- Anatomical terminology
- Skeletal system
- Joints
- Muscles
- Heart
- Blood vessels
- Lymphatic system
- Nervous system
- Respiratory system
- Digestive system
- Urinary system
- Female reproductive system
- Male reproductive system
- Endocrine glands
- Eye
- Ear
Spinal cord
The spinal cord is a part of the central nervous system (CNS) along with the brain. It is located within the vertebral canal of the spine. In the cranial direction, the spinal cord is continuous with the medulla oblongata of the brainstem. In the caudal direction, it terminates as the medullary cone (conus medullaris). Overall, the spinal cord extends between the foramen magnum - a large opening in the external cranial base of the skull - and the first or second lumbar vertebrae (L1/L2) in adults.
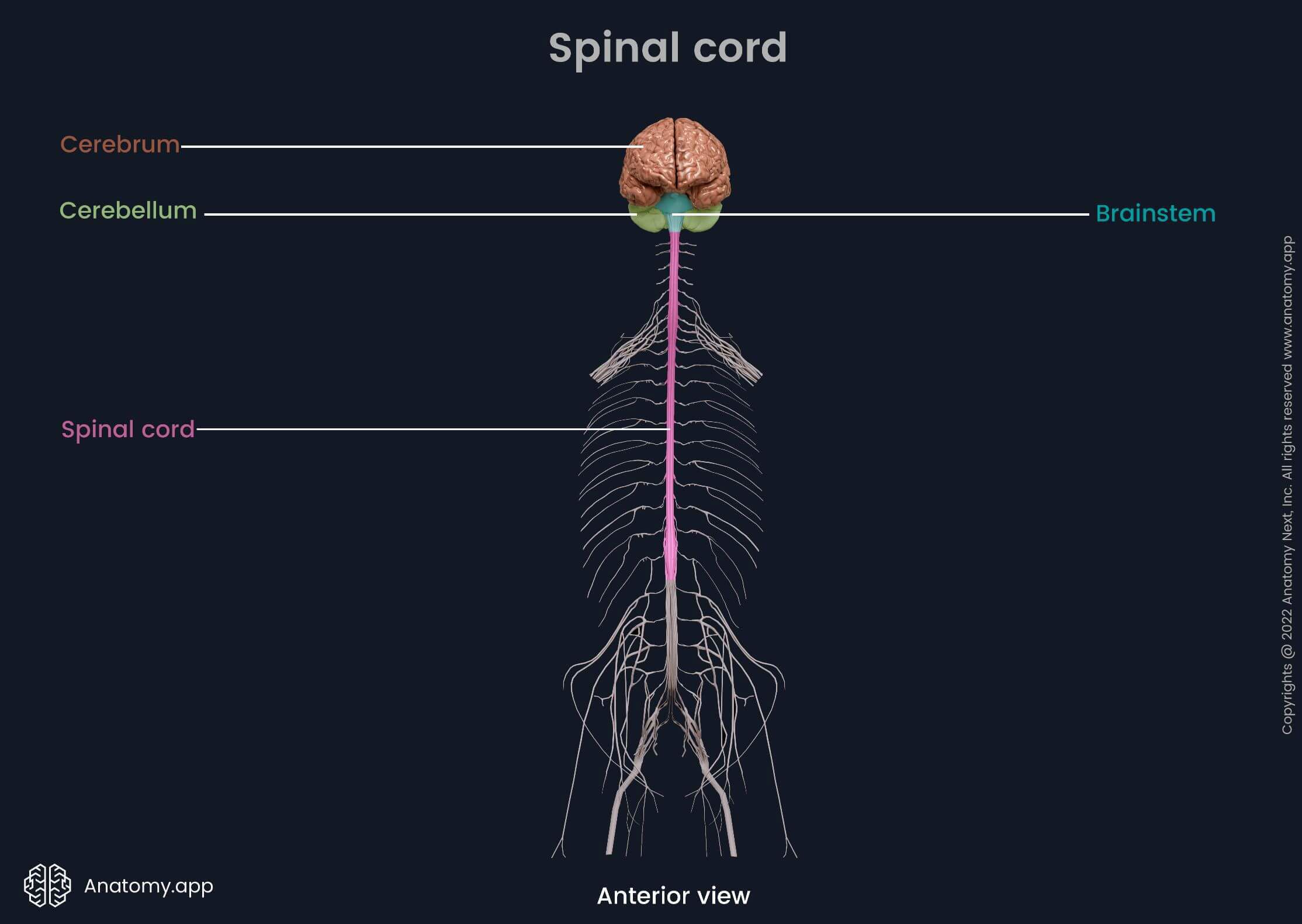
The spinal cord is cylindrical in shape and resembles a long thread of nervous tissue. It connects the brain with the rest of the body through the peripheral nervous system (PNS). The spinal cord receives impulses from the brain and provides innervation of the trunk and upper and lower limbs. It connects the brain with the body via 31 pairs of spinal nerves. The spinal cord sends and receives signals to and from different brain regions through nerve tracts.
Spinal cord external anatomy
Spinal cord segments and enlargements
Like the vertebral column, the spinal cord anatomically can be divided into five parts: cervical, thoracic, lumbar, sacral and coccygeal. All parts correspond to the respective vertebral regions. The spinal cord is also arranged into segments. One segment corresponds to one pair of spinal nerves. There are 31 spinal segments and 31 pairs of spinal nerves that exit the spinal cord. In total, the spinal cord has 8 cervical, 12 thoracic, 5 lumbar, 5 sacral and 1 coccygeal pair of spinal nerves.
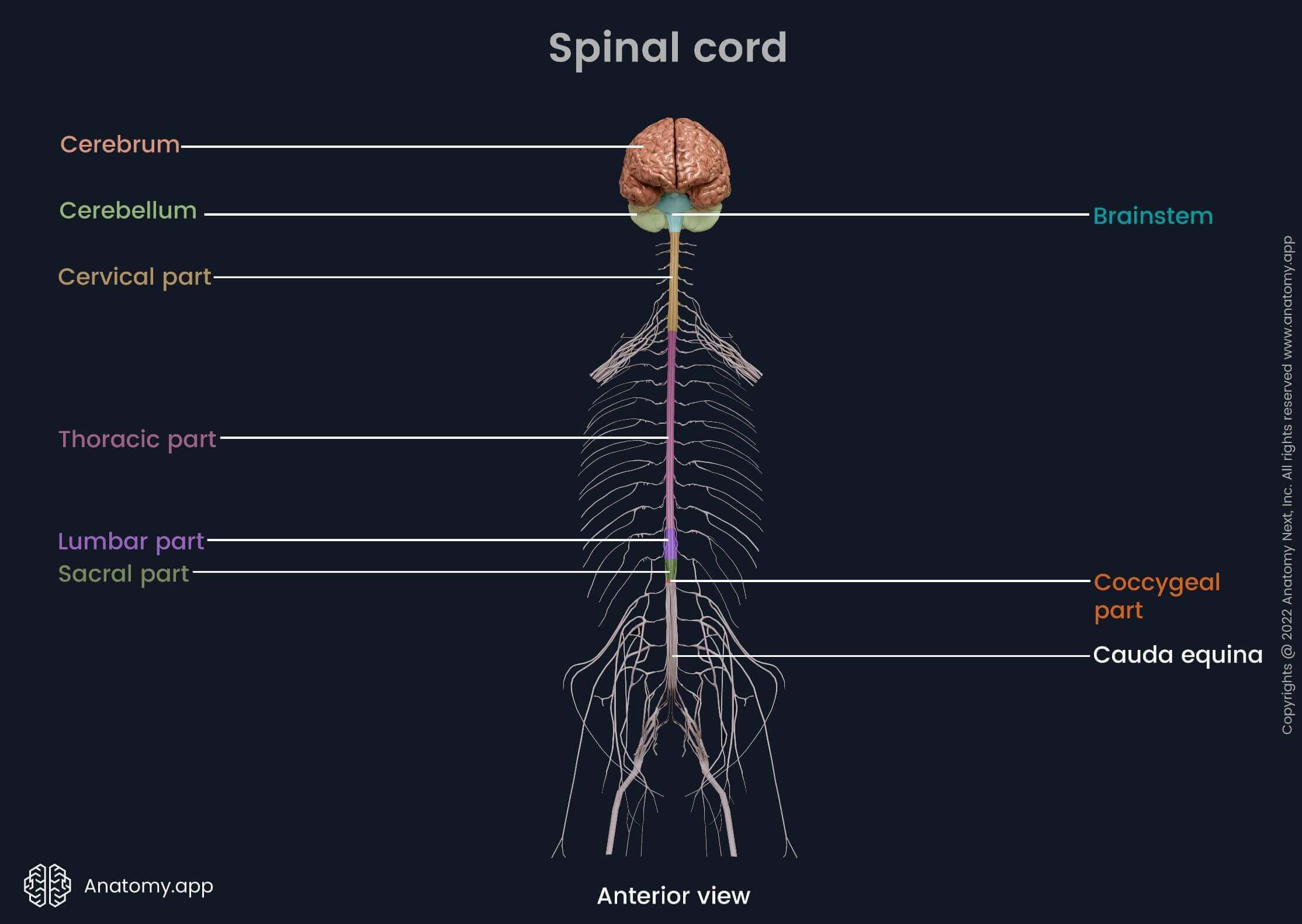
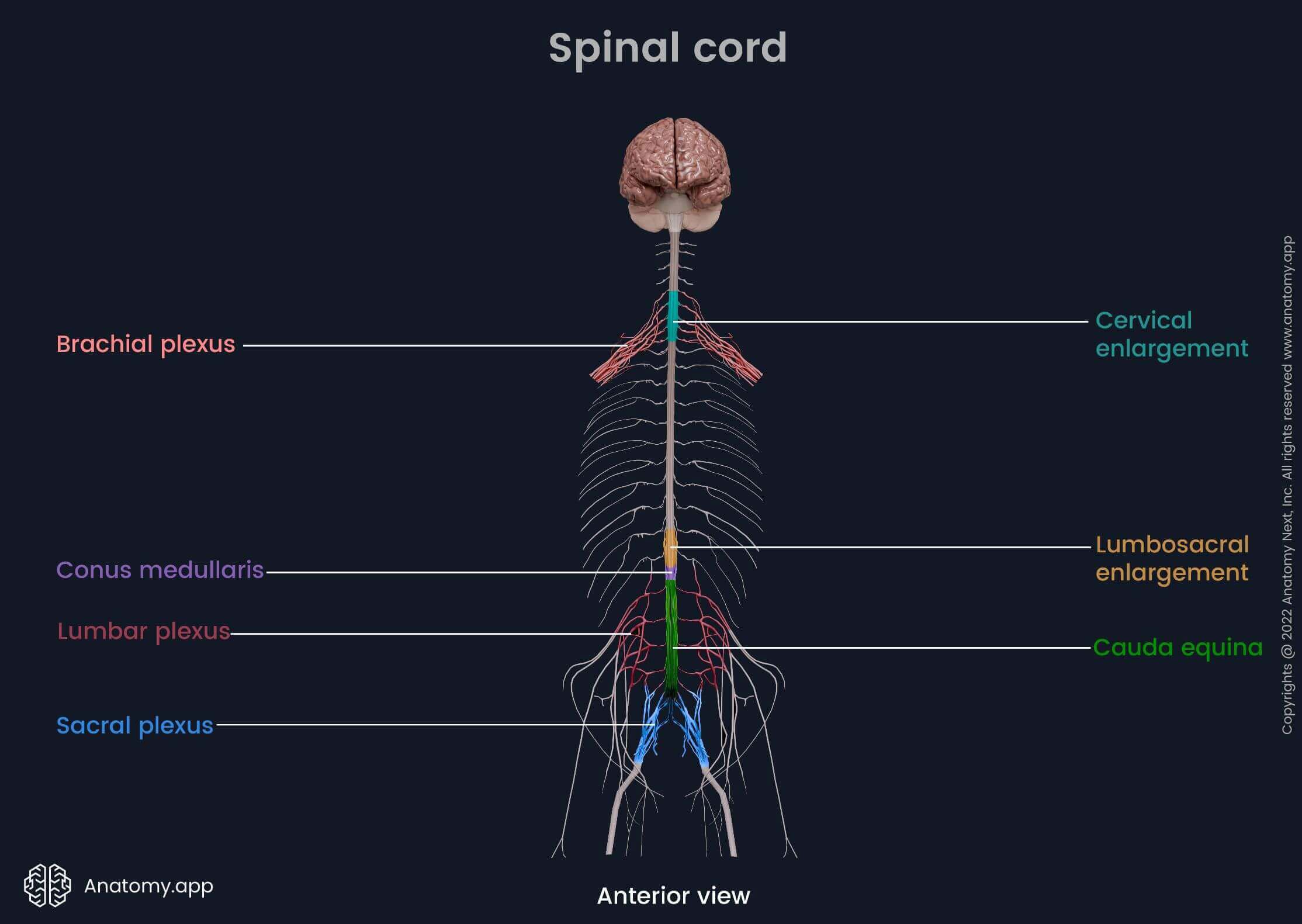
The spinal cord is not the same diameter throughout its length. It has two thicker regions called cervical and lumbosacral enlargements. Both correlate with the nerves that innervate the upper and lower extremities. The cervical enlargement corresponds to the brachial plexus - a group of spinal nerves (C5 to T1 segmental levels) that innervate the upper limbs. The lumbosacral enlargement is associated with the lumbar plexus and sacral plexus. It includes the spinal nerves of the T11 to L1 segmental levels. They provide innervation of the lower limbs.
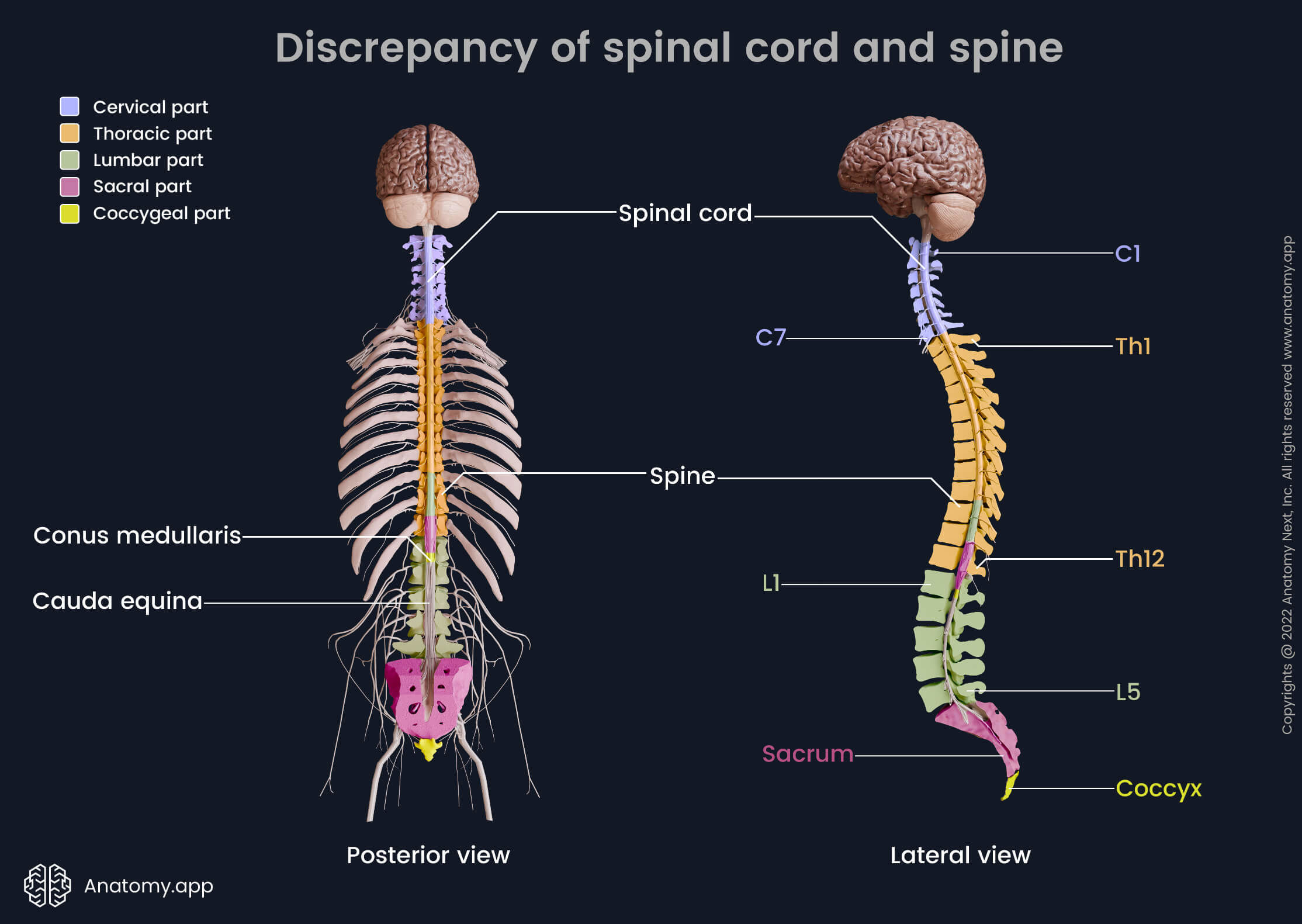
Discrepancy of spinal cord and spine
The spinal cord is shorter than the spine, and its segments are not always situated at the level of their corresponding vertebrae. This difference between the spinal cord and spine is called the discrepancy of the spinal cord and spine or the vertebral-spinal discrepancy. As previously mentioned, the spinal cord segment corresponds to one spinal nerve pair. Note that the spinal cord contains 8 cervical spinal nerve pairs and, therefore, has 8 cervical segments, but the cervical spine is composed of only 7 cervical vertebrae. The spinal cord usually ends at the first or second lumbar vertebrae (L1 / L2) as the conus medullaris. Below the L2 level are bundles of the lower spinal nerves called cauda equina.
- Cervical segments correspond to the cervical part of the spine. C1 and C2 spinal cord segments match the first two cervical vertebrae (C1, C2), while C3 to C8 spinal cord segments are situated between the third through seven cervical vertebrae (C3 - C7).
- Thoracic segments are positioned between the first to eight or ninth thoracic vertebrae (T1 - T8 / T9). T1 and T2 spinal cord segments correspond to the same vertebral levels (T1 and T2 vertebrae). T3 to T12 spinal cord segments are located between T3 through T8 / T9 vertebral levels.
- Lumbar segments are located between vertebrae T8 / T9 through T10 / T11.
- Five sacral segments correspond to the T10 / T11 through L1 / L2 vertebral levels.
- And finally, the coccygeal segment is situated at the first or second lumbar vertebral (L1 / L2) level.
Surfaces and grooves of spinal cord
The spinal cord has four surfaces - anterior, posterior and two lateral on either side of the cord. These surfaces are separated by various sulci and fissures:
- Anterior median fissure - the most prominent groove in the middle of the anterior surface;
- Posterior median fissure (or posterior median sulcus) - extends along the midline of the posterior surface;
- Right and left anterolateral sulci - located between the anterior and lateral surfaces at the sites where ventral (anterior) roots exit the spinal cord;
- Right and left posterolateral sulci - found between the posterior and lateral surfaces at the sites where dorsal (posterior) roots enter the spinal cord.
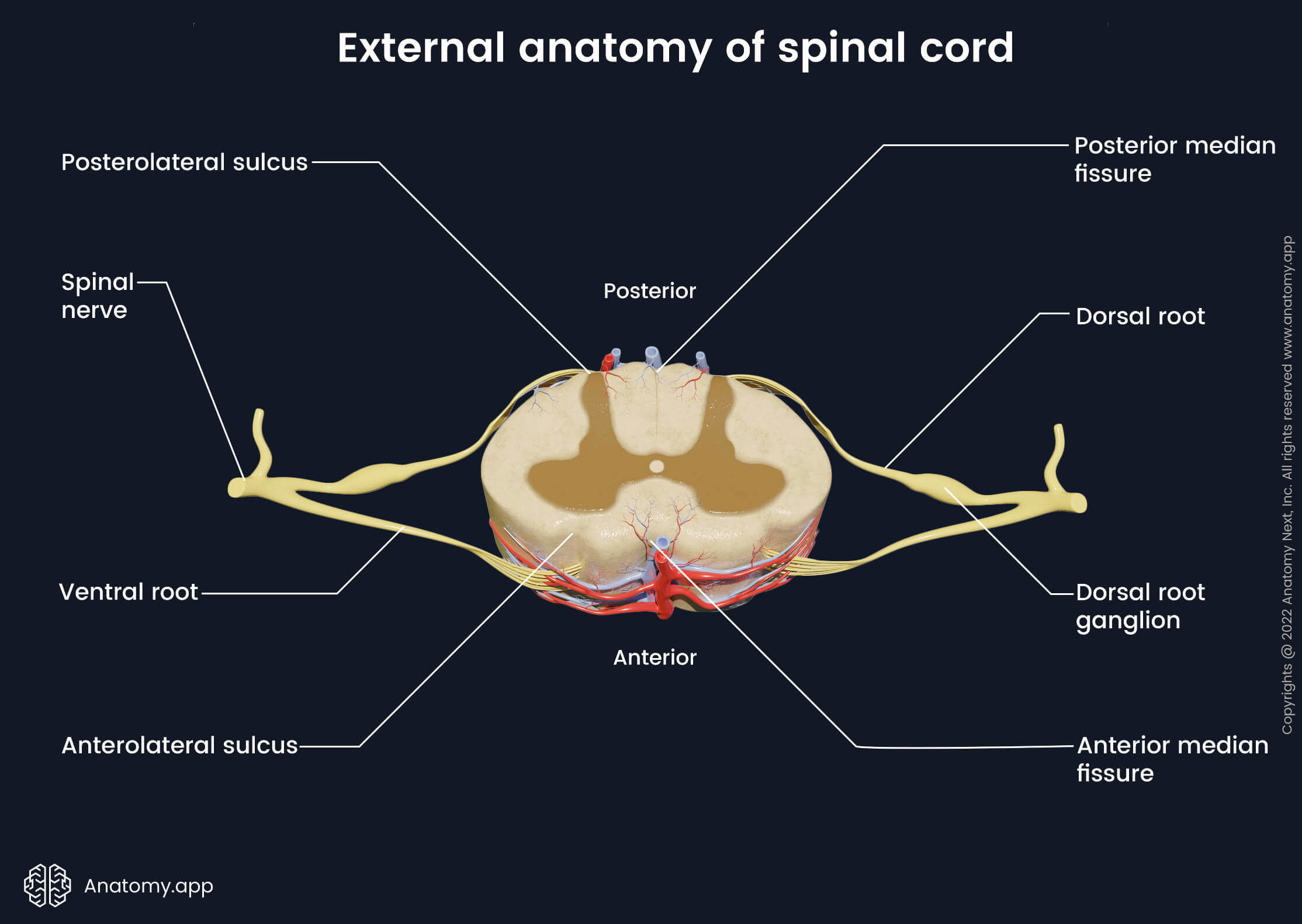
Spinal nerves and roots
As previously mentioned, the spinal cord contains 31 pairs of segmentally organized spinal nerves. Each spinal nerve is attached to the spinal cord with two roots - ventral (anterior) and dorsal (posterior). Both roots enter and exit the vertebral canal through the intervertebral foramina. Each root contains different fibers. The dorsal root is composed of afferent (sensory), while the ventral root contains efferent (motor) fibers.
The dorsal roots consist of afferent fibers coming from nerve cell bodies. Near the spinal cord, the dorsal root has a bulge called the dorsal root ganglion that contains cell bodies of sensory neurons. The ventral roots contain efferent fibers coming from the motor neurons found within the gray matter of the spinal cord. Laterally from the dorsal root ganglion, both roots merge together and form the spinal nerve.
Note: Afferent means that the nerve impulse is headed towards the central nervous system. In other words, the afferent fibers send impulses in the direction of the spinal cord. In contrast, efferent means that the impulse is directed away from the central nervous system to the periphery of the body.
Conus medullaris, cauda equina and filum terminale
The spinal cord is shorter than the vertebral column and it ends at the first or second lumbar vertebrae (L1/L2) level as conus medullaris (medullary cone). The conus medullaris is a cone-shaped termination of the spinal cord that is connected to the coccyx by a fibrous connective tissue strand called filum terminale. It stabilizes the distal aspect of the spinal cord.
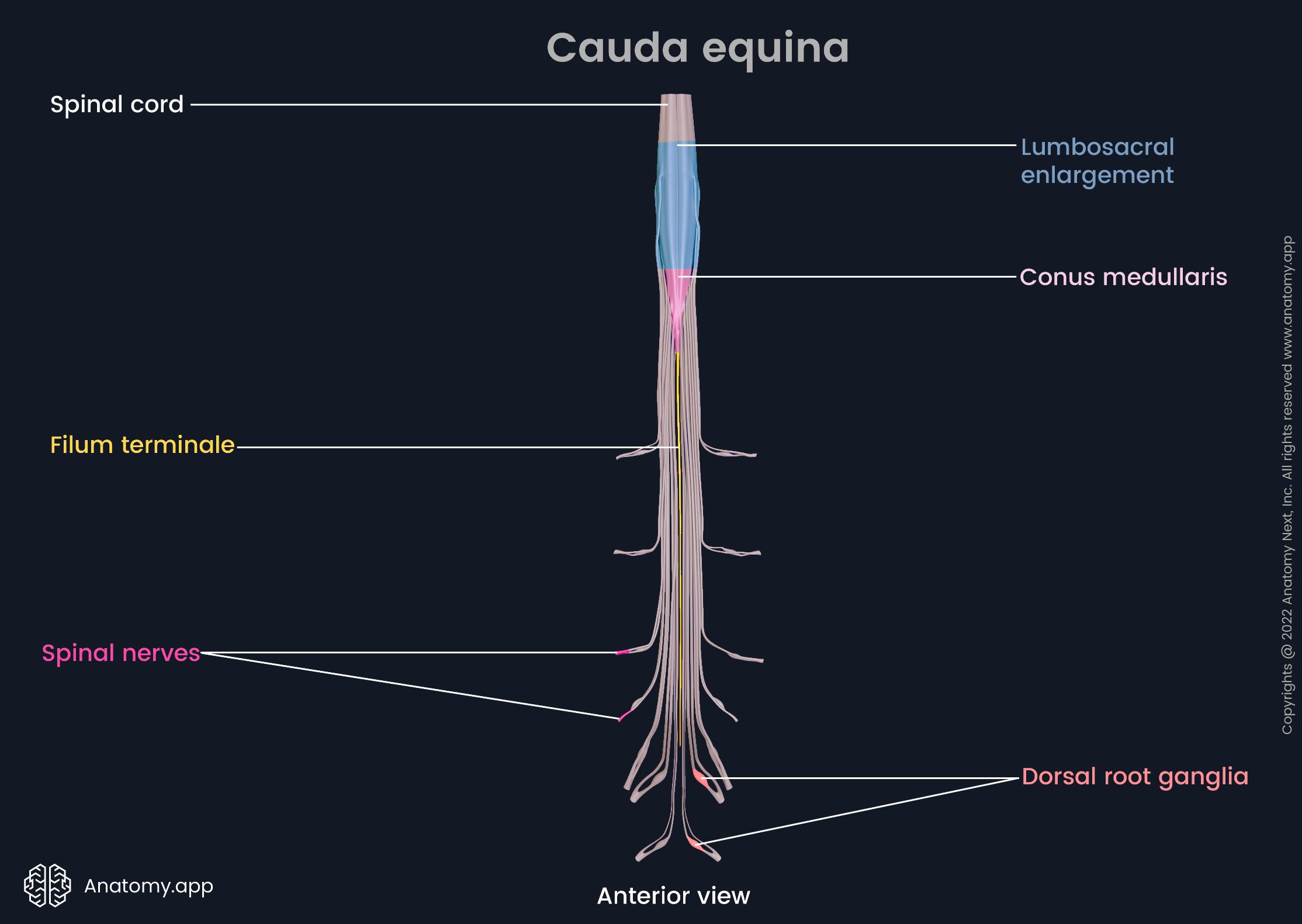
The filum terminale descends together with the cauda equina - a bundle of the lower spinal nerve roots. Its name derives from Latin, meaning “horse's tail” due to its resemblance to a horse tail. The cauda equina is composed of the L2 - L5 lumbar, all the sacral and coccygeal nerve roots. The filum terminale, together with the cauda equina, occupies the lower third of the vertebral canal.
Clinical note: A very rare but extremely important condition not to miss is cauda equina syndrome. It occurs due to intervertebral disc herniation and following lumbar, sacral and coccygeal nerve root compression. Symptoms and signs of cauda equina syndrome are the following:
- Lumbar back pain
- Unilateral or bilateral leg pain (sciatica)
- Bowel and urinary bladder dysfunction
- Loss of sensation in the perineal area (so-called saddle numbness)
The cauda equina syndrome is treated with surgical decompression of the nerve roots, which must be done as soon as possible.
Spinal cord internal anatomy (cross-section)
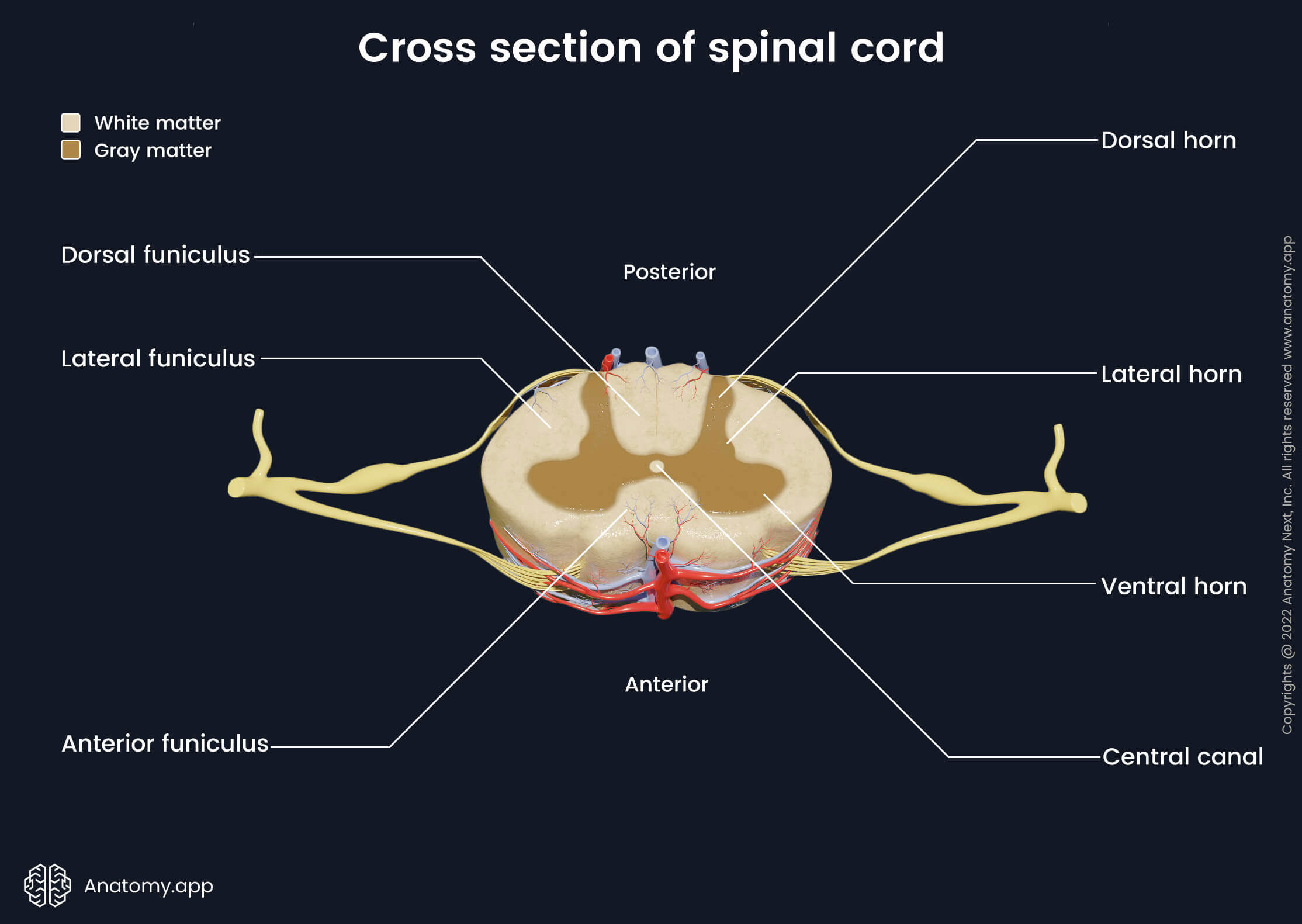
In cross-section, the spinal cord has a small canal in the center - central canal - that is surrounded by a darker butterfly-shaped region that contains gray matter and lighter peripheral area consisting of white matter. The central canal is filled with cerebrospinal fluid and it continues with the fourth ventricle of the brain. The central canal is considered a vestige of the brain’s ventricular system.
Gray matter
The gray matter consists of nerve cell (neuron) bodies and neuroglia that are organized into columns within the spinal cord. The gray matter of the spinal cord resembles a butterfly or letter “H” in cross-section. Therefore, it has several paired projections called horns, and they include the following:
- Ventral (anterior) horns - thin and long projections of the gray matter extending from the central part towards the posterior surface of the spinal cord;
- Dorsal (posterior) horns - wider and shorter, extend towards the anterior surface;
- Lateral horns - the smallest horns located between the ventral and dorsal horns, they are found only in the thoracic and lumbar segments (T1 - L2).
The dorsal and ventral horns are present along the entire length of the spinal cord. On each side of the spinal cord they form columns - right and left anterior and posterior columns. Between the anterior and posterior columns are right and left intermediate columns.
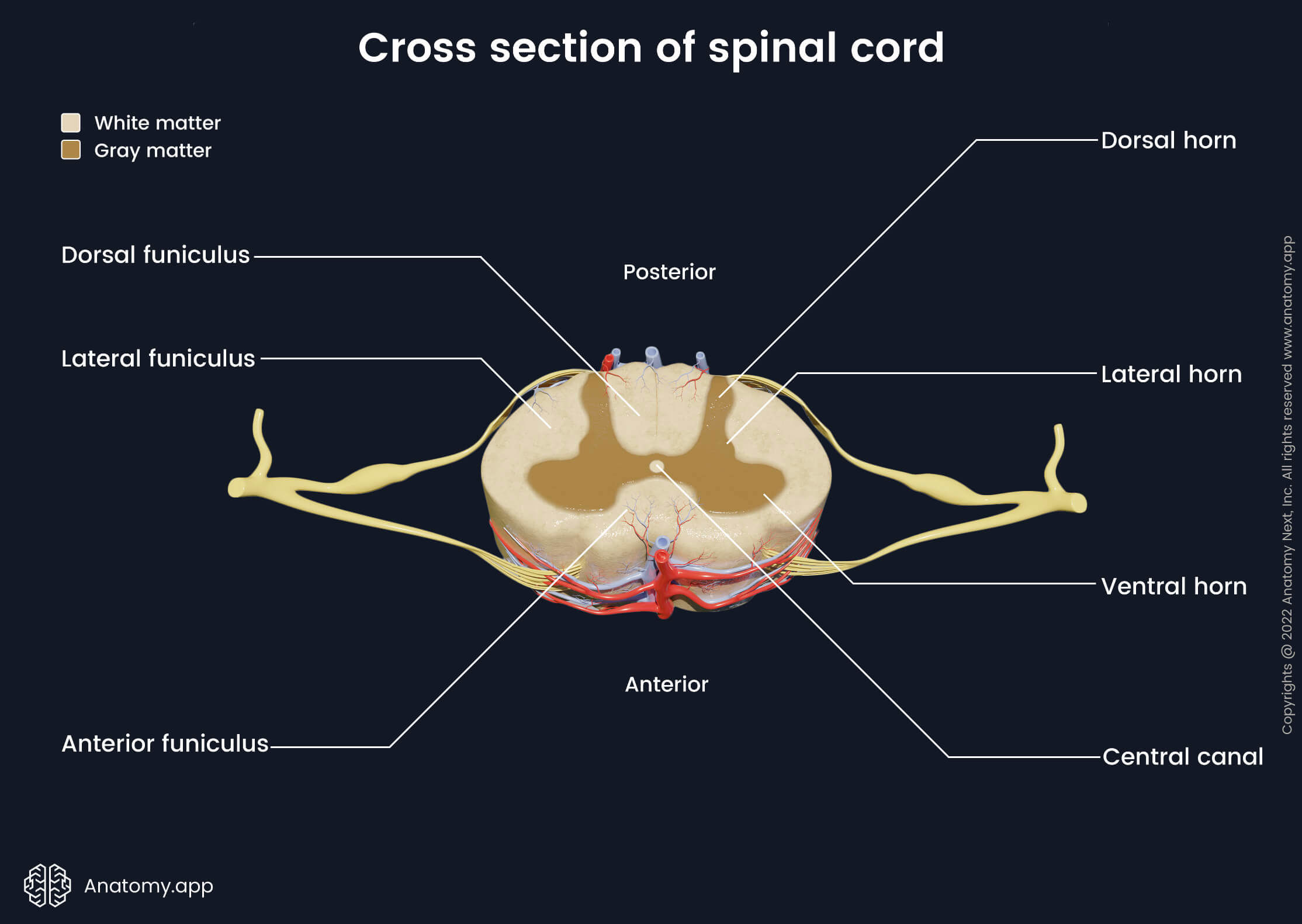
Generally, each horn contains different types of neurons. The dorsal horns primarily contain sensory neurons, while the majority of nerve cells in the ventral horns are motor neurons. The lateral horns mostly contain bodies of sympathetic preganglionic neurons.
Neuron cell bodies that are found within the gray matter form clusters called nuclei. Alternatively, the gray matter is organized into zones known as Rexed's laminae according to the structure and function of neurons located in each zone.
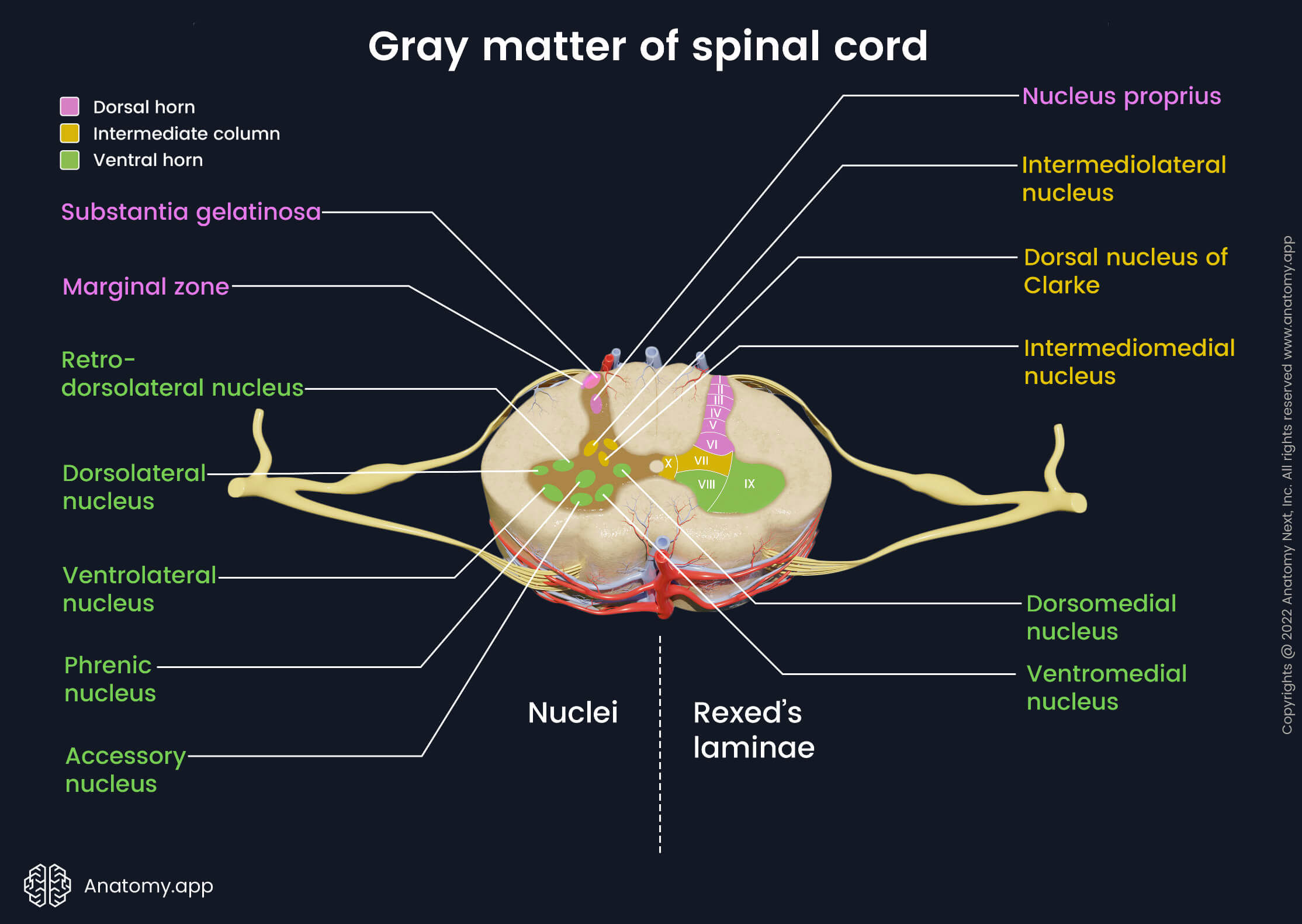
Nuclei of spinal cord
The gray matter of the spinal cord contains multiple groups of neurons called nuclei. These nuclei are located in the horns of the gray matter, and each horn has a different type of nuclei. The dorsal horn contains sensory nuclei, the lateral horn houses sensory and vegetative nuclei, while the anterior horn contains motor nuclei.
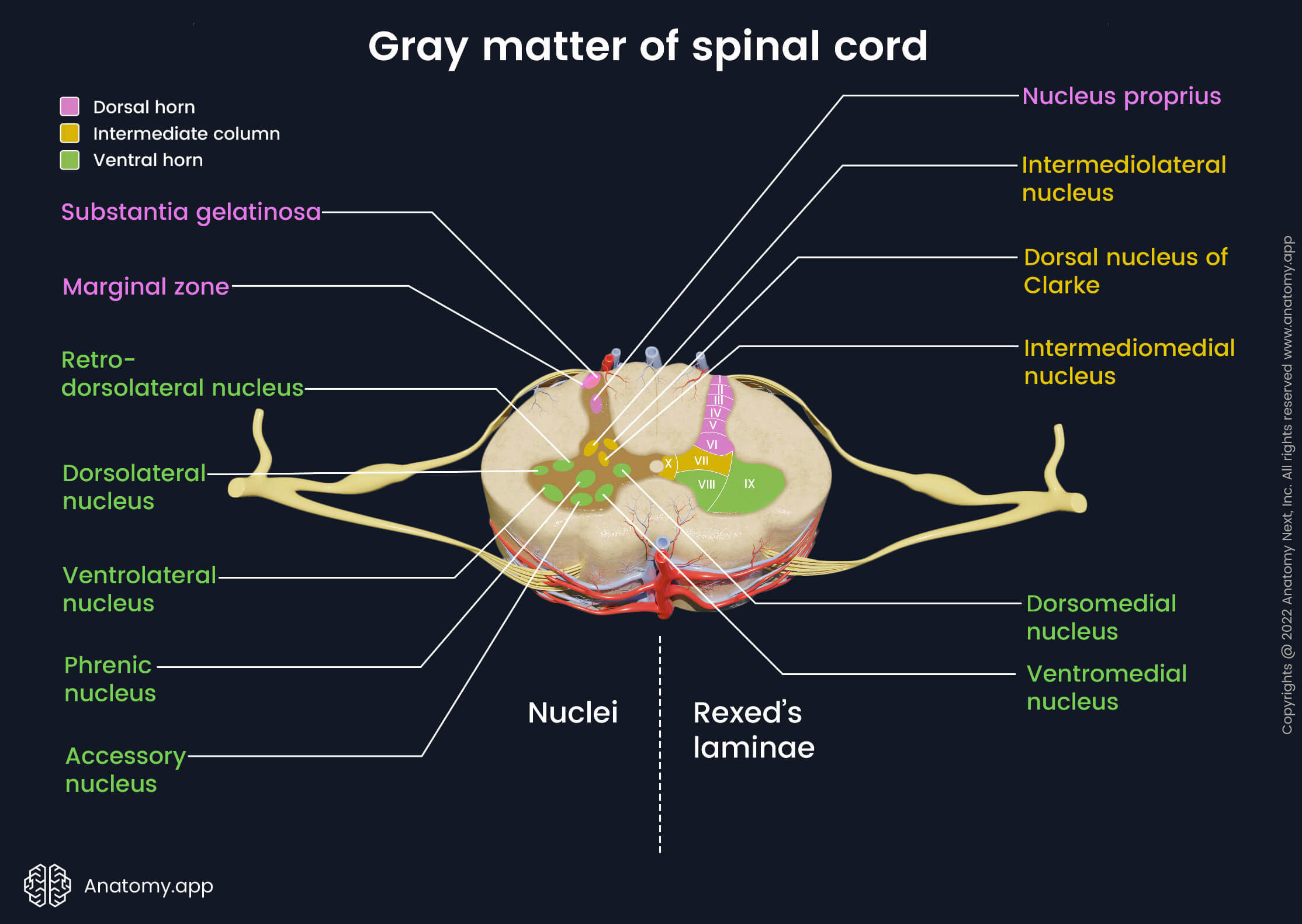
The spinal nuclei belonging to the dorsal horn are the following:
- Marginal zone with marginal nuclei (posteromarginal nuclei) is located at the tip of the dorsal horn. It is found in all spinal cord segments. It receives sensory information about temperature and pain from the skin.
- Substantia gelatinosa (Rolando's gelatinous substance) lies next to the marginal nuclei. It is also present at all segmental levels. It transmits impulses such as pain, temperature and light touch to the brain.
- Nucleus proprius is located below the substantia gelatinosa within the central part of the dorsal horn. This nucleus is also found throughout all segments of the spinal cord. It combines sensory information of light touch, pain and temperature.
Four groups of nuclei are located in the intermediate column of the gray matter:
- Dorsal nucleus of Clarke (Clarke’s column, posterior thoracic nucleus) is situated close to the base of the dorsal horn. It is found from C8 to L2-3 segments. This nucleus is a part of the posterior spinocerebellar tract transmitting unconscious proprioceptive information to the cerebellum. As this nucleus is located almost in between the intermediate column and dorsal horn, some authors consider it a nucleus of the dorsal horn.
- Intermediolateral nucleus is located in the lateral horn. It is found only from T1 to L1-3 segments. This nucleus receives sensory information from internal organs and contains sympathetic preganglionic nerve cells.
- Sacral parasympathetic nucleus is found in a similar location only within S2 - S4 segments. These nuclei contain sacral parasympathetic preganglionic nerve cells.
- Intermediomedial nucleus is located from T1 to L2-3 segments and carries sensory information from internal organs.
In the ventral horn of the spinal cord several motor nuclei are present:
- Medial motor nuclei (ventromedial and dorsomedial nuclei) are found throughout the spinal cord. These nuclei give rise to the fibers that innervate trunk musculature and proximal muscles of the limbs.
- Phrenic nucleus (phrenic nerve nucleus) is located only in the cervical segments (C2-3-5). These nuclei are found in the central part of the ventral horn. It contains neuronal cell bodies that innervate the diaphragm.
- Accessory nucleus (nucleus of spinal roots of the accessory nerve) is positioned only in the cervical segments (C1 - C5). It takes place in the base part of the ventral horn. This nucleus contains neuronal cell bodies that innervate the trapezius and sternocleidomastoid muscles.
- Lateral motor nuclei (ventrolateral, dorsolateral and retrodorsolateral nuclei) are situated in the cervical and lumbar segments. They contain nerve cell bodies that provide motor innervation to the distal muscles of the upper and lower limbs.
Rexed's laminae
In the early 1950s, Swedish neuroscientist Bror Rexed identified and described 10 cytoarchitectonic zones in the gray matter of the spinal cord. These zones are called Rexed's laminae (RL), and they are organized into layers according to their function and structure.
Rexed's laminae are described with Roman numbers from I to X. Each lamina corresponds to a spinal nucleus, and therefore, the laminae are used as an alternative to nuclei when studying the internal anatomy of the spinal cord. The Rexed's laminae are located in all segments of the spinal cord. The spinal cord contains the following Rexed's laminae:
- Laminae I to VI are found within the dorsal horns. RL I corresponds to the marginal nucleus, while RL II to the substantia gelatinosa. RL III - IV are analogous to the nucleus proprius. RL V and VI are the origin of various propriospinal neurons and sometimes are inseparable.
- RL VII is located in the intermediate zone of the gray matter. It corresponds to the dorsal nucleus of Clarke, and the intermediolateral and intermediomedial nuclei.
- RL VIII is found medially in the ventral horn. Therefore, the medial motor nuclei correspond to it. Fibers of many neurons located here cross to the opposite side of the spinal cord.
- RL IX holds the lateral motor, accessory and phrenic nuclei of the ventral horn that innervate skeletal muscles.
- RL X is located around the central canal, and it mainly contains neuroglia.
White matter
The white matter consists mainly of myelinated nerve cell extensions called axons and is located around the gray matter. The axons are organized into tracts (pathways) that connect the brain with the spinal cord and periphery of the body.
A tract is a bundle of nerve fibers with the same origin, destination, course and functions. The name of the pathway usually indicates the place of origin and the site of termination. For example, the corticospinal tract signifies that it starts in the cerebral cortex and ends in the spinal cord.
Tracts can be classified as the ascending or descending. The ascending tracts transmit sensory (afferent) impulses from the periphery of the body and the spinal cord to the brain. The descending tracts carry motor (efferent) information from the brain to the spinal cord and body. The tracts of the spinal cord are organized into three columns or funiculi:
- Anterior (ventral) funiculi - located between anterior horns of the gray matter and anterior median fissure;
- Lateral funiculi - found on either side of the spinal cord between anterior and posterior horns;
- Posterior (dorsal) funiculi - between posterior horns and posterior median sulcus.
Ascending tracts are found in all columns, but descending pathways are located only in the anterior and lateral ones.
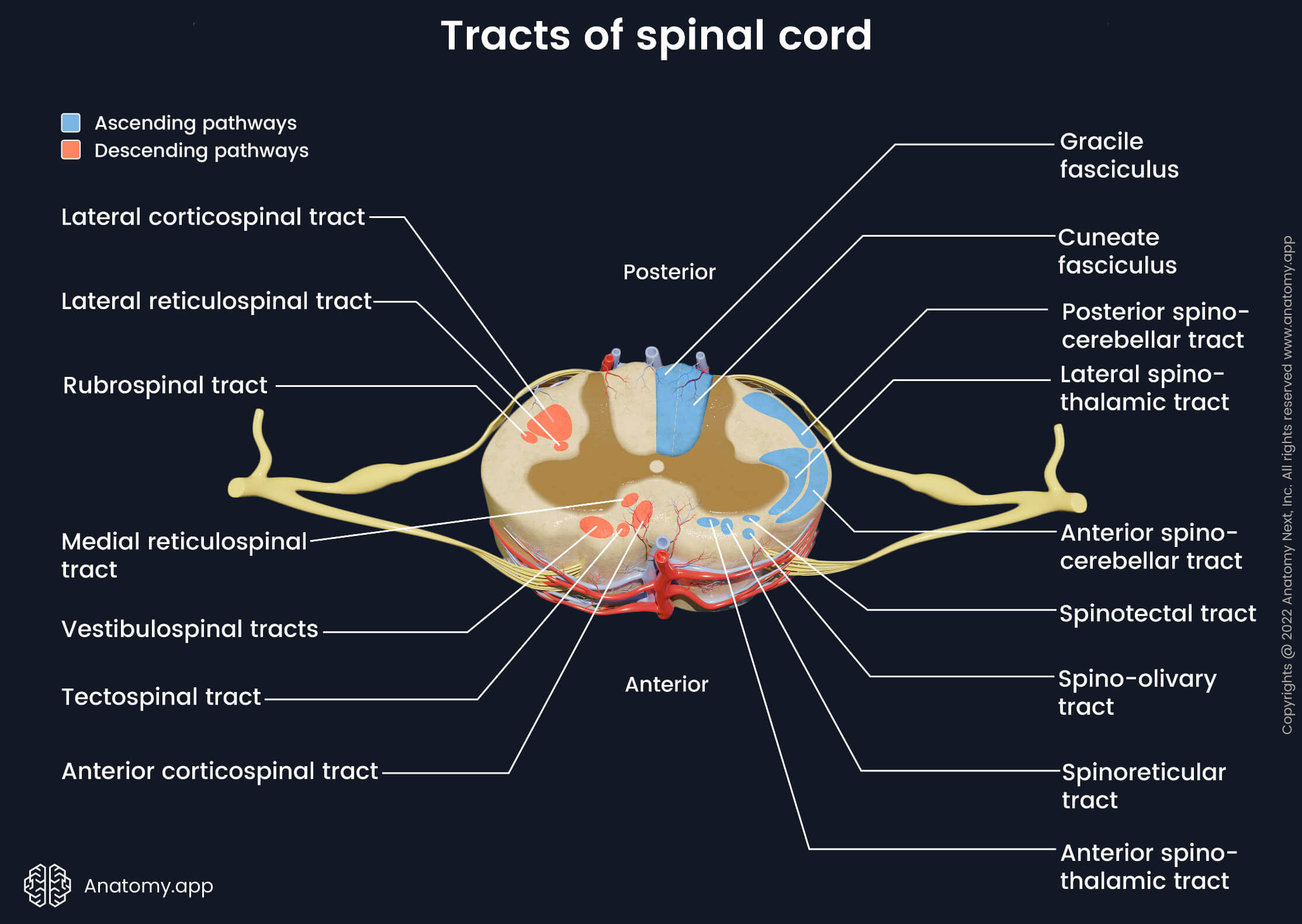
Ascending tracts of spinal cord
Ascending tracts carry sensory nerve fibers from the nerve cell bodies located in the dorsal root ganglion. These pathways include the sensory information about pain, temperature, tactile sense (a sense of touch) and proprioception (perception of the position and motion in the body). This information is carried through a series of neurons that synapse with each other in different locations of the central nervous system.
This sensory information can be perceived in conscious or unconscious levels. Conscious perception of sensory stimuli is processed in the somatosensory area of the cerebral cortex. In contrast, unconscious data is processed in structures of the brain other than the cortex, for example, in the cerebellum. The ascending tracts of the spinal cord include the following:
- Gracile and cuneate fasciculi
- Lateral spinothalamic tract
- Anterior and posterior spinocerebellar tracts
- Anterior spinothalamic tract
- Spino-olivary tract
- Spinoreticular tract
- Spinotectal tract
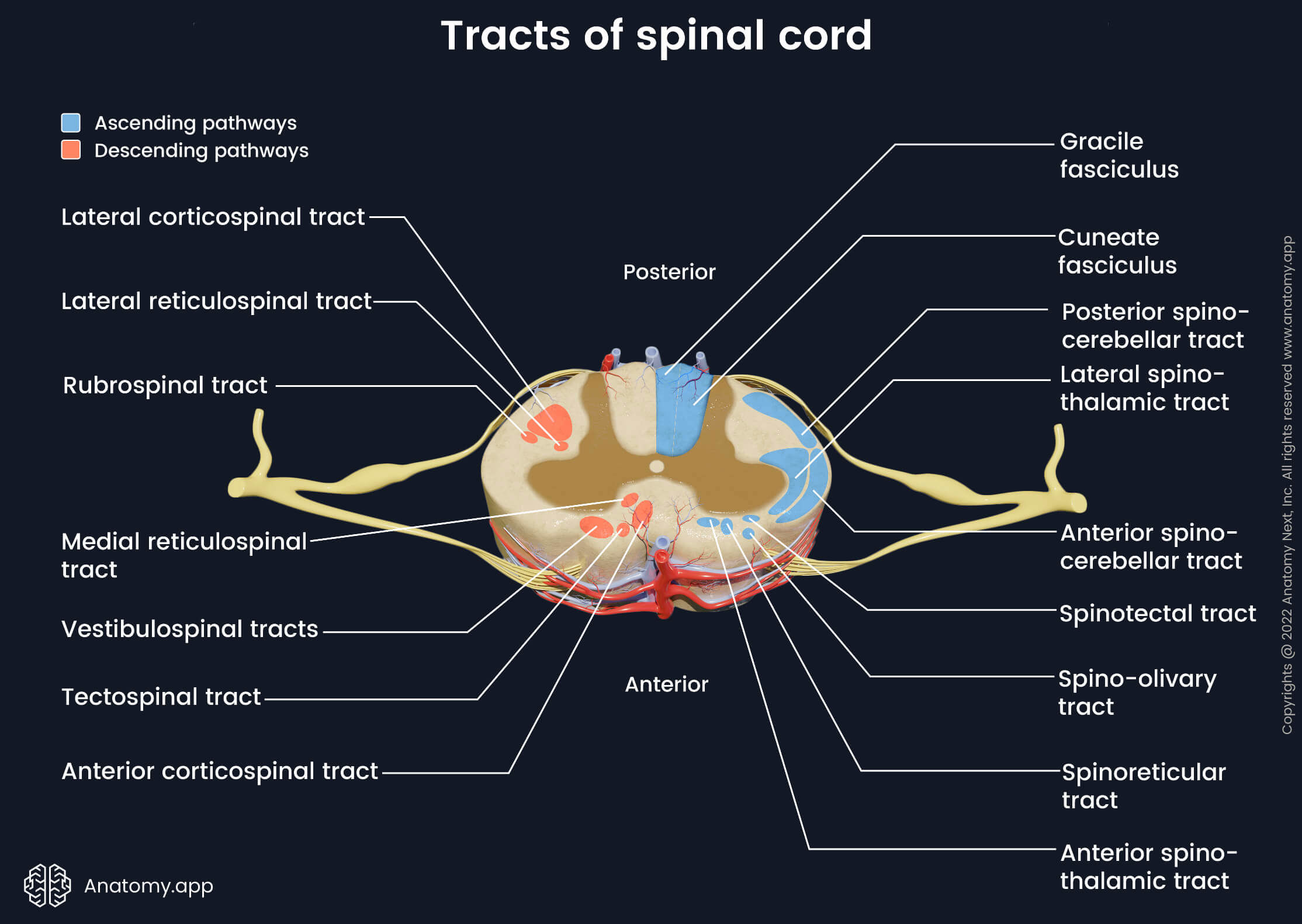
The posterior column contains the ascending gracile fasciculus and cuneate fasciculus. They are also referred to as the dorsal column-medial lemniscus (DCML) pathway. The gracile fasciculus conveys sensory information from the lower trunk and lower limbs. The cuneate fasciculus contains fibers from the upper trunk and upper limbs. These fibers carry information about tactile sense (touch), pressure, vibration and conscious proprioception to the somatosensory cortex.
There are also several ascending tracts in the lateral column. The lateral spinothalamic tract delivers temperature and pain information to the thalamus in the brain. In the thalamus, the fibers of the tract communicate to neurons that convey information further to the cortex. The posterior and anterior spinocerebellar tracts send unconscious proprioception to the cerebellum. The proprioceptors are located in the active and passive parts of the movement apparatus - skeletal muscles, tendons, bursae, ligaments, skin, subcutaneous tissue and joints.
The anterior funiculus joins four various tracts. The anterior spinothalamic tract conveys pressure and crude touch input to the thalamus of the diencephalon and nuclei of the brainstem. The spino-olivary tract connects the spinal cord with the cerebellum via the medulla oblongata. It carries proprioceptive information from the muscles and tendons. The spinoreticular and spinotectal tracts (spinomesencephalic pathway) convey tactile, thermal and pain sensations. The spinoreticular tract connects the spinal cord with the reticular formation of the brainstem, while the spinotectal tract links the spinal cord with the superior colliculi of the midbrain. Some authors describe the spino-olivary, spinotectal and spinoreticular tracts as pathways of the lateral column.
Descending tracts of spinal cord
Descending tracts originate in various regions of the cortex and brainstem nuclei. They carry motor neuron fibers that are in control of voluntary (pyramidal tracts) or involuntary (extrapyramidal tracts) motor functions. These pathways are also responsible for posture, muscle tone, balance, reflexes and coordination of head, neck and eye movements. The descending tracts can be subdivided into two main systems based on their somatotopic organization: lateral and medial motor systems.
The lateral motor system includes the lateral corticospinal and rubrospinal tracts. Fibers of both corticospinal tracts (anterior and lateral) originate from neurons in the motor cortex of the brain. At the level of the caudal medulla, most of the descending corticospinal fibers cross to the opposite (contralateral) side, forming the lateral corticospinal tract. Fibers that stay on the same side (ipsilateral) form the anterior corticospinal tract that is a part of the medial motor system. The lateral corticospinal tract is responsible for the voluntary movements of the upper and lower limbs. The rubrospinal tract originates in the red nucleus of the midbrain. This tract regulates muscle activity and tone in flexor muscle groups.
The medial motor system controls and regulates head, neck, and trunk muscles. It helps to maintain balance, muscle tone and posture, also it coordinates head and eye movements. The anterior corticospinal tract is formed by the fibers of the corticospinal tract that do not cross to the opposite side in the caudal medulla. The fibers descend to reach the spinal cord.
The tectospinal tract starts from the neurons in the superior colliculus of the midbrain. The superior colliculus receives visual information. Hence, according to visual input, the tectospinal tract provides eye and head-turning reflexes as responses to visual and auditory stimuli. The reticulospinal tract originates in the reticular formation of either pons (medial (pontine) reticulospinal tract) or medulla oblongata (lateral (medullary) reticulospinal tract). This tract regulates involuntary movements and reflexes related to posture and gait.
Two vestibulospinal tracts originate from the vestibular nuclei in the pons and medulla. The medial vestibulospinal tract starts in the medial vestibular nucleus and terminates in the upper thoracic spinal cord segments. The lateral vestibulospinal tract arises from the lateral vestibular nucleus and extends throughout the entire length of the spinal cord. Vestibular nuclei receive sensory information from the middle ear and cerebellum. Therefore, this tract coordinates between flexor and extensor muscles to maintain balance and posture.
Blood supply of spinal cord
Arterial blood supply
The arterial blood supply of the spinal cord primarily comes from the vertebral arteries - branches of the subclavian arteries. All blood vessels supplying the spinal cord are organized in two directions - longitudinal (vertical) and horizontal. The longitudinally-oriented blood vessels are located on the outer surfaces of the spinal cord and they extend throughout its length. The horizontal-lying segmental spinal arteries and their branches supply each spinal cord segment by entering the vertebral canal via intervertebral foramina.
The segmental spinal arteries originate mainly from the deep and ascending cervical and vertebral arteries in the neck region, posterior intercostal and subcostal arteries in the thoracic region and lumbar arteries in the abdominal region. Within the vertebral canal, the segmental spinal arteries further divide into several smaller arteries:
- Anterior and posterior radicular arteries - vessels that supply the anterior and posterior roots, respectively;
- Segmental medullary arteries - eight to ten arteries that directly flow into the anterior and posterior spinal arteries.
The largest of the segmental medullary arteries is the great anterior radiculomedullary artery (also called the artery of Adamkiewicz). This artery arises between T8/9 and L2 levels and supplies the lumbosacral enlargement of the spinal cord.
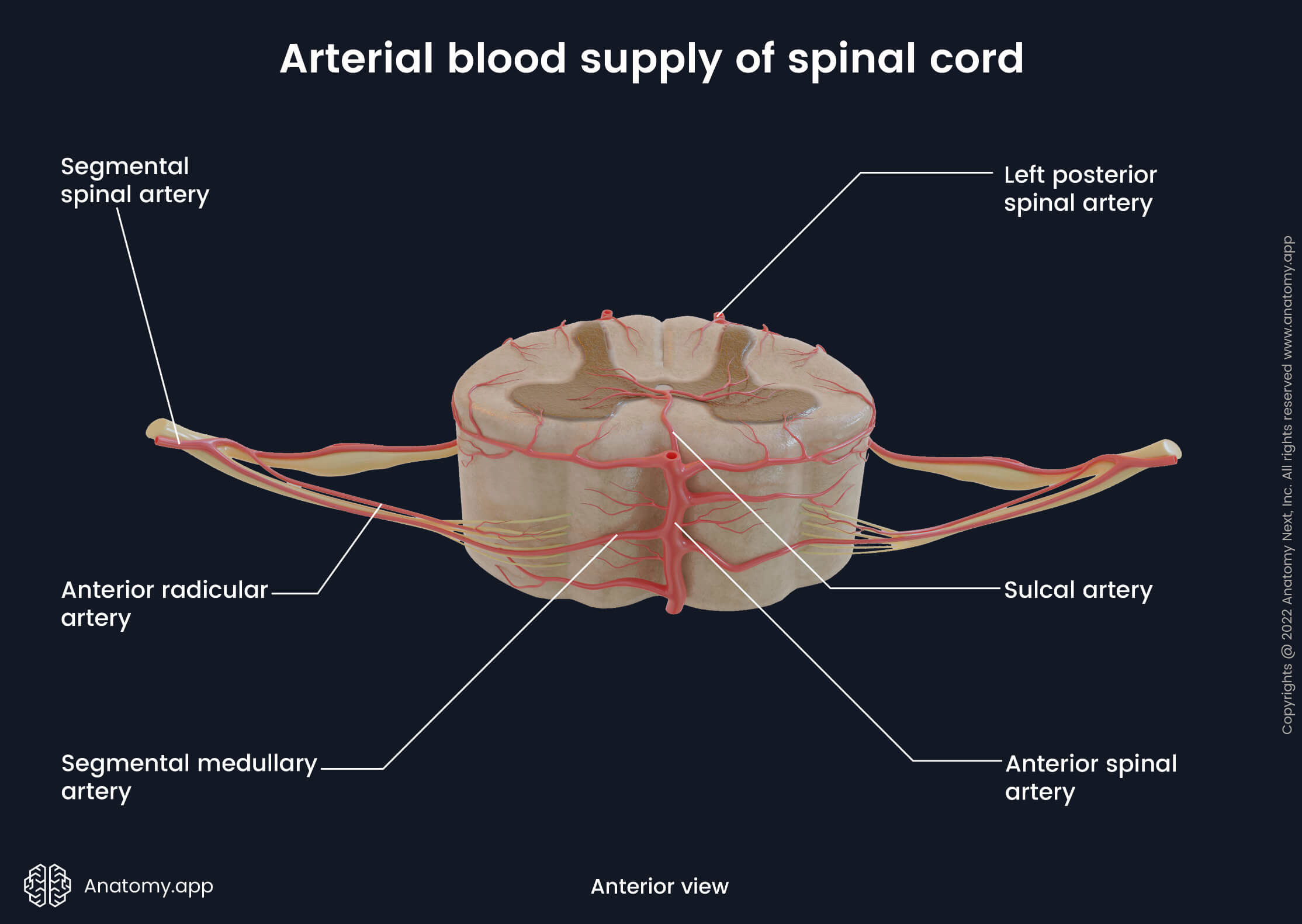
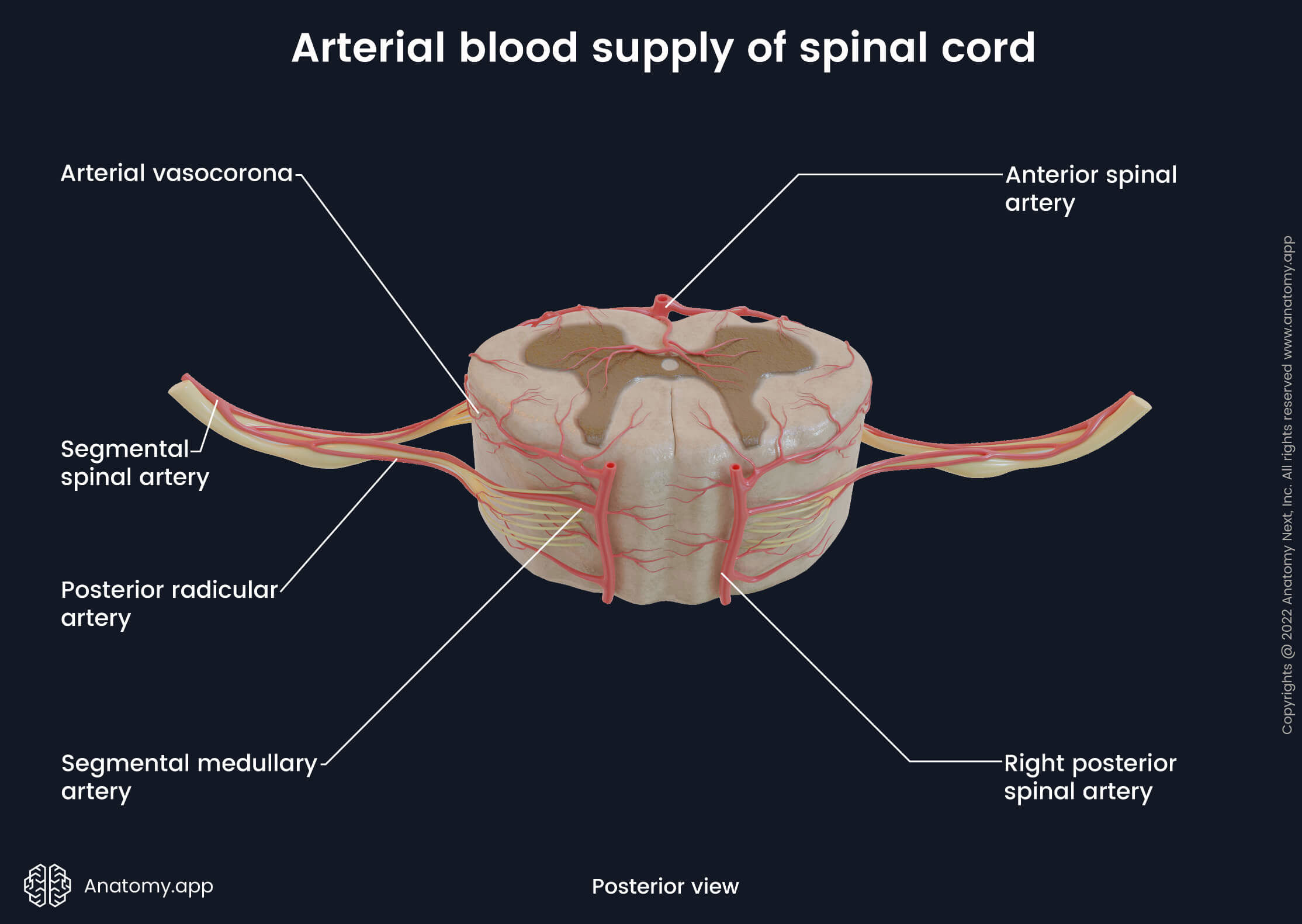
The longitudinal arteries arise from the vertebral arteries, and they include the following:
- One anterior spinal artery - formed in the cranial cavity at the level of the foramen magnum by merging of two anterior spinal branches of each intracranial vertebral artery. It goes down the spinal cord along the anterior median fissure and supplies anterior two-thirds of the spinal cord.
- Two posterior spinal arteries - also branch off each vertebral artery in the cranial cavity. Both posterior spinal arteries descend along the right and left posterolateral sulci, and they supply posterior one-third of the spinal cord.
The anterior and posterior spinal arteries are connected with each other by pial anastomoses and plexuses known as the arterial vasocorona. They encircle the spinal cord and supply its lateral aspects. As mentioned earlier, the anterior and posterior spinal arteries also anastomose with the segmental medullary arteries.
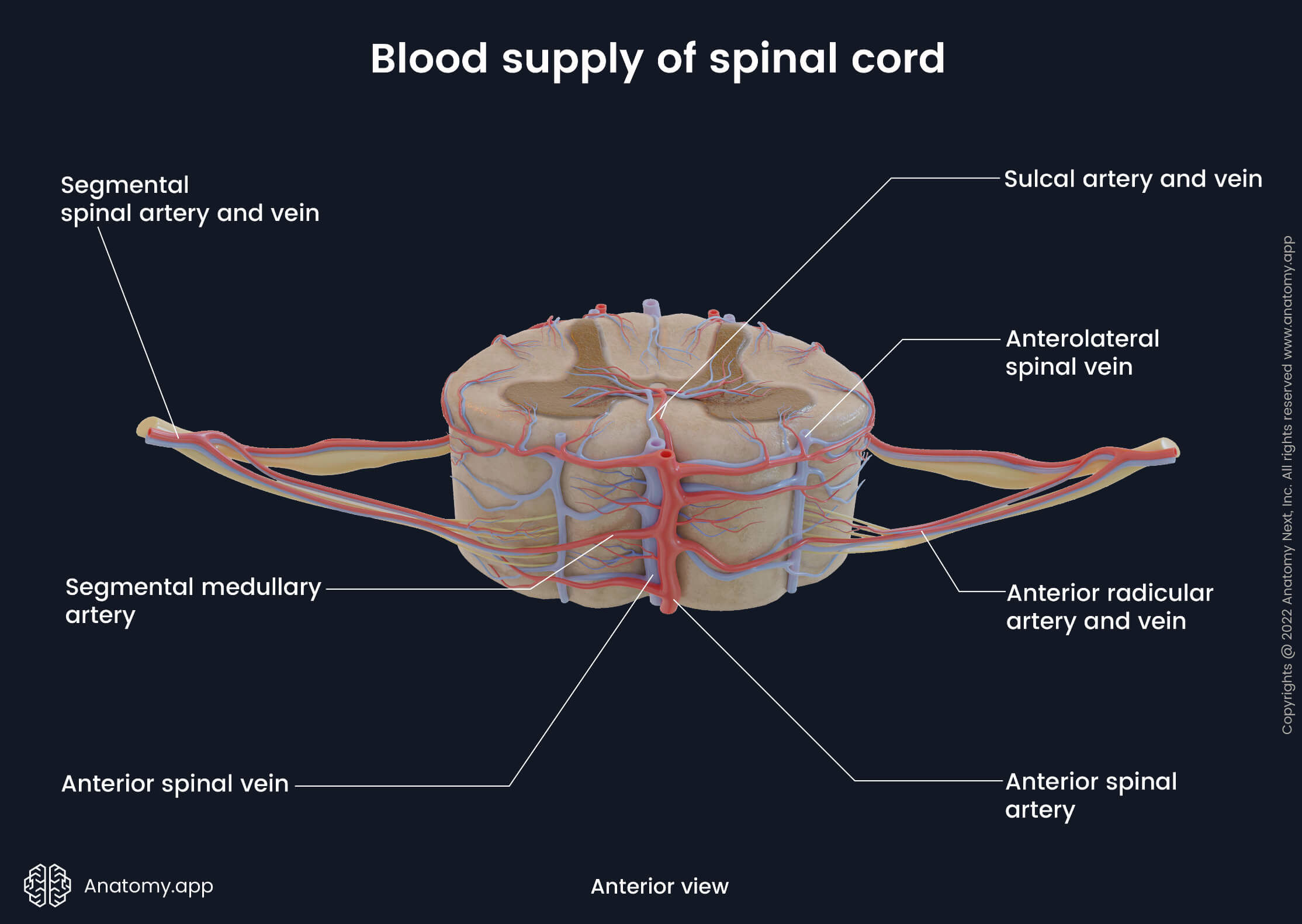
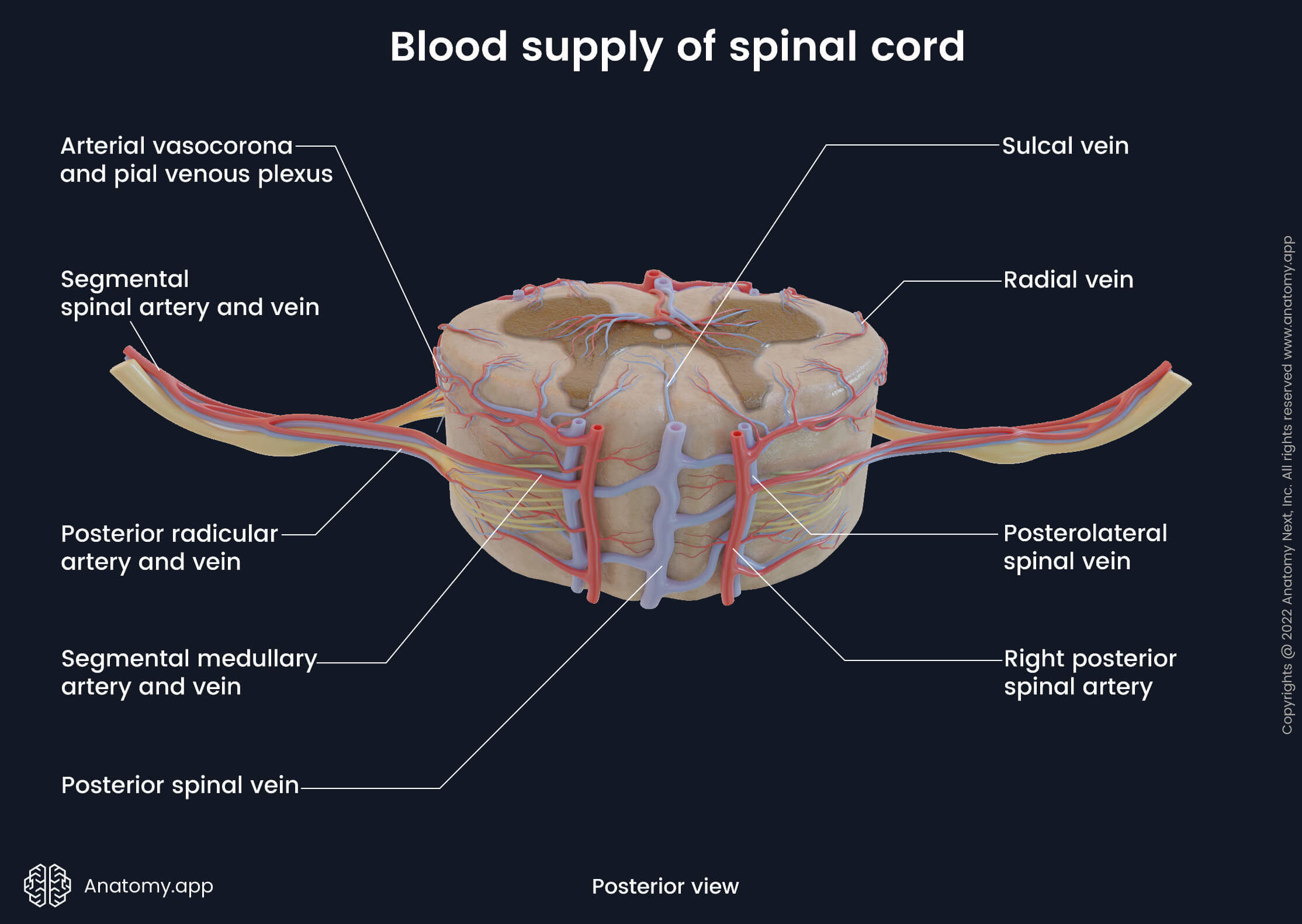
Venous drainage
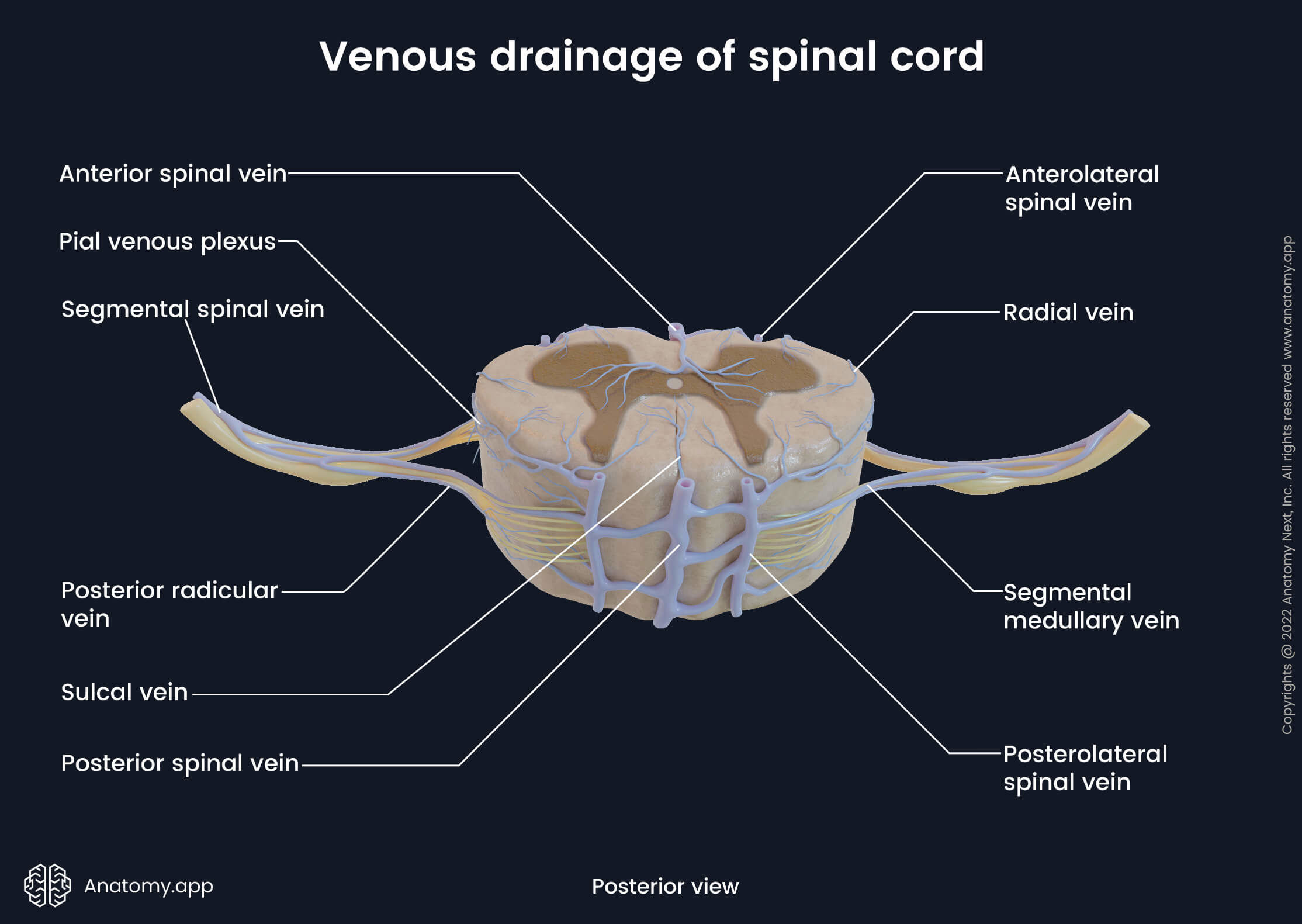
The venous drainage of the spinal cord is primarily provided by six longitudinal oriented spinal veins that surround the spinal cord and are located within the grooves and fissures of its external surface. These veins do not contain valves, and venous drainage of the spinal cord is induced by the gravity, intra-thoracic and intra-abdominal pressures and body position. The spinal veins go parallel to their respective arteries, and they share almost the same location as the arteries. And finally, all spinal veins are also organized in two directions - longitudinal (vertical) and horizontal.
The longitudinal veins include the following:
- Anterior spinal vein (anterior median spinal vein) - central vein that drains the anterior aspect of the spinal cord; lies in the anterior median fissure;
- Posterior spinal vein (posterior median spinal vein) - central vein that drains the rear aspect of the spinal cord; passes in the posterior median fissure;
- Posterolateral spinal veins - two veins that extend along the right and left posterolateral sulci and drain posterolateral parts of the spinal cord;
- Anterolateral spinal veins - two veins that go along the right and left anterolateral sulci and drain anterolateral portions of the spinal cord.
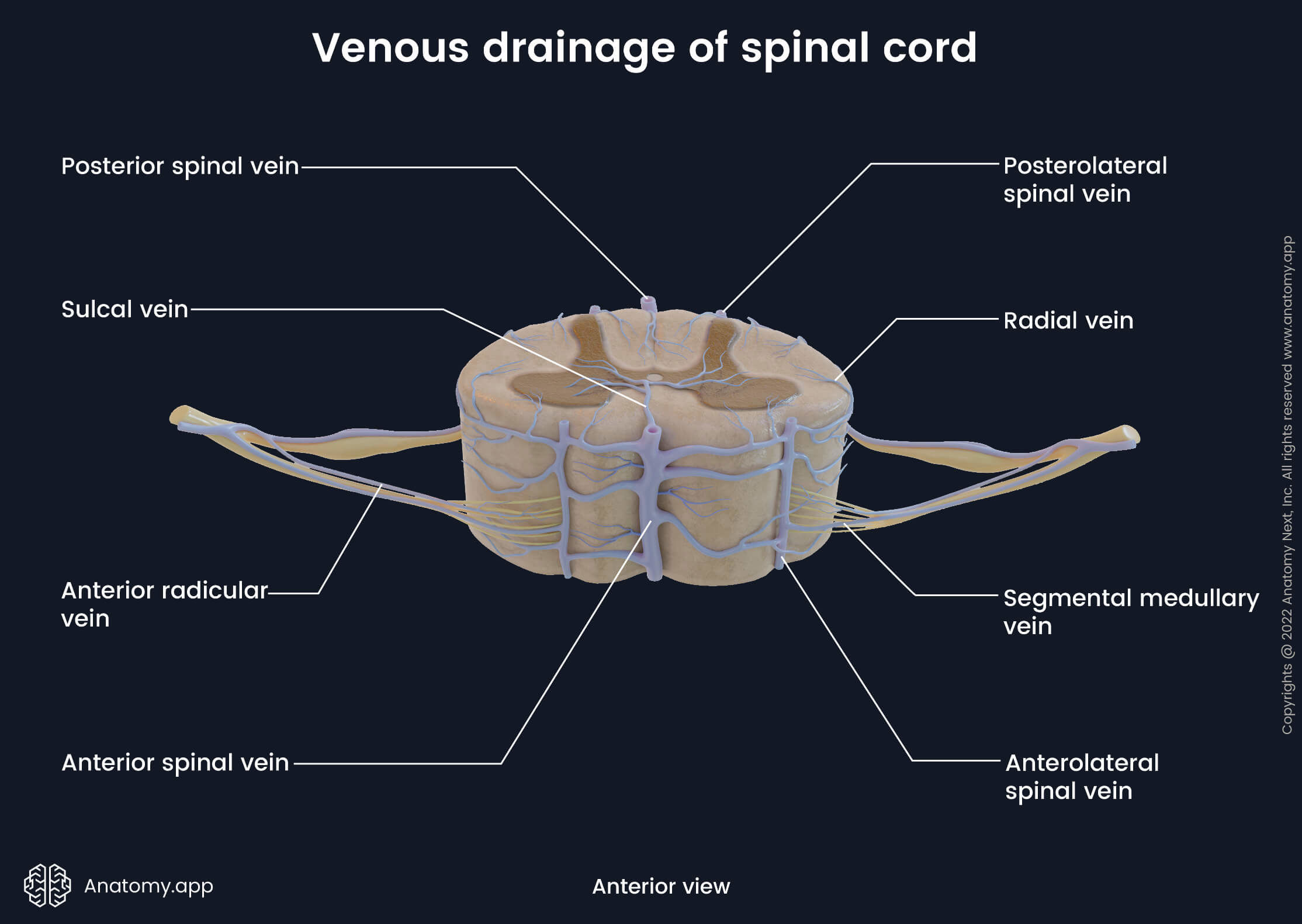
All these longitudinal veins communicate with each other and form numerous anastomoses on the external surface of the spinal cord. This anastomosing venous network is called the pial venous plexus. Longitudinal spinal veins and pial venous plexus can also be classified as extramedullary veins that do not extend into the spinal cord. In contrast, small veins that extend into the spinal cord and are located within it are called the intramedullary veins.
The intramedullary veins include the radial and sulcal veins. In cross-section, the radial veins are found along the sides of the spinal cord. In contrast, the sulcal (central) veins are situated within the central part of the spinal cord, and usually, they extend into the anterior and posterior median fissures.
The segmental veins share the same names as the arteries, and they include the anterior and posterior radicular veins and segmental medullary veins. These veins are also referred to as radiculomedullary veins, and they drain roots of the spinal nerves and longitudinal veins. Venous blood from the radiculomedullary veins is carried to the anterior and posterior internal vertebral venous plexuses located within the subdural space.
The internal vertebral venous plexus further drains blood via the intervertebral veins to the anterior and posterior external vertebral venous plexuses that surround the spine. And finally, the external vertebral venous plexuses in the neck region drain into the vertebral veins while in the trunk into the intercostal, lumbar and lateral sacral veins.
Spinal meninges
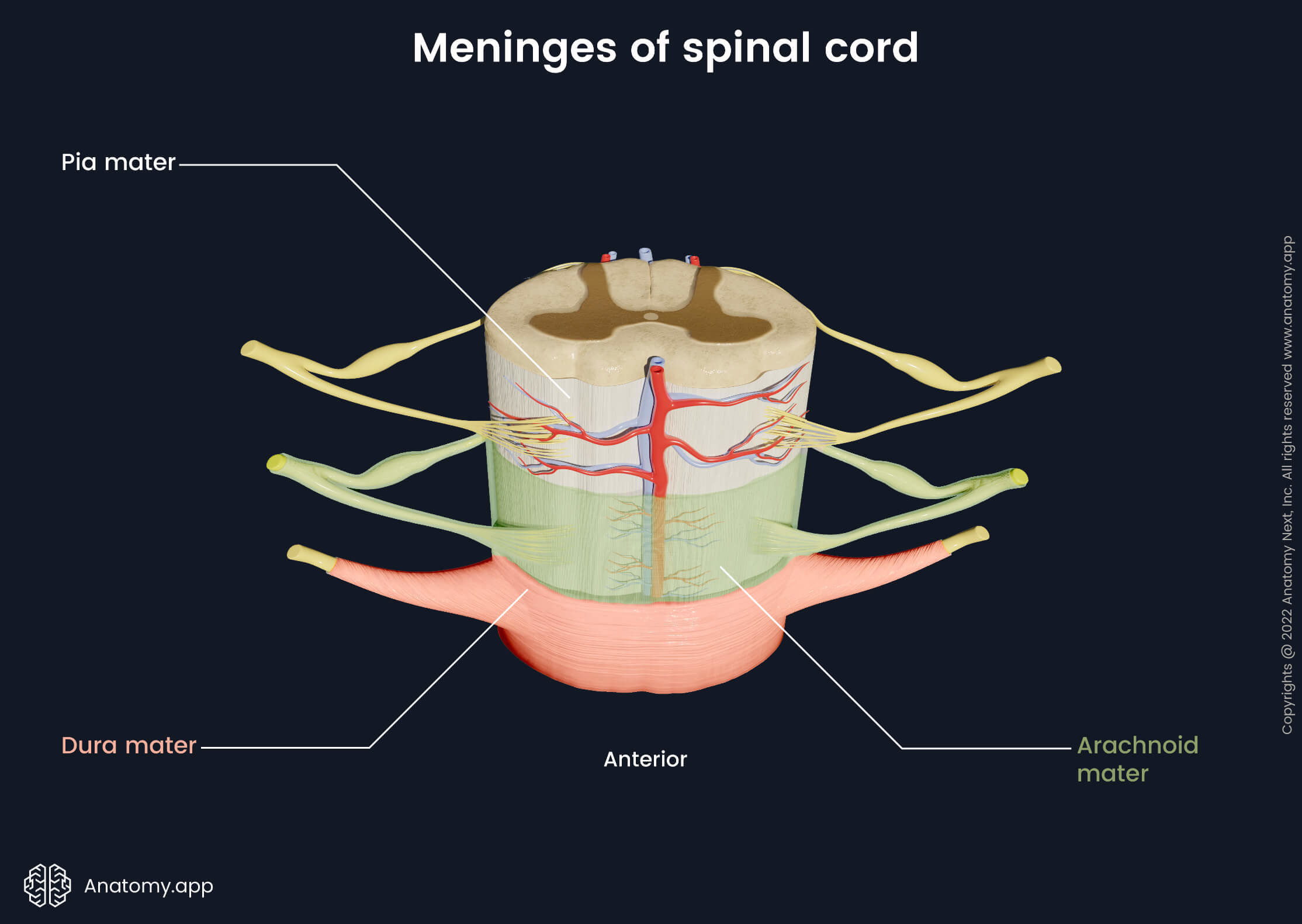
Like the brain, the spinal cord is covered and protected by three membranous layers called spinal meninges. The three meninges are pia mater, arachnoid mater and dura mater. The pia mater is the innermost layer. It is highly vascular and contains many blood vessels. The pia mater provides blood supply to the spinal cord.
The arachnoid mater is a nonvascular middle layer that lies next to the outermost layer - the dura mater - but is not connected to it. The dura mater is a tough outer layer that covers the spinal cord. It is formed by connective tissue that contains a great amount of collagen and elastin fibers. The dura mater also covers the spinal nerve roots as they leave the intervertebral foramina.
Meningeal spaces
All three meningeal layers do not connect. Instead, between each of them and the vertebral canal walls are three gaps called meningeal spaces. The space between the vertebral canal wall and dura mater is known as the epidural space, which is an injection site for epidural anesthesia. Between the dura mater and arachnoid mater is the subdural space, while between the arachnoid mater and pia mater is the subarachnoid space containing cerebrospinal fluid (CSF). The subarachnoid space extends from the foramen magnum superiorly to the second sacral vertebra (S2) level inferiorly. The subarachnoid space contains:
- Cerebrospinal fluid
- Spinal nerves
- Blood vessels supplying the spinal cord
- Denticulate ligaments (extensions of the pia mater)
- Trabecular network (arachnoid trabeculae) between the pia mater and arachnoid membrane
Clinical applications
The subarachnoid space can be assessed in the lumbar region without damaging the spinal cord. It is important in lumbar puncture, during which a sample of CSF is obtained for examination. Additionally, some antibacterial, chemotherapy and pain medication (anesthetics) can be injected into the subarachnoid space. Also, during the lumbar puncture, the pressure of the CSF can be measured and controlled. If needed, it can be reduced by removing a small amount of the fluid. The subarachnoid space can be assessed below the L2 level, usually between the L3 and L4 or L4 and L5 levels.
Lumbar puncture
The lumbar puncture technique requires precision. The patient usually lies on the side with the chin tucked to the chest and knees tucked to the abdomen. A needle is inserted between the spinous processes of the vertebrae reaching the epidural space. By piercing the dura mater and arachnoid mater, the subarachnoid space is attained. Most needles can push the nerve roots away from its tip and not cause the patient any nerve damage.
Anesthesia
Besides collection of CSF from the subarachnoid space, some medications, including anesthetics, can be administered to it. Overall, local anesthetics can be administered into two spaces - the epidural space (called epidural anesthesia) or the subarachnoid space (spinal anesthesia). Such anesthesia is useful in surgeries performed on the pelvis and legs, and also in obstetrics during child delivery. It allows proper pain relief without the need for general anesthesia. Both anesthesias affect the sacral and lumbar nerve roots in slightly different places.
In the case of epidural anesthesia, the needle pierces the supraspinous, interspinous and yellow ligaments (ligamenta flava). The medication is distributed in the vertebral canal and affects nerves located within the epidural space. In spinal anesthesia, the needle is pierced further through the dura mater and arachnoid mater. The anesthetic then affects the nerve roots directly in the subarachnoid space.
References:
- Canale, T. S. (2021). Campbell’s Operative Orthopaedics. Volume One. 10th Edition (Volume 1). Mosby.
- Chestnut, D., Wong, C., & Tsen, L. (2019). Chestnut’s Obstetric Anesthesia: Principles and Practice: Expert Consult - Online and Print (6th ed.). Elsevier.
- Drake, R., Vogl, W., & Mitchell, A. (2017). Gray’s Basic Anatomy (2nd ed.). Elsevier.
- Drake, R., & Vogl, W. (2014). Gray’s Anatomy for Students: With Student Consult Online Access (3rd ed.). Churchill Livingstone.
- Gray, H., & Carter, H. (2021). Gray’s Anatomy (Leatherbound Classics) (Leatherbound Classic Collection) by F.R.S. Henry Gray (2011) Leather Bound (2010th Edition). Barnes & Noble.
- Naidich, T. P., Castillo, M., Cha, S., Raybaud, C., Smirniotopoulos, J. G., Kollias, S., & Kleinman, G. M. (2010). Imaging of the Spine: Expert Radiology Series, Expert Consult-Online and Print (1st ed.). Saunders.
- Winn, R. (2022). Youmans and Winn Neurological Surgery: 4 - Volume Set (Youmans Neurological Surgery) (8th ed.). Elsevier.