- Anatomical terminology
- Skeletal system
- Joints
- Muscles
- Heart
- Blood vessels
- Lymphatic system
- Nervous system
- Respiratory system
- Digestive system
- Urinary system
- Female reproductive system
- Male reproductive system
- Endocrine glands
- Eye
- Ear
Lungs
The lungs (plural in Latin: pulmones, singular: pulmo) are the main respiratory organs located in the thorax. There are two lungs in the human body - right and left. They are expandable organs with a spongy structure that occupy most of the thoracic cavity and are situated on both sides of the mediastinum. The lungs are the central organs of the respiratory system and, at the same time, the terminal part of the respiratory tract. The main function of the lungs is to provide gas exchange between the atmosphere and blood by uptaking oxygen from the inhaled air and removing carbon dioxide from the blood.
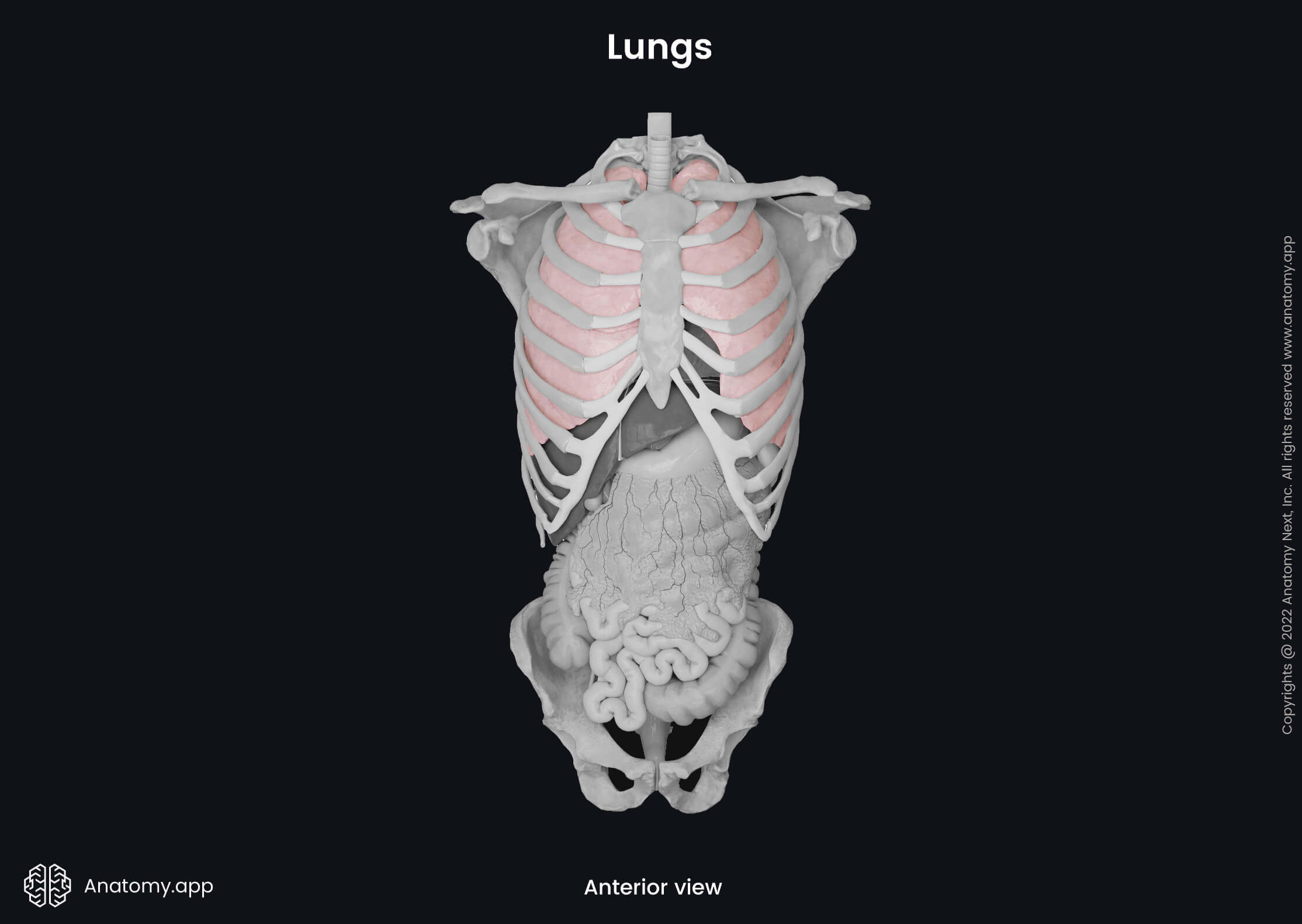
The lungs are surrounded by a serous membrane called pleura. It consists of two layers - visceral and parietal. The visceral pleura is fused with the surfaces of the lungs, while the parietal pleura covers the inner surface of the thoracic wall. Between both layers is a space called the pleural cavity. This space is filled with serous fluid that produces surface tension, so the lungs would expand when the thorax expands during inhalation. Also, it provides lubrication between both layers of pleura.
Lung anatomy
Both lungs are separated from each other by the heart and other structures of the mediastinum, and they are surrounded by the thoracic cage. Each lung appears somewhat conical-shaped, with a rounded apex pointed upwards and a flat base directed downwards. The base of the lung rests on the convex thoracic surface of the diaphragm.
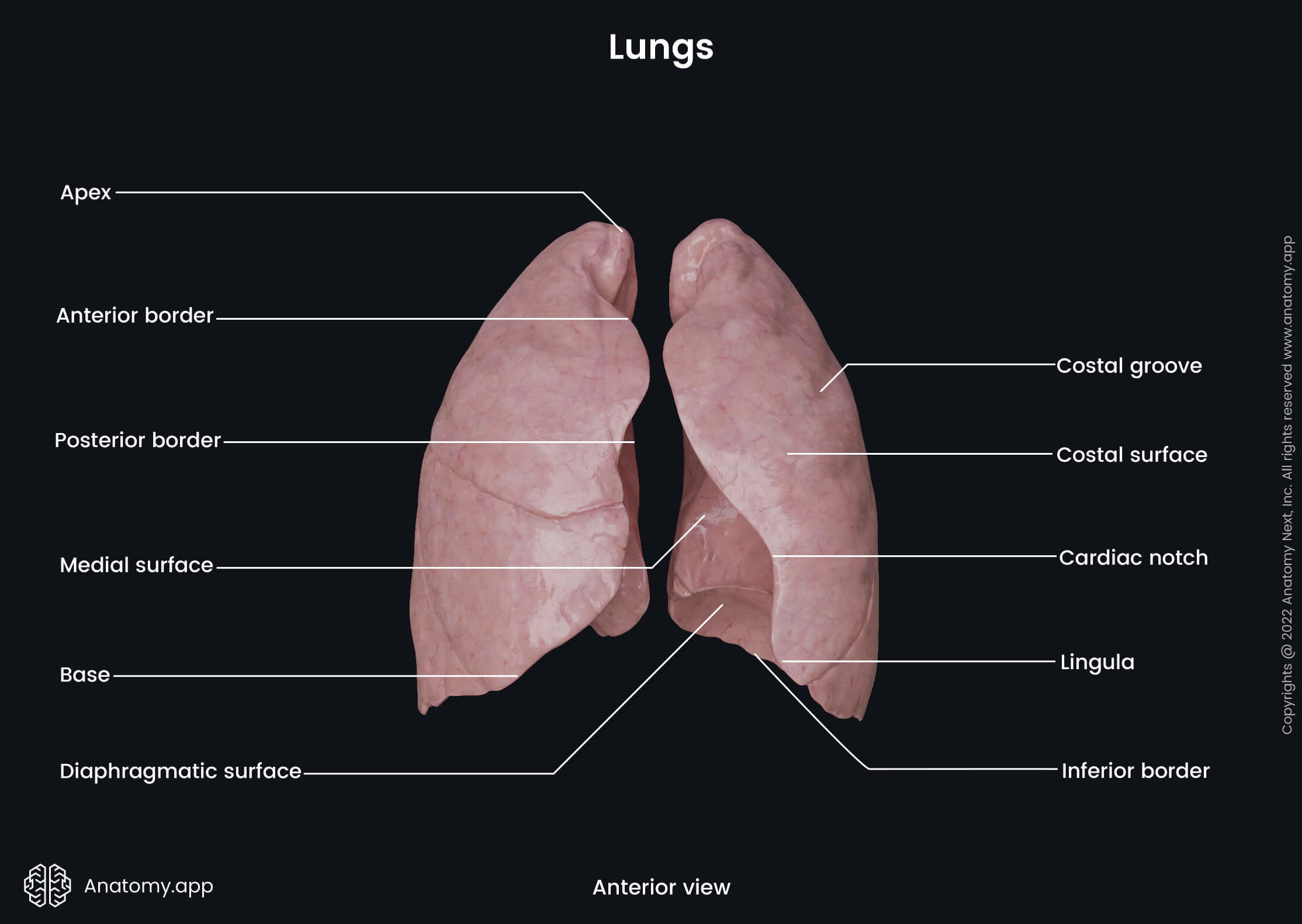
Besides the apex and base, each lung has three borders, three surfaces and a hilum. The hilum is a site of entry for the root of the lung that contains several structures associated with the lungs, including the major bronchi, blood vessels and nerves. Each lung contains fissures that divide the lungs into three (right lung) or two (left lung) sections known as lobes. The lobes are subdivided into segments, and segments are further split into lobules.
Apex of lung
The apex is a rounded tip of the superior end of each lung that projects at the level of the spinous process of the seventh cervical vertebrae (C7). It is situated above the superior thoracic aperture (thoracic inlet) posterior to the scalene muscles. More precisely, the apex is located in the root of the neck, approximately 1 - 2 cm above the clavicle and 3 - 4 cm above the first rib. It is covered by the cervical part of the pleura. The thickened extension of the endothoracic fascia called the suprapleural membrane (Sibson's fascia) extends over the cervical pleura and, therefore, also covers the apex of each lung.
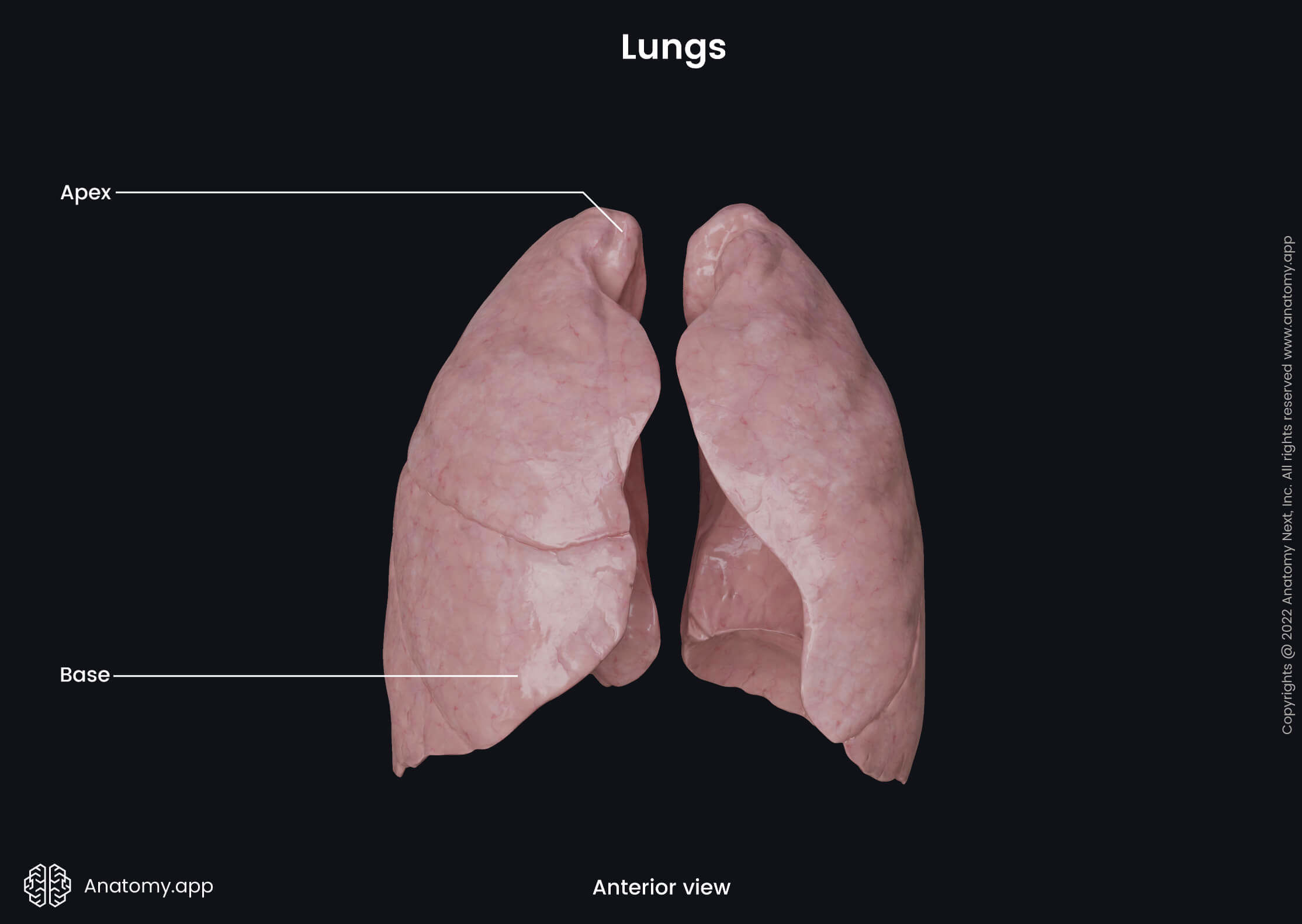
Base of lung
The base of each lung is broad, semilunar and concave. It lies on the thoracic surface of each diaphragmatic dome. The concavity of the base of the right lung is deeper than that of the left lung because the diaphragm lies higher on the right side as the liver is located below it. The location of the liver is also the reason why the right lung appears broader and shorter, but the left lung is longer and narrower.
Surfaces of lungs
Each lung has three major surfaces - costal, medial and diaphragmatic. The lungs also contain smaller inner surfaces between lobes called interlobar surfaces. The interlobar surface faces the surface of the adjacent lobe, and both are separated by an interlobar fissure.
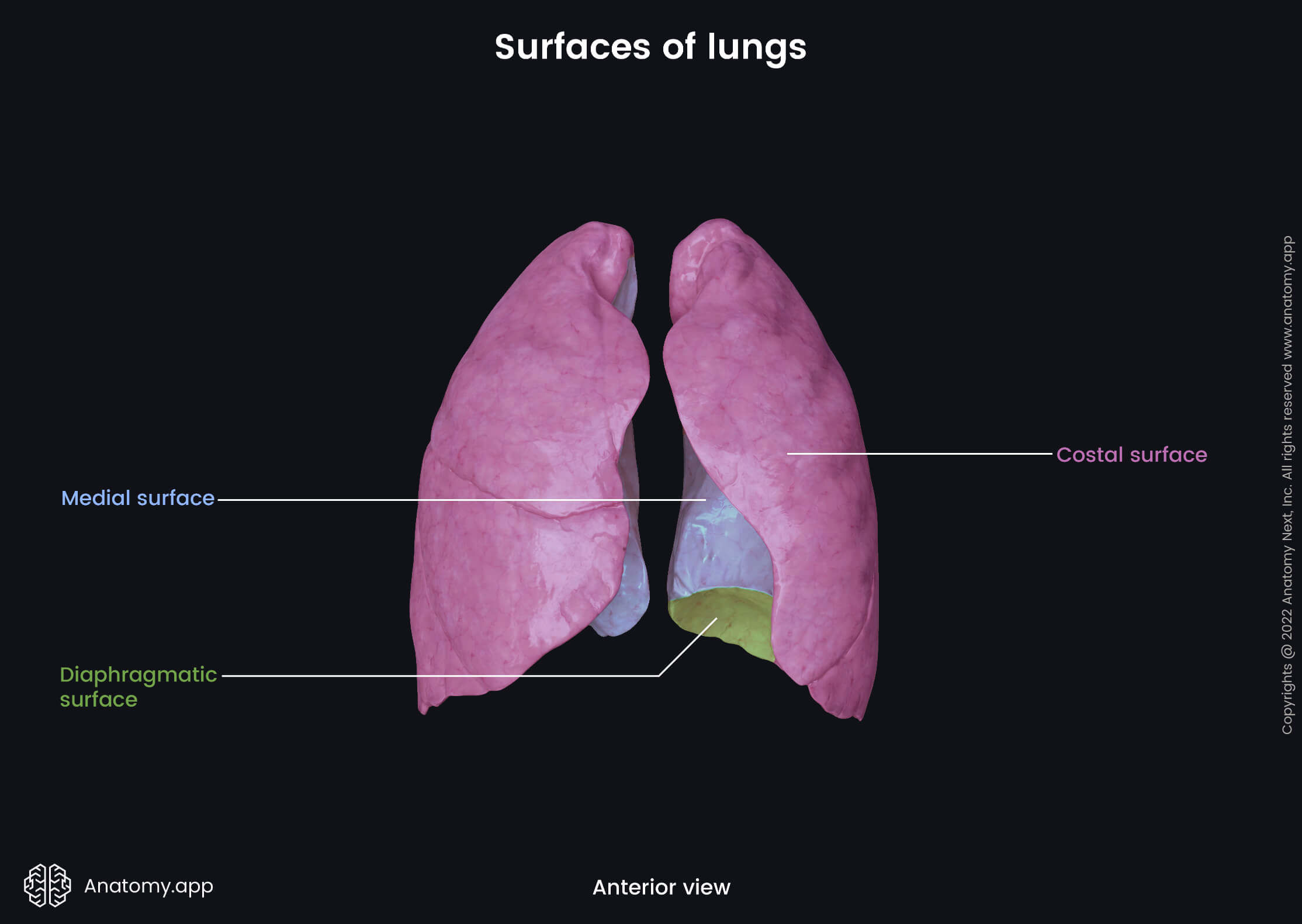
Costal surface
The costal surface of the lung is curved and convex. It connects with the costal pleura and lies against the internal surface of the rib cage. The costal surface contains rib impressions known as the costal grooves.
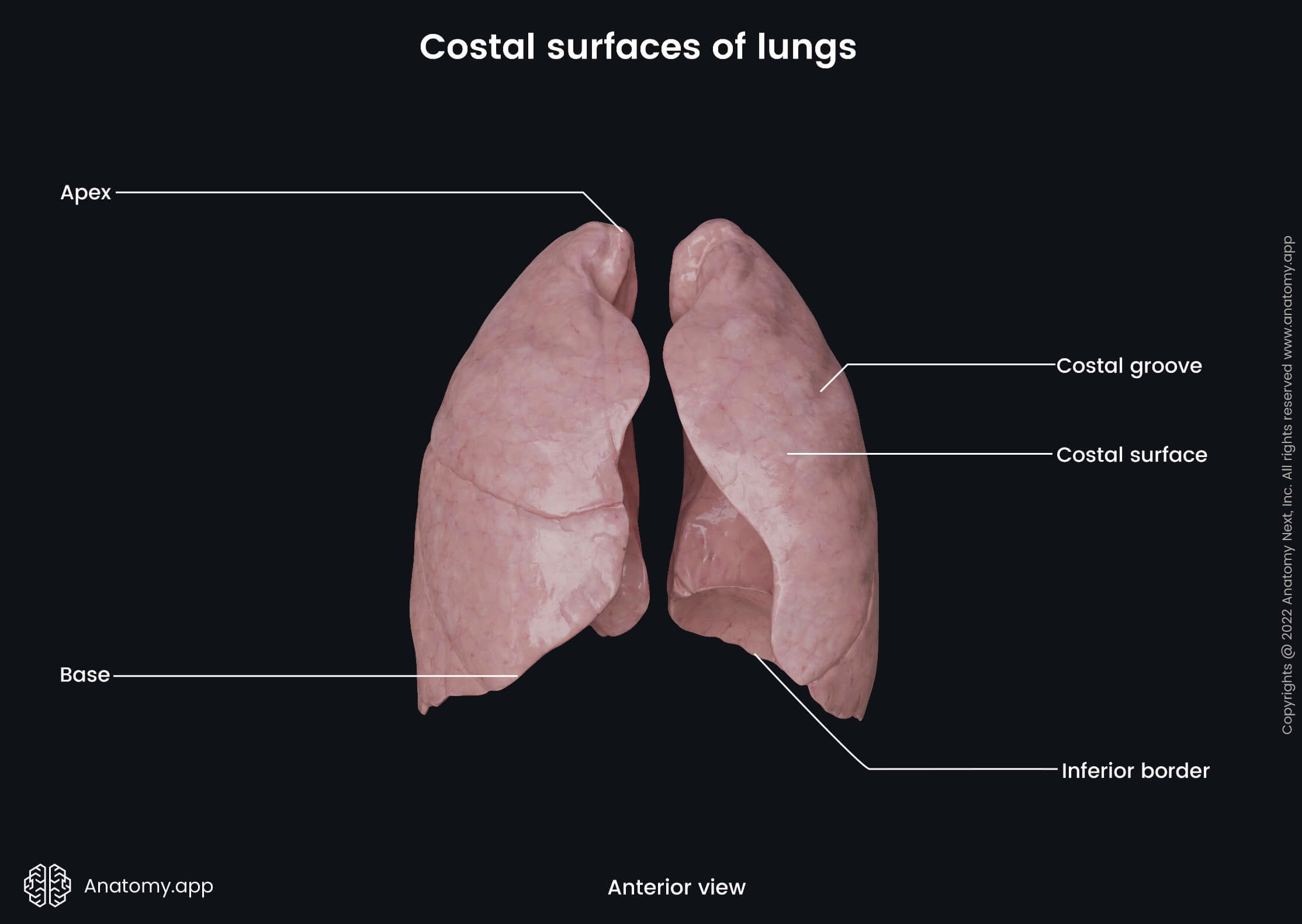
Medial surface
The medial surface, also known as the mediastinal surface, faces the mediastinum, and it is located in the sagittal plane. The medial surface can be subdivided into two smaller parts - vertebral and mediastinal. The vertebral part is the posterior aspect of the medial surface that is connected to the sides of the thoracic spine. The mediastinal part projects anterior to the vertebral part, and it is deeply concave because it contains a cardiac impression - a depression that accommodates the pericardium. Although both lungs have cardiac impressions, it is more pronounced on the left lung surface, where most parts of the heart project.
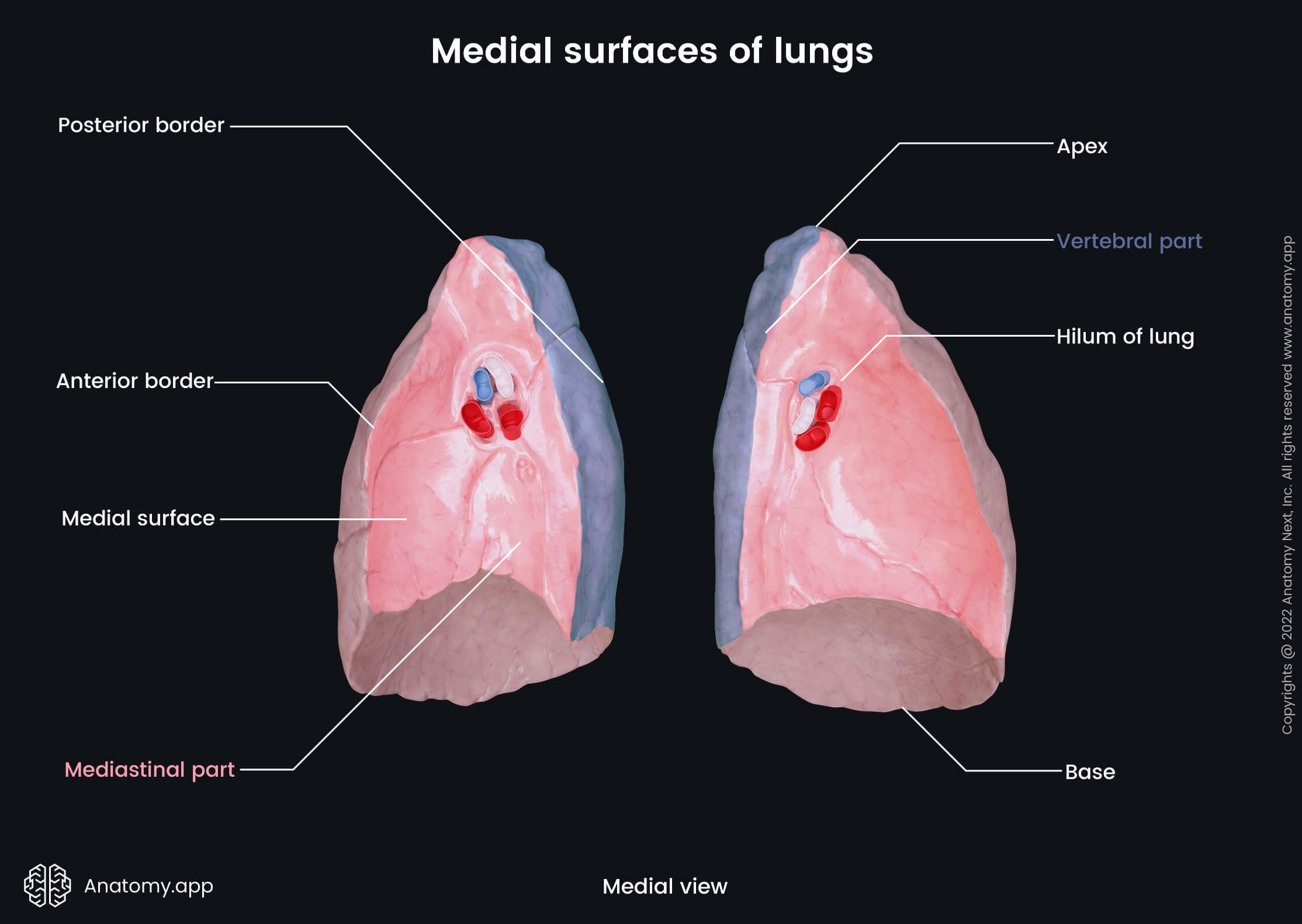
Impressions and grooves of medial surfaces
Besides the heart, the medial surfaces of the lungs contact other organs and vessels of the mediastinum. Therefore, these surfaces contain several more impressions and grooves. Each lung has:
- Groove for the subclavian artery - located on the upper aspect of each superior lobe; it goes on the medial surface of the apex;
- Groove for the brachiocephalic vein - runs adjacent and anterior to the subclavian groove on the apex;
- Groove for the esophagus - positioned on the posterior aspect of the anterior mediastinal part, close to the vertebral part of the medial surface; it goes in a vertical direction from the superior aspect of the inferior lobe to the base of each lung.
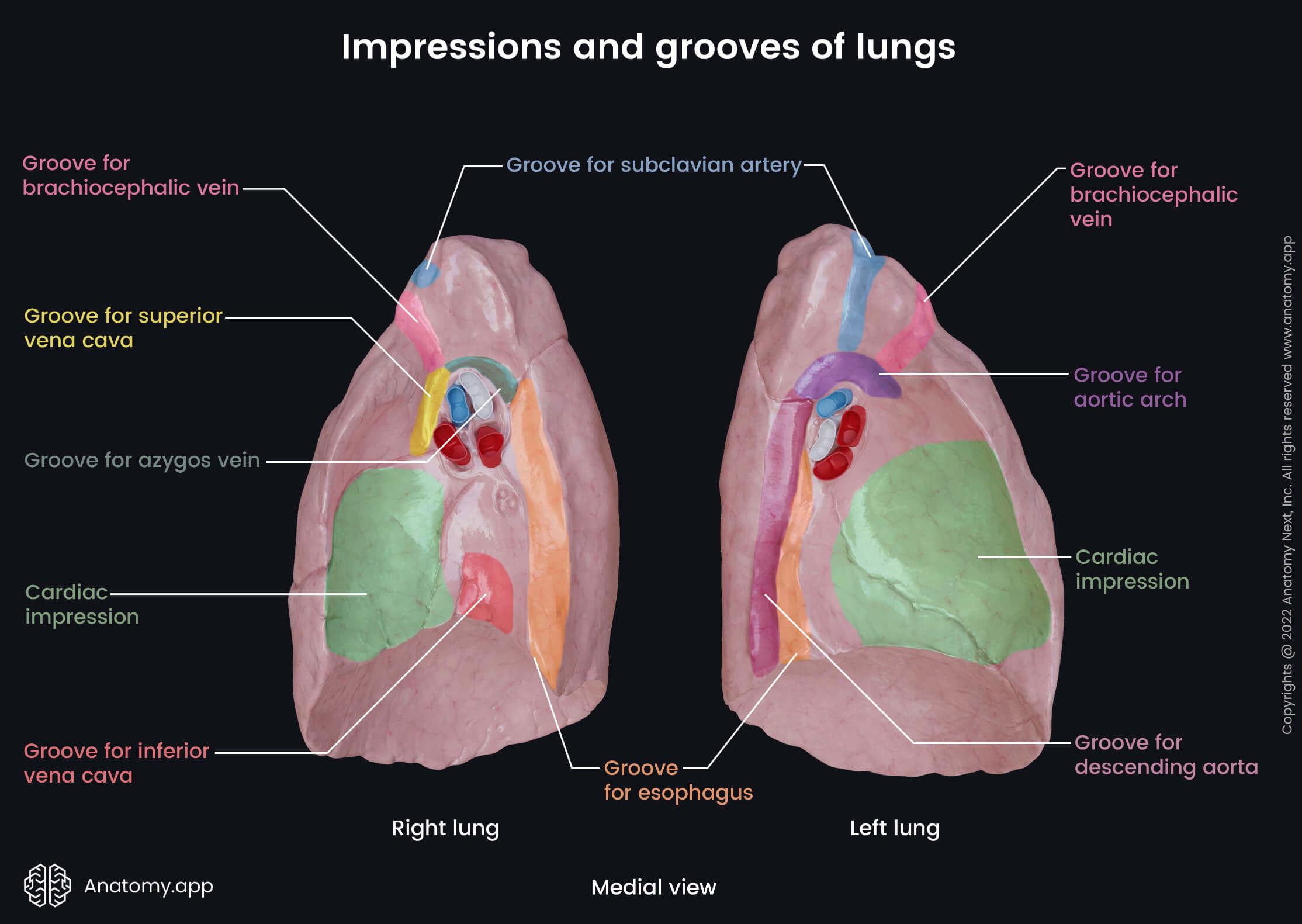
Additionally, the right lung has three more grooves on its medial surface: a groove for the azygos vein that passes over the hilum of the right lung; a groove for the inferior vena cava that is located on the posteroinferior aspect of the medial surface close to the base of the right lung, it descends vertically from the hilum of the right lung; and finally, the medial surface of the right lung also has a groove for the superior vena cava that can be found anterior to the hilum of the right lung, it goes from the cardiac impression to the groove for the azygos vein.
Unlike the right lung, the left lung features a groove for the aortic arch that arises above the hilum and has a curved route. Also, the medial surface of the left lung presents with a groove for the descending aorta. It goes down the medial surface from the groove for the aortic arch to the base of the left lung.
Diaphragmatic surface
The diaphragmatic surface is the inferior surface. It is smooth, concave and corresponds to the convex dome of the diaphragm. On the right side, the diaphragm separates the right lung from the liver. On the left, the diaphragm lies between the left lung, spleen and stomach.
Borders of lungs
Three borders can be distinguished on each lung, and these include the inferior, anterior and posterior borders.
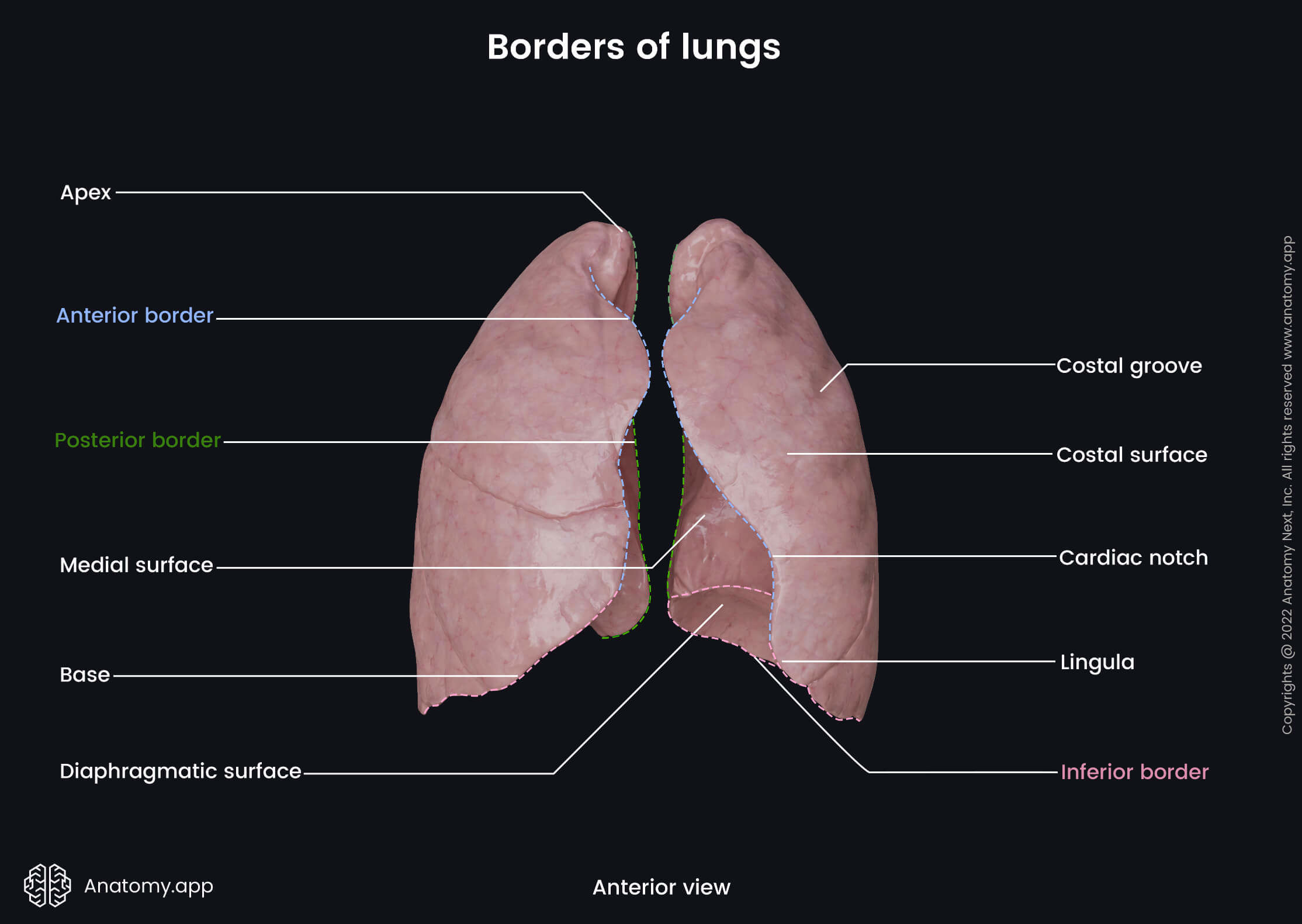
Inferior border
The inferior border of the lung separates the diaphragmatic surface from the costal and medial surfaces. It is thin and sharper at the site where it separates the diaphragmatic surface from the costal surface. But it is more rounded medially where it separates the diaphragmatic surface from the medial surface. The inferior border of the lung extends from the lowest point of the anterior border to the 6th rib at the midclavicular line. Then it continues to the 8th rib at the midaxillary line. Further, it extends posteriorly and reaches the spinous process of the 11th thoracic vertebra (T11).
Anterior border
The anterior border of the lungs is relatively thin and sharp. It corresponds to the pleural reflection and projects into the costomediastinal recess, which is a potential space between the costal pleura and mediastinal pleura. The anterior border of the left lung presents with a deep notch called the cardiac notch. It is created by the apex of the heart. Below the notch is the lingula of the left lung - a tongue-like projection of the left superior lobe.
Posterior border
The posterior border of the lungs is thick, and it separates the costal surface from the medial surface. It extends from the apex of the lung to the inferior border or from the seventh cervical (C7) to the tenth thoracic vertebra (T10).
Hilum of lung
The hilum of the lung (pulmonary hilum) is a large triangular-shaped depressed area situated near the center of the medial surface of each lung. It is located posterior to the cardiac impression and anterior to the fifth through seventh thoracic vertebrae (T5 - T7). The hilum is located more in the posterior aspect of the mediastinal part of the medial surface. It is the site at which various anatomical structures enter and leave the lung via the root of the lung. The area that is situated around the hilum is called the perihilar area.
The visceral pleura covers all surfaces of the lungs except the medial surface at the hilum. Instead, together with the parietal pleura, it overlies the root of the lung and forms the so-called pleural sleeve. Parietal and visceral pleura are continuous at the hilum, and it is a site where both connect. The pleura extends inferiorly from the hilum towards the base of the lung and forms a narrow fold known as the pulmonary ligament.
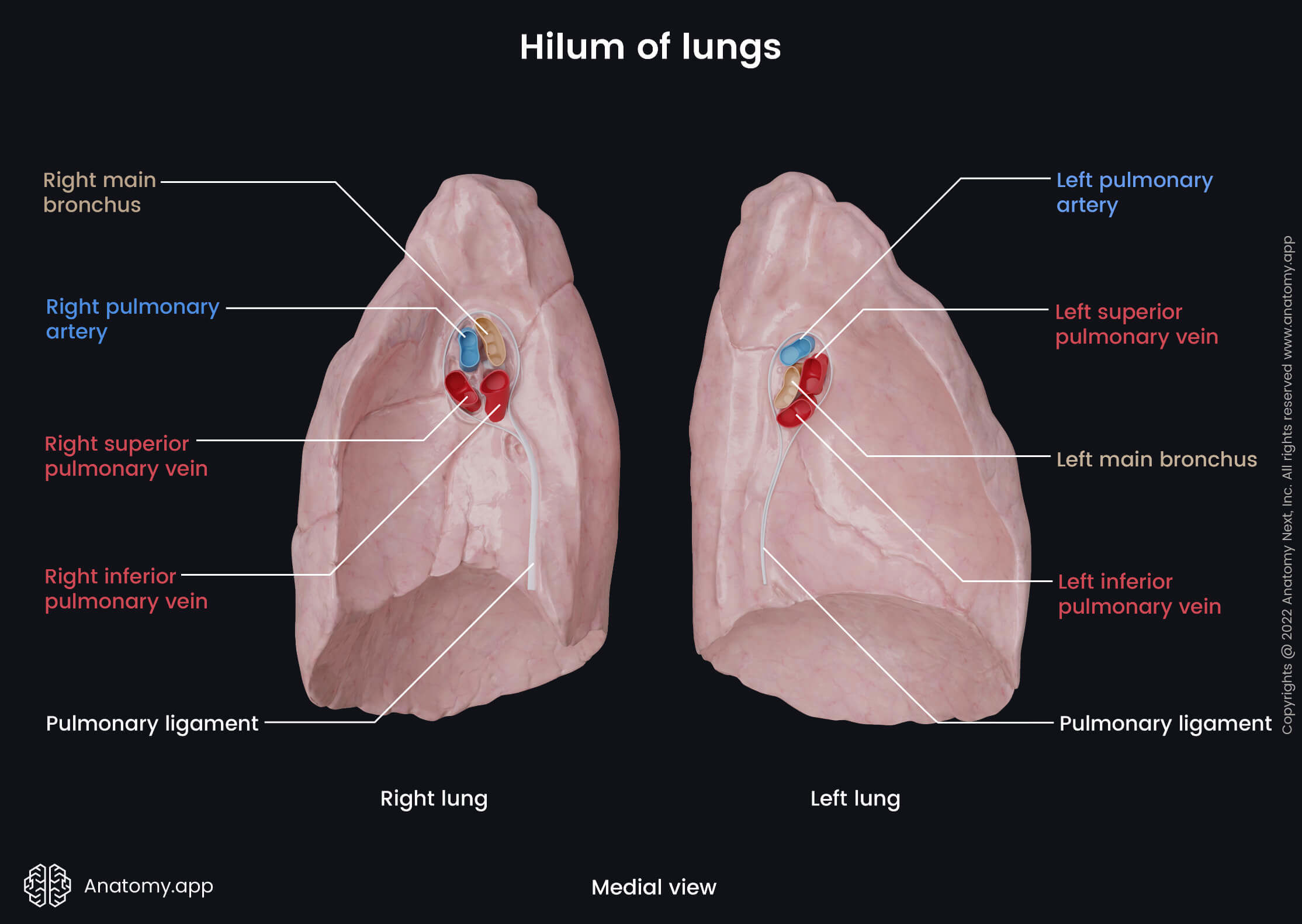
Root of lung
The root of the lung (pulmonary root) is a short and broad stalk formed by a collection of structures that enter and leave the lung and connect it to the heart, trachea and surrounding anatomical structures. The content of the pulmonary root includes the following:
- Main (principal) and lobar bronchi
- Pulmonary artery
- Superior and inferior pulmonary veins
- Bronchial arteries (one on the right side and two on the left)
- Bronchial veins
- Anterior and posterior pulmonary nerve plexuses
- Lymphatic vessels and bronchopulmonary lymph nodes
- Loose connective tissue
The topography and sequence of structures found within the pulmonary roots are different for both lungs. In the right lung, the most superiorly located is the right main (principal) bronchus, the right pulmonary artery is in the middle, while the most inferior are the right superior and inferior pulmonary veins. In the left lung, the left pulmonary artery is the most superior, the left main (principal) bronchus lies in the middle, and the left inferior pulmonary vein is the most inferiorly located. Antero-inferior to the left pulmonary artery and anterior to the left main (principal) bronchus is the left superior pulmonary vein.
The roots of the lungs are related to other anatomical structures, most of which are blood vessels and nerves. The root of the right lung is located posterior to the superior vena cava, part of the right atrium of the heart and inferior to the azygos vein. The root of the left lung is situated beneath the aortic arch and lies anterior to the descending thoracic aorta. Anterior to each root are the phrenic nerves, anterior pulmonary plexus and the pericardiacophrenic artery and vein. The vagus nerve (CN X) and posterior pulmonary plexus are located posterior to each root.
Difference between right and left lung
The right lung is situated on the right side of the heart and mediastinum. As mentioned before, the right lung is shorter than the left due to the liver lying beneath it, causing the right dome of the diaphragm to be higher. Also, the right lung is wider than the left as the left lung has a more prominent cardiac impression. Therefore, the right lung has a greater capacity, and it weighs more than the left lung.
The left lung is situated on the left side of the mediastinum and heart. As mentioned previously, it is more narrow than the right lung because the left lung contains a prominent cardiac impression on its medial surface. The anatomical division of the left lung also differs from the right one, which is described further in this article.
Lobes, fissures and segments of lungs
Each lung is divided into three or two smaller sections called lobes separated by fissures. Every lobe can be subdivided into even smaller portions called bronchopulmonary segments. A bronchopulmonary segment is the anatomical, physiological and surgical unit of the lungs, and surgical removal of a segment does not affect the functions of other segments. Each segment can be further split into even smaller parts called lobules. They are hexagonal structures and the smallest subdivisions of the lungs visible to the naked eye.
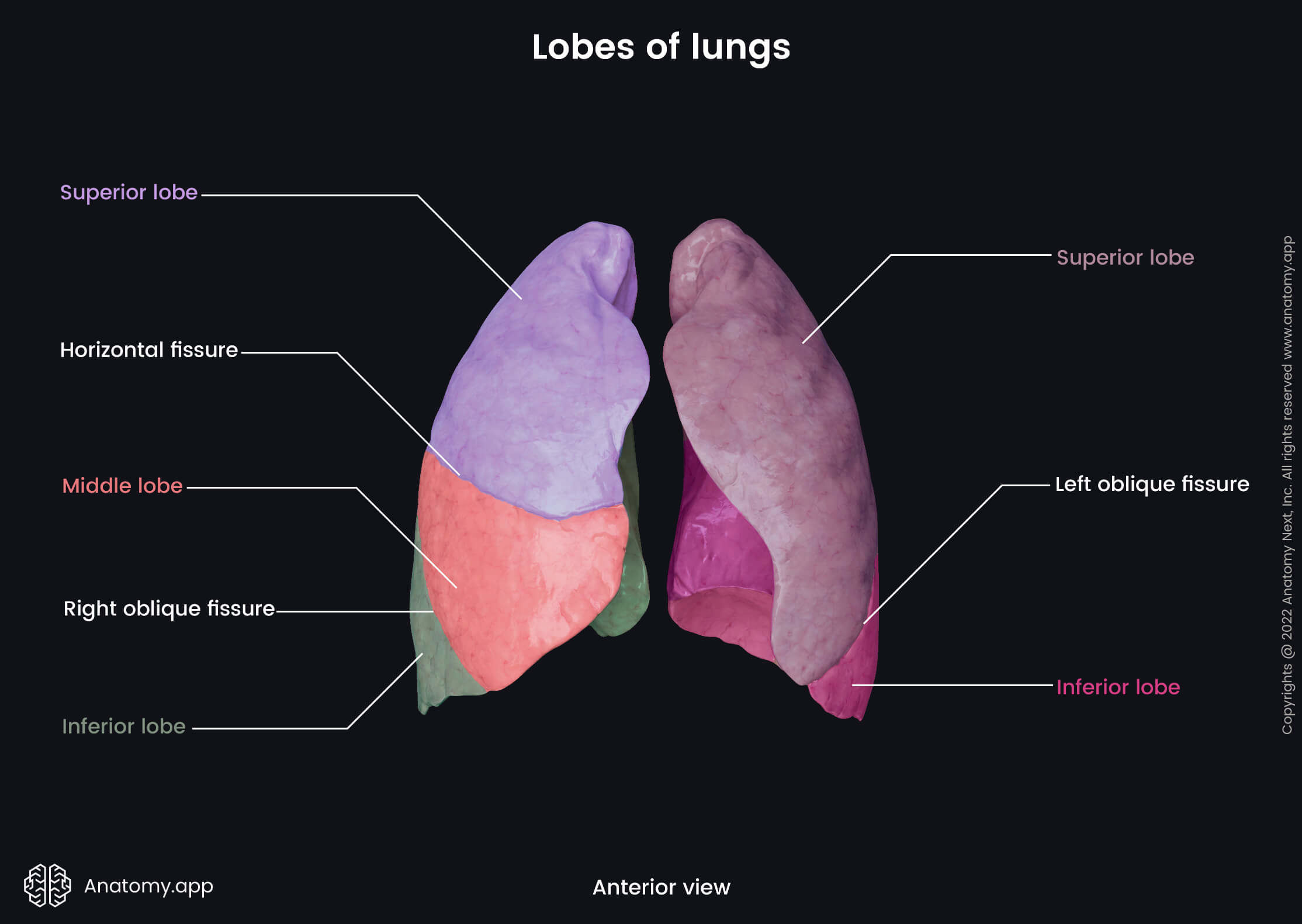
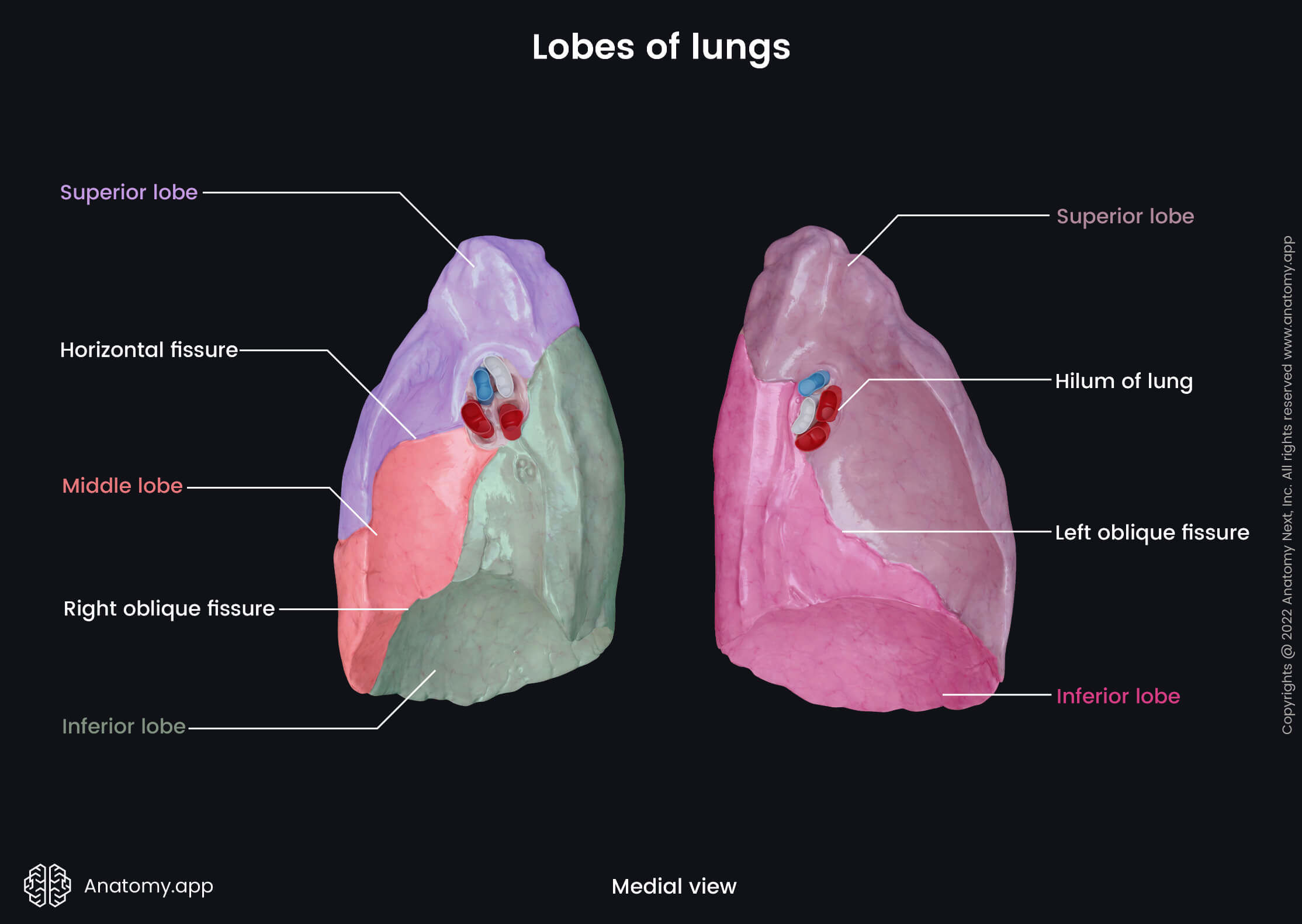
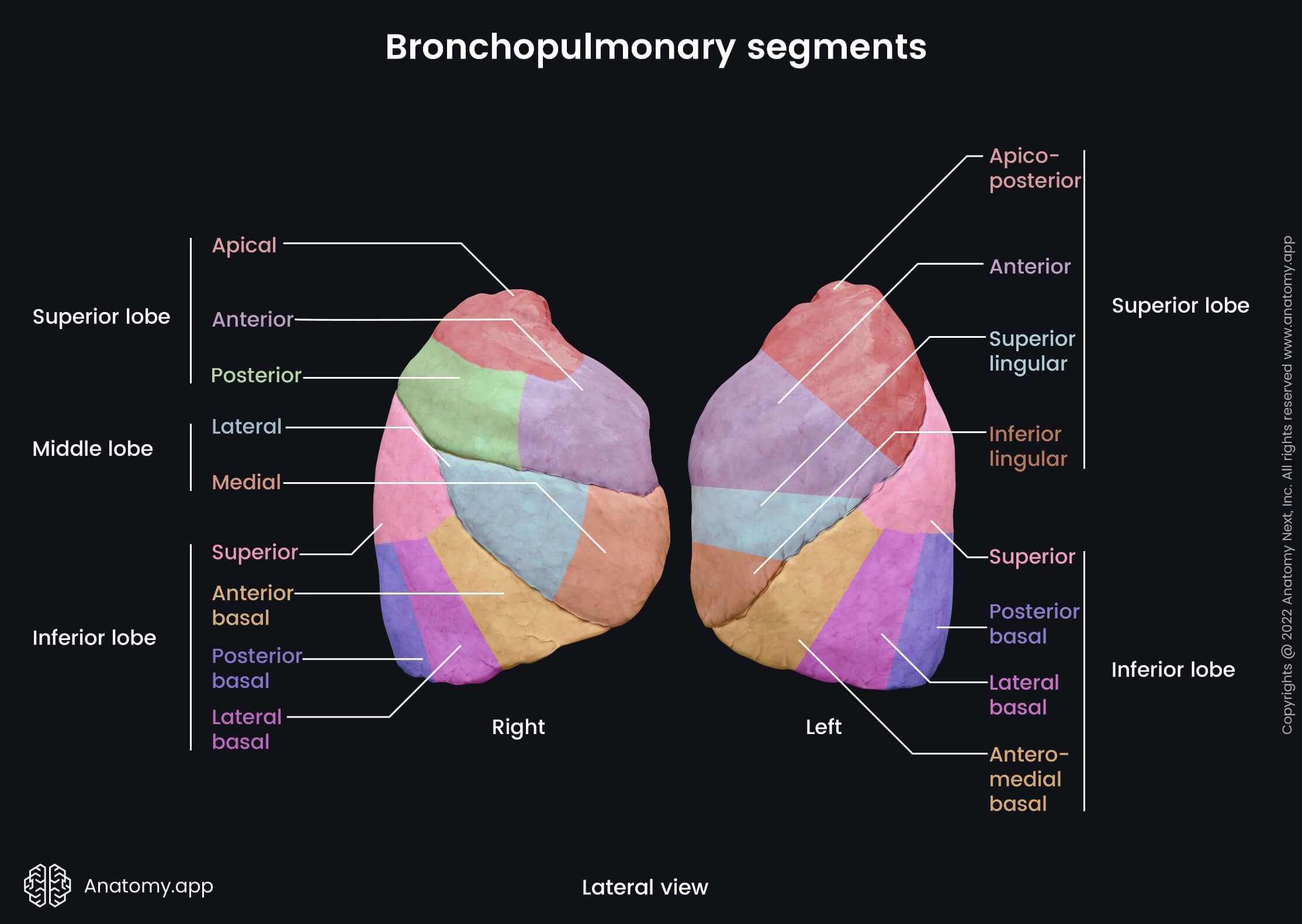
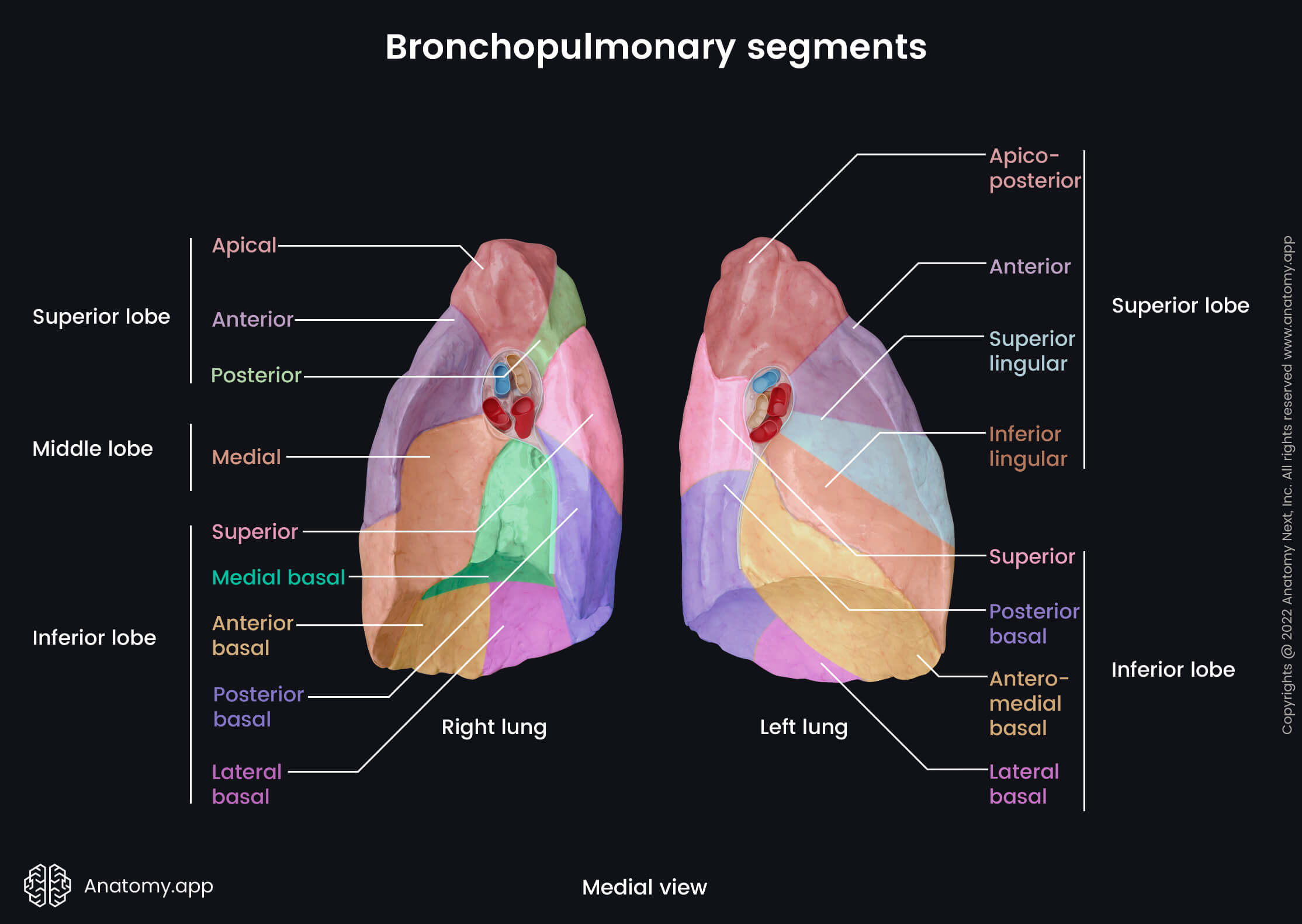
The bronchopulmonary segments appear more or less pyramidal in shape, and they are separated from each other by a layer of connective tissue. The bases of the segments face the outer surfaces of the lung and pleura, while their apices are directed towards the center of the lung and hilum. Through the central aspects of each bronchopulmonary segment, the segmental bronchi and artery pass and give branches. In contrast, the segmental veins are located in the connective tissue between adjacent segments. Each lung contains a different amount of lobes and fissures, as well as segments.
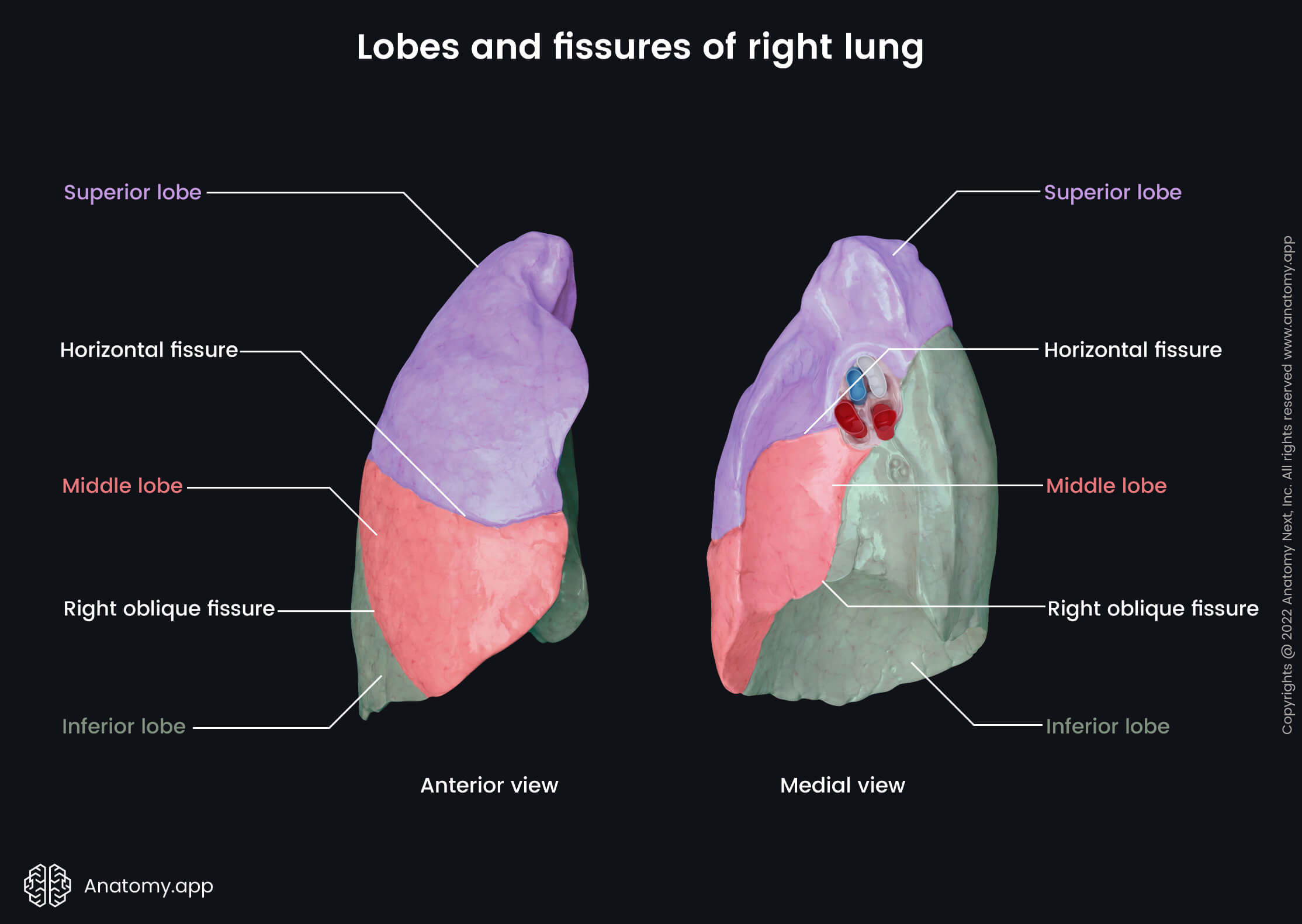
Lobes and fissures of right lung
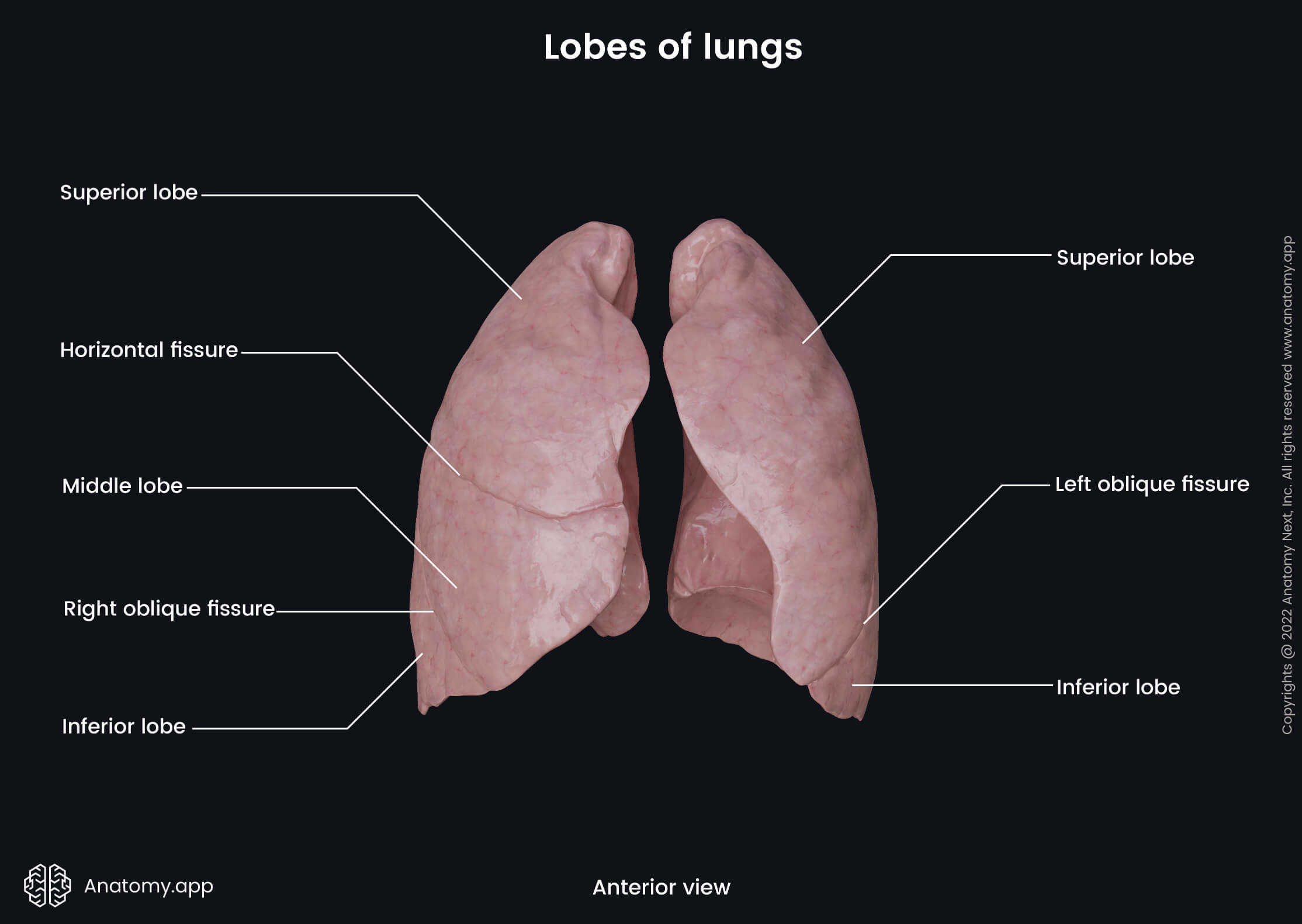
The right lung is divided into three lobes by two fissures. The lobes of the right lung include the superior, middle and inferior lobes, while the fissures separating them are called the right oblique fissure and horizontal fissure.
The right oblique fissure, also known as the right major or great fissure, separates the inferior lobe from the middle and superior lobes. This fissure begins at the level of the spinous process of the fourth thoracic vertebra (T4). It goes obliquely forward and downward along the costal surface of the right lung. The right oblique fissure crosses the fifth intercostal space laterally and ends at the inferior border of the right lung. Once the fissure crosses the fifth intercostal space, it follows the contour of the sixth rib to reach the sixth costochondral joint.
The horizontal fissure, also known as the minor fissure, is a short fissure that separates the superior and middle lobes. It arises from the right oblique fissure at the right midaxillary line. The horizontal fissure goes along the fourth rib and fourth intercostal space forward and downward to reach the anterior border of the right lung.
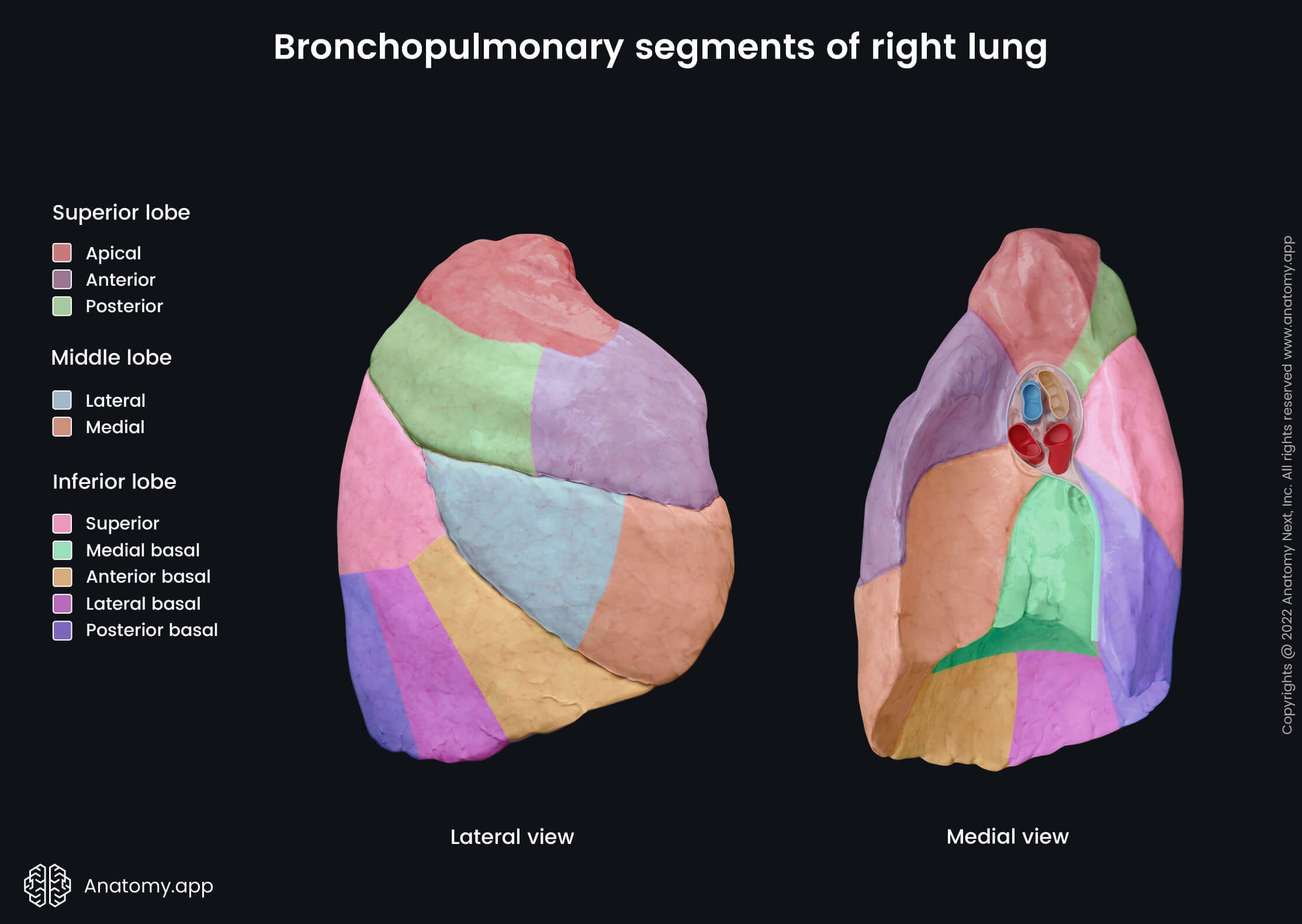
Bronchopulmonary segments of right lung
The right lung has ten bronchopulmonary segments. Each lobe is composed of a different amount of segments, and they are listed below.
The superior lobe of the right lung has three bronchopulmonary segments:
The middle lobe contains two bronchopulmonary segments:
Finally, the inferior lobe of the right lung consists of five segments:
- Superior segment
- Anterior basal segment
- Medial basal segment
- Lateral basal segment
- Posterior basal segment
Lobes and fissure of left lung
The left lung is divided into two lobes - superior and inferior - by the left oblique fissure. The inferior lobe is larger than the superior one. The left oblique fissure, also known as the left major or great fissure, is more vertical than the right oblique fissure. The left oblique fissure usually arises between the spinous processes of the third and fourth thoracic vertebrae (T3, T4) or from the spinous process of the third thoracic vertebra (T3). Similarly to the right oblique fissure, it crosses the fifth intercostal space laterally and follows the contour of the sixth rib to reach the inferior border of the left lung and sixth left costochondral joint.
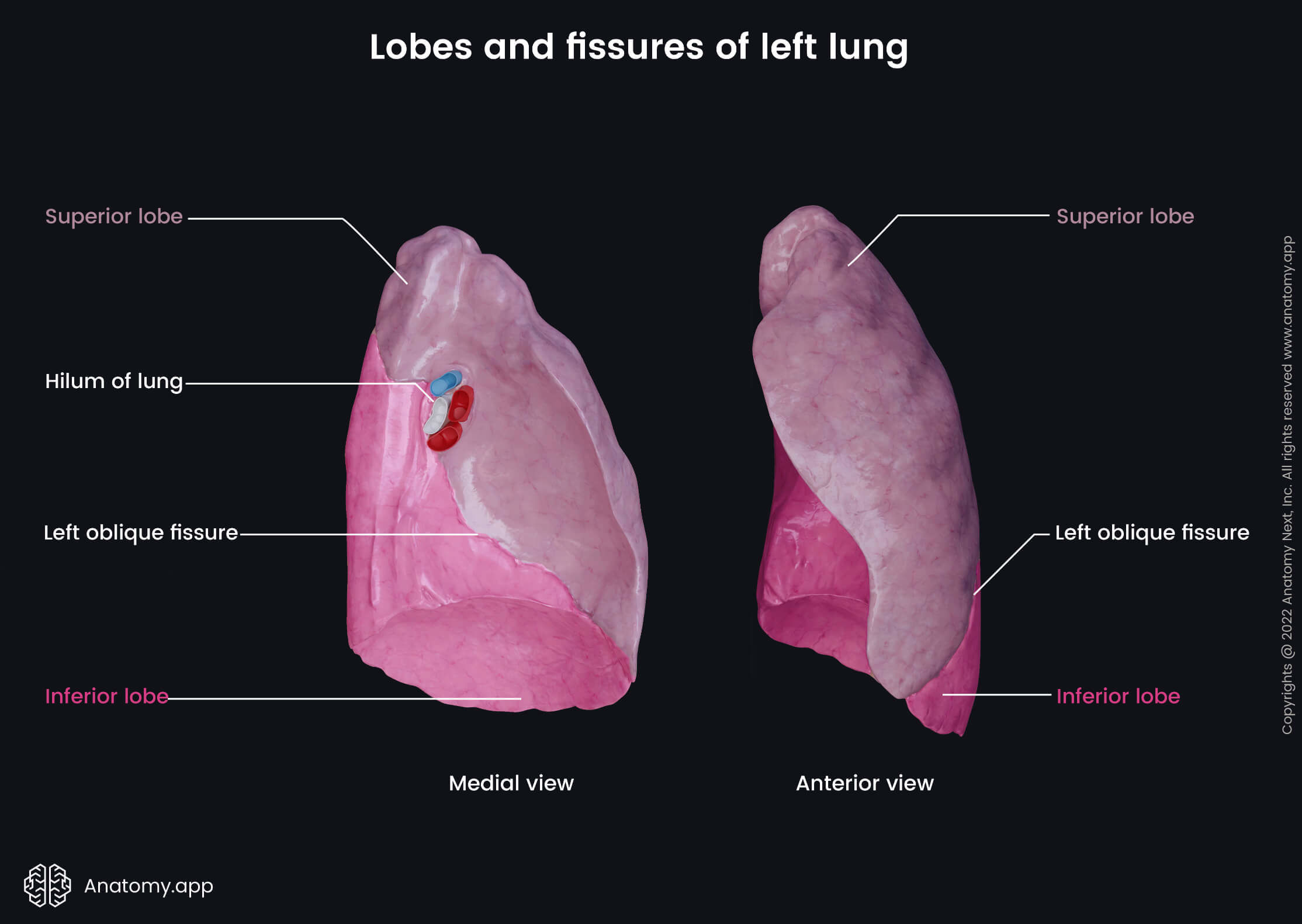
Bronchopulmonary segments of left lung
The left lung has eight bronchopulmonary segments. Each lobe of the left lung consists of four segments listed below. The superior lobe of the left lung consists of the following four bronchopulmonary segments:
The inferior lobe of the left lung also has four bronchopulmonary segments:
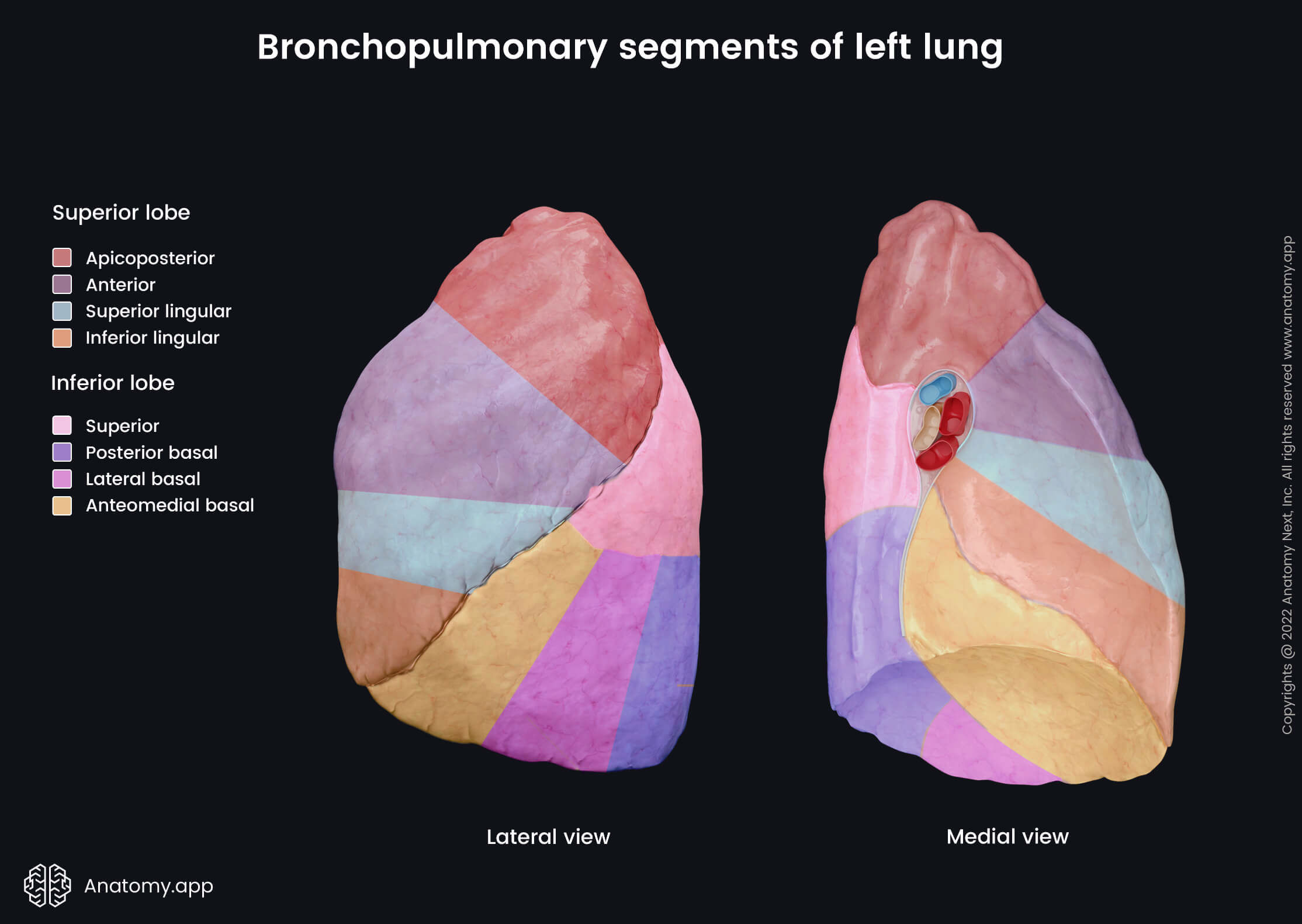
Lung histology
Microscopically, the lungs bear a strong resemblance to the structure of an alveolar gland. The lungs contain two parts (also known as trees) - bronchial and alveolar trees. Most of the bronchial tree extends into the lungs, but it does not form the lung parenchyma. It is the conducting part that transmits the air from the external environment to the site of the gas exchange. In contrast, the terminal portions of the alveolar tree known as the alveoli form the lung parenchyma. Therefore, the alveolar tree is the respiratory part of the lungs where the gas exchange happens.
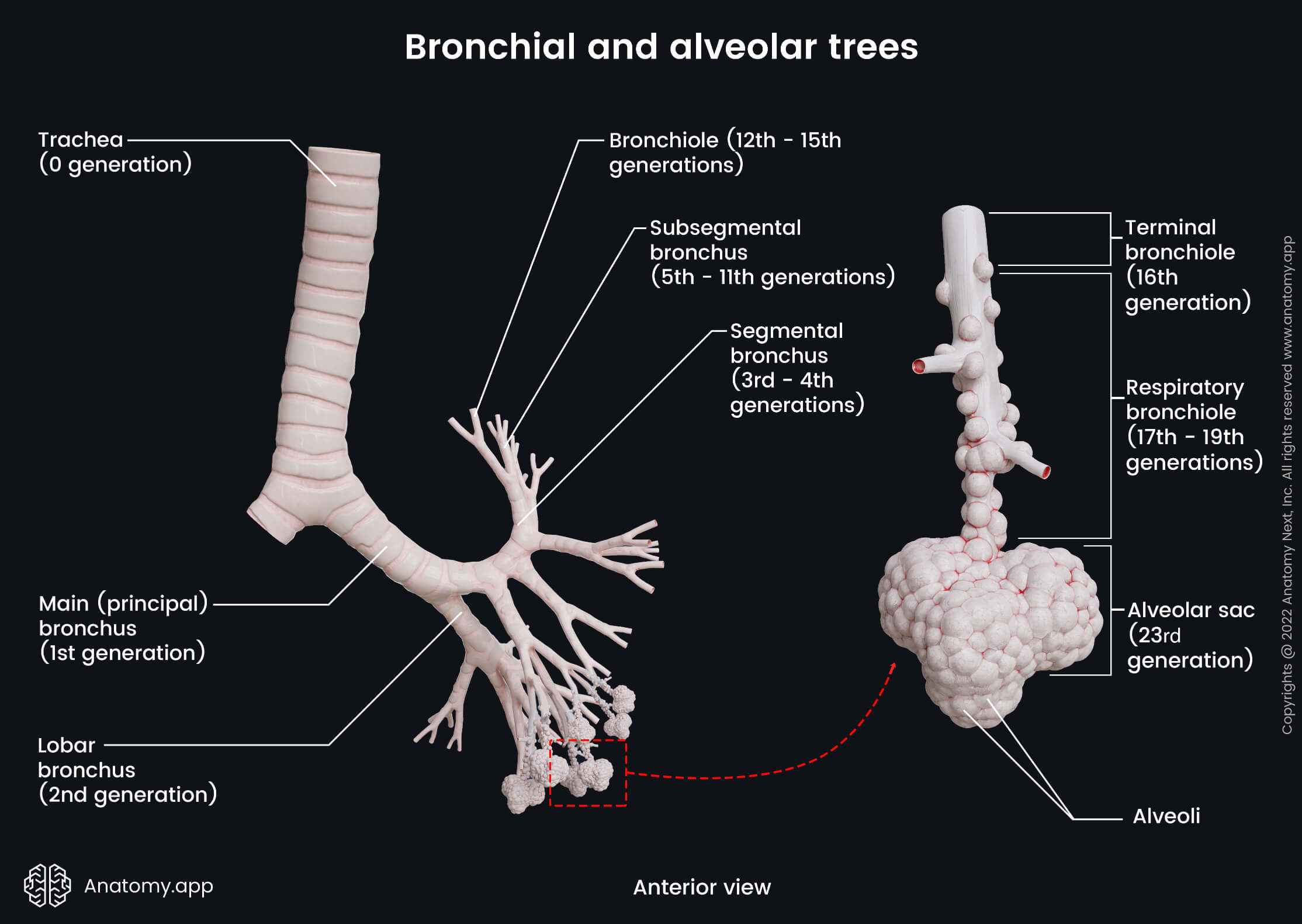
Bronchial tree
The bronchial tree starts at the tracheal bifurcation with the right and left principal (main) bronchi that branch into two or three lobar bronchi depending on the lung. The lobar bronchi further divide into several segmental bronchi that subdivide into even smaller subsegmental bronchi. Finally, the subsegmental bronchi branch into bronchioles. The final bronchiole of the bronchial tree is called the terminal bronchiole, and the bronchial tree ends with it. The bronchi are classified as parts of the respiratory system separated from the lungs, therefore, in this article we do not discuss their histology. To learn in detail about the histology of the bronchial wall, go to our article dedicated to bronchi.
Alveolar tree
A terminal bronchiole is the origin of the alveolar tree. All structures that form the alveolar tree are included in a pulmonary acinus. The pulmonary acini are located distally to the terminal bronchioles and give the alveolar tree the appearance of a bunch of grapes. The pulmonary acinus contains respiratory bronchioles dividing into alveolar ducts that end with alveolar sacs containing alveoli. The respiratory bronchiole is considered a transition structure between the bronchial and alveolar trees. The walls of the alveolar sacs and ducts are composed of the alveoli. However, few alveoli usually are also visible within the walls of the respiratory bronchioles. Alveoli are structural and functional units of the respiratory system. Every lung contains approximately 300-400 million alveoli.
Respiratory bronchioles
The respiratory bronchioles structurally are very similar to the terminal bronchioles. They are lined with simple ciliated cuboidal epithelium proximally, but distally the cilia might be absent as they gradually disappear. The respiratory bronchioles contain small amounts of non-ciliated Clara cells that produce and secrete surfactant components, and they become the dominant cells in the distal portions. The epithelium of the respiratory bronchiole lacks Goblet cells. Beneath the epithelium is the connective tissue with elastic fibers and bundles of smooth muscle cells. The smooth muscle layer is very thin. Distally, the amount of the alveoli within the wall of the respiratory bronchiole gradually increases.
Alveolar ducts, alveolar sacs and alveoli
The alveolar ducts give rise to numerous alveolar sacs and alveoli. Therefore, the walls of the alveolar ducts contain only the alveolar sacs and alveoli. Like the walls of the respiratory bronchioles, the walls of the alveolar ducts still have small amounts of smooth muscle cells. And the alveolar ducts are the most distal respiratory structures containing muscles. The alveolar sacs are sac-like outpouchings (outpocketings) composed of alveoli clusters. The alveolar ducts and alveoli are lined by simple squamous epithelium.
The alveoli function as the primary gas exchange site between the inhaled air and blood within the pulmonary capillaries. They are specialized blind-ending and sac-like structures that give a spongy appearance to the lungs. The alveoli are the terminal part of the airways, and they are lined with a very thin, simple epithelium. Between the alveoli is a very slender layer of connective tissue containing capillaries and nerve fibers. The wall of the alveoli forms the respiratory membrane together with the capillary wall. Gas exchange occurs through this membrane, which is known as the blood-gas barrier. The barrier is formed by the following three layers: squamous epithelial cells (type I pneumocytes) of an alveolus, endothelial cells of the capillary, and an interstitial layer in between. The interstitial layer consists of fused basement membranes of the pneumocytes and capillary endothelium.
The epithelial cells of the alveolar wall are called the pneumocytes. There are two types of pneumocytes - type I and type II. The wall of alveoli mostly contains the type I pneumocytes, which are flattened simple squamous cells providing gas exchange. Type II pneumocytes are dome-shaped cuboidal epithelium cells that secrete surfactant. Surfactant reduces surface tension and prevents the lungs from collapsing. The connective tissue of alveoli contains many macrophages, also called dust cells, that derive from blood monocytes and phagocyte foreign particles such as dust, viruses, microbes and dead cells.
Lung functions
The primary function of the lungs is to provide the external and internal respiration processes. The lungs fill up with air during external respiration by inhaling it from the environment. The gas exchange happens at the level of the alveoli between the pulmonary capillaries containing carbon dioxide and air in the lungs that is rich in oxygen. Once the exchange has occurred, the air now rich in carbon dioxide is released back into the atmosphere by exhalation. This process is also referred to as breathing. But during internal respiration, the gas exchange happens at the level of the body capillaries between blood containing oxygen and body cells rich in carbon dioxide. However, respiration is not the only function provided by the human lungs. Other functions include the following:
- Thermoregulation of the body - lungs remove excess heat by insensible perspiration from the surfaces of the airways;
- Synthetic function - lungs produce various substances such as heparin, surfactant, histamine, prostaglandins;
- Regulation of hemostasis - lungs produce thromboplastin and heparin; therefore, they are involved in the physiological processes that stop the bleeding from a blood vessel once it occurs;
- Regulation of the water balance - lungs provide insensible perspiration from the surfaces of the airways;
- Regulation of acid-base and pH balance - lungs hypoventilate to compensate for metabolic alkalosis and hyperventilate during metabolic acidosis;
- Regulation of blood pressure - endothelial cells of lung capillaries contain angiotensin-converting enzyme; therefore, angiotensin I is converted to angiotensin II in lung capillaries;
- Excretion and removal of various substances - lungs remove some substances, including amines, and, for example, in the case of uremia, urea is partly excreted through the lungs;
- Immune defense against various antigens - provided by the immunoglobulin A, complement activation, lymphocytes, plasma cells, macrophages and leukocyte recruitment;
- Mucociliary clearance - a primary defense mechanism of the lungs, in which respiratory epithelial cells, with the help of their cilia (hair-like extensions) and mucus, move foreign particles such as dust and microorganisms upward and out of the airways;
- Blood storage and reservoir function - the lungs can accumulate a massive amount of blood if necessary and therefore function as a blood reservoir;
- Blood filtering function - lungs filter tiny gas bubbles and small blood clots that can appear in the bloodstream;
- Phonation function - expiration of the air sets the vocal cords into vibration;
- Drug delivery - lungs can be a route for anesthesia and drugs that are administered through inhalation.
External respiration process
As mentioned previously, the main function of the lungs is to provide external and internal respiration. The external respiration is known as the breathing process, and it consists of two main phases - inspiration and expiration.
Inspiration
Inspiration is an active process. It involves inspiratory muscles and happens because of their contractions. The main inspiratory muscles include the diaphragm and external intercostal muscles.
When the diaphragm and muscles of inspiration contract, the diaphragm pulls the diaphragmatic surfaces of the lungs downward. But the inspiratory muscles raise the rib cage. It increases the intrathoracic volume and creates reduced intrapulmonary pressure. The intrapulmonary pressure is decreased to less than the atmospheric pressure. It results in air being drawn through the upper respiratory tract into the trachea, lower airways and then into the alveoli, where the gas exchange occurs.
During peaceful inspiration, the inspiratory muscles are the diaphragm, external intercostal muscles and the interchondral parts of the internal intercostal muscles. But during intensive or forced inspiration, the accessory muscles of the inspiration also participate. They mainly include the sternocleidomastoid, scalene muscles, serratus anterior, pectoralis minor and pectoralis major.
Expiration
Opposite to inspiration, expiration is mostly a passive process provided by the elasticity of the lungs and thorax. During expiration, the diaphragm relaxes, and the elastic recoil of the lungs, thoracic wall, and abdominal structures compresses the lungs and expels the air.
During peaceful breathing, the expiration results from passive recoil of lungs and rib cage. Some muscles of the expiration participate during forced expiration. They are the internal intercostal muscles (except for the interchondral parts) and muscles of the anterior abdominal wall - rectus abdominis, transverse abdominis, external abdominal oblique and internal abdominal oblique muscles.
Neurovascular supply of lungs
Arterial blood supply and venous drainage of lungs
The arterial blood supply and venous drainage of the lungs includes two circulation systems - pulmonary and bronchial. The bronchial circulation is part of the systemic circulation, and it is formed by the bronchial arteries and bronchial veins. The bronchial arteries supply oxygenated blood to the lungs. The bronchial veins collect deoxygenated blood from the bronchi and hila of the lungs and mostly drain into the pulmonary veins.
In contrast, the pulmonary circulation is provided by the pulmonary arteries and pulmonary veins. The pulmonary arteries receive deoxygenated blood from the right ventricle of the heart via the pulmonary trunk. Gas exchange happens at the level of the lung alveoli, and deoxygenated blood becomes oxygenated. Oxygenated blood from the long tissue reaches the left atrium of the heart via four pulmonary veins.
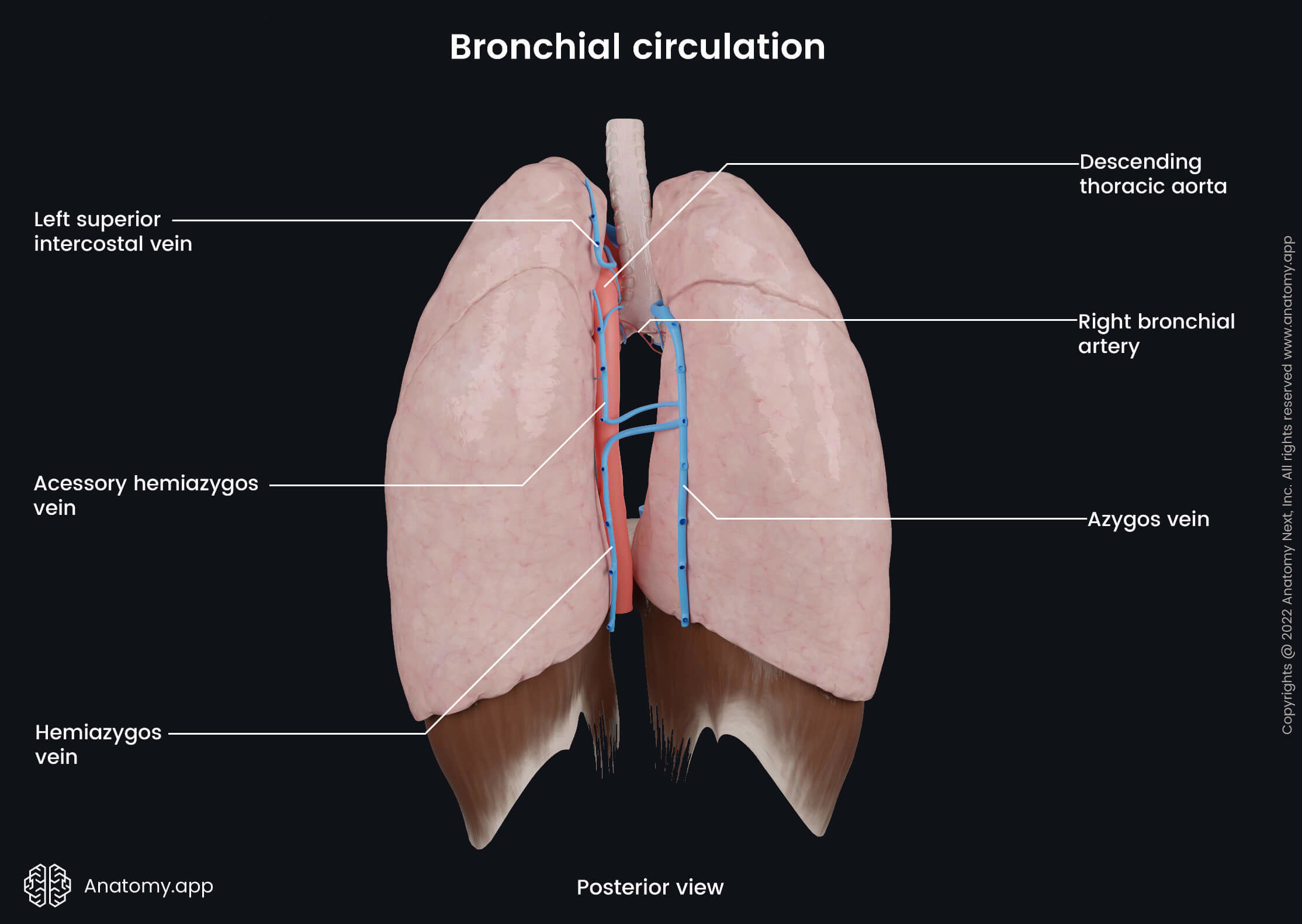
Bronchial circulation
Bronchial arteries
The left lung typically is provided by two bronchial arteries, while the right lung has only one. The bronchial arteries primarily provide blood supply to the trachea, bronchi, middle-third of the esophagus, roots of the lungs, visceral pleura, part of the pericardium, pulmonary vessels and aorta, vagus nerve (CN X) and supporting connective tissue of the lungs. The bronchial arteries run with and branch along with the bronchi, ending at the level of the respiratory bronchioles.
Both left bronchial arteries (superior and inferior) usually arise from the descending thoracic aorta. The superior left bronchial artery supplies part of the aortic arch, but the inferior left bronchial artery supplies the bronchi and connective tissue of the pulmonary hilum. The origin of the right bronchial artery is variable. However, it usually arises from the intercostobronchial trunk.
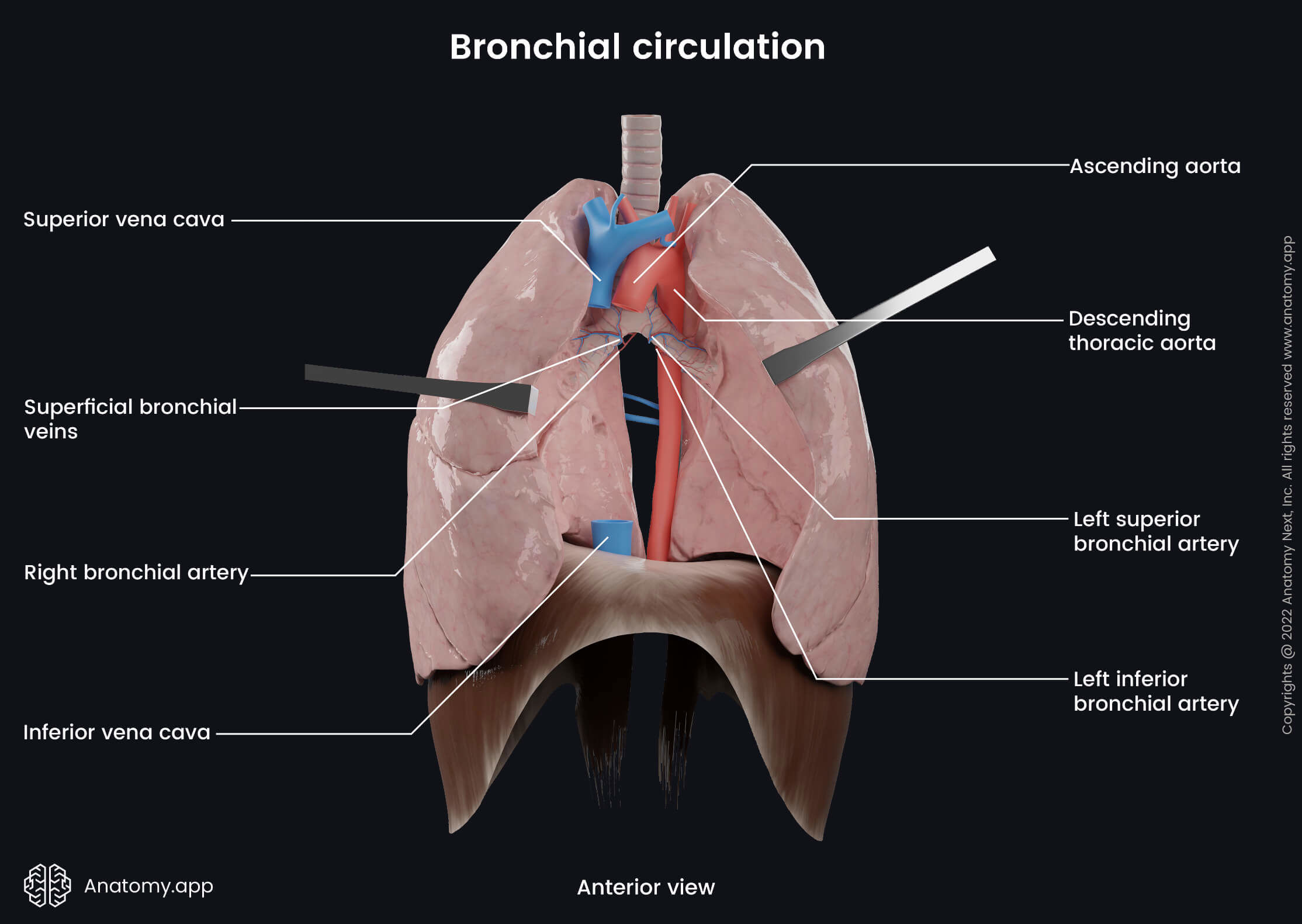
Bronchial veins
The bronchial veins are small veins that participate in the venous drainage of the lungs. They collect deoxygenated blood from the areas supplied by the bronchial arteries. Drainage happens through two systems - superficial and deep. The superficial bronchial veins drain the extrapulmonary bronchi, visceral pleura at the hilum and hilar lymph nodes. The deep bronchial veins are formed by the intrapulmonary bronchiolar venous plexuses. The deep bronchial veins receive venous blood from the intrapulmonary bronchi.
The superficial bronchial veins drain into the azygos vein on the right side and the left superior intercostal vein or the accessory hemiazygos vein on the left side. The deep bronchial veins drain into the pulmonary veins or directly into the left atrium of the heart.
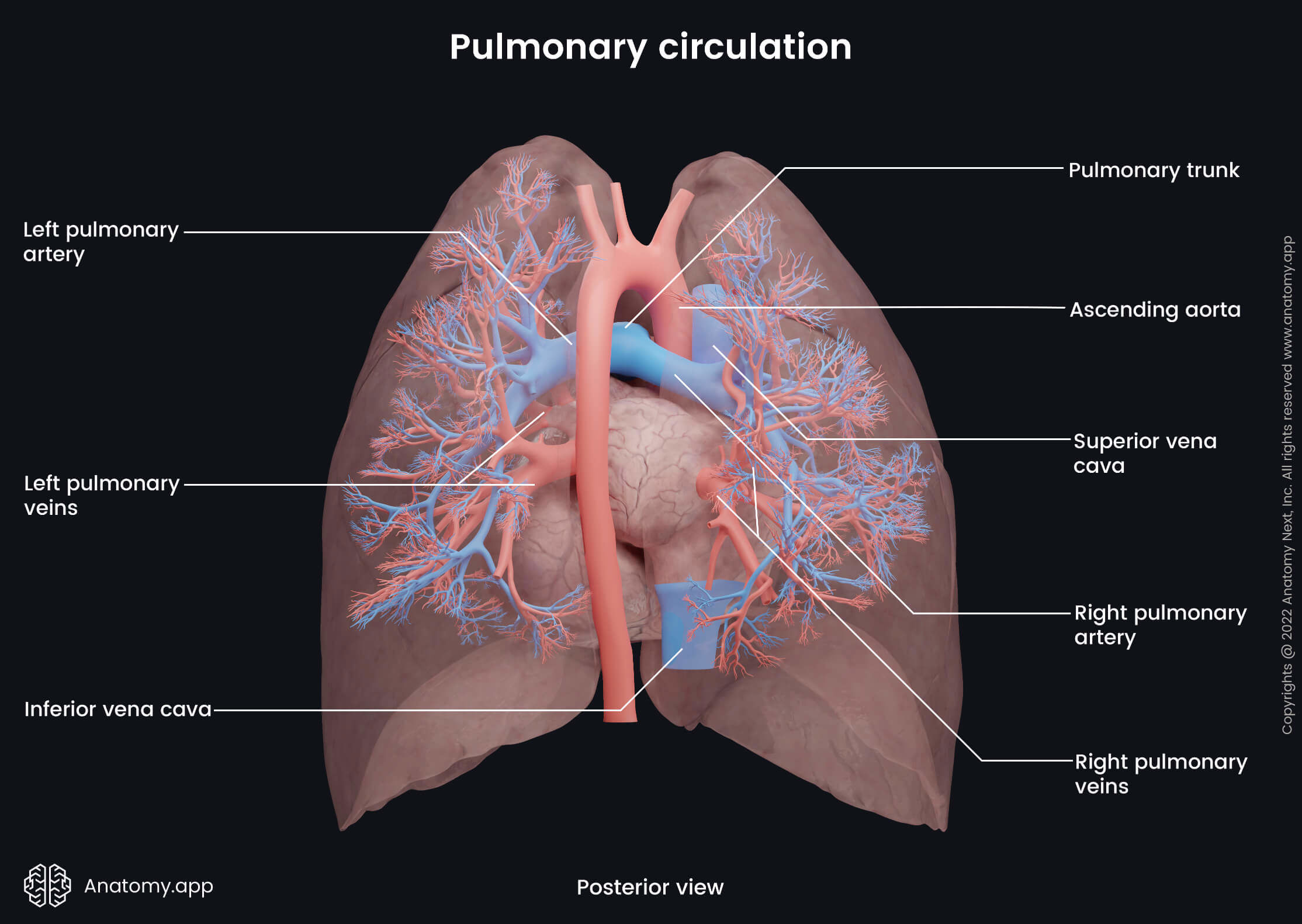
Pulmonary circulation
Pulmonary trunk and pulmonary arteries
The pulmonary trunk arises from the infundibulum (conus arteriosus) of the right ventricle. It passes posteriorly and slightly upwards and crosses the anterior surface of the ascending aorta. It reaches the aortic arch and below it divides into two pulmonary arteries - left and right pulmonary arteries.
The right pulmonary artery passes horizontally to the right side behind the ascending aorta and superior vena cava. And near the pulmonary hilum, it divides into superior, middle and inferior branches, supplying the upper, middle, and lower lobes of the right lung, respectively.
The left pulmonary artery passes posteroinferiorly, enters the hilum of the left lung, and divides into superior and inferior branches, which supply the upper and lower lobes, respectively. The left pulmonary artery also has a branch supplying the lingula.
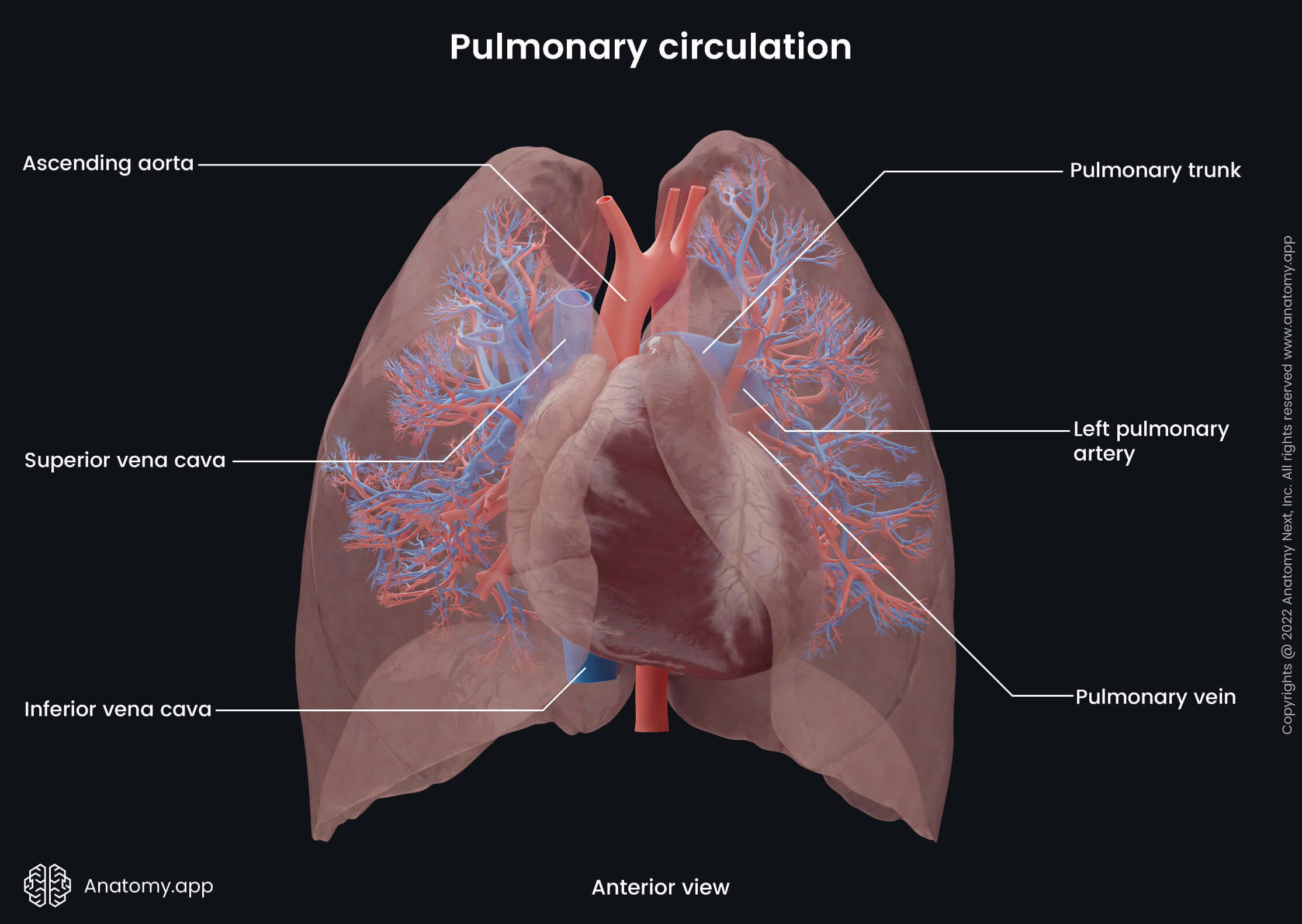
Pulmonary veins
The lungs are drained by two pulmonary veins on each side, which carry oxygenated blood from the lungs to the left atrium of the heart. The pulmonary veins collect blood from the areas supplied by the pulmonary arteries. The veins originate from the pulmonary capillary network that joins together and forms larger vessels. Capillaries form the intrasegmental veins that further unite and form the segmental veins. The segmental veins also merge, forming the intersegmental veins, which combine into the lobar veins. The right lung has three lobar veins, while the left lung has two lobar veins according to the number of lobes each lung has. Finally, the lobar veins merge, forming the four pulmonary veins, which drain the parenchyma of the lungs. The pulmonary veins emerge from each lung at the hilum and flow into the left atrium. On their course, the pulmonary veins also receive the bronchial veins.
Lymphatic drainage of lungs
The lymphatic drainage of the lungs is provided by two lymphatic plexuses - the subpleural lymphatic plexus located below the pleura and the deep lymphatic plexus around the bronchi and bronchioles. The subpleural plexus (also called the superficial plexus) lies under the visceral pleura. It collects lymph from the peripheral lung tissue and drains to the ipsilateral (same side) bronchopulmonary (hilar) lymph nodes at the pulmonary hilum.
The deep plexus lies along the bronchial tree and pulmonary blood vessels, and it drains the bronchial tree and deeper structures of the lungs. Lymphatics from the deep plexus drain into the pulmonary nodes found within the lung parenchyma, and then lymph is carried next to the bronchopulmonary (hilar) nodes.
From the hilar nodes lymph is carried next to the tracheobronchial nodes located around the bifurcation of the trachea. The lower lobes of the lungs are drained via the inferior tracheobronchial nodes, but the superior lobes via the superior tracheobronchial nodes. From the tracheobronchial nodes, lymph further drains to the paratracheal lymph nodes along the trachea and then to the right and left bronchomediastinal trunks. From the bronchomediastinal trunks, lymph is carried to the thoracic duct on the left side and to the right lymphatic duct on the right side.
Innervation of lungs
The lungs receive autonomic nerve supply through the vagus nerve (CN X) and the sympathetic trunk. Sympathetic innervation happens through the upper thoracic and cervical sympathetic ganglia of the sympathetic trunk. Parasympathetic and sensory innervation is provided by the vagus nerve (CN X). Nerves arising from the vagus nerve and sympathetic trunk form two pulmonary plexuses - anterior and posterior. As their names suggest, they lie anterior and posterior to the structures going through the hilum. Both plexuses connect with the cardiac plexuses.
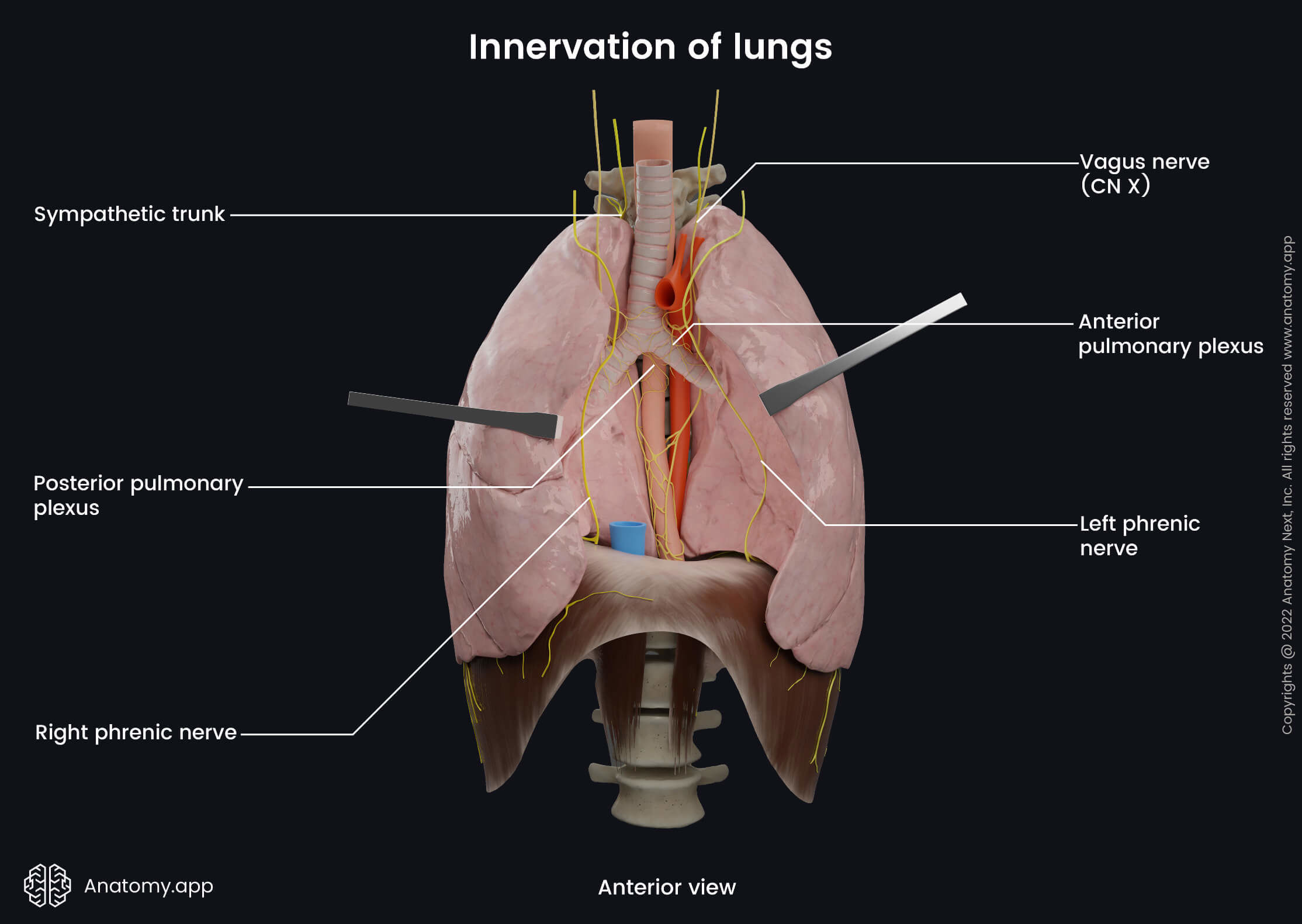
The anterior pulmonary plexus is continuous posteriorly from the superficial cardiac plexus. It includes 2 - 4 branches of the vagus nerve and cervical sympathetic cardiac nerves via the deep and superficial parts of the cardiac plexus. The posterior pulmonary plexus is continuous laterally from the deep cardiac plexus. It is formed by 8 - 18 branches of the vagus nerve and cardiac branches from the second to fifth thoracic sympathetic ganglia.
The parasympathetic nervous system stimulates the secretion from the bronchial glands. Also, it provides contractions of bronchial smooth muscle cells(bronchoconstriction) and the widening (vasodilatation) of the pulmonary vessels. The sympathetic system provides opposite effects. It causes relaxation of the bronchial smooth muscles (bronchodilation) and narrowing (vasoconstriction) of the pulmonary vessels.
Pleura
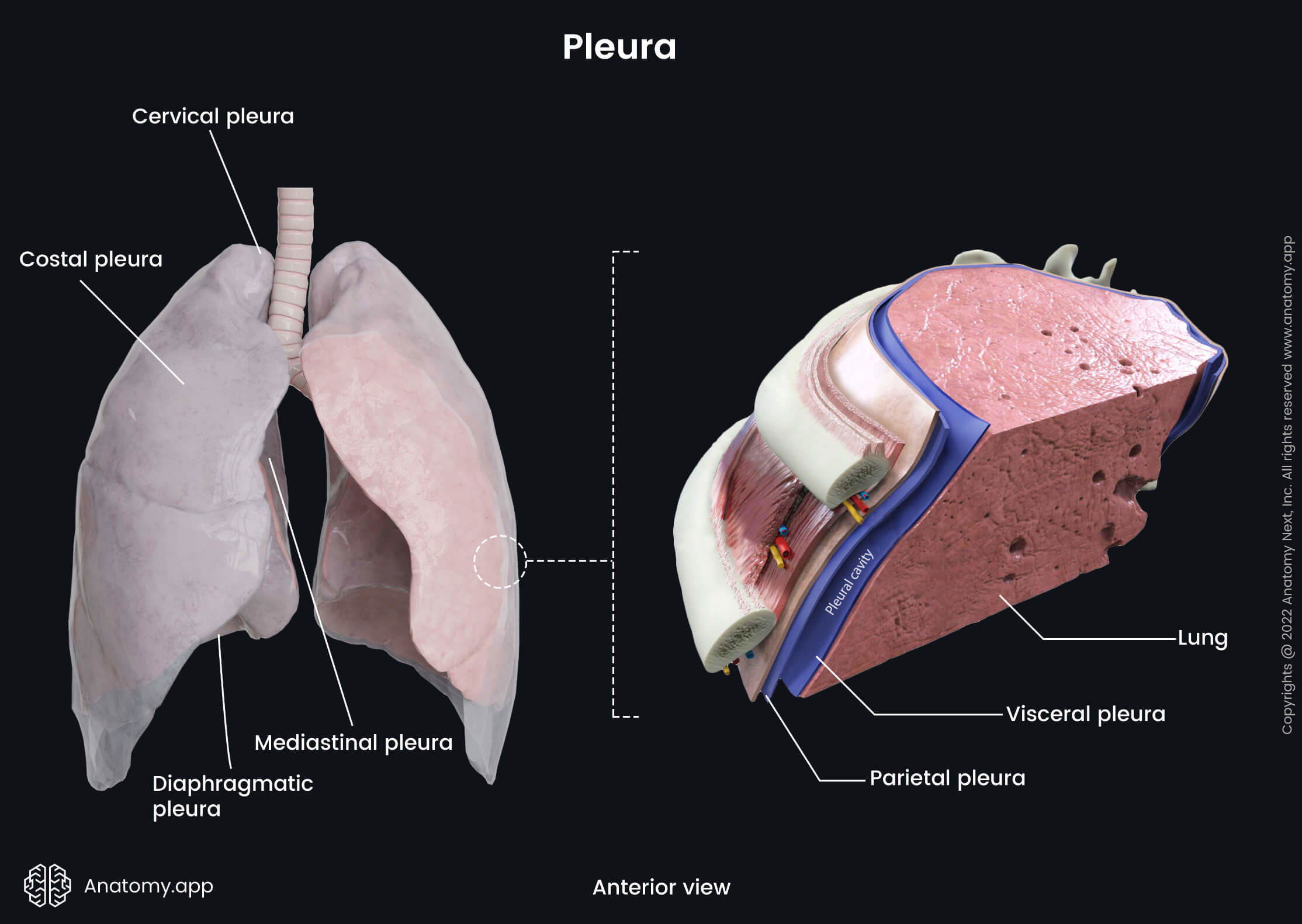
The term pleura describes a thin serous membrane that covers each lung and lines the thoracic cavity. It is formed by two layers: parietal and visceral. The parietal layer (also known as the parietal pleura) is attached to the internal surface of the thoracic wall. The visceral layer (or visceral pleura) surrounds the lungs and extends into the fissures between the lobes of the lungs.
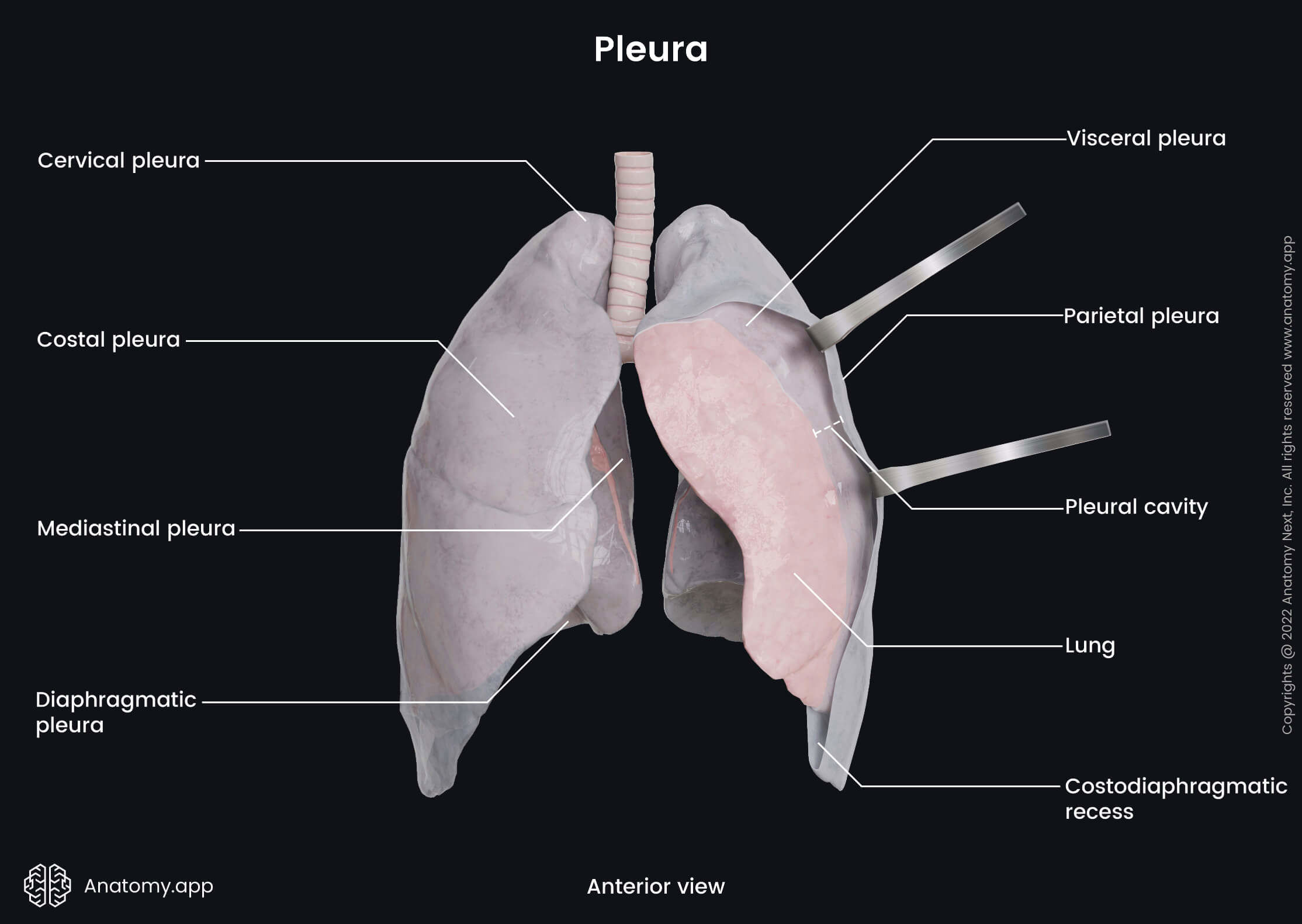
Both layers are continuous with each other at the pulmonary hilum. The parietal pleura is the thicker of the two. Moreover, it can be further subdivided into four portions. They are named according to the adjacent anatomical structures. The four parts of the parietal pleura are:
- Costal pleura - lines the thoracic walls along the ribs;
- Mediastinal pleura - lines the central aspects of the thorax along the mediastinum;
- Diaphragmatic pleura - lines the thoracic cavity along the superior surface of the diaphragm;
- Cervical pleura (also known as the pleural cupula) - lines the dome that forms at the apex of the lung.
Between both pleural layers is a potential space known as the pleural cavity. This space contains a small amount of a serous fluid that lubricates the membranes allowing them to slide along each other during breathing. The fluid also produces surface tension, allowing the lungs to expand together with the thorax during inspiration.
References:
- Broaddus, V. C., Ernst, J., King, T., & Lazarus, S. (2021). Murray & Nadel’s Textbook of Respiratory Medicine, 2-Volume Set (7th ed.). Elsevier.
- Drake, R., Vogl, W., & Mitchell, A. (2019). Gray’s Anatomy for Students: With Student Consult Online Access (4th ed.). Elsevier.
- Gray, H., & Carter, H. (2021). Gray’s Anatomy (Leatherbound Classics) (Leatherbound Classic Collection) by F.R.S. Henry Gray (2011) Leather Bound (2010th Edition). Barnes & Noble.
- Morris, M. J. (2021, May 3). Asthma: Practice Essentials, Background, Anatomy. Medscape. https://emedicine.medscape.com/article/296301-overview