- Anatomical terminology
- Skeletal system
- Joints
- Muscles
- Heart
- Blood vessels
- Lymphatic system
- Nervous system
- Respiratory system
- Digestive system
- Urinary system
- Female reproductive system
- Male reproductive system
- Endocrine glands
- Eye
- Ear
Accessory nerve (CN XI)
The accessory nerve (Latin: nervus accessorius) or the eleventh cranial nerve (CN XI) is a motor nerve supplying the sternocleidomastoid and trapezius muscles. Traditionally, the accessory nerve is described as arising from both - the medulla oblongata and spinal cord, consisting of a cranial and a spinal root. However, the existence of a cranial contribution to the accessory nerve is controversial, and many neuroanatomists no longer consider this nerve to be a true cranial nerve, rather as a unique spinal nerve, and the previously thought cranial root to be part of the vagus nerve (CN X). (See the discussion below!)
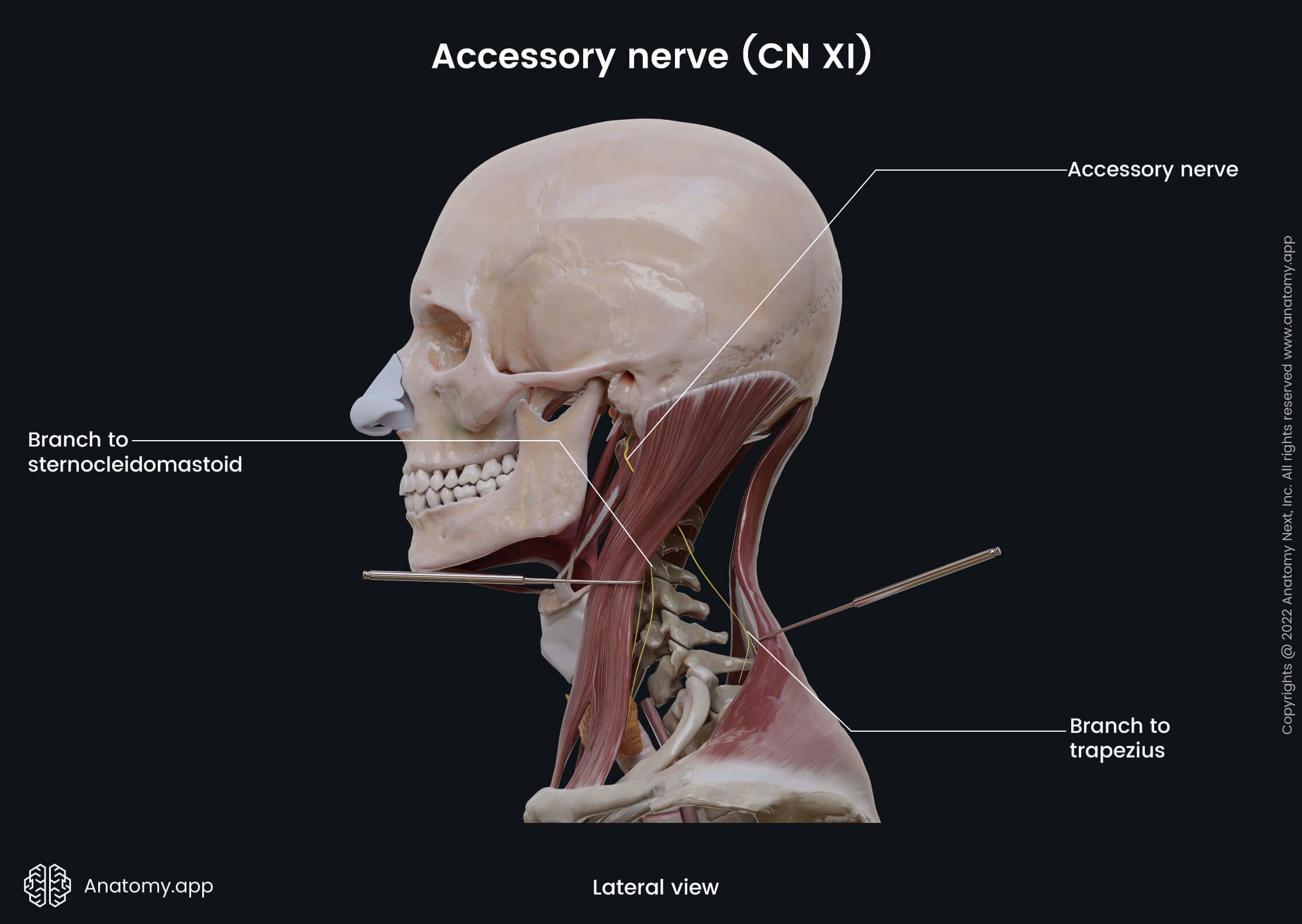
Spinal accessory nerve origin and course
The accessory nerve, also referred to as the spinal accessory nerve, originates from the spinal accessory nucleus located in the posterolateral aspect of the anterior horns of the spinal cord at the levels C1 - C5 (or C6, C7). The fibers coming from the nuclei form delicate spinal rootlets emerging from the lateral surface of the spinal cord, and all together, they collect to form the accessory nerve.
The nerve ascends parallel to the spinal cord, enters the cranial cavity through the foramen magnum, and continues on the lateral aspect of the medulla oblongata. The nerve then joins with the aberrant fibers of the vagus nerve (CN X) as they emerge from the medulla oblongata on its posterolateral sulcus as a distinct rootlet.
These two groups of nerve fibers travel alongside for a short distance through the jugular foramen and then separate to go in different directions. Those separate divisions are known as the internal and external branches.
The aberrant vagal fibers or the internal branches (previously called the "cranial root" of the accessory nerve) join the vagus nerve on the border between its superior and inferior ganglions to ultimately reach the pharyngeal muscles (except the stylopharyngeus muscle), muscles of the soft palate (except the tensor veli palatini muscle) and intrinsic laryngeal muscles.
The external branch or the accessory nerve exits the skull via the jugular foramen and enters the anterior triangle of the neck. It then travels downward, going anterolateral to the internal jugular vein. The occipital artery crosses the nerve as it goes further, and the nerve goes medially behind the digastric and stylohyoid muscles to reach the upper part of the sternocleidomastoid muscle.
This branch enters the deep surface of the sternocleidomastoid muscle and provides motor branches to innervate it, also forming anastomosis with fibers from spinal nerves C2 and/or C3 in the posterior triangle of the neck, and, below the trapezius muscle, it anastomoses with the fibers from the spinal nerves C3 and/or C4.
After piercing the sternocleidomastoid, the accessory nerve descends further, exiting from the posterior border of the muscle. The nerve crosses over the posterior triangle of the neck, lying deep to the cervical plexus. It goes between the layers of the deep cervical fascia and reaches the deep surface of the upper part of the trapezius muscle, and supplies it with motor innervation.
Discussion: cranial root of accessory nerve?
The reports on the cranial contribution to the accessory nerve have been inconsistent, and there has been a controversy regarding the anatomy of the eleventh cranial nerve. There are three main views about the cranial root of the accessory nerve.
The first is the long-established view that the accessory nerve is composed of a cranial root emerging from the medulla oblongata and a spinal root - from the spinal cord. The cranial root of the accessory nerve joins and distributes through the internal branch of the vagus nerve (CN X), so it has been described to functionally be a part of the vagus nerve. It has been suggested that the cranial root of the accessory nerve carries motor fibers that eventually innervate muscles of larynx, pharynx, and soft palate.
The second view is that there is no cranial root of the accessory nerve, as some reports show. (Lachman et al., 2002) In this case, the cranial root of the accessory nerve can be viewed as aberrant vagal fibers arising from the nucleus ambiguus in the medulla oblongata. These fibers emerge as a distinct rootlet, that travels along the accessory nerve for a short distance, and joins the vagus nerve. The accessory nerve, on the other hand, originates only from a nucleus located in the spinal cord. Many neuroanatomists no longer consider the accessory nerve as a true cranial nerve, rather as a unique spinal nerve.
Other studies suggest a third view - that there is a morphologically distinct cranial root of the accessory nerve as recent reports show, but it exists variably (Wiles et al., 2007), while some reports show that the cranial root exists in the majority (Tubbs et al., 2014), and in some cases in all the specimens. (Liu et al., 2014)
Although the cranial root of the accessory nerve appears to be distinct from the vagus nerve in the cranial cavity, this rootlet and the vagus nerve can be regarded functionally as the same nerve based on their distribution in the laryngeal muscles. (Liu et al., 2015)
References:
- Lachman N, Acland RD, Rosse C. 2002. Anatomical evidence for the absence of a morphologically distinct cranial root of the accessory nerve in man. Clin Anat 15:4-10.
- Liu, HF, Won, HS, Chung, IH, Oh, CS, and Kim, IB. (2014). Variable composition of the internal and external branches of the accessory nerve. Clin. Anat., 27: 97-101.
- Liu HF, Won HS, Chung IH, Kim IB, Han SH. (2015). Distribution of the internal branch of the human accessory nerve. Anat Sci Int., 90(3):180-186.
- Wiles, CCR, Wrigley, B. and Greene, JRT. (2007). Re-examination of the medullary rootlets of the accessory and vagus nerves. Clin. Anat., 20: 19-22.
- Tubbs, RS, Benninger, B, Loukas, M, and Cohen-Gadol, AA. (2014). Cranial roots of the accessory nerve exist in the majority of adult humans. Clin. Anat, 27: 102-107.