- Anatomical terminology
- Skeletal system
- Joints
- Muscles
- Heart
- Blood vessels
- Lymphatic system
- Nervous system
- Respiratory system
- Digestive system
- Urinary system
- Female reproductive system
- Male reproductive system
- Endocrine glands
- Eye
- Ear
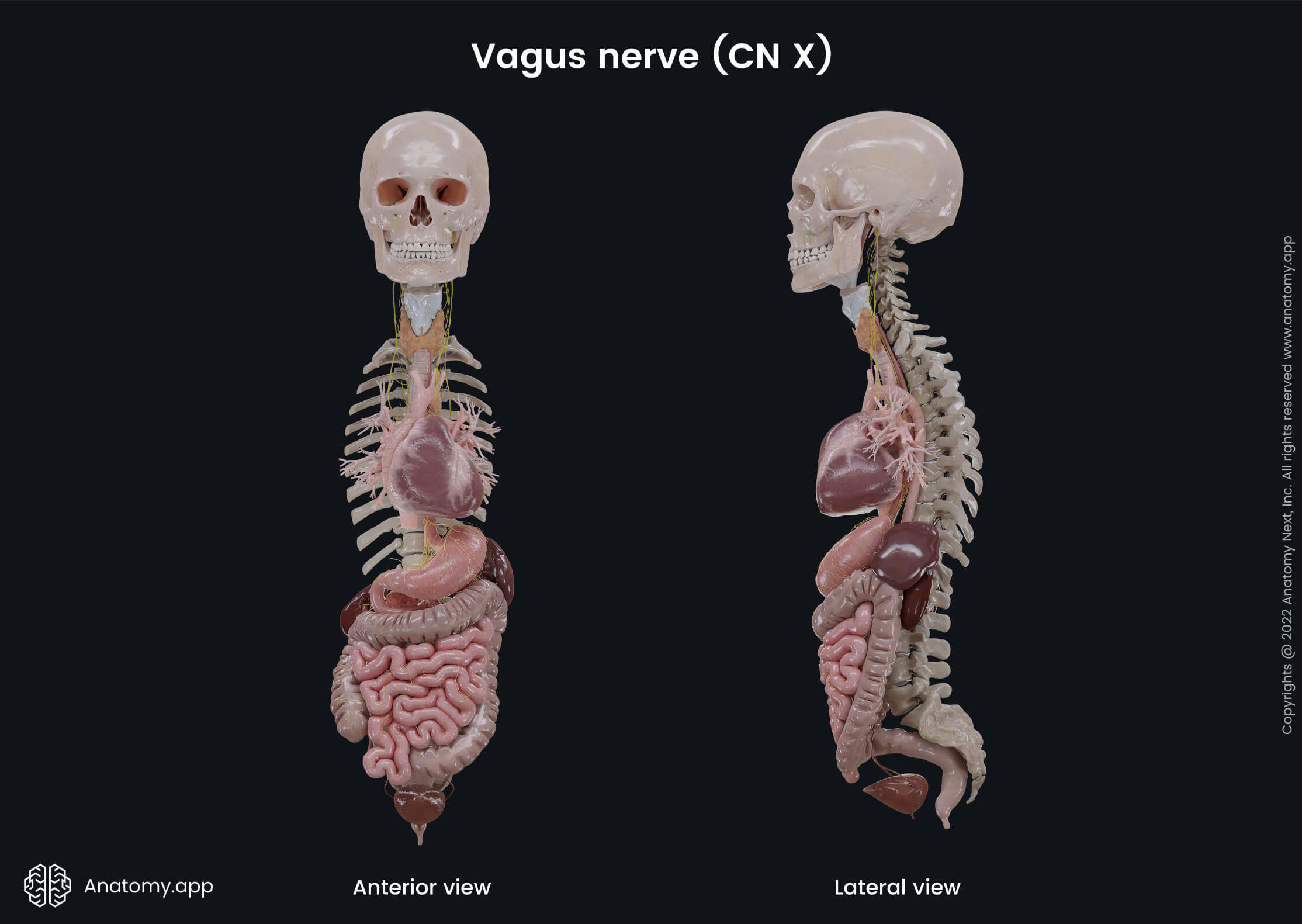
Vagus nerve (CN X)
The vagus nerve (Latin: nervus vagus), also called the vagus, is the tenth cranial nerve (CN X). It is the cranial nerve with the widest distribution in the human body because it innervates not only structures in the head but also runs through the neck, thorax, and abdomen, supplying most of the visceral organs there.
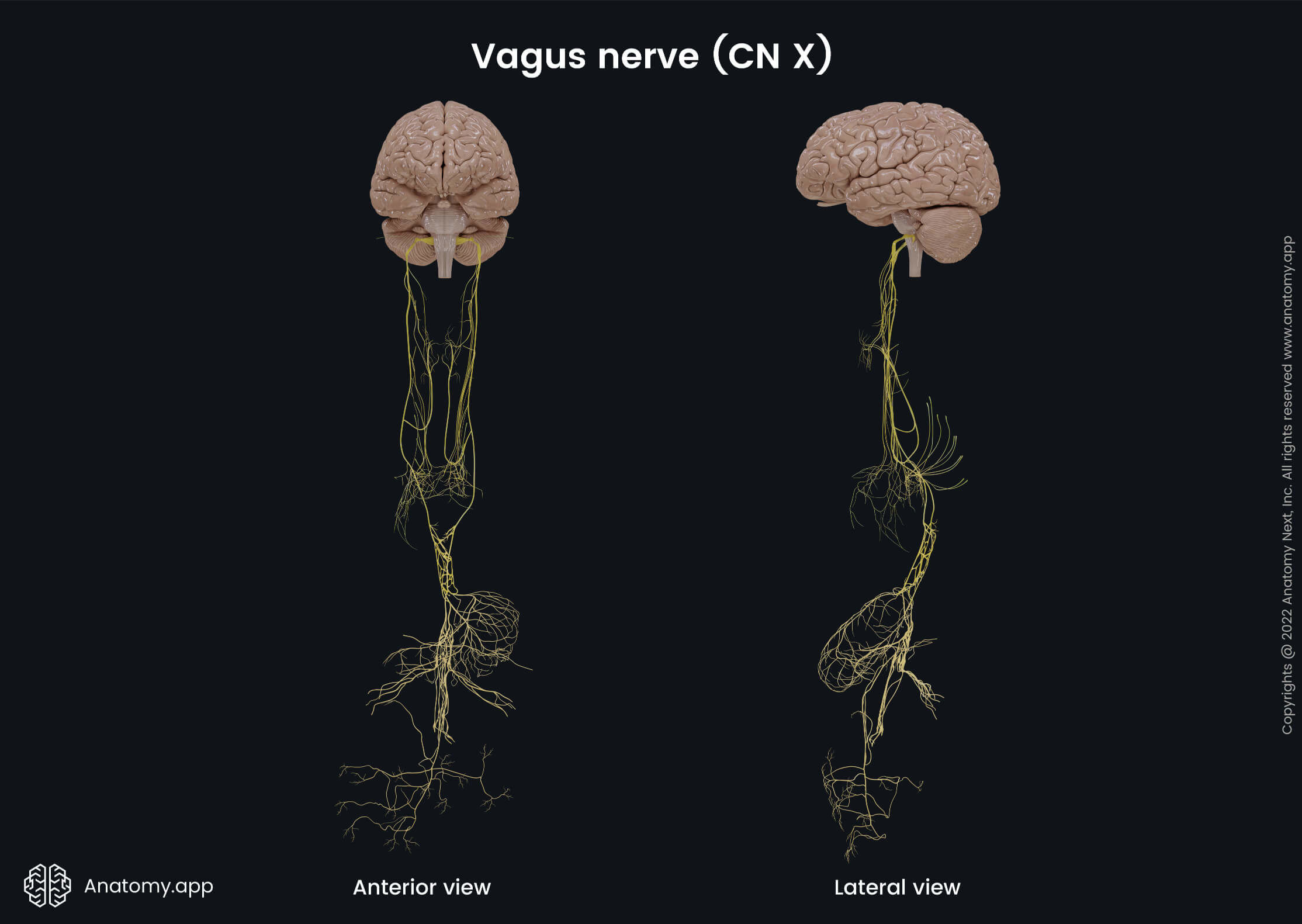
The vagus is the longest nerve in the human body, providing various important internal organ functions such as breathing, heart rate, digestion, as well as different reflex actions, for example, coughing, sneezing, vomiting, and swallowing.
The vagus nerve is a mixed nerve containing both - afferent (sensory) and efferent (motor) - fibers, as well as parasympathetic fibers. It provides motor signals through the somatic and visceral efferent fibers to the organs, as well as carries general, special sensory, and special visceral afferent information from the organs back to the brain.
The general sensory fibers, for example, supply the skin or the mucous membrane of the external acoustic meatus, pharynx, and larynx, while the special sensory fibers provide taste sensation to the epiglottis and the root of the tongue. The motor fibers provide innervation to the muscles of the pharynx and larynx, as well as the soft palate. The parasympathetic fibers provide the supply to the smooth muscles of the trachea, gastrointestinal tract, and bronchi, as well as regulate the heart rhythm.
Vagus nerve parts
The vagus nerve can be divided into four parts:
Origin and cranial part of vagus nerve
The axons of the vagus nerve emerge from four nuclei located in the inferior aspect of the rhomboid fossa within the medulla oblongata. The vagal nuclei include the following:
- Nucleus ambiguus - motor nucleus, shared with the glossopharyngeal (CN IX) and accessory nerve (CN XI); also contains parasympathetic neurons for the heart; the efferent motor fibers provide innervation for the somatic muscles of the pharynx, larynx, and soft palate;
- Solitary nucleus (solitary tract nucleus) - visceral sensory nucleus, shared with the intermediate nerve and glossopharyngeal nerve (CN IX); receives afferent fibers from the visceral organs (taste sensation and sensory information from the middle ear);
- Dorsal nucleus (dorsal vagal nucleus) - parasympathetic motor nucleus; provides parasympathetic efferent fibers to the organs of the thorax and abdomen (primarily gastrointestinal tract and lungs);
- Spinal trigeminal nucleus - general sensory nucleus.
Rootlets that arise from the medulla oblongata form smaller inferior and larger superior bundles that collectively form the vagus nerve after it exits the medulla through the posterolateral sulcus along with the glossopharyngeal nerve (CN IX) and the cranial root of the accessory nerve (CN XI).
The vagus nerve leaves the cranial cavity through the jugular foramen accompanied by the accessory nerve (CN XI), both sharing an arachnoid and a dural sheath. The vagus nerve has two enlargements - the first one is the superior (jugular) ganglion at the level of the jugular fossa, and the second is the inferior (nodose) ganglion below the fossa.
Both ganglions contain sensory afferent neurons, which dendrites begin in the periphery of the body, but axons end in the brain at the solitary nucleus. The cranial part gives off the following branches in the jugular fossa from the superior ganglion:
- Meningeal branch - contains general afferent (sensory) fibers innervating the dura mater in the posterior cranial fossa; it re-enters the cranial cavity through the jugular foramen;
- Auricular branch (Arnold's nerve) - provides general afferent (sensory) fibers innervating the skin of the posterior wall of the external acoustic meatus, the outer part of the tympanic membrane, and the posterior aspect of the auricle.
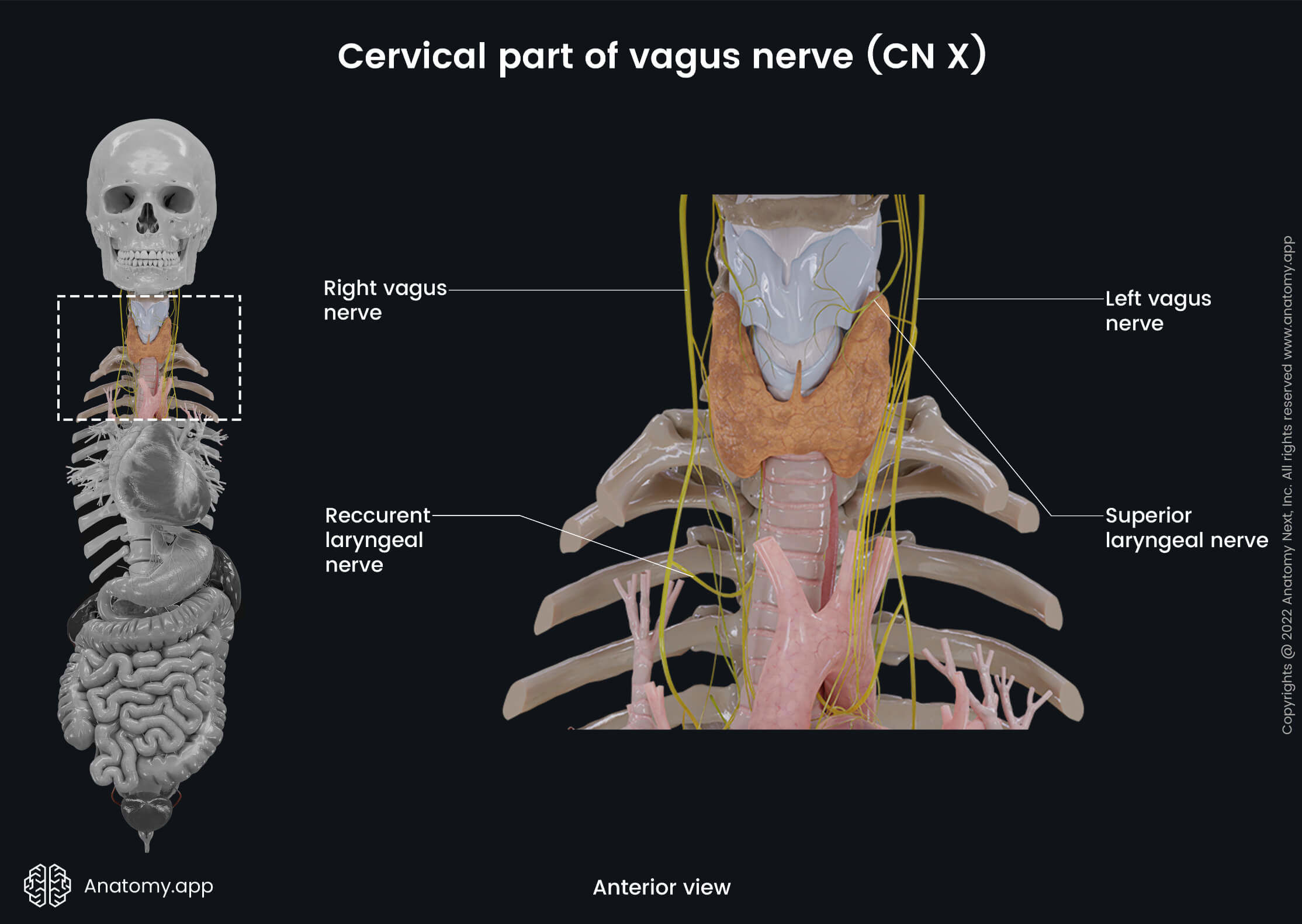
Cervical part of vagus nerve
After leaving the skull through the jugular foramen, the vagus nerve descends in the neck. It is covered by the carotid sheath and goes through the neck together with the internal carotid artery and the internal jugular vein. Further, it travels between the common carotid artery and the internal jugular vein, going posteriorly to the mentioned blood vessels.
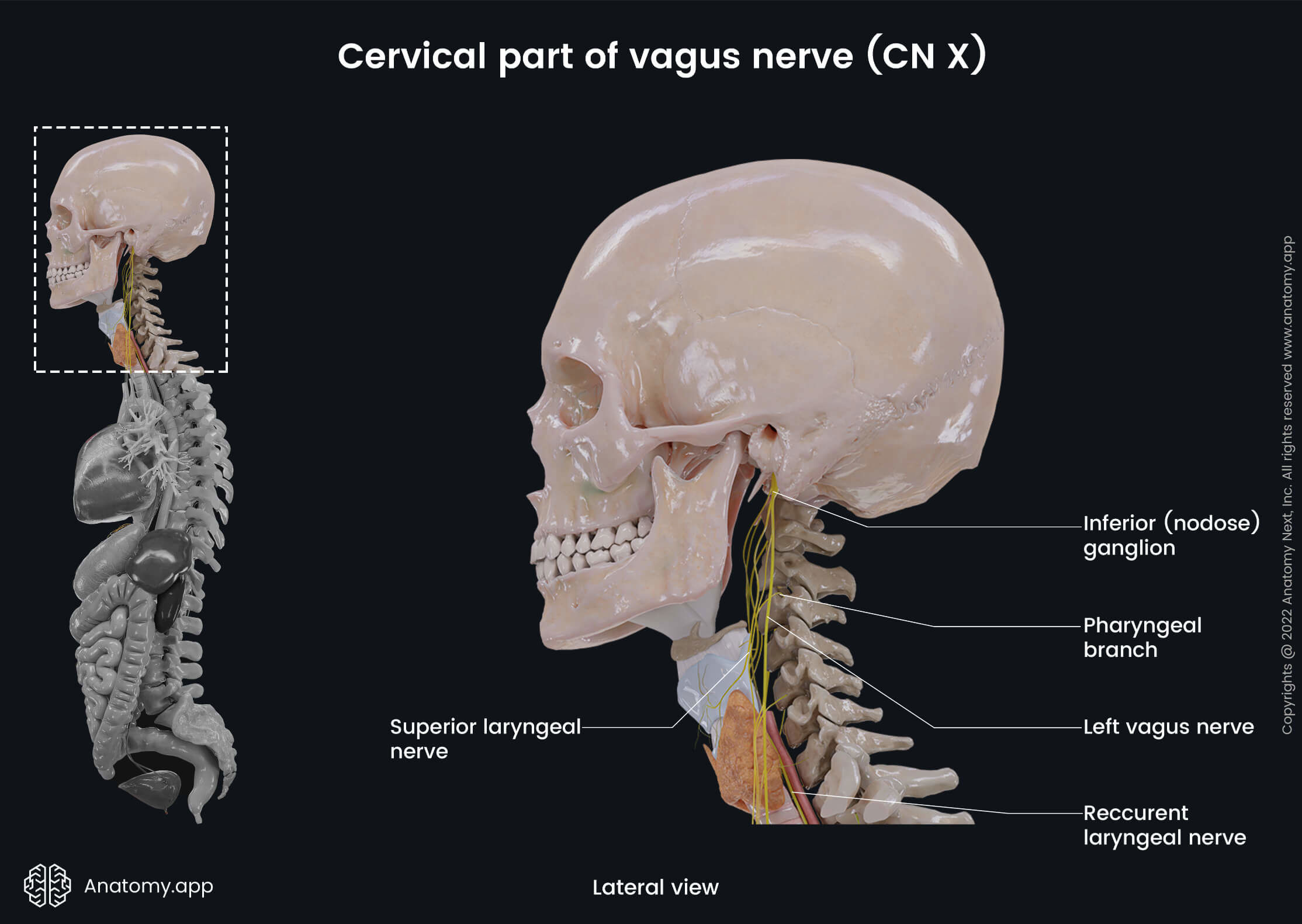
At the level of the superior thoracic aperture, the vagus nerve descends into the thorax. The cervical part of the vagus nerve gives off four sets of branches:
- Pharyngeal branches - contain visceral afferent and motor efferent fibers; they arise from the inferior ganglion and travel between the external and internal carotid arteries to the superior border of the middle pharyngeal constrictor, where they distribute into several filaments, which enter branches of the sympathetic chain and glossopharyngeal nerve (CN IX) and participate in forming the pharyngeal nerve plexus that innervates the muscles of the pharynx (except the stylopharyngeus muscle) and the inferior aspect of the mucous membrane of the pharynx, as well as the muscles of the soft palate (except the tensor veli palatini muscle);
- Superior laryngeal nerve - contains all three types of fibers; arises from the inferior ganglion and travels alongside the internal carotid artery to the pharynx, where it divides into internal and external branches of the superior laryngeal nerve; the internal branch contains sensory and parasympathetic fibers, it travels through the thyrohyoid membrane and supplies the mucous membrane of the larynx above the vocal folds, mucous membrane of the pharynx at the pyriform sinus area, and the mucous membrane of the root of the tongue, as well as provides small branches to the thyroid and parathyroid glands; in contrast, the external branch of the superior laryngeal nerve carries motor fibers, which innervate the cricothyroid muscle of the larynx;
- Recurrent laryngeal nerve (inferior laryngeal nerve) - contains all three types of fibers; differs in origin and course on the left and right side; the term "recurrent" indicates that these nerves travel in the opposite direction to the nerve they branch from; on the left side, the left recurrent laryngeal nerve loops around the aortic arch, while the right nerve loops under the first part of the right subclavian artery, and at this level, both nerves give cardiac filaments to the deep cardiac plexus; after that, the left and right recurrent laryngeal nerves ascend in a groove between the esophagus and trachea, closely to the medial surface of the thyroid gland, and then penetrate the lower border of the inferior constrictor muscle, entering the larynx; its terminal branch supplies the mucous membrane of the larynx below the vocal folds and, together with the accessory nerve (CN XI), innervates the muscles of the larynx (except the cricothyroid muscle), thyroid, and parathyroid glands; the recurrent laryngeal nerve gives tracheal branches to the mucous membrane of the trachea, its glands, and smooth muscle cells; besides tracheal branches, it also provides esophageal branches innervating glands and skeletal muscles of the upper one-third of the esophagus;
- Superior cardiac branches - contain sensory and parasympathetic fibers; branches descend along the common carotid artery and, together with the branches of the sympathetic trunk and recurrent laryngeal nerve, form the cardiac plexus, from which nerves travel to the heart; the superior cardiac branches are divided into smaller divisions known as the superior and inferior divisions of the superior cardiac branches.
Thoracic part of vagus nerve
In the thorax, both the left and right vagus nerves run behind the pulmonary radix (the root of the lung). The left vagus nerve crosses anterior to the left subclavian artery when entering the thorax and descends behind the primary left bronchus and lateral to the aortic arch.
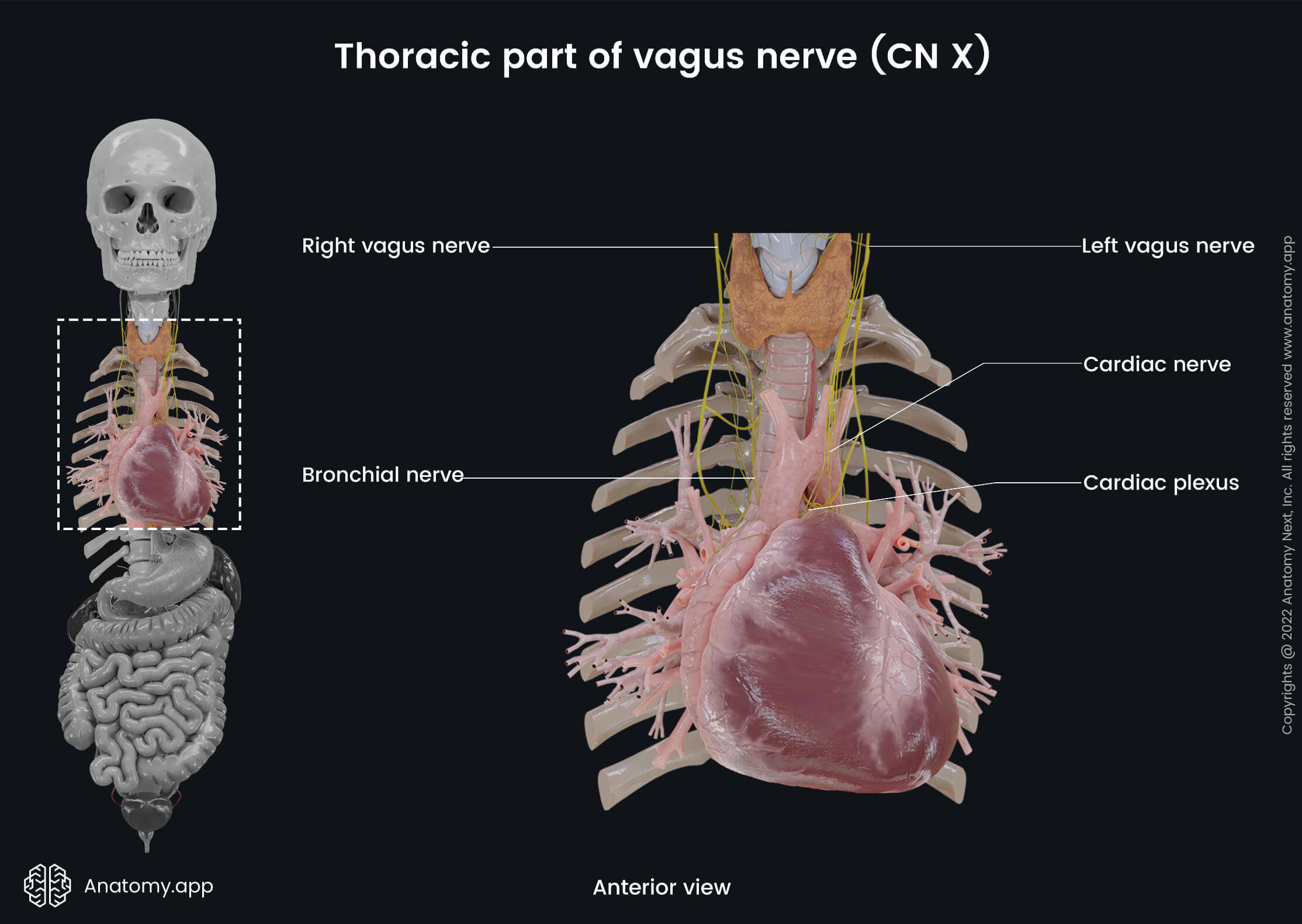
The right vagus crosses anterior to the right subclavian artery and goes behind the primary right bronchus and esophagus. At the level of the middle third of the esophagus, the left and right fibers mix together to form the esophageal plexus, which wraps around the esophagus. The inferior fibers of the esophageal plexus form the anterior and posterior vagal trunks containing fibers of both vagus nerves.
The anterior vagal trunk distributes fibers on the anterior surface of the esophagus, and it consists primarily of fibers from the left vagus nerve. The posterior vagal trunk consists primarily of fibers from the right vagus nerve, and they are distributed on the posterior surface of the esophagus.
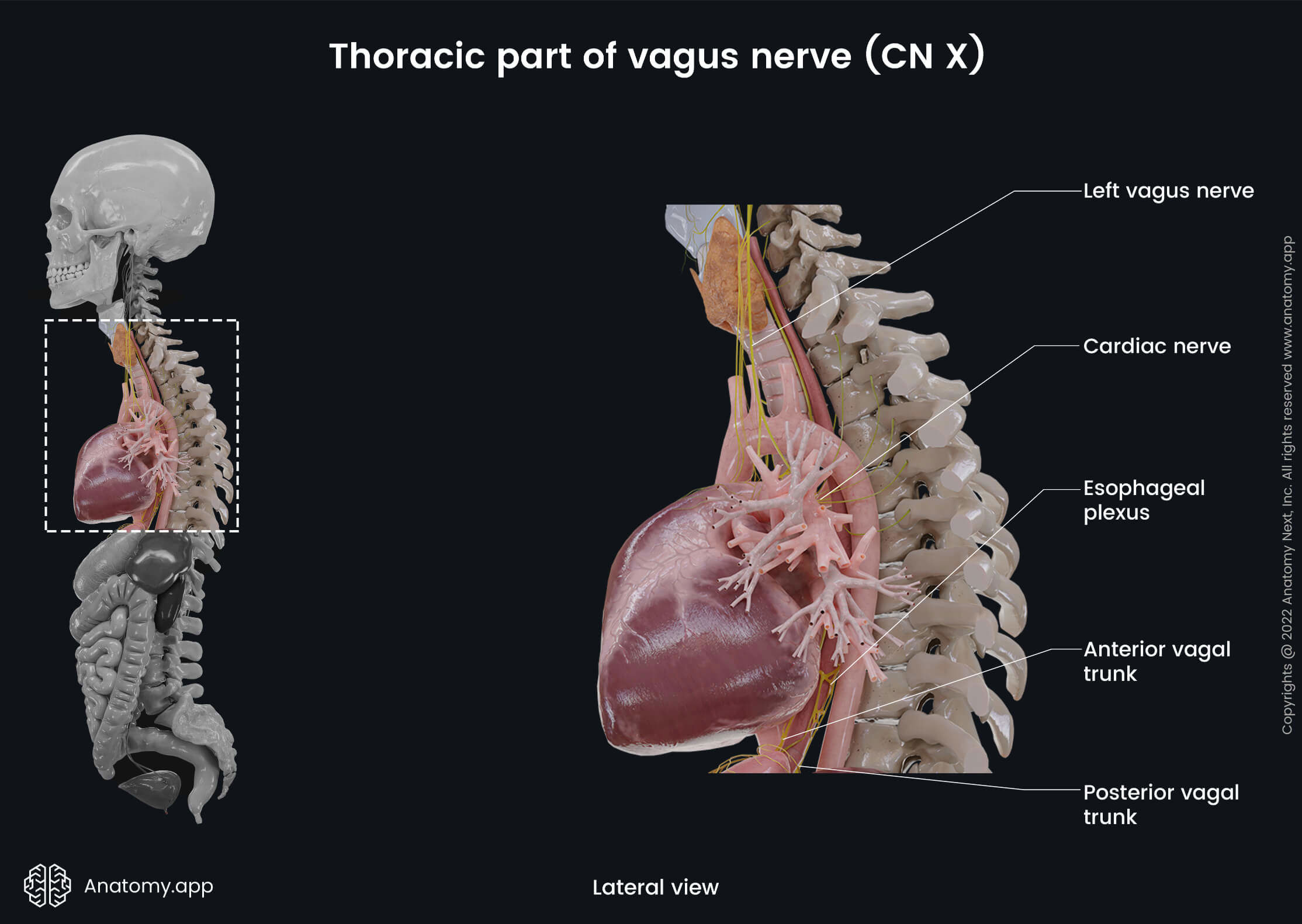
Both trunks together with the esophagus descend through the esophageal hiatus of the diaphragm into the abdominal cavity. In the thorax, the vagus nerve and its branches contain only sensory and parasympathetic fibers. The branches arising from the thoracic part of the vagus include the following:
- Inferior cardiac nerves - together with the inferior branches of the superior cardiac nerves and sympathetic trunk, as well as recurrent laryngeal nerve form the cardiac plexus, which innervates the heart;
- Bronchial branches - together with the branches of the sympathetic trunk, these branches form the pulmonary plexus, which provides innervation of the mucous membrane of the bronchi, their glands, and smooth muscle cells, as well as lung tissue and visceral pleura; bronchial branches are divided into two subdivisions - anterior and posterior bronchial branches - depending on which aspect of the root of the lung they are located;
- Esophageal branches - together with the branches of the sympathetic trunk form the esophageal plexus, which provides motor and sensory fibers to the mucous membrane of the esophagus, its glands, and smooth muscle cells.
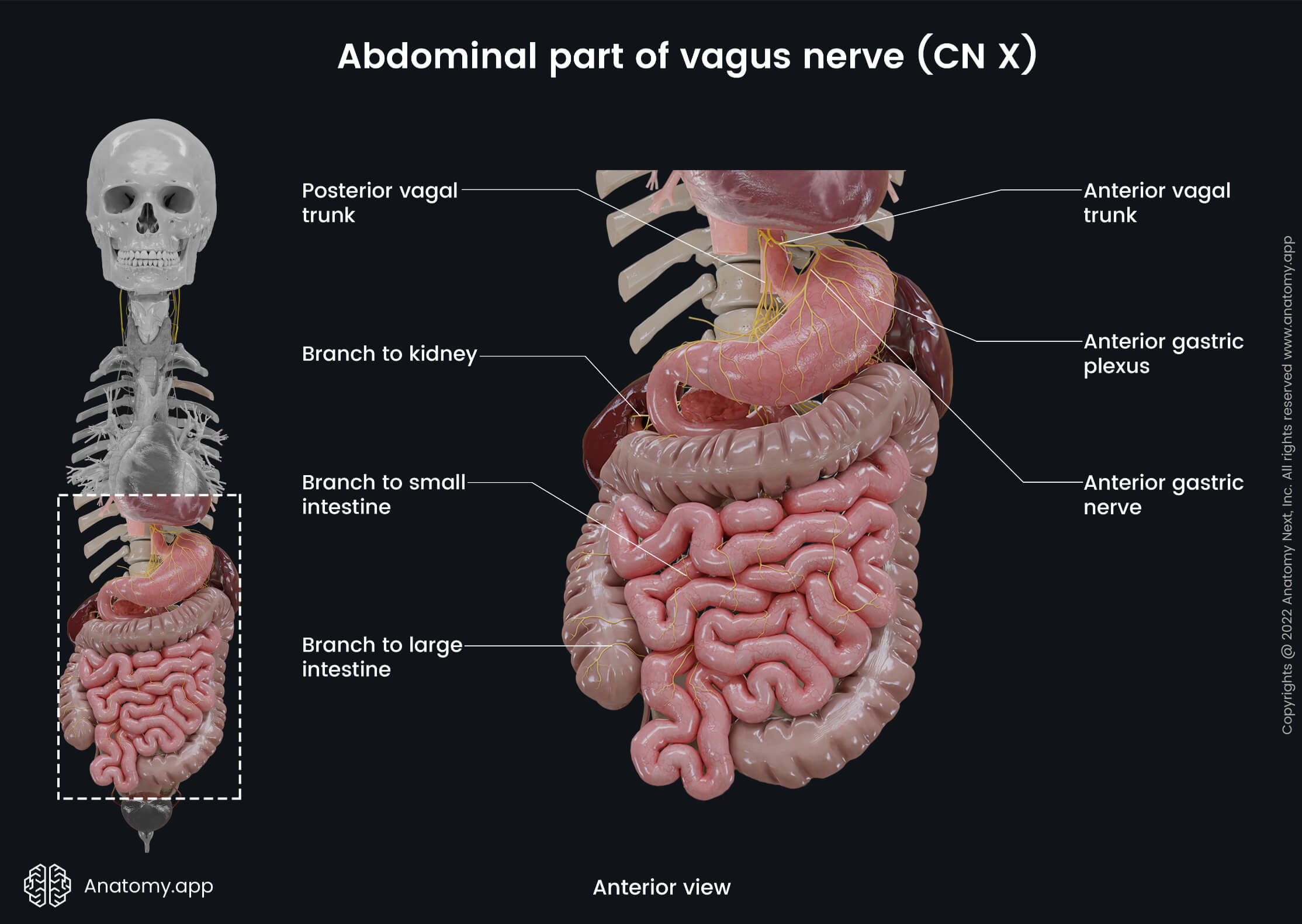
Abdominal part of vagus nerve
In the abdomen, both vagal trunks contain sensory and parasympathetic fibers. The anterior vagal trunk runs along the lesser curvature of the stomach, where it divides into several sets of branches:
- Anterior gastric branches - these branches of the vagus nerve form the anterior gastric plexus and supply the stomach;
- Hepatic branch - travels along with the lesser omentum to the liver.
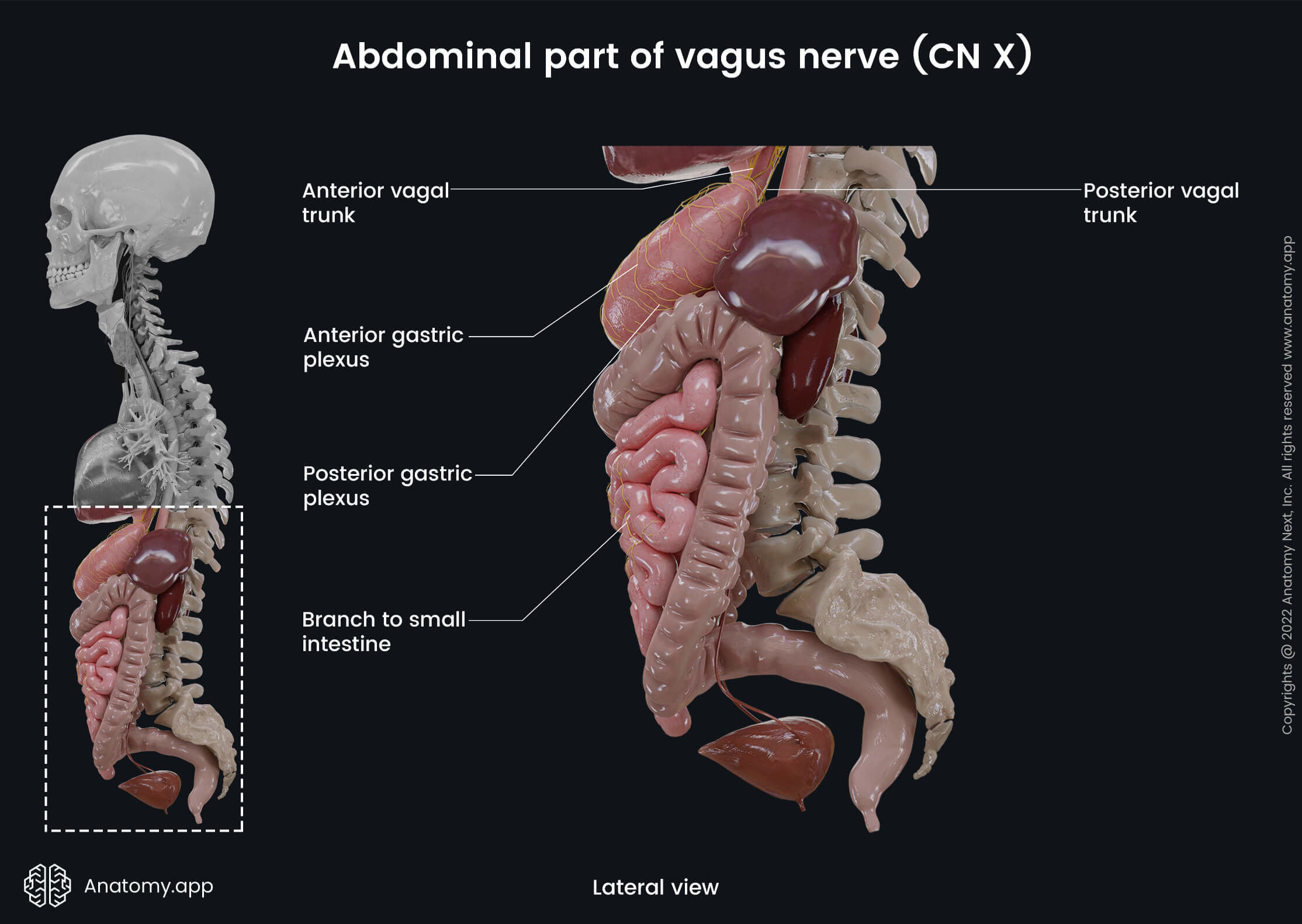
The posterior vagal trunk travels more posteriorly along the lesser curvature of the stomach to reach the posterior surface, where it splits into several sets of branches:
- Posterior gastric branches - participate in forming the posterior gastric plexus, which provides the nerve supply to the stomach and is located on the posterior surface of the stomach at the cardia;
- Branches to the kidneys, liver, and biliary tract;
- Celiac branch - joins the celiac nerve plexus and supplies almost all abdominal organs (small and large intestines till the transverse colon, liver, pancreas, spleen, adrenal glands, kidneys, two-thirds of ureters, testicles, epididymis, ovaries).