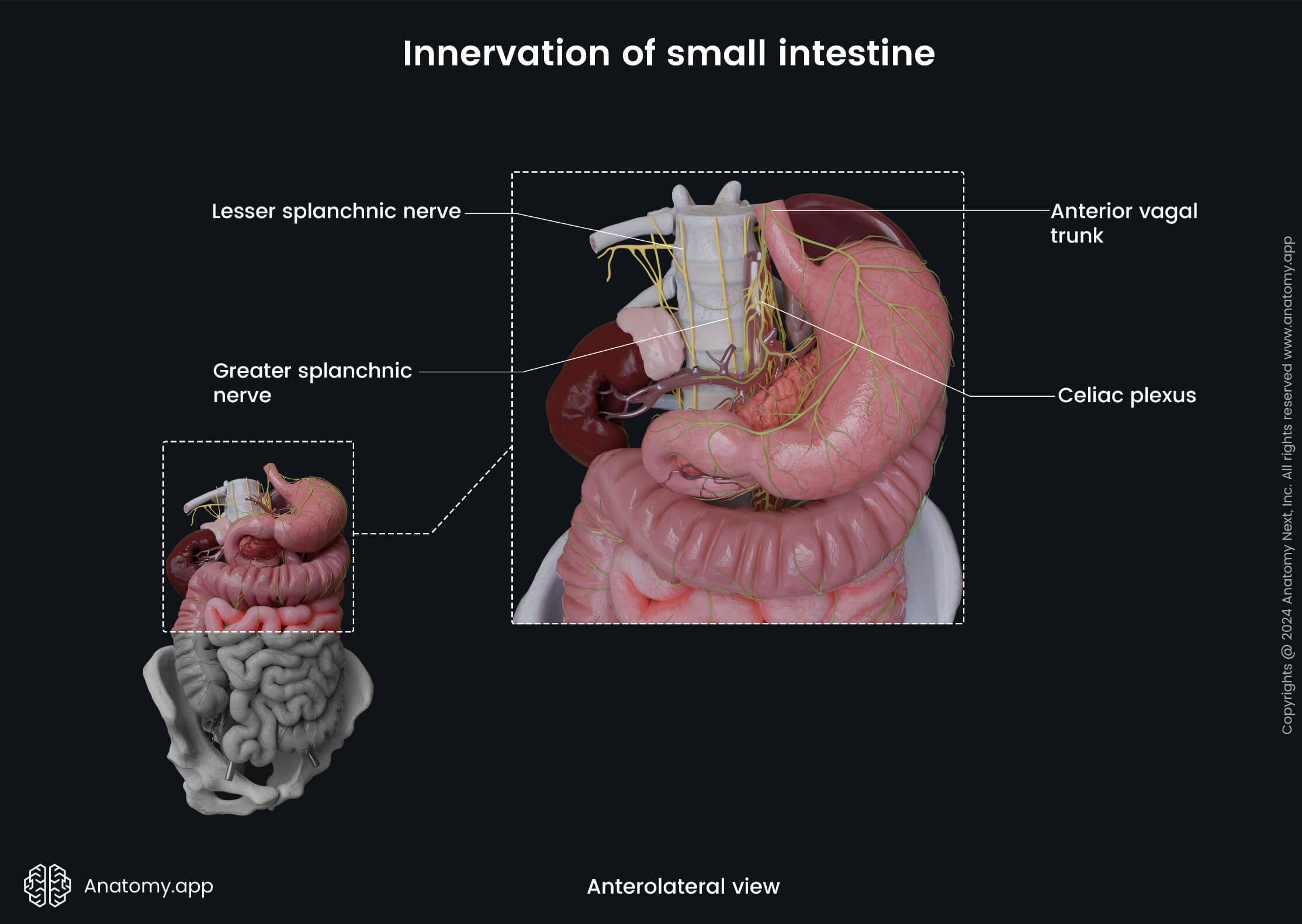
In contrast, the parasympathetic innervation is provided by fibers of the vagus nerve (CN X) via the anterior and posterior vagal trunks. The parasympathetic fibers stimulate intestinal gland secretion and smooth muscle cell contractions. Also, they provide vasodilation (widening of the lumen of vessels) of the intestinal blood vessels.
The nerve fibers of both systems extend throughout the entire length of the small intestine and synapse with the neurons located in the intestinal wall, forming two plexuses:
- Submucosal plexus (Meissner’s plexus) - located in the submucosal layer; contains only the parasympathetic fibers;
- Myenteric plexus (Auerbach’s plexus) - positioned in the muscularis externa between both its layers; contains parasympathetic and sympathetic nerve fibers.
Lymphatic drainage
Due to the specific physiologic characteristics of the small intestine, the intestinal lymphatic system has various very important functions:
- It provides immune system responses.
- The intestinal lymphatic system regulates the removal of interstitial fluid.
- It transports dietary fat and fat-soluble vitamins absorbed by the intestinal mucosa.
Several lymphatic networks are located within the small intestine - one in the submucosal tissue, one in the villi and another one in the smooth muscle layer.
The lymph collected from the duodenum drains to the pancreaticoduodenal lymph nodes located along the superior and inferior pancreaticoduodenal arteries, pyloric lymph nodes found around the pylorus of the stomach, superior mesenteric lymph nodes situated along the superior mesenteric artery and celiac lymph nodes along the celiac trunk.
The lymph from the jejunum and ileum is drained mainly to the juxta-intestinal and mesenteric lymph nodes located around the peripheral arterial arcades and jejunal and ileal arteries and then further to the superior mesenteric lymph nodes found around the superior mesenteric artery. The lymph collected from the terminal ileum usually is drained to the ileocolic lymph nodes.
Small intestine functions
The main functions of the small intestine include the absorption of nutrients (proteins, fats, carbohydrates, vitamins and minerals) and water from partially digested food and completion of nutrient breakdown, secretion of hormones and intestinal juice. Also, the small intestine participates in providing immune responses.
- The intestinal epithelial cells are also responsible for the absorption of electrolytes and water. The majority of the water absorption occurs in the proximal small intestine, while the remaining water is absorbed by the large intestine.
- The gastrointestinal tract organs produce numerous enzymes necessary for nutrient breakdown, which mostly happens in the small intestine. Mainly the pancreas secretes these enzymes, and they reach the small intestine via the main pancreatic duct that opens in the descending part of the duodenum.
- Proteins are broken down into amino acids, and complex carbohydrates break down into monosaccharides. And finally, fats break down into fatty acids and glycerol. Before the breakdown, fats are emulsified by the bile that reaches the duodenum via the vessels of the biliary tree.
- Minerals, such as calcium, iron, magnesium and phosphorus, are absorbed mainly in the duodenum and proximal jejunum. Vitamin B12 is absorbed in the distal ileum. It binds with the intrinsic factor secreted by the gastric parietal cells and forms a complex so that it can be later absorbed in the small intestine.
- The small intestine is also responsible for intestinal motility - movements provided by the muscle fibers within the small intestine wall. These muscle contractions transit intestinal content towards the large intestine.
- The functions of the small intestine that provide immune responses include the following: intestinal motility that helps to decrease contact with bacteria and pathogens, antibacterial substances secreted by Paneth cells, antigen presentation and production of antibodies by plasma cells.
References:
- Drake, R., Vogl, W., & Mitchell, A. (2019). Gray’s Anatomy for Students: With Student Consult Online Access (4th ed.). Elsevier.
- Gray, H., & Carter, H. (2021). Gray’s Anatomy (Leatherbound Classics) (Leatherbound Classic Collection) by F.R.S. Henry Gray (2011) Leather Bound (2010th Edition). Barnes & Noble.
- Moore, K.L., Dalley, A.F., Agur, A.M. (2018). Clinically Oriented Anatomy, 8th Edition, Lippincott Williams & Wilkins.
- Santaolalla, R., Fukata, M., & Abreu, M. T. (2011). Innate immunity in the small intestine. Current Opinion in Gastroenterology, 27(2), 125–131. https://doi.org/10.1097/mog.0b013e3283438dea