- Anatomical terminology
- Skeletal system
- Joints
- Muscles
- Heart
- Blood vessels
- Lymphatic system
- Nervous system
- Respiratory system
- Digestive system
- Urinary system
- Female reproductive system
- Male reproductive system
- Endocrine glands
- Eye
- Ear
Testicles
The testicle (Latin: testis), also called testis, is a paired ovoid-shaped internal genital organ of the male reproductive system. The testicle of an adult male is located in the scrotum. It provides spermatogenesis and produces spermatozoa. Also, it synthesizes various sex hormones, including testosterone and a minimal amount of estrogen. Therefore, the testicle, at the same time, also functions as an endocrine gland.
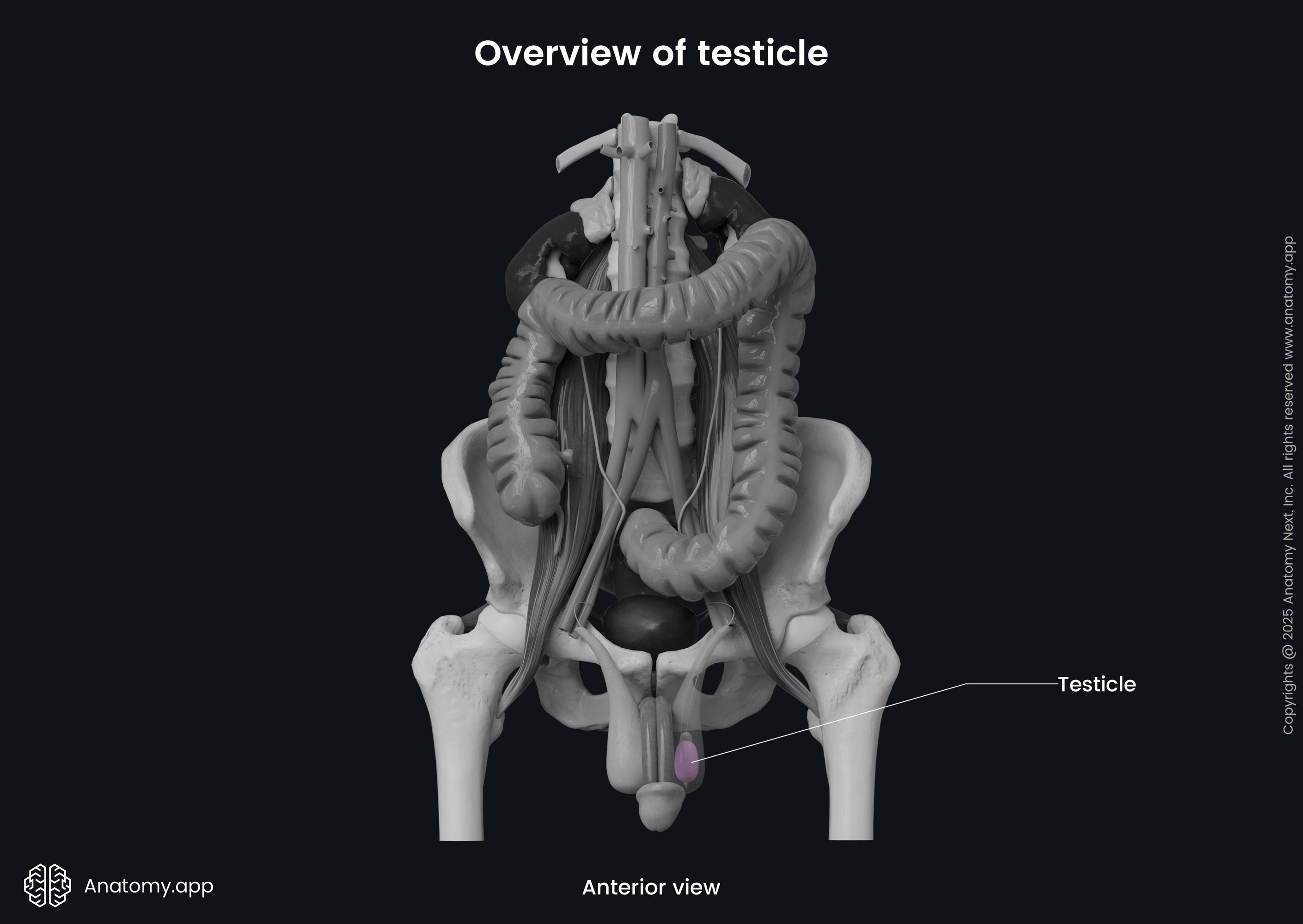
Anatomy of testicles
The testicle is analogous to the ovary of the female reproductive system, and it resembles a small egg in shape and size. Usually, the testicle is 1.58 - 1.97 inches (4 - 5 centimeters) in length, and its thickness varies from 0.79 - 1.18 inches (2 to 3 centimeters). A testicle of an adult male weighs between 0.71 and 1.06 ounces (20 - 30 grams).
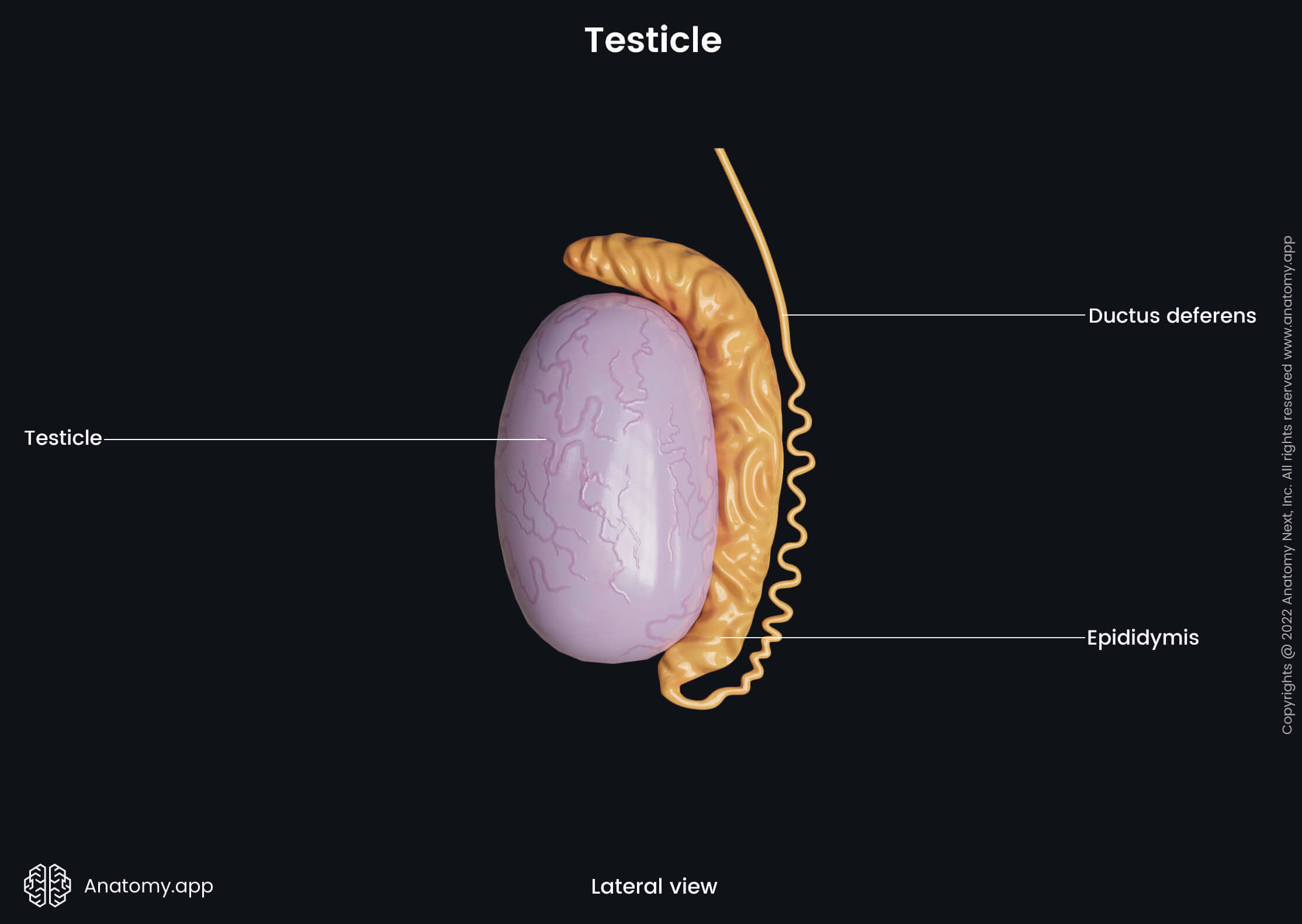
Both testicles are located in the scrotum, which is a saccular extension of the anterior abdominal wall made of skin and smooth muscle cells. The scrotum is subdivided into two compartments by a scrotal septum - a thin, vertically positioned midline fibrous tissue layer. Each compartment contains one testicle. Usually, the left testicle is positioned slightly lower than the right one.
Both testicles are located within the scrotum together with the epididymides and spermatic cords that contain the initial parts of the vasa deferentia (ductus deferentes), blood vessels, lymphatic vessels and nerves. The epididymis is a long paired coiled tube that overlies the top and posterior aspects of the testicle. Overall, it is attached to the posterior margin of the testicle. The epididymis is a site where spermatozoa mature and are stored.
During embryological development, the testicles are retroperitoneally located organs, and they are found on the posterior wall of the abdomen. They descend to the scrotum via the inguinal canal before birth, and the whole descending process usually ends by the seventh month of gestation. However, the testicles remain connected to the abdominal cavity by spermatic cords.
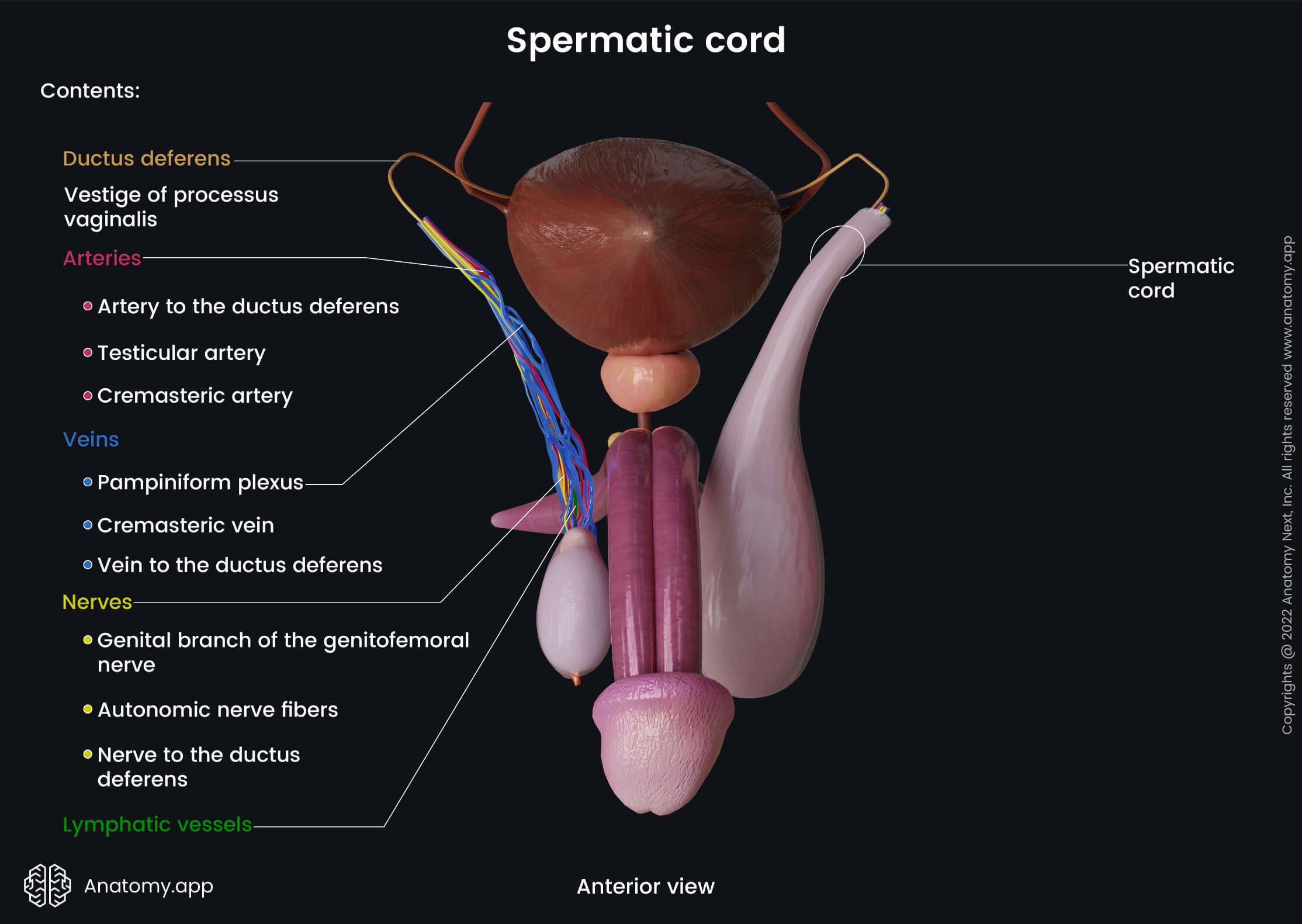
The descent of the testicles is necessary for spermatogenesis. The scrotum helps to regulate the temperature of the testicles, which is an important physical factor that can affect sperm production. Effective spermatogenesis requires a temperature that is a few degrees lower than the actual body temperature. The ideal temperature is believed to be 93.2 degrees Fahrenheit (34 degrees Celsius). If testicles do not descend, spermatozoa can not be produced.
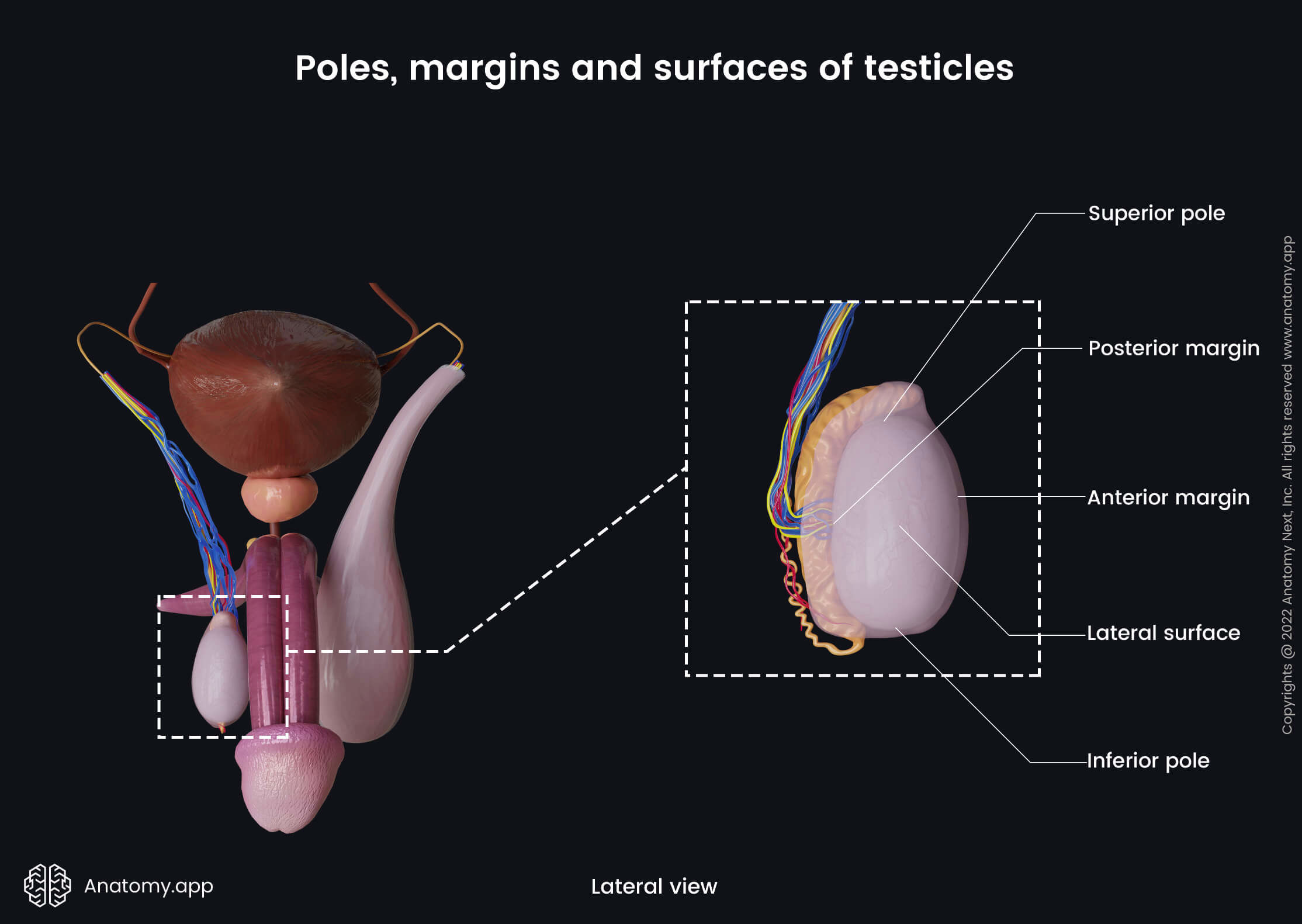
Poles, margins and surfaces of testicles
As mentioned, each testicle appears ovoid-shaped. Therefore, it has two poles - superior and inferior. The superior pole is covered by the epididymis, while the inferior pole is connected to the inferior aspect of the scrotum by the scrotal ligament.
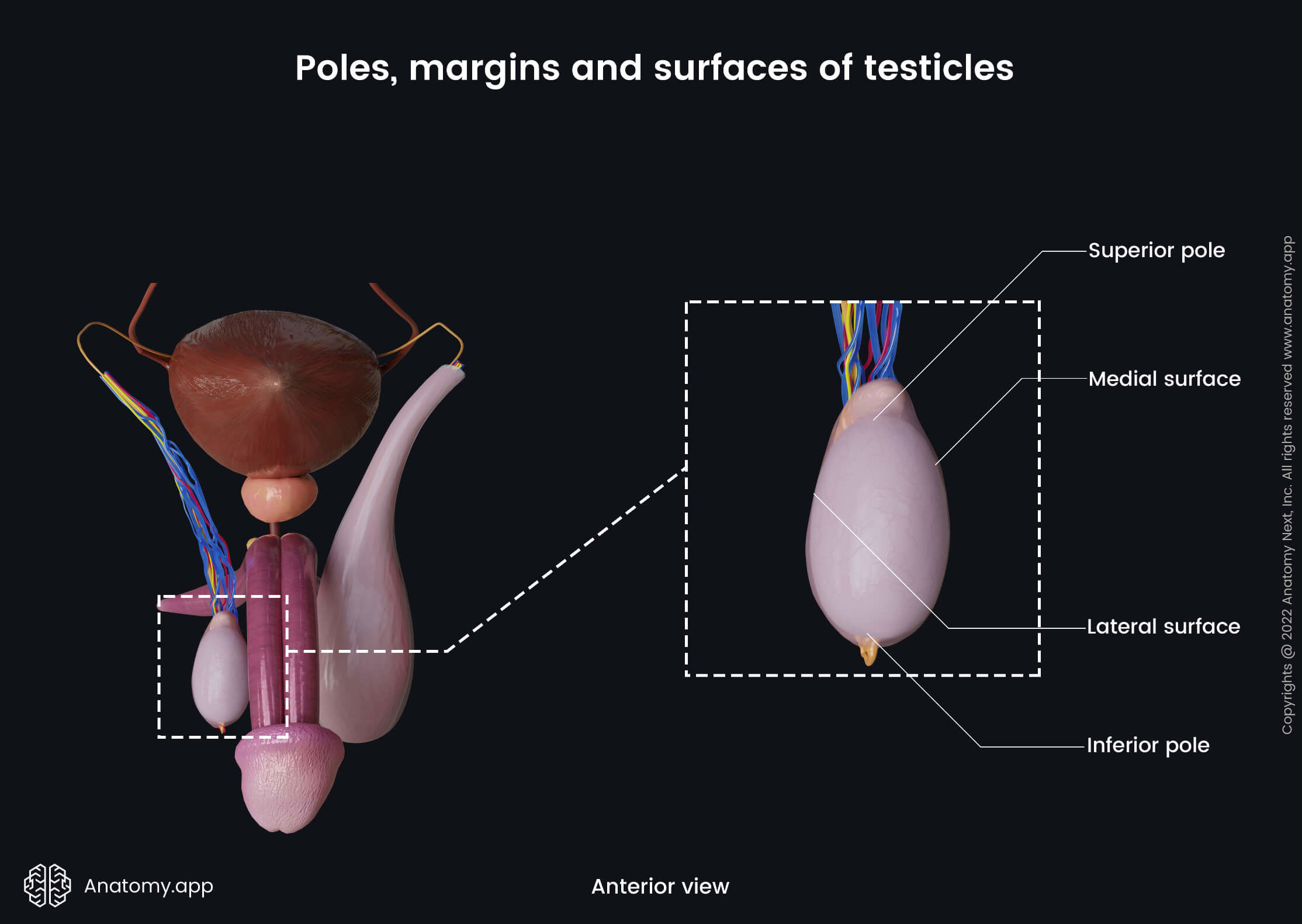
The scrotal ligament is a remnant of the gubernaculum testis, which is an important structure during the descent of the testicle. Besides the poles, each testicle also has two margins and two surfaces.
- Anterior margin - facing forward; it is not connected to other structures;
- Posterior margin - facing backward; epididymis attaches to this border;
- Medial surface - flat;
- Lateral surface - more curved and appears a bit convex.
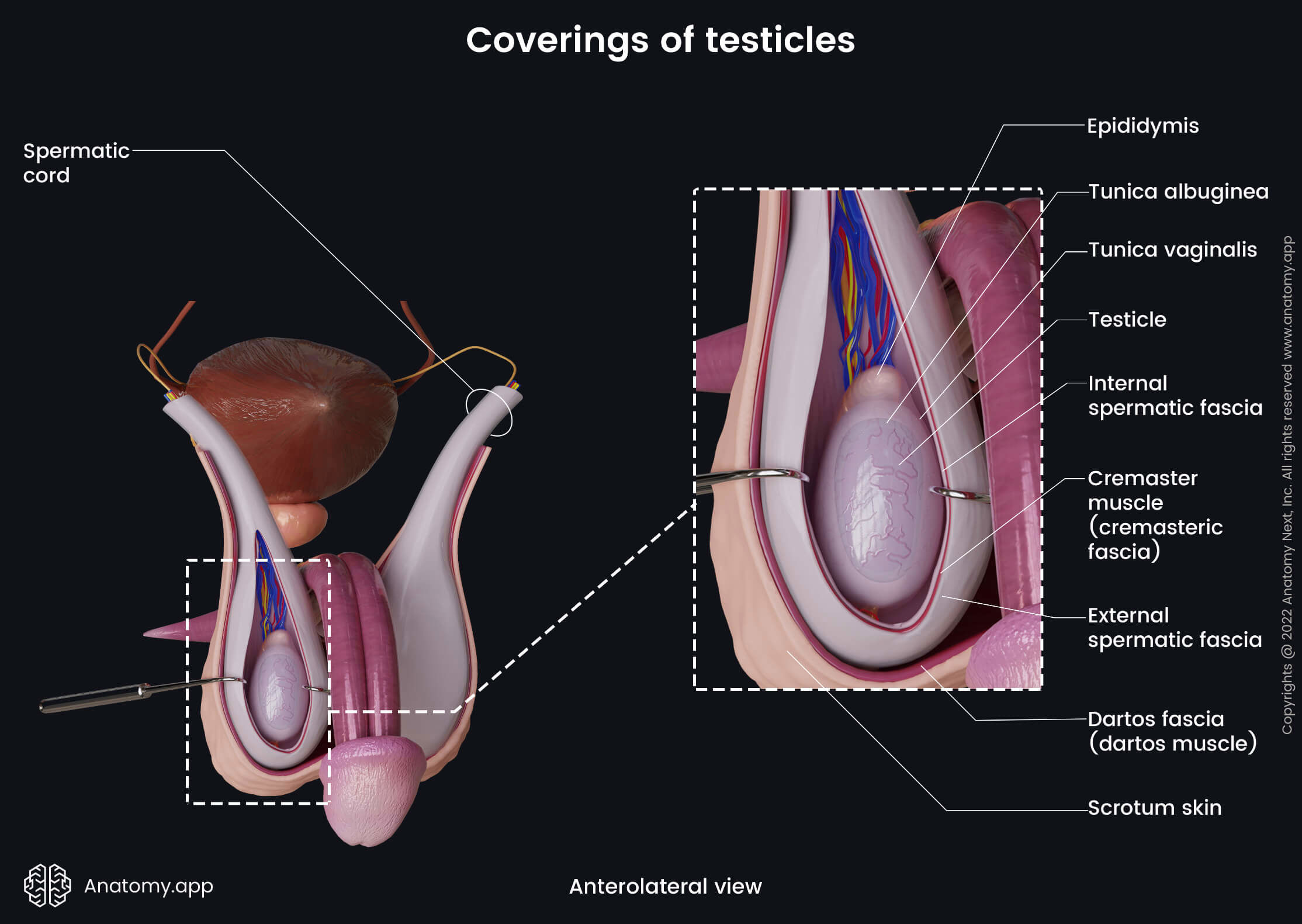
Coverings of testicles
The outer aspects of the testicle and epididymis are covered by a dense fibrous connective tissue capsule known as the tunica albuginea. Above the tunica albuginea, both male internal genital organs are covered by several more layers formed during the descent of the testicles by the exaggeration of the peritoneum and the elements of the abdominal wall. The most external layer is the skin. From deep to superficial, each testicle is covered by the following layers:
- Tunica albuginea
- Tunica vaginalis
- Internal spermatic fascia
- Cremaster muscle (cremasteric fascia)
- External spermatic fascia
- Dartos fascia (dartos muscle)
- Skin
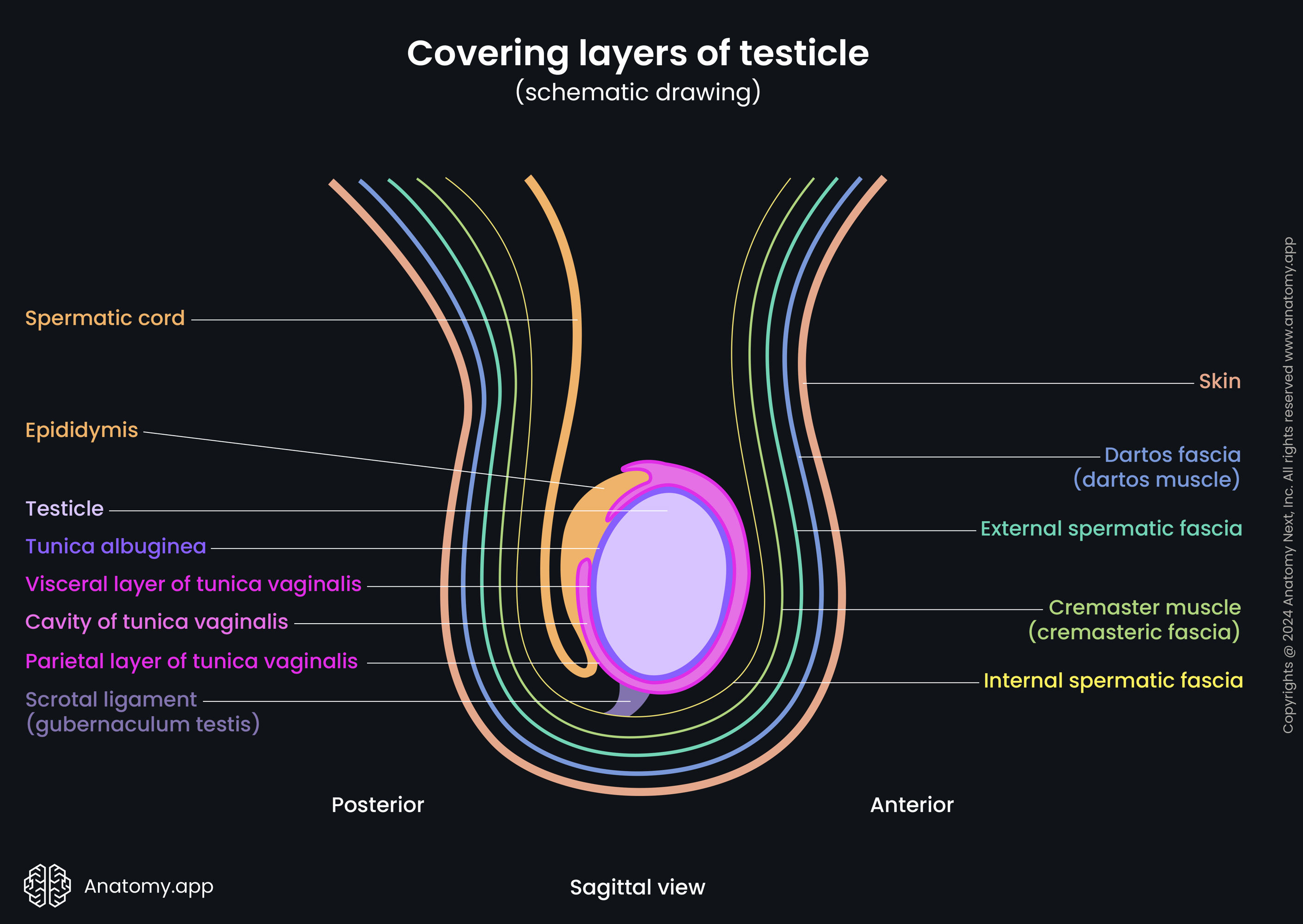
The tunica vaginalis is the next layer found above the tunica albuginea. It partially encloses the testicle. The tunica vaginalis forms during the descent of the testicle, and it is derived from the peritoneum and embryonic vaginal process. It has two layers - visceral and parietal. The visceral layer is the internal layer, and it covers the testicle, the head of the epididymis, and the inferior portion of the ductus deferens.
The visceral layer changes into the external or parietal layer at the posterior margin of the epididymis. It is larger, and at first, it covers the distal portion of the spermatic cord, then it continues over the visceral layer and covers the duct of the epididymis. Finally, it blends with the visceral layer. The tunica vaginalis produces a small amount of serous fluid. It is found between both layers and acts as a lubricant, preventing friction and allowing the testicle to move freely within the scrotum.
The internal spermatic fascia merges with the parietal layer of the tunica vaginalis. It is a thin fascial layer formed by the transversalis fascia.
The cremaster muscle covers the testicle and spermatic cord. When it contracts, the muscle pulls the testicle superiorly towards the inguinal canal, protecting the testicle from various harmful environmental factors such as temperature changes.
The cremaster muscle is composed of striated and smooth muscle cells and is derived from the internal abdominal oblique muscle, its aponeurosis and fibers of the inguinal ligament. Some authors state that it is also derived from the transversus abdominis muscle. Sometimes this layer is simply called a cremasteric fascia, as the muscle fibers of the cremaster unite with the surrounding loose connective tissue.
The external spermatic fascia is a thin membrane covering the previous layer. It originates from the external abdominal oblique muscle and its aponeurosis.
The final two layers - the dartos fascia (dartos muscle) and the skin - are layers of the scrotum. The dartos fascia contains smooth muscle fibers, which is why it is also called the dartos muscle or simply dartos. These muscle fibers participate in the thermoregulation of the testicles, and they contract when it gets cold, resulting in wrinkling of the skin covering the scrotum. This action brings both testicles closer to the warmer body temperature and reduces heat loss.
Histology of testicles
As mentioned, the testicle is enclosed by a dense connective tissue capsule called the tunica albuginea. The connective tissue from the capsule extends into the parenchyma of a testicle, forming numerous septae and subdividing it into smaller compartments known as lobules. These septae extend tol the mediastinum, which is a connective tissue network found at the posterior aspect of the testicle.
The majority of the lobules are formed by small coiled ducts called the seminiferous tubules, which are the sites of origin of sperm cells. The epithelium of these tubules is composed of various cells, such as germ cells and Sertoli cells.
Between seminiferous tubules are relatively sparse connective tissue stroma known as interstitial connective tissue. The interstitial tissue contains Leydig (interstitial) cells responsible for the endocrine function. They secrete testosterone. Tubules are also surrounded by contractile myoid cells.
Besides the seminiferous tubules, the testicles have a few more tubules. The spermatozoa mature in the seminiferous tubules, and further, they reach the epididymis via the straight tubules, rete testis and efferent ductules.
Duct system
At the posterior aspect of each testicle, the connective tissue forms the mediastinum testis. It is a connective tissue network found more or less centrally at the mentioned aspect of the testicle. It is connected to the septae that divide the parenchyma of a testicle into lobules.
Each testicle has 200 - 300 lobules. Each lobule usually contains 2 - 4 convoluted seminiferous tubules, which are sites of spermatogenesis. Towards the mediastinum, these convoluted seminiferous tubules of each lobule merge, straighten and become straight tubules.
After entering the mediastinum testis, the straight seminiferous tubules form an extensive anastomosing network of tubules called rete testis. And finally, 10 - 15 efferent ductules usually leave the rete testis and enter the head of the epididymis.
Sertoli cells
Sertoli cells are long pyramidal-shaped support cells forming the simple columnar epithelium of the seminiferous tubules. These cells are closely attached to each other. Moreover, they are firmly connected to the basement membrane. From the basement membrane, Sertoli cells extend into the lumen of the seminiferous tubules.
Sertoli cells can be described as the sites where sperm cells develop, as germ cells are closely related to them. In fact, germ cells are found within the invaginations and crypts of Sertoli cells. Overall, Sertoli cells provide physical, regulatory and nutritional functions.
Sertoli cells provide structural support for germ cells and control their differentiation. Also, they secrete fluid rich in proteins and ions that nourishes developing germ cells. Moreover, these cells form the blood-testis barrier. And finally, they are also responsible for spermiation and provide phagocytosis of cellular remnants and residual bodies, as they contain relatively large amounts of lysosomes.
Blood-testis barrier
The blood-testis barrier is one of the tightest barriers in the human body. It is an essential formation for germ cell development. Overall, it can be described as a structural and physiological barrier formed by tight junctions between adjacent Sertoli cells. It is found on the luminal side of the basally located spermatogonia. This barrier prevents arterial blood and cells within the blood vessels from reaching more mature and differentiated cells.
The barrier subdivides the epithelium of the seminiferous tubule into basal and adluminal compartments. Each compartment provides an environment for particular cells. The basal compartment includes young germ cells (spermatogonia), while the adluminal compartment has an environment that protects and nourishes more mature and developing cells. One of the main functions of this barrier is to separate immune cells from the more mature cells. Immune cells can not yet recognize developing cells and, therefore, can potentially harm them.
Myoid cells
The myoid cells are smooth muscle cells found within the interstitial tissue. They surround the seminiferous tubules. These cells provide contraction waves that move immature spermatozoa out of the seminiferous tubules. This contractile function allows moving the spermatozoa to the straight tubules from where they reach the rete testes and further enter the epididymis via efferent ductules.
Leydig cells
Leydig cells are also known as interstitial cells, as they form cell clusters within the interstitial tissue found between the seminiferous tubules. They are endocrine cells, and they synthesize testosterone under the influence of the luteinizing hormone.
The luteinizing hormone is secreted by pituitary glands, and by acting on Leydig cells, it stimulates the production of testosterone, which in turn initiates spermatogenesis. Leydig cells also synthesize small amounts of estrogen.
Leydig cells can easily be recognized not only by their location but also by their round nuclei and extensive acidophilic cytoplasm. These cells may contain small eosinophilic cytoplasmic inclusions known as Reinke crystals. Besides that, Leydig cells may also have lipofuscin vesicles.
Functions of testicles
The testicles are analogous to the ovaries of the female reproductive system. Like ovaries, the testicles have several main functions - they produce sperm and are responsible for the androgen and principal male sex hormone - testosterone - synthesis. Besides the androgens, the testicles also produce small amounts of estrogens.
Spermatogenesis
The testicles produce sperm in a process called spermatogenesis. During spermatogenesis, the primordial germ cells develop and differentiate into mature spermatozoa.
On average, the duration of spermatogenesis in humans is from 64 to 75 days. A healthy adult man produces approximately 200 - 300 million sperm cells daily. Each primary spermatogonium gives rise to 64 spermatozoa.
The whole process happens within the seminiferous tubules and can be subdivided into three stages:
- Spermatocytogenesis
- Spermatidogenesis
- Spermiogenesis
The initial stage of spermatogenesis is called spermatocytogenesis. During this stage, the primordial and most undifferentiated germ cells called spermatogonia repeatedly divide by mitosis to renew themselves and provide more spermatogonia so that later these identical cells can differentiate into primary spermatocytes.
There are two types of spermatogonia - A and B. Only B spermatogonia can further differentiate into primary spermatocytes. This stage is the proliferation phase of spermatocytogenesis.
Spermatidogenesis is the next stage. During this stage, two meiotic divisions happen. Each primary spermatocyte undergoes meiosis I, generating two secondary spermatocytes that further enter meiosis II. As a result of the second meiotic division, four round spermatids are produced from each primary spermatocyte.
Further, during spermiogenesis, round spermatids differentiate into elongated and sperm-like spermatids. And finally, the elongated spermatids differentiate into sperm cells. These cells are then released from the supporting Sertoli cells into the seminiferous tubule during a process known as spermiation.
Testosterone production
The testicles are responsible for the production of androgens, including the synthesis of the primary male sex hormone - testosterone. Testosterone is responsible for regulating sex differentiation, initiation of spermatogenesis, development of sexual characteristics in males and fertility.
During the intrauterine period, fetal testosterone is responsible for primary sexual development and the development of the male phenotype, including the development of male reproductive organs. Also, it affects the descent of the testicles. Besides the reproductive organs, testosterone influences the brain and is involved in its development.
During puberty, testosterone is responsible for developing male secondary sex characteristics. These include the hypertrophy of the larynx that causes vocal changes and deepening of the voice, increase in muscle mass as testosterone stimulates protein synthesis, broadening of the shoulders, further development of the testes, penis and other male reproductive tract organs, initiation of spermatogenesis, male hair patterns and increased body hair growth, including the growth of pubic, axillary and facial hair. Also, testosterone causes behavior changes that are associated with sex drive (libido).
During adulthood, testosterone has metabolic and reproductive effects. It regulates sex drive, bone density and mass, muscle mass and strength, and fat distribution. Besides the production of sperm, it also stimulates erythropoiesis and regulates the production of red blood cells. Testosterone levels tend to drop as men get older. It leads to opposite effects - decreased testicular size, a drop in sex drive, decreased bone density, a decline in muscle mass, and increased fat production.
Estrogen production
In the male reproductive tract, estrogen is synthesized by Leydig cells and germ cells found in the testicles. Most estrogen receptors are located in the testis (efferent ductules), epididymis and prostate.
Estrogen influences male behavior, as well as it is essential for male fertility and the development and function of efferent ductules and the prostate. Also, in adult males, estrogen regulates the flow of sperm cells from the testicles to the epididymis.
Neurovascular supply of testicles
Arterial blood supply
The arterial blood supply of the testicles is provided by paired arteries called testicular arteries. They are visceral branches of the abdominal aorta, arising from each its side below the origin sites of the renal arteries. It usually happens at the level of the second or third lumbar vertebrae (L2 or L3). The testicular arteries are included in the contents of the spermatic cords, and they reach the testicles through the inguinal canals.
Additionally, the testicles can have a collateral blood supply that is essential if the testicular arteries, for some reason, get obstructed. In that case, these arteries will keep the testes functioning and allow their survival. The collateral blood supply comes from the cremasteric artery and the artery of ductus deferens. The first is a branch of the inferior epigastric artery, while the second usually arises from the umbilical artery.
Venous drainage
The venous drainage of the testicle starts from small veins that emerge from its posterior aspect and form a vascular network called the pampiniform plexus. At the same time, these veins surround the branches of the testicular artery and are involved in temperature regulation - they cool the warm blood that flows within the testicular artery. Thus, the testicle receives colder arterial blood, which is an important physical factor for spermatogenesis.
Each pampiniform plexus is included in the spermatic cord. It ascends towards the abdomen anterior to the ductus deferens. At the level of the superficial (external) inguinal ring, the veins of the plexus merge and form three to four larger veins that travel through the inguinal canal. At the level of the deep (internal) inguinal ring, these veins unite and form a single testicular vein that enters the abdominal cavity and further goes on the anterior surface of the psoas major muscle together with the testicular artery.
Both testicular veins drain into different blood vessels. The right testicular vein enters the inferior vena cava on its right anterolateral aspect at an acute angle. Sometimes, it may alternatively drain into the right renal vein instead of the inferior vena cava. In contrast, the left testicular vein drains into the left renal vein at a right angle.
Lymphatic drainage
The lymphatic drainage of the testicle is provided by the lymphatic vessels that are included in the content of the spermatic cord. These vessels usually do not drain in the nearby inguinal lymph nodes. The testicle is an organ with a retroperitoneal origin, and that is why the lymph from the testicles is carried to the para-aortic and pre-aortic lymph nodes located along the abdominal aorta.
Innervation
The innervation of the testicle is provided by the sensory, parasympathetic and sympathetic nerve fibers. Like the blood and lymphatic vessels described above, the nerve fibers reach the testicle via the spermatic cord.
The sensory innervation is usually reviewed together with the scrotum, as both structures are related and have common sensory innervation sources. The sensory innervation originates from the T12 - L2 and S2 - S4 spinal nerves via the ilioinguinal, genitofemoral and pudendal nerves:
- The ilioinguinal nerve supplies the skin over the base of the penis, the inner aspect of the thigh and the upper aspect of the scrotum.
- The genitofemoral nerve has two terminal branches - genital and femoral branches. The genital branch enters the spermatic cord and innervates the cremaster muscle and tunica vaginalis.
- The pudendal nerve gives off the perineal nerve that is responsible for the sensory innervation of the posterior aspect of the scrotum.
The sympathetic innervation comes from the T10 - L2 segments of the spinal cord. The sympathetic nerve fibers reach the testicles via the lesser thoracic and lumbar splanchnic nerves.
In contrast, parasympathetic innervation mostly comes from the S2 - S4 segments of the spinal cord via the lesser pelvic splanchnic nerves. Overall, three nerves containing autonomic fibers supply the testicles - superior, middle and inferior spermatic nerves.
- The superior spermatic nerves contain fibers from the intermesenteric and renal plexuses, and they travel together with the testicular artery to reach the testicle.
- The fibers of the middle spermatic nerves come from the superior hypogastric plexus. These fibers go together with the ductus deferens until they reach the deep ring of the inguinal canal, where they join the spermatic cord.
- The inferior spermatic nerves arise from the inferior hypogastric (pelvic) plexus. These nerves join the middle spermatic nerves at the level where the prostate is related to the urinary bladder.